Thoracentesis
Reading File
search_medical_text
thoracentesis indications contraindications technique procedure
search_medical_text
thoracentesis complications pleural effusion fluid analysis Light criteria
search_medical_image
thoracentesis procedure technique pleural effusion
GradeResponse
GradeResponse
GradeResponse
Thoracentesis
Overview
Thoracentesis (also called pleurocentesis) is the percutaneous aspiration of fluid from the pleural space. It can be performed for diagnostic purposes (to characterize a pleural effusion) or therapeutic purposes (to relieve dyspnea). The current standard of care mandates ultrasound guidance at the point of care to locate the optimal puncture site, reduce "dry taps," and minimize complications such as pneumothorax (Harrison's, p. 7875).
Indications
| Purpose | Details |
|---|---|
| Diagnostic | New unilateral or bilateral pleural effusion of unknown cause; exudate vs. transudate differentiation |
| Therapeutic | Symptomatic relief of dyspnea from large effusions; empyema drainage |
| Combined | Most clinical scenarios involve both goals simultaneously |
Contraindications
| Absolute | Relative |
|---|---|
| No safe access window (even under ultrasound) | Coagulopathy / anticoagulation (correct INR >1.5–2.0 if possible) |
| Uncooperative patient | Thrombocytopenia (platelets <50,000) |
| — | Mechanical ventilation (higher pneumothorax risk) |
| — | Small effusion (<1 cm on ultrasound) |
| — | Overlying skin infection at puncture site |
There is no absolute platelet or INR threshold that mandates correction prior to ultrasound-guided thoracentesis in most guidelines; clinical judgment applies.
Technique
Patient Positioning
- Preferred: seated upright, leaning forward over a bedside table (gravity pools fluid inferiorly)
- Alternative: lateral decubitus (ipsilateral side down) for bedbound patients
Ultrasound Guidance
- Use a low-frequency convex (curvilinear) probe
- Identify the effusion, diaphragm, lung, and rib shadows
- Mark the optimal entry point: one interspace below the upper fluid level, above the rib (to avoid the neurovascular bundle running below each rib)
Needle Insertion
- Prep and drape the site sterilely
- Infiltrate skin and periosteum with local anesthetic (1% lidocaine)
- Advance the thoracentesis needle (or catheter-over-needle) while aspirating, entering over the superior border of the lower rib
- Confirm free flow of fluid; connect to a stopcock/syringe or drainage system
- Withdraw no more than 1–1.5 L per session to reduce re-expansion pulmonary edema risk
Ultrasound-Guided Procedure (Image)
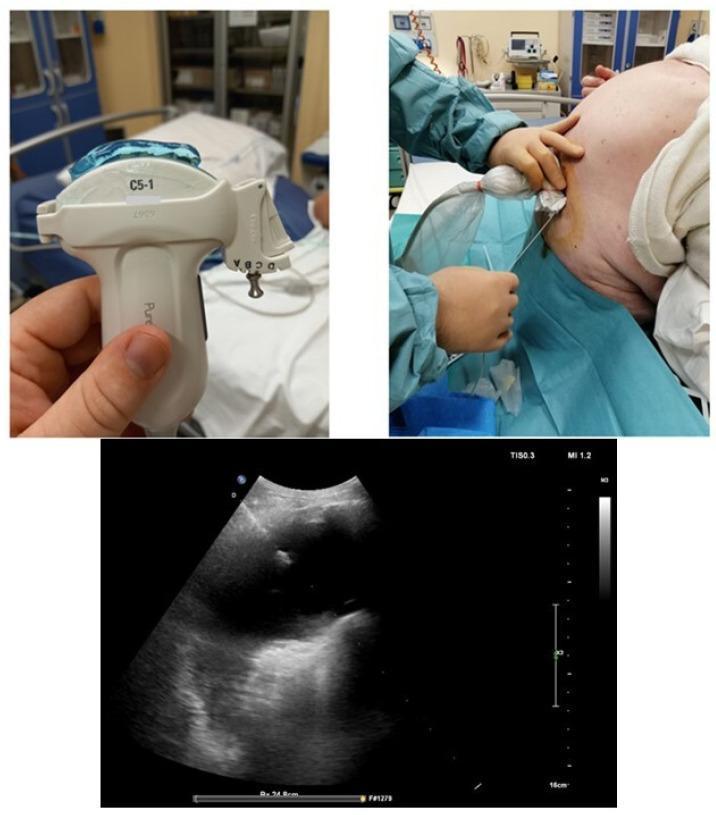
Composite image showing equipment, patient positioning (lateral decubitus with sterile drape), and the corresponding ultrasound view. The anechoic (black) pleural effusion sits above the hyperechoic diaphragm; the needle trajectory is visualized in real time to a depth of ~16 cm.
Pleural Fluid Analysis
Light's Criteria (1972)
An effusion is an exudate if any one of the following is met:
| Criterion | Threshold |
|---|---|
| Pleural fluid protein / serum protein | > 0.5 |
| Pleural fluid LDH / serum LDH | > 0.6 |
| Pleural fluid LDH | > 2/3 upper limit of normal serum LDH |
If none are met → transudate (most commonly heart failure, cirrhosis, nephrotic syndrome).
Standard Studies to Send
| Category | Tests |
|---|---|
| Biochemical | Protein, LDH, glucose, pH, amylase |
| Hematologic | Cell count with differential, hematocrit |
| Microbiologic | Gram stain, culture (aerobic/anaerobic), AFB if TB suspected |
| Cytologic | Malignant cells |
| Special | Mesothelin (mesothelioma), ADA (TB), triglycerides (chylothorax), cholesterol |
Fluid Appearance Clues
| Appearance | Suggests |
|---|---|
| Straw-colored | Transudate or simple exudate |
| Bloody / hemorrhagic | Malignancy, trauma, PE |
| Turbid / purulent | Empyema |
| Milky | Chylothorax |
| Black | Aspergillus infection (rare) |
Complications
| Complication | Frequency | Notes |
|---|---|---|
| Pneumothorax | ~3–5% (lower with ultrasound guidance) | Most are small and self-limiting |
| Dry tap | Rare with ultrasound | Usually loculated effusion |
| Re-expansion pulmonary edema | <1% | Risk increases >1.5 L drained |
| Hemothorax | Rare | Intercostal artery injury |
| Infection / empyema | Very rare | Maintain strict sterile technique |
| Vasovagal reaction | ~5% | Pretreat with atropine if high risk |
| Splenic/hepatic laceration | Very rare | Ultrasound guidance virtually eliminates this |
Post-Procedure
- Chest X-ray is no longer routinely required after ultrasound-guided thoracentesis in asymptomatic patients (per multiple guidelines), but should be obtained if:
- Air was aspirated
- Multiple needle passes were needed
- Patient develops new symptoms (cough, dyspnea, chest pain)
- Monitor oxygen saturation for 1–2 hours
- Document volume and appearance of fluid removed
Key Points
- Always use ultrasound guidance — reduces complications significantly
- Insert needle above the rib to avoid the neurovascular bundle
- Limit drainage to ≤1.5 L per session
- Light's criteria remain the cornerstone of exudate/transudate differentiation (Harrison's, p. 7875)
- A post-procedure CXR is not mandatory in asymptomatic patients after ultrasound-guided procedures
This is a shared conversation. Sign in to Orris to start your own chat.