post traumatic osteoarthritis of hip
Reading File
search_medical_text
post-traumatic osteoarthritis hip pathophysiology etiology clinical features
search_medical_text
post-traumatic hip osteoarthritis diagnosis management treatment
search_medical_image
post-traumatic osteoarthritis hip X-ray radiograph
GradeResponse
GradeResponse
GradeResponse
Post-Traumatic Osteoarthritis of the Hip
Post-traumatic osteoarthritis (PTOA) of the hip is a secondary form of osteoarthritis that develops following direct joint injury, accounting for approximately 12% of all symptomatic OA cases. Unlike primary OA, it affects younger, more active individuals and is directly attributable to a preceding traumatic event.
Etiology & Common Precipitating Injuries
| Injury Type | Mechanism of PTOA |
|---|---|
| Acetabular fractures | Articular incongruity, avascular necrosis of femoral head |
| Femoral head/neck fractures | Disruption of blood supply → AVN; malunion → altered mechanics |
| Hip dislocation | Cartilage impact loading, capsular/labral disruption, AVN |
| Proximal femur fractures | Post-surgical malunion, altered joint biomechanics |
| Retained intra-articular fragments | Direct mechanical destruction (e.g., ballistic injury) |
| Labral tears | Loss of hip joint sealing, abnormal contact pressures |
Acetabular fractures carry the highest risk — PTOA develops in 20–60% of cases depending on fracture type, degree of displacement, and quality of reduction.
Pathophysiology
Following trauma, a cascade of events drives joint degeneration:
- Acute phase: Impact loading causes chondrocyte death, matrix disruption, and release of pro-inflammatory cytokines (IL-1β, TNF-α, IL-6) into the joint space.
- Subacute phase: Synovitis, hemarthrosis, and reactive oxygen species amplify cartilage catabolism.
- Chronic phase: Progressive loss of articular cartilage, subchondral bone changes (sclerosis, cyst formation), osteophyte formation, and joint space narrowing.
- Mechanical factors: Post-traumatic malalignment and joint incongruity create focal areas of elevated contact stress, accelerating wear even in the absence of ongoing inflammation.
AVN of the femoral head is a critical intermediate step in many cases, particularly after femoral neck fractures and hip dislocations with disruption of the medial femoral circumflex artery.
Clinical Features
Symptoms:
- Groin/anterior hip pain, often radiating to the thigh or buttock
- Pain with weight-bearing, prolonged standing, stairs
- Morning stiffness (<30 minutes, distinguishing from inflammatory arthritis)
- Reduced range of motion — particularly internal rotation and abduction
- Antalgic gait (Trendelenburg sign in advanced disease)
- Functional limitation (difficulty with shoes/socks, cutting toenails)
History clues:
- Prior hip fracture, dislocation, or acetabular surgery
- Latency period: PTOA may develop months to decades after the original injury (average 2–5 years for high-energy trauma; up to 20+ years for labral injuries)
Diagnosis
Clinical Criteria
Diagnosis is primarily clinical + radiographic. The ACR criteria for hip OA require hip pain plus at least 2 of:
- ESR < 20 mm/hr
- Radiographic femoral or acetabular osteophytes
- Radiographic joint space narrowing
Radiographic Evaluation (Weight-Bearing Plain Films)
The cornerstone of diagnosis is weight-bearing AP pelvis and lateral hip radiographs.
Key radiographic findings (Kellgren-Lawrence grading):
| Grade | Findings |
|---|---|
| 0 | Normal |
| 1 | Doubtful narrowing, possible osteophytes |
| 2 | Definite osteophytes, possible narrowing |
| 3 | Multiple osteophytes, definite narrowing, sclerosis |
| 4 | Large osteophytes, marked narrowing, severe sclerosis, possible bony deformity |
The image below shows a lateral hip radiograph demonstrating classic features of post-traumatic OA following a ballistic injury, with a retained intra-articular fragment:
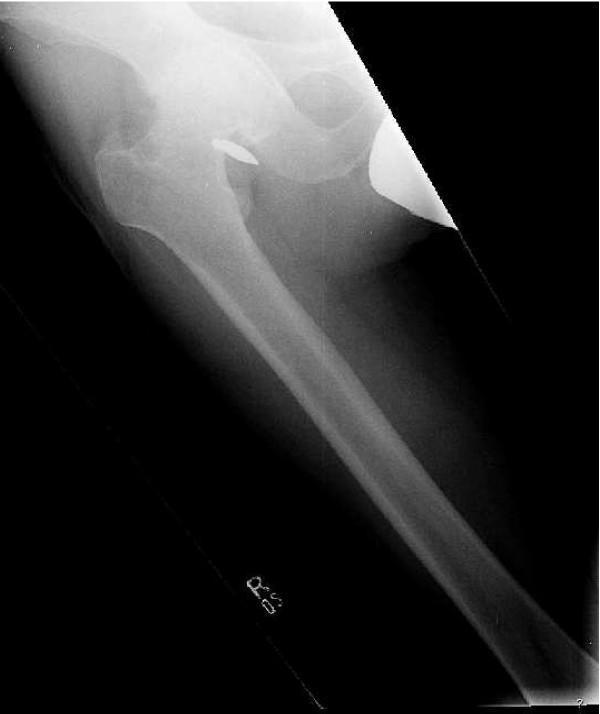
Lateral hip radiograph: severe PTOA with marked joint space narrowing, subchondral sclerosis, femoral head flattening/loss of sphericity, marginal osteophytes, cortical irregularities, and a radiopaque intra-articular fragment. (Source: PMC Clinical VQA)
MRI: Useful for early cartilage loss, AVN staging, labral pathology, bone marrow edema — particularly when X-rays are normal but symptoms are significant.
CT: Best for assessing residual fracture deformity, malunion, acetabular incongruity, and pre-surgical planning.
Differential Diagnosis
- Primary (idiopathic) OA
- Avascular necrosis (can coexist)
- Inflammatory arthritis (RA, seronegative spondyloarthropathy)
- Septic arthritis
- Pigmented villonodular synovitis (PVNS)
- Stress fracture
- Referred pain (lumbar spine, sacroiliac joint)
Management
Per the VA/DoD Clinical Practice Guideline for Non-Surgical Management of Hip & Knee Osteoarthritis, management follows a stepwise, individualized approach:
Step 1 — Core Non-Surgical Management (All Patients)
- Education and self-management: Weight loss (if BMI >25), activity modification, joint protection strategies
- Exercise: Aerobic (aquatic, cycling) and strengthening exercises — strongest evidence for symptom reduction
- Physical therapy: Gait training, ROM exercises, hip strengthening (abductors, extensors)
- Weight management: Each pound lost reduces hip joint load by 3–6 lbs
Step 2 — Pharmacotherapy
| Agent | Notes |
|---|---|
| Topical NSAIDs (diclofenac gel) | First-line, especially in elderly or those with GI risk |
| Oral NSAIDs/COX-2 inhibitors | Effective; use lowest effective dose; consider GI/CV/renal risk |
| Acetaminophen | Modest efficacy; useful for mild pain or NSAID contraindication |
| Duloxetine | Consider for chronic pain with central sensitization |
| Intra-articular corticosteroids | Short-term relief (4–8 weeks); limit to 3–4/year |
| Intra-articular hyaluronic acid | Controversial; not recommended by all guidelines |
| Opioids | Reserved for refractory cases; risk/benefit carefully weighed |
Step 3 — Interventional/Surgical Options
When conservative management fails (typically after 3–6 months of optimized non-surgical care), obtain weight-bearing plain radiographs and refer for surgical consultation.
| Procedure | Indication |
|---|---|
| Total hip arthroplasty (THA) | Gold standard for advanced PTOA; excellent outcomes; most common surgical intervention |
| Periacetabular osteotomy (PAO) | Young patients with residual acetabular dysplasia/malunion without advanced OA |
| Femoral osteotomy | Proximal femur malunion with focal OA |
| Hip arthroscopy | Early PTOA with labral tear, loose bodies, femoroacetabular impingement (FAI) |
| Hip resurfacing | Selected young, active patients with preserved femoral head stock |
THA outcomes in PTOA vs. primary OA: Generally good, but technically more challenging due to prior hardware, scarring, altered anatomy, and bone defects. Infection rates and revision rates are somewhat higher than primary OA THA.
Prognosis & Special Considerations
- Young patients (<50 years) pose the greatest management challenge — THA implants have a limited lifespan (~15–20 years), meaning revision surgery is likely.
- Timing of surgery: Early anatomic reduction of acetabular fractures significantly reduces PTOA risk. Quality of reduction is the single most important modifiable risk factor.
- Avascular necrosis: If present, core decompression or vascularized fibular grafting may be considered prior to THA in appropriate candidates.
- Military/high-energy trauma population: Often younger, with complex injury patterns, retained hardware, and higher functional demands — multidisciplinary planning is essential.
Sources: VA/DoD Clinical Practice Guideline for Non-Surgical Management of Hip & Knee Osteoarthritis (pp. 1, 110); PMC Clinical VQA Dataset (radiographic example).
This is a shared conversation. Sign in to Orris to start your own chat.