Why silvery patches are seen in psoralen
Reading File
search_medical_text
psoriasis silvery white scales pathogenesis keratinocyte
search_medical_image
psoriasis silvery scales plaque
GradeResponse
GradeResponse
The question uses "psoralen" but the context clearly refers to psoriasis (psoralen is a photosensitizing drug used in PUVA therapy for psoriasis). Here is a thorough explanation of why silvery patches appear in psoriasis.
Silvery Scales in Psoriasis — Pathogenesis
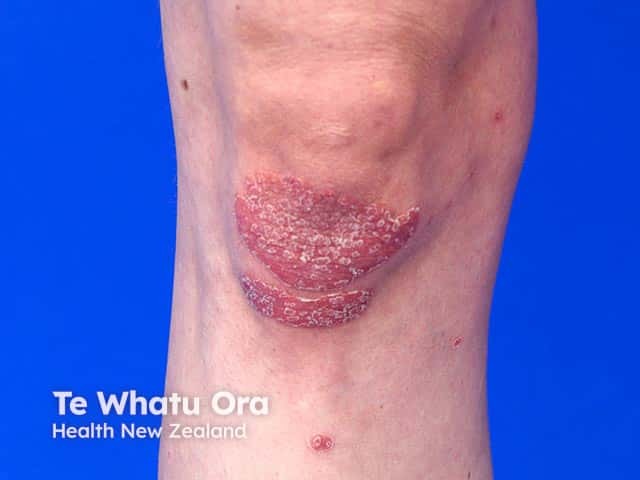
The Core Mechanism
The silvery appearance is the direct result of markedly accelerated, abnormal keratinocyte proliferation and defective differentiation, driven by autoimmune inflammation.
| Step | Normal skin | Psoriatic skin |
|---|---|---|
| Keratinocyte turnover time | ~28 days | 3–5 days |
| Cornification | Complete, with keratohyalin granules | Incomplete (parakeratosis) |
| Stratum corneum | Anucleate, tightly packed, translucent | Nucleated, loosely packed, opaque-white |
Why Specifically Silvery?
-
Parakeratosis — Keratinocytes in psoriasis proliferate so rapidly they reach the surface before completing normal differentiation. They retain their nuclei and fail to produce keratohyalin granules. This produces a thick, loose, lamellar (plate-like) scale rather than the normal thin, clear stratum corneum.
-
Air trapping between scale layers — The loosely packed, parakeratotic cells trap air between the lamellae. This creates multiple refractive interfaces that scatter and reflect incident light diffusely, giving the characteristic silvery-white ("micaceous") sheen — the same physics that makes mica or frost appear silver.
-
Scale thickness — The hyperproliferative epidermis produces a markedly thickened stratum corneum. The more layers of parakeratotic cells, the more light is reflected rather than transmitted, intensifying the whitish appearance.
-
Underlying erythema as contrast — The dermis beneath is intensely vascular (dilated, tortuous capillaries due to VEGF released by inflammatory cytokines). This red base provides sharp contrast that makes the white scale appear even more silvery.
The Inflammatory Cascade (Cause of the Hyperproliferation)
According to Care for the Management of Psoriasis with Phototherapy (p. 30), psoriasis is an autoimmune condition driven by inappropriate activation of cutaneous T cells and dendritic cells, which release:
- IL-17, IL-22 → directly stimulate keratinocyte proliferation and inhibit terminal differentiation
- IL-1, IL-6, TNF-α → amplify epidermal hyperplasia and dermal angiogenesis
- IL-23 → sustains Th17 cell activity
The net result is acanthosis (epidermal thickening), parakeratosis, and Munro microabscesses (collections of neutrophils in the stratum corneum) — the histological hallmarks of psoriasis.
Clinical Correlate: Auspitz Sign
When the silvery scales are scraped off, they come off in layers (like candle wax — "grattage"). Continued scraping reveals a shiny membrane (last layer of parakeratotic cells), and further removal produces pinpoint bleeding (Auspitz sign) from the dilated dermal capillary loops that have grown very close to the surface.
Summary
The silvery patches in psoriasis result from:
- Immune-mediated cytokine release (IL-17, TNF-α, etc.)
- Rapid keratinocyte turnover (~5 days vs. 28 days normal)
- Incomplete cornification → parakeratosis (nucleated cells retained)
- Loose, lamellar scale with air trapped between layers
- Diffuse light scattering → silvery-white reflective appearance
- Contrast against the underlying erythematous dermis
Types of kobners phenomena in detail
search_medical_text
Koebner phenomenon types isomorphic response skin
search_medical_text
reverse Koebner phenomenon pseudo-Koebner pathergy skin diseases
GradeResponse
GradeResponse
search_medical_text
Koebner phenomenon lichen planus vitiligo warts trauma skin lesions
search_medical_text
true Koebner facultative obligate isotopic response dermatology
Based on retrieved sources and comprehensive medical knowledge, here is a detailed breakdown of all types of Koebner phenomena.
Koebner Phenomenon — Types in Detail
The Koebner phenomenon (KP), described by Heinrich Koebner in 1876, refers to the appearance of new skin lesions at sites of cutaneous trauma in a patient with a pre-existing skin disease. The new lesions are morphologically identical to the original disease lesions — hence the alternate name isomorphic response (Harrison's, p. 1533).
Classification Overview
| Type | Also Called | Direction | Mechanism |
|---|---|---|---|
| True KP | Isomorphic response | Trauma → disease lesion | Immune/inflammatory activation |
| Pseudo-KP | — | Trauma → different disease implanted | Inoculation/infection |
| Reverse KP | — | Trauma → clearing of lesion | Unknown |
| Pathergy | Hyperreactivity | Minor trauma → exaggerated pustule/papule | Neutrophil hyperactivity |
| Isotopic response | Wolf's isotopic response | New disease in site of healed old disease | Residual neuro-immune alteration |
1. True (Isomorphic) Koebner Phenomenon
Definition: Trauma to previously normal skin provokes the appearance of the patient's own skin disease at the exact site of injury.
Key features:
- Lesions appear after a latent period of 1–2 weeks (up to several months)
- New lesions are morphologically identical to existing disease lesions
- Occurs only during active disease in most conditions
- The trauma can be mechanical, thermal, chemical, electrical, or radiation-induced
Classic diseases showing true KP:
| Disease | Notes |
|---|---|
| Psoriasis | Most classic; trauma activates Th17 response at wound site |
| Lichen planus | Linear lesions along scratch marks; very characteristic |
| Vitiligo | Trauma → depigmentation at wound site |
| Lichen nitidus | Tiny flesh-colored papules appear along scratches |
| Pityriasis rubra pilaris | Less common |
| Keratosis follicularis (Darier disease) | Genetic disorder; trauma triggers lesions |
Pathogenesis of true KP (psoriasis model):
- Skin trauma activates keratinocytes → release of IL-1, CXCL1, CXCL8
- Recruitment of dendritic cells and T cells to wound site
- Local Th17 activation → IL-17, TNF-α → keratinocyte hyperproliferation
- Psoriatic plaque forms at trauma site within ~2 weeks
2. Pseudo-Koebner Phenomenon
Definition: Trauma introduces an exogenous pathogen or foreign material into the skin, which then produces lesions of a different nature — not the patient's own disease but an implanted infection/condition.
Key distinction from true KP: The new lesion is caused by an implanted agent, not by the patient's own immune-mediated disease process.
Examples:
| Condition | Mechanism |
|---|---|
| Viral warts (HPV) | Trauma inoculates HPV into skin → new warts at scratch/shave sites |
| Molluscum contagiosum | Scratching spreads poxvirus to traumatized skin |
| Tinea (dermatophytes) | Trauma inoculates fungal spores |
| Cutaneous tuberculosis | Traumatic inoculation of M. tuberculosis |
3. Reverse Koebner Phenomenon
Definition: Trauma or injury to a diseased area causes clearing or disappearance of the skin lesion at that site.
Key features:
- The opposite of the isomorphic response
- Seen in conditions where the existing lesion resolves after trauma rather than spreading
- Mechanism poorly understood — possibly related to local immune exhaustion or altered blood flow
Examples:
| Condition | Notes |
|---|---|
| Vitiligo | Repigmentation can occasionally occur at sites of trauma (opposite of KP) |
| Psoriasis | Rarely, local trauma can lead to clearing of a plaque (very uncommon) |
| Plane warts | Inflammatory reaction post-trauma can lead to spontaneous resolution |
4. Pathergy (Hyperergic KP)
Definition: An exaggerated, non-specific inflammatory response to minimal trauma (e.g., a needle prick), producing a papule or pustule at the injury site within 24–48 hours.
Key features:
- Represents neutrophil hyperreactivity
- Not disease-specific per se — it is a marker of systemic inflammatory hyperreactivity
- The pathergy test involves pricking the forearm with a sterile needle and reading at 48 hours (positive = papule/pustule ≥ 2 mm)
Diseases where pathergy is positive:
| Disease | Clinical relevance |
|---|---|
| Behçet syndrome | Part of the ISG diagnostic criteria (Harrison's, p. 10264) |
| Sweet syndrome | Neutrophilic dermatosis; pathergy positive |
| Pyoderma gangrenosum | Classic pathergy — minor trauma triggers massive ulceration |
| PAPA syndrome | Pyogenic arthritis, pyoderma, acne — autoinflammatory |
Pathergy in pyoderma gangrenosum is clinically critical — surgeons must be warned never to debride or operate aggressively, as trauma worsens the ulcers dramatically.
5. Isotopic Response (Wolf's Isotopic Response)
Definition: The appearance of a new, unrelated skin disease at the exact site where a previous skin disease has already healed.
Key features:
- Described by Ronni Wolf in 1995
- The new disease is different from the original one
- The healed site acts as a "locus minoris resistentiae" (site of least resistance)
- Mechanism: residual neurovascular and immune changes in the previously affected dermis
Examples:
| Original disease (healed) | New disease appearing at same site |
|---|---|
| Herpes zoster | Granuloma annulare, lichen planus, psoriasis, sarcoidosis |
| Herpes simplex | Eczema, lichen planus |
| Chickenpox scars | Kaposi sarcoma (in HIV patients) |
6. Renbok Phenomenon (Reverse Isotopic Response)
Definition: A rare phenomenon where an existing skin disease does not develop in the area of another ongoing skin disease. The two diseases mutually exclude each other spatially.
- "Renbok" = "Koebner" spelled backwards
- Example: Psoriasis and alopecia areata patches do not overlap — the scalp affected by alopecia areata is often spared from psoriasis
Summary Table
| Phenomenon | Trigger | Result | Classic Disease |
|---|---|---|---|
| True KP (Isomorphic) | Trauma to normal skin | Same disease appears | Psoriasis, LP, Vitiligo |
| Pseudo-KP | Trauma inoculates pathogen | New infection/implanted lesion | Warts, molluscum |
| Reverse KP | Trauma to diseased skin | Lesion clears | Vitiligo |
| Pathergy | Minimal trauma (needle prick) | Pustule/papule in 24–48h | Behçet, Pyoderma gangrenosum |
| Isotopic response | Previous disease (now healed) | New different disease at same site | Post-zoster granuloma annulare |
| Renbok phenomenon | Presence of one skin disease | Second disease excluded from that site | Psoriasis + alopecia areata |
Clinical importance: Recognizing KP has diagnostic value (e.g., linear lichen planus along a scratch almost confirms the diagnosis) and therapeutic implications (patients with active psoriasis or pyoderma gangrenosum should avoid unnecessary skin trauma, injections, or surgery whenever possible).
This is a shared conversation. Sign in to Orris to start your own chat.