Premature birth
Reading File
search_medical_text
premature birth preterm labor definition causes risk factors
search_medical_text
preterm infant complications management neonatal care
search_medical_image
preterm infant premature baby neonatal
GradeResponse
GradeResponse
GradeResponse
Premature Birth (Preterm Birth)
Definition
Premature (preterm) birth is defined as delivery before 37 completed weeks of gestation. It affects nearly 1 in 10 newborns worldwide and is a major cause of perinatal morbidity and mortality (Management of Pregnancy, p. 82).
Classification by Gestational Age
| Category | Gestational Age |
|---|---|
| Extremely preterm | < 28 weeks |
| Very preterm | 28–31 weeks |
| Moderate preterm | 32–33 weeks |
| Late preterm | 34–36 weeks |
Causes & Risk Factors
About 50% of preterm births are related to spontaneous preterm labor; the rest result from medically indicated early delivery or premature rupture of membranes (PROM).
Strongest predictors:
- Prior history of spontaneous preterm birth (single strongest risk factor)
- Prior preterm pre-labor rupture of membranes (PPROM)
- Multiple gestation (twins, triplets, etc.)
- Short cervical length (< 25 mm on ultrasound)
Other risk factors:
- Uterine/cervical anomalies
- Infections (chorioamnionitis, bacterial vaginosis, UTI)
- Placenta previa or placental abruption
- Polyhydramnios
- Maternal age extremes (< 17 or > 35)
- Low socioeconomic status, smoking, substance use
- Psychological distress / chronic stress
- Inadequate prenatal care
Preterm Infant: NICU Care
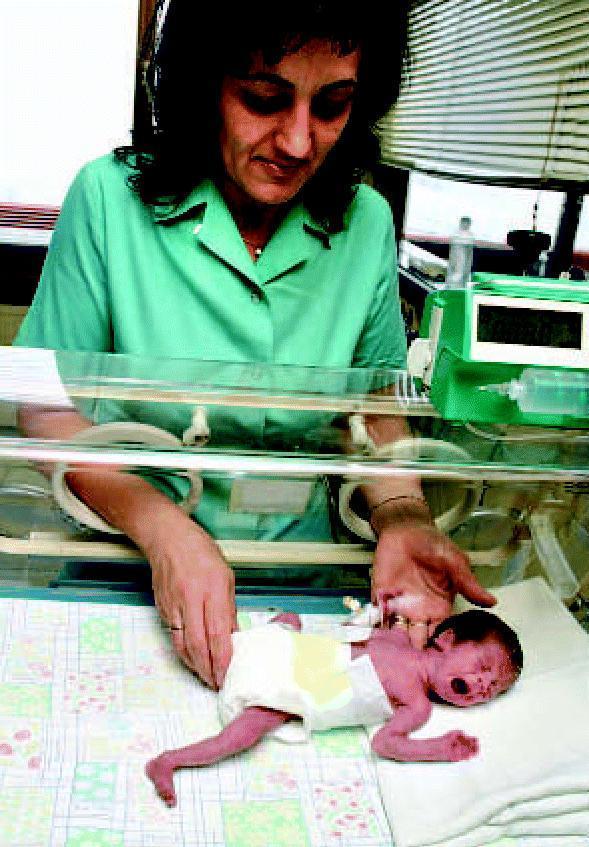
Premature infants are cared for in the Neonatal Intensive Care Unit (NICU) in isolettes (incubators) that provide:
- Thermoregulation (preterm infants cannot maintain body temperature)
- Precise IV fluid/medication delivery via infusion pumps
- Continuous cardiorespiratory monitoring
- Umbilical catheters for vascular access
Complications of Prematurity
Complications vary significantly by degree of prematurity:
Respiratory
- Respiratory Distress Syndrome (RDS) — surfactant deficiency; most common cause of early death
- Bronchopulmonary dysplasia (BPD) / chronic lung disease
- Apnea of prematurity
Neurological
- Intraventricular hemorrhage (IVH)
- Periventricular leukomalacia (PVL)
- Long-term risk of cerebral palsy, cognitive delays
Cardiovascular
- Patent ductus arteriosus (PDA)
- Hypotension
Gastrointestinal
- Necrotizing enterocolitis (NEC) — serious bowel inflammation/necrosis
- Feeding intolerance, poor sucking reflex
Infectious
- Sepsis (common pathogens: CoNS, E. coli, Group B Streptococcus, Candida spp.)
- Higher susceptibility due to immature immune system
Metabolic
- Hypoglycemia, hypocalcemia
- Jaundice (hyperbilirubinemia)
Ophthalmologic
- Retinopathy of prematurity (ROP)
Prevention
Risk assessment should occur at the first prenatal visit for all patients (Management of Pregnancy, p. 82).
| Intervention | Indication |
|---|---|
| Vaginal progesterone | Short cervix (< 25 mm) on mid-trimester ultrasound |
| 17-hydroxyprogesterone caproate (17-OHPC) | History of prior spontaneous preterm birth (singleton pregnancy) |
| Cervical cerclage | Cervical insufficiency + prior preterm birth or short cervix |
| Antenatal corticosteroids (betamethasone) | 24–34 weeks at risk of delivery within 7 days — accelerates fetal lung maturation |
| Magnesium sulfate | < 32 weeks — neuroprotection against cerebral palsy |
| Antibiotics | GBS prophylaxis in labor; treat infections promptly |
Management of Preterm Labor
- Tocolytics — delay delivery to allow corticosteroid administration (e.g., nifedipine, indomethacin, atosiban); not for long-term use
- Antenatal corticosteroids — most important intervention (betamethasone IM × 2 doses)
- Antibiotics — for PPROM to prolong latency and reduce neonatal infection
- Delivery planning — at an appropriate-level facility with NICU capability
- Mental health support — women with high-risk status should be offered mental health treatment (Management of Pregnancy, p. 82)
Prognosis
Outcomes improve significantly with each additional week of gestation:
- < 23 weeks: survival rare; outcomes very poor
- 23–24 weeks: survival ~50%; high morbidity
- 28–31 weeks: ~90%+ survival with NICU care
- 34–36 weeks (late preterm): generally good outcomes but higher risk than term for respiratory issues, feeding problems, and readmission
The syndrome of intrauterine development of foetus
search_medical_text
intrauterine fetal development syndrome stages growth
search_medical_text
fetal growth restriction intrauterine growth retardation IUGR diagnosis management
search_medical_image
intrauterine fetal development growth ultrasound
GradeResponse
GradeResponse
GradeResponse
Syndrome of Intrauterine Fetal Development
This topic covers two interrelated subjects: (1) normal intrauterine fetal development — the sequential stages from conception to term — and (2) intrauterine growth restriction (IUGR) — the pathological syndrome where fetal growth deviates from expected parameters.
Part 1: Normal Intrauterine Development
Intrauterine development spans approximately 40 weeks (280 days) from the last menstrual period and is divided into three major periods:
1. Pre-embryonic Period (Weeks 1–2)
- Fertilization → zygote formation
- Cleavage, blastocyst formation, implantation into the uterine wall
- Formation of the bilaminar disc (epiblast + hypoblast)
2. Embryonic Period (Weeks 3–8)
This is the critical period of organogenesis — the embryo is most vulnerable to teratogens.
| Week | Key Developments |
|---|---|
| 3–4 | Gastrulation (trilaminar disc); neural tube formation; heart begins beating |
| 5–6 | Limb buds appear; face begins forming; liver, lungs, pancreas rudiments |
| 7–8 | Fingers/toes distinguishable; all major organs established; embryo → fetus transition |
3. Fetal Period (Weeks 9–40)
Characterized by rapid growth and maturation of established organs.
| Trimester | Weeks | Major Milestones |
|---|---|---|
| 1st | 1–13 | Organogenesis complete by week 8; sex differentiation (week 9–12); kidneys begin urine production |
| 2nd | 14–27 | Rapid growth; fetal movements felt (~18–20 wks); viability threshold (~23–24 wks); surfactant production begins (~24 wks) |
| 3rd | 28–40 | Lung maturation; brain myelination; fat deposition; CNS refinement; weight gain (~200 g/week) |
Hormonal Orchestration of Development
Fetal development is tightly regulated by an interplay of hormones. Key axes include:
- HCG — sustains corpus luteum in early pregnancy
- Placental estrogen & progesterone — maintain uterine quiescence and support organogenesis
- Fetal thyroid hormones — critical for brain and skeletal maturation
- IGF-1 and IGF-2 — primary drivers of intrauterine somatic growth
- Cortisol — surges before term; triggers lung surfactant production and organ maturation
Part 2: Intrauterine Growth Restriction (IUGR)
Definition
IUGR (also called fetal growth restriction, FGR) is a condition in which the fetus fails to achieve its genetically determined growth potential. Defined as estimated fetal weight (EFW) or abdominal circumference (AC) < 10th percentile for gestational age.
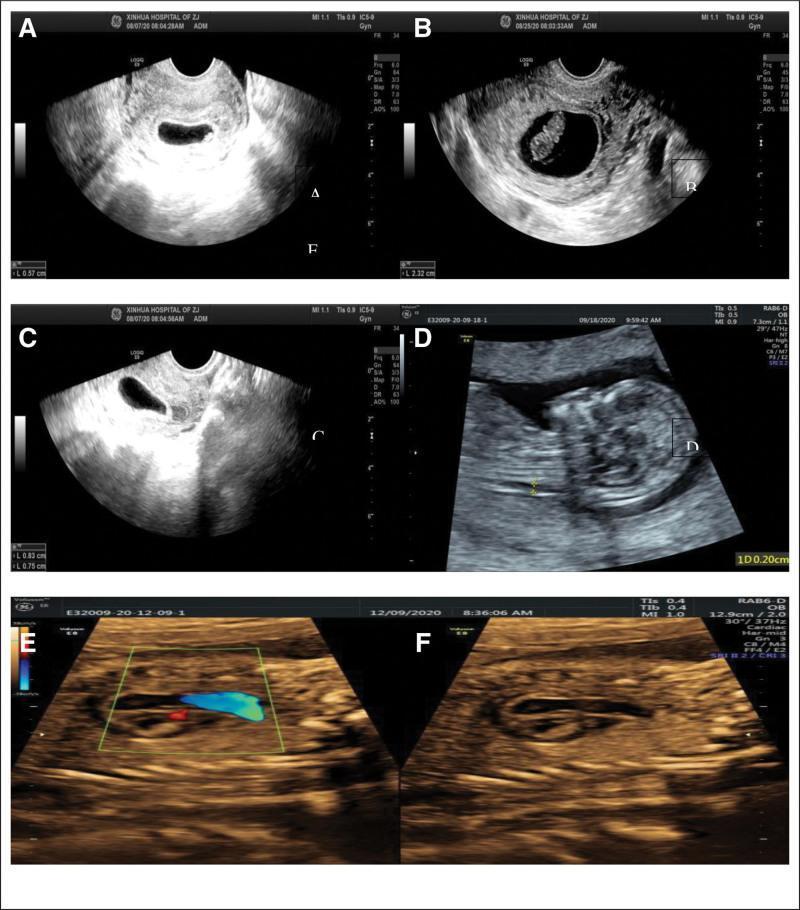
Classification
| Type | Description | Cause |
|---|---|---|
| Symmetric IUGR | All organs equally small; head circumference reduced | Early insult (chromosomal anomaly, infection); affects ~20–30% |
| Asymmetric IUGR | Head-sparing; abdomen disproportionately small | Late uteroplacental insufficiency; affects ~70–80% |
Etiology / Causes
Maternal (most common):
- Hypertensive disorders (preeclampsia, chronic hypertension)
- Diabetes mellitus with vascular disease
- Smoking, alcohol, substance abuse (cocaine, opioids)
- Malnutrition / severe anemia
- Thrombophilias (antiphospholipid syndrome)
- Chronic renal or cardiac disease
- Smoking — directly reduces fetal growth (Harrison's, p. 11110)
Placental:
- Placental insufficiency (most common cause of asymmetric IUGR)
- Placenta previa, abruption
- Umbilical cord abnormalities
Fetal:
- Chromosomal anomalies (trisomy 13, 18, 21)
- Congenital malformations
- Multiple gestation
- Congenital infections — TORCH: Toxoplasmosis, Rubella, CMV, Herpes/HIV
Diagnosis
- Accurate gestational dating — fundal height measurement (< 10th percentile for GA)
- Ultrasound biometry — key parameters:
- Abdominal circumference (AC) — most sensitive single parameter
- Estimated fetal weight (EFW)
- Head circumference (HC) and femur length (FL)
- Doppler studies — assess uteroplacental blood flow:
- Umbilical artery (UA) Doppler — absent/reversed end-diastolic flow = severe compromise
- Middle cerebral artery (MCA) — "brain-sparing" pattern
- Ductus venosus (DV) — waveform abnormalities indicate imminent fetal compromise
- Amniotic fluid assessment — oligohydramnios common in IUGR
- Biophysical profile (BPP)
- Karyotyping — if structural anomalies present
- TORCH serology
Management
| Step | Action |
|---|---|
| Identify & treat cause | Optimize maternal disease; stop smoking/substances |
| Increased surveillance | Serial growth scans every 2–4 weeks; Doppler twice weekly in severe IUGR |
| Antenatal corticosteroids | Betamethasone if preterm delivery anticipated (< 34 weeks) |
| Magnesium sulfate | Neuroprotection if delivery < 32 weeks |
| Timing of delivery | Balance risk of prematurity vs. fetal compromise (individualized) |
| Delivery | Vaginal delivery if stable; cesarean section if fetal compromise detected |
Delivery timing guidelines:
- Absent UA end-diastolic flow → deliver at 34 weeks
- Reversed UA flow / abnormal DV → deliver at 32 weeks or earlier
- Severe IUGR < 32 weeks → tertiary center with NICU
Complications
In utero:
- Fetal hypoxia and acidosis
- Stillbirth
Neonatal:
- Hypoglycemia, hypothermia, polycythemia
- Respiratory distress
- Necrotizing enterocolitis (NEC)
- Increased susceptibility to sepsis
Long-term (Barker Hypothesis / Developmental Origins of Health and Disease):
- Cardiovascular disease (hypertension, coronary artery disease)
- Type 2 diabetes mellitus
- Metabolic syndrome
- Neurodevelopmental delays
Prognosis
Prognosis depends on gestational age at onset, severity of growth restriction, and underlying etiology. Early-onset IUGR (< 32 weeks) carries the worst prognosis. With modern Doppler surveillance and timely delivery, perinatal mortality has been significantly reduced.
This is a shared conversation. Sign in to Orris to start your own chat.