Zn staining full details for md exams 15marks
Reading File
search_medical_text
Ziehl-Neelsen ZN staining technique procedure principle acid-fast bacilli
search_medical_text
acid fast staining mycobacterium tuberculosis grading reporting results
search_medical_image
Ziehl-Neelsen staining acid fast bacilli microscopy
GradeResponse
GradeResponse
GradeResponse
Here is a comprehensive, exam-ready answer on Ziehl-Neelsen (ZN) Staining for MD examinations.
Ziehl-Neelsen (ZN) Staining — Complete Guide (15 Marks)
1. Introduction & Historical Background
Ziehl-Neelsen staining, also called acid-fast staining or carbol fuchsin staining, is a differential bacteriological stain used to identify acid-fast organisms — primarily Mycobacterium tuberculosis and other mycobacteria.
- Franz Ziehl (1882): introduced carbolic acid (phenol) as a mordant
- Friedrich Neelsen (1883): modified the technique using carbol fuchsin
2. Principle
The principle is based on the unique cell wall composition of mycobacteria:
- The mycobacterial cell wall contains mycolic acids — long-chain, cross-linked fatty acids — along with arabinogalactan and peptidoglycan
- These wax-like lipids make the wall highly hydrophobic and impermeable to ordinary stains
- When carbol fuchsin (a phenol-based dye) is applied with heat, it penetrates the waxy wall and binds to the mycolic acids
- On subsequent decolorization with 20% H₂SO₄ + 95% alcohol (acid-alcohol), ordinary bacteria lose the stain — but mycobacteria resist decolorization → hence the term "acid-fast"
- Counterstain (methylene blue or malachite green) colors background organisms blue/green, leaving AFB bright red/pink
According to Harrison's Principles of Internal Medicine (21st Edition, p. 5105): "Once stained, the bacilli cannot be decolorized by acid alcohol; this characteristic justifies their classification as acid-fast bacilli (AFB). Acid fastness is due mainly to the organisms' high content of mycolic acids, long-chain cross-linked fatty acids, and other cell-wall lipids."
3. Reagents Required
| Reagent | Composition | Purpose |
|---|---|---|
| Carbol fuchsin | Basic fuchsin + 5% phenol in 95% alcohol | Primary stain |
| Decolorizer | 3% HCl in 95% ethanol (acid-alcohol) or 20% H₂SO₄ | Removes stain from non-AFB |
| Counterstain | 0.3% Methylene blue (or Malachite green) | Colors background |
4. Types of ZN Staining
A. Hot ZN Stain (Classical Method)
Used for Mycobacterium tuberculosis and M. leprae
- Uses heat to drive carbol fuchsin into the waxy wall
- Decolorizer: 3% acid-alcohol
B. Cold ZN Stain (Modified — Kinyoun Method)
- No heat required
- Uses higher concentration of phenol (8%) to facilitate dye penetration
- Used when a heat source is unavailable
C. Modified ZN Stain (Weak Acid-Fast Staining)
- Decolorizer: 1% H₂SO₄ (weak acid) instead of acid-alcohol
- Used for partially acid-fast organisms: Nocardia, Cryptosporidium, Isospora, Cyclospora
- M. leprae also uses weak decolorization for better results
5. Procedure (Step-by-Step)
| Step | Action | Time |
|---|---|---|
| 1 | Prepare thin smear on clean glass slide, air dry, heat fix | — |
| 2 | Flood slide with carbol fuchsin, heat gently (steaming, not boiling) | 3–5 min |
| 3 | Allow to cool, wash with tap water | — |
| 4 | Decolorize with acid-alcohol (3% HCl in 95% ethanol) | 2–3 min |
| 5 | Wash with tap water | — |
| 6 | Counterstain with Loeffler's methylene blue | 1–2 min |
| 7 | Wash, blot dry, examine under oil immersion (100×) | — |
Key tip: Heat should cause steaming but not boiling — boiling destroys morphology.
6. Result / Appearance
| Structure | Appearance |
|---|---|
| Acid-fast bacilli (AFB) | Bright red/pink, rod-shaped, may be beaded |
| Non-acid-fast bacteria | Blue (counterstained) |
| Background / cells | Blue |
| M. tuberculosis morphology | Slender rods, 0.5 × 3 µm, may appear beaded |
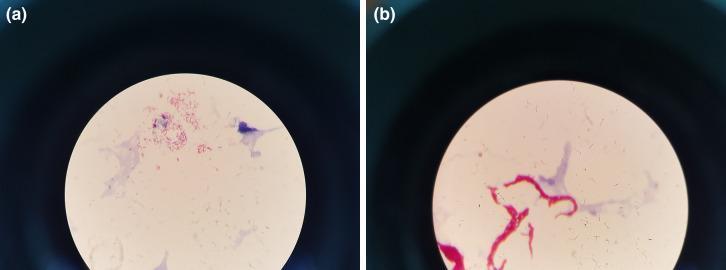
7. Grading of ZN Smear (WHO/RNTCP Grading)
| Grade | AFB Count per Field | Report |
|---|---|---|
| Negative (−) | No AFB in 100 fields | Negative |
| Scanty | 1–9 AFB per 100 fields | Report actual number |
| 1+ | 10–99 AFB per 100 fields | 1+ |
| 2+ | 1–10 AFB per field in 50 fields | 2+ |
| 3+ | >10 AFB per field in 20 fields | 3+ |
Minimum fields to examine: 100 fields before reporting negative.
8. Organisms Identified by ZN Staining
Strongly Acid-Fast (Classic ZN)
- Mycobacterium tuberculosis
- M. bovis
- M. leprae
- Non-tuberculous mycobacteria (NTM): M. avium, M. kansasii, M. fortuitum
Weakly/Partially Acid-Fast (Modified ZN)
- Nocardia spp.
- Cryptosporidium parvum (oocysts)
- Isospora belli (oocysts)
- Cyclospora cayetanensis
Not Acid-Fast
- All other routine bacteria (Gram-positive and Gram-negative)
9. Sensitivity & Limitations
| Parameter | Details |
|---|---|
| Sensitivity | ~40–60% (requires ≥5,000–10,000 bacilli/mL) |
| Specificity | ~99% |
| Minimum bacilli needed | 10,000/mL for smear positivity |
| False positive | Contamination with non-pathogenic AFB |
| False negative | Paucibacillary disease, poor sample quality |
10. Comparison: ZN vs Auramine-Rhodamine (Fluorescence) Staining
| Feature | ZN Stain | Auramine-Rhodamine |
|---|---|---|
| Microscope | Light microscope (oil immersion) | Fluorescence microscope |
| AFB appearance | Bright red on blue | Bright yellow-green on dark |
| Screening speed | Slow (100× oil immersion) | Fast (25× or 40×) |
| Sensitivity | Lower | Higher (~10% more) |
| Cost | Low | Higher |
| Confirmatory role | Gold standard for confirmation | Used for screening |
11. Uses / Applications
- Diagnosis of pulmonary tuberculosis — sputum smear microscopy (cornerstone of TB diagnosis in resource-limited settings)
- Monitoring treatment response in TB — serial smears
- Diagnosis of cutaneous/systemic mycobacteriosis
- Diagnosis of leprosy — slit-skin smear using modified ZN (cold method)
- Diagnosis of opportunistic infections — Cryptosporidium, Isospora in HIV patients
- Histopathology — ZN stain on tissue sections (Bailey & Love, p. 210: "demonstrates acid-fast bacilli, particularly mycobacteria, by staining them bright red on a blue background")
12. Specimen Types
- Sputum (most common) — early morning sample preferred
- Bronchoalveolar lavage (BAL)
- Gastric lavage (children, unable to expectorate)
- Urine, CSF, pleural fluid
- Pus from abscess
- Tissue biopsy sections
- Slit-skin smear (leprosy)
13. Quality Control Points
- Slide must be grease-free
- Smear should be thin and uniform
- Heat during staining = steaming, not boiling
- Decolorization is the critical step — over-decolorization causes false negatives
- Minimum 100 oil-immersion fields must be examined before reporting negative
- Positive and negative controls must be run with each batch
14. Exam High-Yield Points (Quick Recall)
| Question | Answer |
|---|---|
| Basis of acid-fastness | Mycolic acids in the cell wall |
| Primary stain | Carbol fuchsin |
| Decolorizer | 3% acid-alcohol (HCl + ethanol) |
| Counterstain | Methylene blue |
| AFB color | Bright red/pink on blue background |
| Modified ZN decolorizer | 1% H₂SO₄ (for Nocardia, Cryptosporidium) |
| Sensitivity | 10,000 bacilli/mL needed |
| WHO scanty grade | 1–9 AFB per 100 fields |
| Kinyoun method | Cold ZN — no heat required |
| Most sensitive stain | Auramine-rhodamine (fluorescence) |
Summary
Ziehl-Neelsen staining remains the most widely used, cost-effective method for diagnosing tuberculosis and other mycobacterial diseases. Its principle rests on the resistance of mycolic acid-rich mycobacterial cell walls to decolorization by acid-alcohol after staining with hot carbol fuchsin. Despite lower sensitivity than culture or molecular methods, its simplicity and specificity make it irreplaceable in clinical microbiology, particularly in high-burden TB settings.
This is a shared conversation. Sign in to Orris to start your own chat.