Thoracentesis
Reading File
search_medical_text
thoracentesis indications contraindications technique procedure
search_medical_text
pleural fluid analysis Light's criteria exudate transudate
search_medical_image
thoracentesis procedure technique pleural effusion
GradeResponse
GradeResponse
GradeResponse
Here is a comprehensive overview of thoracentesis:
Thoracentesis
Definition
Thoracentesis is the percutaneous insertion of a needle or catheter into the pleural space to aspirate fluid (or occasionally air). It serves both diagnostic and therapeutic purposes.
Indications
| Purpose | Examples |
|---|---|
| Diagnostic | New pleural effusion of unknown cause; suspected empyema, malignancy, or TB |
| Therapeutic | Symptomatic relief of large effusion causing dyspnea; drainage of empyema |
Contraindications
| Absolute | Relative |
|---|---|
| No safe access site | Coagulopathy (INR >1.5–2.0) / thrombocytopenia (<50,000) |
| — | Anticoagulation therapy |
| — | Small effusion (<1 cm on lateral decubitus / ultrasound) |
| — | Mechanical ventilation (increased pneumothorax risk) |
| — | Uncooperative patient |
There is no absolute INR threshold that precludes thoracentesis; risk-benefit assessment guides each case.
Technique
Patient Positioning
- Seated upright, leaning forward over a pillow or bedside table (arms resting forward).
- Alternatively lateral decubitus for bedridden patients.
Landmark vs. Ultrasound-Guided
- Ultrasound guidance is strongly preferred and has largely replaced landmark-based and lateral decubitus X-ray approaches. It reduces complications (pneumothorax, dry taps) and improves safety.
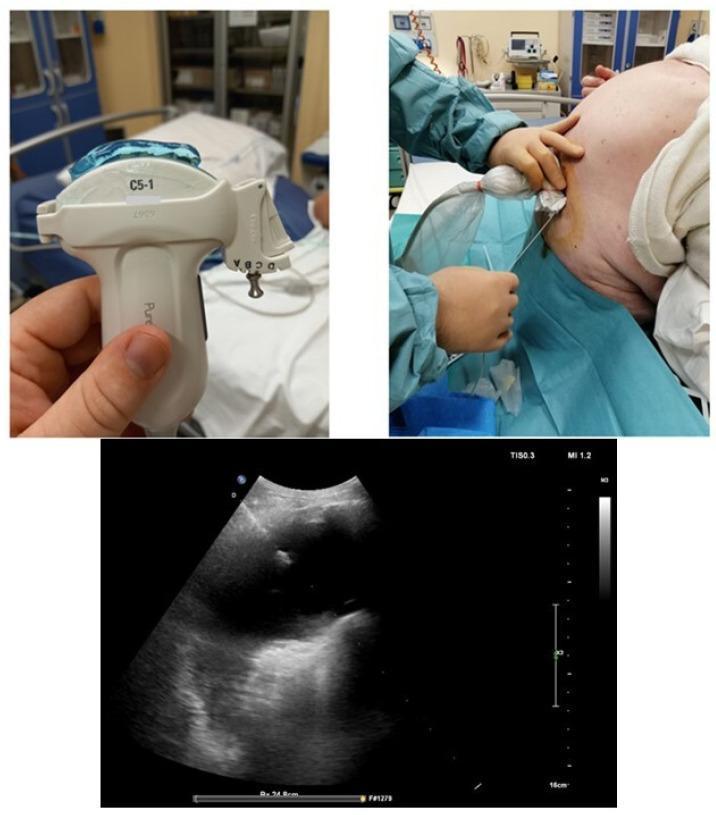
Needle Entry
- Insert just above the rib (to avoid the neurovascular bundle running below each rib).
- Common sites: posterior or posterolateral chest wall, typically at the 7th–9th intercostal space, mid-scapular to posterior axillary line.
- Confirm fluid with ultrasound before needle insertion.
Procedure Steps
- Prep and drape in sterile fashion.
- Infiltrate skin and periosteum with local anesthetic (1% lidocaine).
- Advance needle/catheter with continuous aspiration; entry into pleural space confirmed by free flow of fluid.
- Attach syringe or drainage system; aspirate required volume.
- Remove needle; apply dressing; post-procedure chest X-ray (or ultrasound) to rule out pneumothorax.
Volume Limits
- Diagnostic: 50–100 mL is sufficient.
- Therapeutic: Up to 1,500 mL per session is generally safe. Draining >1,500 mL risks re-expansion pulmonary edema.
Pleural Fluid Analysis
Step 1: Transudate vs. Exudate — Light's Criteria
A fluid is an exudate if it meets ≥1 of the following (Harrison's, p. 8084):
| Criterion | Exudate |
|---|---|
| Pleural fluid protein / serum protein | >0.5 |
| Pleural fluid LDH / serum LDH | >0.6 |
| Pleural fluid LDH | >2/3 upper limit of normal serum LDH |
If none are met → transudate.
Common Causes
| Transudate | Exudate |
|---|---|
| Left ventricular failure (most common in US) | Parapneumonic effusion / empyema |
| Cirrhosis (hepatic hydrothorax) | Malignancy |
| Nephrotic syndrome | Tuberculosis |
| Hypoalbuminemia | Pulmonary embolism |
| Constrictive pericarditis | Rheumatoid / autoimmune |
Step 2: Additional Studies (for Exudates)
| Test | Interpretation |
|---|---|
| Cell count & differential | Neutrophils ↑ → parapneumonic; lymphocytes ↑ → TB, malignancy |
| Glucose | <60 mg/dL → empyema, rheumatoid, malignancy |
| pH | <7.2 → complicated parapneumonic (needs drainage) |
| Amylase | ↑ → esophageal rupture, pancreatitis |
| Triglycerides | >110 mg/dL → chylothorax |
| Cytology | Malignant cells |
| Culture & Gram stain | Infectious etiology |
| ADA (adenosine deaminase) | ↑ → TB (especially in high-prevalence settings) |
| Hematocrit | Hct fluid/Hct blood >0.5 → hemothorax |
Complications
| Complication | Notes |
|---|---|
| Pneumothorax | Most common (~6% without US, ~1% with US guidance) |
| Bleeding / hemothorax | Intercostal vessel laceration |
| Re-expansion pulmonary edema | Risk with large-volume drainage >1,500 mL |
| Infection / empyema | Poor sterile technique |
| Vasovagal reaction | Common; manage with positioning + IV fluids |
| Liver/spleen laceration | Incorrect needle position; prevented by US guidance |
| Subcutaneous emphysema | Rare |
Post-Procedure
- Chest X-ray or point-of-care ultrasound to exclude pneumothorax.
- If the patient is asymptomatic and a small pneumothorax is detected, observation is often appropriate.
- Symptomatic or large pneumothorax → chest tube.
Key takeaway: Ultrasound guidance is the current standard of care for thoracentesis, significantly reducing complication rates. Light's criteria remain the cornerstone of pleural fluid classification, directing subsequent workup and management.
This is a shared conversation. Sign in to Orris to start your own chat.