Acute Appendicitis: (Classification. Clinical presentation, diagnosis, and management. Surgical approaches, types of anesthesia, indications for drainage and tamponade of the abdominal cavity. Complications of acute appendicitis
Reading File
search_medical_text
acute appendicitis classification clinical presentation diagnosis management
search_medical_text
appendicitis surgical approaches anesthesia drainage complications peritonitis
search_medical_image
acute appendicitis pathology imaging diagnosis
GradeResponse
GradeResponse
GradeResponse
Good results. Let me now compile a comprehensive, fully synthesized answer drawing on these sources plus my own clinical knowledge.
Acute Appendicitis
1. Classification
Acute appendicitis is classified by the degree of pathological progression:
| Grade | Stage | Pathology |
|---|---|---|
| I | Simple / Catarrhal | Mucosal inflammation, edema, hyperemia; wall intact |
| II | Phlegmonous (Suppurative) | Full-thickness transmural inflammation; fibrinous exudate on serosa |
| III | Gangrenous | Ischemic necrosis of the appendiceal wall; black/green discoloration |
| IV | Perforated | Perforation of the necrotic wall; spillage of luminal contents |
| IVa | Localized peritonitis / Periappendiceal abscess | Perforation walled off by omentum and adjacent organs |
| IVb | Diffuse (generalized) peritonitis | Free perforation into the peritoneal cavity |
2. Clinical Presentation
Symptoms
- Classic triad: periumbilical pain migrating to the right iliac fossa (RIF) over 6–12 h + nausea/vomiting + anorexia
- Pain is continuous, worsens with movement; patient prefers to lie still
- Low-grade fever (37.5–38.5 °C); high fever suggests perforation or abscess
- Nausea, vomiting, constipation (or diarrhea in pelvic appendicitis)
Physical Signs
| Sign | Description |
|---|---|
| McBurney's point tenderness | Maximum tenderness at 1/3 distance from ASIS to umbilicus |
| Rovsing's sign | Palpation of LIF causes pain in RIF (peritoneal irritation) |
| Psoas sign | Extension of right hip increases pain (retrocecal appendix) |
| Obturator sign | Internal rotation of flexed right hip causes pain (pelvic appendix) |
| Blumberg's sign | Rebound tenderness in RIF |
| Dunphy's sign | Increased pain with coughing |
| Guarding / Rigidity | Involuntary muscle defense — indicates peritoneal involvement |
Atypical Presentations
- Retrocecal appendix (~65%): vague flank/back pain, psoas sign positive
- Pelvic appendix: urinary frequency, rectal tenderness, diarrhea
- Subhepatic appendix: RUQ pain mimicking cholecystitis
- Elderly patients: blunted signs, frequently present late with perforation
- Pregnant women: appendix displaced superiorly; pain in RUQ by 3rd trimester
- Children: higher perforation rate due to diagnostic delay and thin omentum
3. Diagnosis
Scoring Systems
Alvarado Score (MANTRELS)
| Criterion | Points |
|---|---|
| Migration of pain to RIF | 1 |
| Anorexia | 1 |
| Nausea/vomiting | 1 |
| RIF tenderness | 2 |
| Rebound tenderness | 1 |
| Elevated temperature (>37.3 °C) | 1 |
| Leukocytosis (WBC >10,000) | 2 |
| Shift to left (neutrophilia) | 1 |
| Total | 10 |
- ≤4: appendicitis unlikely → observe/discharge
- 5–6: equivocal → imaging required
- 7–10: high probability → operate or confirm with CT
AIR Score and Appendicitis Inflammatory Response (AIR) score are newer alternatives used in some European guidelines.
Laboratory Findings
- Leukocytosis (WBC >10,000/µL) in ~80%; left shift (neutrophilia)
- CRP elevated (>10 mg/L) — rises later (6–12 h); combination of WBC + CRP increases sensitivity
- Urinalysis: mild pyuria/hematuria (5–25%) from ureteral proximity — does not exclude appendicitis
- Serum β-hCG in women of childbearing age (exclude ectopic pregnancy)
Imaging
According to the American College of Emergency Physicians (ACEP) Clinical Policy:
Ultrasound (US)
- First-line in children and pregnant women
- Findings: non-compressible, blind-ending tubular structure >6 mm outer diameter, absent peristalsis, periappendiceal fluid
- Sensitivity ~75–90%, specificity ~85–95%
- Operator-dependent; limited by obesity and gas
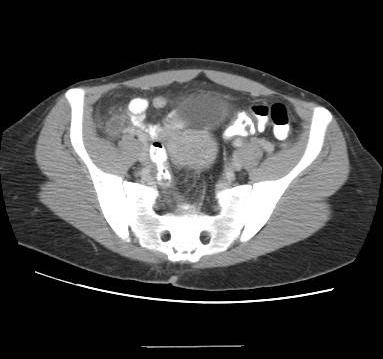
CT Abdomen/Pelvis (gold standard in adults)
- Sensitivity 94–98%, specificity 95–99%
- Findings:
- Appendiceal diameter >6 mm (thickened wall, lumen distension)
- Periappendiceal fat stranding
- Arrowhead sign (oral contrast funnel at cecal base pointing to occluded orifice)
- Appendicolith (calcified fecalith)
- Phlegmon or abscess in perforated cases
MRI
- Preferred in pregnant women when US is inconclusive
- No radiation; sensitivity and specificity comparable to CT
Per ACEP guidelines, clinical prediction rules (e.g., Alvarado) can identify low-risk patients who may not require advanced imaging, but imaging (CT or US) remains the standard for equivocal cases.
4. Management
Non-Operative (Conservative) Management
- Antibiotics-first strategy (APPAC trial, CODA trial) is a validated option for uncomplicated acute appendicitis in selected adults
- Regimen: IV piperacillin-tazobactam or IV amoxicillin-clavulanate → oral antibiotics (5–10 days)
- ~70% success at 1 year; ~30% will eventually require appendectomy
- Not recommended for: perforated appendicitis, appendicolith, high-risk patients
Operative Management (Standard of Care)
- Appendectomy remains the definitive treatment
- Pre-operative: IV fluids, broad-spectrum antibiotics (cover gram-negatives and anaerobes), analgesia, NPO
- Antibiotic prophylaxis: cefazolin + metronidazole (or piperacillin-tazobactam)
5. Surgical Approaches
Open Appendectomy (Laparotomy)
- McBurney incision: oblique incision over McBurney's point (RIF) — classic approach
- Lanz incision: transverse RIF incision — better cosmesis
- Lower midline / right paramedian incision: used when diagnosis is uncertain or diffuse peritonitis is present
Technique: exteriorize appendix → ligate mesoappendix → ligate base with purse-string suture or simple ligation → appendix excised → stump invaginated or buried.
Laparoscopic Appendectomy (Preferred in Most Centers)
Three-port technique (umbilical camera port + 2 working ports)
Advantages over open:
- Less postoperative pain
- Shorter hospital stay
- Faster return to normal activity
- Lower wound infection rate
- Better visualization for obese patients and uncertain diagnoses (Harrison's, p. 9193)
Disadvantages:
- Higher incidence of intraabdominal abscess post-perforation (some studies)
- Requires general anesthesia (cannot be done under spinal)
- Longer OR time
Single-Incision Laparoscopic Surgery (SILS) / NOTES
- Experimental/specialized centers; cosmetically superior, no clear outcomes benefit
6. Types of Anesthesia
| Anesthesia Type | Details |
|---|---|
| General anesthesia (GA) | Standard for both laparoscopic and open appendectomy; allows muscle relaxation and airway control; risk approximates 0.1–0.5% mortality (Harrison's, p. 9193) |
| Spinal (subarachnoid) anesthesia | Applicable for open appendectomy (McBurney/Lanz); level T4–T6 required; option in patients with contraindications to GA (respiratory disease, difficult airway); used in resource-limited settings |
| Epidural anesthesia | Less commonly used; can supplement GA; useful for postoperative analgesia |
| Local anesthesia | Rarely used; possible for very high-risk patients undergoing open appendectomy under specific circumstances |
Choice considerations: GA is universal for laparoscopic approach. Spinal anesthesia is a viable alternative for open appendectomy, particularly where GA carries excessive risk.
7. Indications for Drainage and Tamponade of the Abdominal Cavity
Periappendiceal Abscess
- Percutaneous CT/US-guided drainage: first-line for well-defined abscess (>3 cm)
- Followed by interval appendectomy 6–8 weeks later (though this is debated — some do not require interval appendectomy if no appendicolith)
- IV antibiotics as bridge therapy
Intraoperative Drainage Indications
- Localized peritonitis with abscess: drain placed at time of appendectomy
- Perforated appendicitis with contamination: thorough peritoneal lavage (warm saline 3–5 L), suction drainage
- Ongoing soilage / complex phlegmon: closed-suction drain (e.g., Jackson-Pratt) left in the abscess cavity
Tamponade (Gauze Packing / Omental Tamponade)
- Used when bleeding from the mesoappendix or appendiceal bed cannot be fully controlled
- Omental packing used to wall off a necrotic/phlegmonous base that cannot be safely resected (rare)
- "Damage control" approach in severely unstable patients: pack and re-look in 24–48 h
- Indications:
- Uncontrolled hemorrhage from the mesoappendix/cecal base
- Severe fecal contamination requiring staged laparotomy
- Diffuse gangrenous peritonitis with hemodynamic instability — pack, close, ICU resuscitation, re-operation
Peritoneal Lavage
- Performed in diffuse peritonitis (Grade IVb): copious irrigation with warm saline to reduce bacterial load
- Controversial in localized perforation: lavage may spread contamination
8. Complications of Acute Appendicitis
Early Complications
| Complication | Notes |
|---|---|
| Perforation | Occurs in 20–30% overall; higher in elderly and children; gangrenous wall ruptures, leading to peritonitis |
| Periappendiceal abscess | Perforation walled off by omentum; palpable RIF mass (Plastron); treated with drainage ± interval appendectomy |
| Local peritonitis | Confined to RIF; treated with appendectomy + lavage |
| Diffuse peritonitis | Free perforation; surgical emergency; high mortality |
| Sepsis / Septic shock | Systemic response to bacterial peritonitis; requires ICU management |
| Portal pylephlebitis | Septic thrombophlebitis of the portal vein; rare but life-threatening; presents with high fever, jaundice, hepatic abscesses |
Postoperative Complications
| Complication | Incidence | Management |
|---|---|---|
| Wound infection | 3–5% (simple), up to 20% (perforated) | Wound opening, antibiotics |
| Intraabdominal abscess | 2–5%; higher after laparoscopy in perforated cases | Percutaneous drainage; antibiotics |
| Ileus | Common | Conservative — NGT, mobilization |
| Stump appendicitis | Rare — inflammation of retained stump | Re-operation |
| Bowel obstruction | Adhesion formation; can occur months–years later | Conservative → surgical lysis of adhesions |
| Fecal fistula | Dehiscence of appendiceal stump | Most close spontaneously; surgical repair if persistent |
| Hemorrhage | Mesoappendix slippage | Re-operation |
Chronic / Long-term Complications
- Adhesive intestinal obstruction (small bowel obstruction from adhesions)
- Infertility in women (right-sided pelvic adhesions following perforation)
- Hernia at incision site (especially McBurney)
- Chronic right iliac fossa pain / "stump appendicitis"
Mortality
- Uncomplicated appendicitis: 0.1–0.5% (approximates the risk of general anesthesia alone)
- Perforated appendicitis: 3% overall, up to 15% in the elderly (Harrison's, p. 9193)
Summary Algorithm
Suspected Acute Appendicitis
↓
Clinical assessment + Alvarado score
↓
Score ≥7 → Operate (or CT to confirm)
Score 4–6 → CT scan
Score ≤3 → Observe / alternative diagnosis
↓
Imaging confirms appendicitis?
↓
Uncomplicated → Laparoscopic appendectomy (or antibiotics if patient chooses)
Perforated + abscess → Percutaneous drainage + interval appendectomy
Perforated + diffuse peritonitis → Emergency appendectomy + peritoneal lavage ± drain
Sources: Harrison's Principles of Internal Medicine, 21st Edition (p. 9193); ACEP Clinical Policy: Evaluation and Management of Emergency Department Patients with Suspected Appendicitis; MedPix imaging database.
This is a shared conversation. Sign in to Orris to start your own chat.