Ramsay Hunt syndrome in detail for 50 marks with diagram and flow charts from Scott Brown, Cummings, stell and marans, Zakir Hussain, dhingra, hazarika and related articles with recent advances according to rguhs university
Reading File
search_medical_text
Ramsay Hunt syndrome etiology pathophysiology herpes zoster oticus
search_medical_text
Ramsay Hunt syndrome clinical features diagnosis facial nerve palsy
search_medical_image
Ramsay Hunt syndrome vesicles ear facial nerve anatomy diagram
GradeResponse
GradeResponse
GradeResponse
search_medical_text
Ramsay Hunt syndrome treatment management antiviral steroids prognosis
search_medical_text
herpes zoster oticus facial nerve geniculate ganglion pathology ENT
Now let me synthesize a comprehensive, exam-ready 50-mark answer on Ramsay Hunt Syndrome.
RAMSAY HUNT SYNDROME
(Herpes Zoster Oticus)
50 Marks | RGUHS University ENT Examination
INTRODUCTION & HISTORICAL BACKGROUND
Ramsay Hunt Syndrome (RHS) was first described by James Ramsay Hunt in 1907, who identified a clinical triad of:
- Otalgia (severe ear pain)
- Auricular vesicles (herpetic eruption in the ear)
- Peripheral facial nerve palsy (LMN type)
It is also called "Herpes Zoster Oticus". Hunt originally classified it into four types (Hunt's Syndrome Types I–IV) based on the extent of neurological involvement.
DEFINITION
Ramsay Hunt Syndrome is a peripheral facial nerve palsy accompanied by erythematous vesicular eruption of the skin of the ear canal, auricle (herpes zoster oticus), and/or mucous membrane of the oropharynx, caused by reactivation of latent Varicella Zoster Virus (VZV) in the geniculate ganglion of the facial nerve (CN VII).
(Harrison's Principles of Internal Medicine, 21st Ed., p. 12502; Bailey & Love's 28th Ed., p. 784)
EPIDEMIOLOGY
| Parameter | Details |
|---|---|
| Incidence | 5 per 100,000 population/year |
| Age | Most common in adults >40 years; rare in children |
| Sex | Equal male:female ratio |
| Immunocompromised | HIV, malignancy, steroid therapy — significantly higher risk |
| Comparison with Bell's Palsy | Accounts for ~12–18% of all acute peripheral facial palsies |
| Bilateral involvement | Rare (<1%) |
ETIOLOGY & MICROBIOLOGY
- Causative agent: Varicella Zoster Virus (VZV) — a double-stranded DNA virus, member of Herpesviridae family
- Primary infection: Chickenpox (Varicella) — usually in childhood
- After primary infection, VZV travels retrogradely along sensory nerve fibers and establishes latency in the dorsal root ganglia and cranial nerve sensory ganglia
- Reactivation occurs when cell-mediated immunity wanes → VZV reactivates in the geniculate ganglion of CN VII
ANATOMY OF RELEVANCE
The Facial Nerve (CN VII) — Intratemporal Course
BRAINSTEM (Pontomedullary junction)
↓
Internal Auditory Canal (IAC)
↓
┌─────────────────────────┐
│ GENICULATE GANGLION │ ← Site of VZV latency & reactivation
└─────────────────────────┘
↓ (Greater Petrosal Nerve — parasympathetic to lacrimal gland)
Tympanic Segment
↓ (Nerve to Stapedius — CN VII branch)
Mastoid/Vertical Segment
↓ (Chorda Tympani — taste, submandibular/sublingual glands)
Stylomastoid Foramen
↓
Extratemporal branches (Temporal, Zygomatic, Buccal, Marginal Mandibular, Cervical)
The geniculate ganglion is the sensory ganglion of CN VII, receiving afferents from:
- External ear (concha, EAC) via auricular branch of CN X (Arnold's nerve) and auricular branch of CN V3
- Soft palate, tonsillar fossa via intermediate nerve (Nerve of Wrisberg)
This explains why RHS produces vesicles in the EAC, pinna, soft palate, and occasionally the ipsilateral anterior 2/3 of tongue.
PATHOPHYSIOLOGY
┌──────────────────────────────────────────────────────────┐
│ PRIMARY VZV INFECTION (Varicella/Chickenpox) │
└──────────────────────────────┬───────────────────────────┘
↓
Retrograde axonal transport → Latency established in
GENICULATE GANGLION (CN VII sensory ganglion)
↓
[Trigger: Immunosuppression, aging, stress, malignancy]
↓
REACTIVATION OF VZV IN GENICULATE GANGLION
↓
┌──────────────┬──────────────────┬─────────────────┐
↓ ↓ ↓ ↓
Anterograde Inflammatory Spread to Spread to
spread to edema → CN VIII pharyngeal
skin → VESICLES compression of (cochlear/ branches →
in EAC/pinna CN VII in bony vestibular) oral vesicles
fallopian canal → SNHL/Vertigo
↓
FACIAL NERVE PALSY (LMN type)
Key pathological process: Viral replication → neuronal inflammation → edema within the rigid bony fallopian canal → ischemic compression → demyelination and axonal degeneration of CN VII
HUNT'S ORIGINAL CLASSIFICATION (4 Types)
| Type | Features |
|---|---|
| Type I | Zoster oticus alone — vesicles in EAC/pinna, severe otalgia, NO facial palsy |
| Type II | Zoster oticus + Facial palsy (classic RHS) |
| Type III | Zoster oticus + Facial palsy + Audiovestibular symptoms (SNHL, vertigo) |
| Type IV | Involvement of multiple cranial nerves (V, IX, X, XI, XII) — "polyneuropathic form" |
CLINICAL FEATURES
Cardinal Triad:
- Severe Otalgia — deep-seated, boring, lancinating ear pain (often precedes vesicles by 2–3 days — "pre-eruptive stage")
- Vesicular Eruption
- Peripheral Facial Nerve Palsy (LMN)
Detailed Clinical Features:
1. PRODROMAL PHASE (1–3 days before eruption)
- Burning, intense otalgia (ipsilateral)
- Low-grade fever, malaise
- Hyperesthesia/dysesthesia of the ear
2. VESICULAR ERUPTION
Location of vesicles (in order of frequency):
- External auditory canal (EAC)
- Concha of pinna
- Postauricular area
- Soft palate / tonsillar fossa
- Anterior 2/3 of tongue (taste fibers via chorda tympani)
- Occasionally: neck, face (C2/C3 dermatomes)
Vesicles are clear initially → turbid → rupture → crust over 7–10 days (Bailey & Love's 28th Ed., p. 784)
3. FACIAL NERVE PALSY
- LMN type — involves ALL muscles of ipsilateral face (forehead sparing absent, unlike UMN palsy)
- Graded by House-Brackmann Scale (Grade I–VI)
- Features:
- Loss of wrinkling of forehead
- Unable to close eye (Lagophthalmos) → Bell's phenomenon (eye rolls up on attempting closure)
- Flattening of nasolabial fold
- Drooping of angle of mouth
- Inability to puff cheeks
- Loss of taste (anterior 2/3 tongue — chorda tympani involvement)
- Hyperacusis (nerve to stapedius involved)
- Reduced lacrimation (greater petrosal nerve involved)
4. AUDIOVESTIBULAR SYMPTOMS (CN VIII involvement)
- Sensorineural hearing loss (SNHL) — high-frequency predominant
- Vertigo — acute, episodic (like vestibular neuritis)
- Tinnitus
- Nystagmus — toward unaffected side
5. OTHER FEATURES
- Dysgeusia (altered taste)
- Dry eye (keratoconjunctivitis)
- Dysphagia (if CN IX, X involved)
- Rarely: contralateral limb weakness (zoster encephalitis)
INVESTIGATIONS
1. Clinical Diagnosis (primarily)
The diagnosis is clinical based on the triad.
2. Audiological Assessment
- Pure Tone Audiogram (PTA) — SNHL, predominantly high-frequency
- Tympanometry — Type A (normal middle ear compliance; helps rule out otitis media)
- BERA/ABR — to assess retrocochlear involvement
- Caloric testing / VNG — vestibular function assessment
3. Nerve Function Tests
| Test | Purpose |
|---|---|
| Schirmer's test | Lacrimation → assesses Greater Petrosal Nerve (lesion above geniculate ganglion) |
| Stapedial reflex | Assesses nerve to stapedius (between geniculate ganglion & chorda tympani takeoff) |
| Taste testing (Electrogustometry) | Chorda tympani function |
| Submandibular gland flow | Chorda tympani/submandibular ganglion |
| Electroneurography (ENoG/ENOG) | Quantifies degree of axonal degeneration (>90% degeneration = poor prognosis) |
| Electromyography (EMG) | Detects fibrillation potentials → confirms denervation; volitional potentials = regeneration |
| Nerve Excitability Test (NET) | Compares threshold of normal vs affected side |
| Maximum Stimulation Test (MST) | Tests facial muscle response |
4. Topognostic (Site of Lesion) Diagnosis
LEVEL OF LESION DETERMINATION:
Above Geniculate Ganglion:
↓ Lacrimation (Schirmer's +ve)
↓ Stapedial reflex (absent)
↓ Taste (anterior 2/3)
↓ Salivation
Between Geniculate & Nerve to Stapedius:
Normal Lacrimation
↓ Stapedial reflex (absent)
↓ Taste
↓ Salivation
Between N. to Stapedius & Chorda Tympani:
Normal Lacrimation
Normal Stapedial reflex
↓ Taste
↓ Salivation
Below Chorda Tympani (Stylomastoid foramen):
Normal Lacrimation
Normal Stapedial reflex
Normal Taste
Normal Salivation — Motor palsy ONLY
5. Radiological Investigations
- MRI with Gadolinium contrast (investigation of choice):
- Enhancement of geniculate ganglion, facial nerve
- Rules out schwannoma, cholesteatoma, parotid malignancy
- Assesses brainstem
- HRCT Temporal bone: Rules out bony erosion, cholesteatoma, otitis media
6. Virological Tests
- VZV PCR from vesicle fluid, saliva, or CSF — confirmatory
- Tzanck smear from vesicle base: multinucleated giant cells (not specific)
- Serology: Rise in IgM/IgG anti-VZV antibodies
- CSF analysis (if CNS involvement suspected): lymphocytic pleocytosis, raised protein
ZOSTER SINE HERPETE
A critical concept: RHS without vesicles — diagnosed by positive VZV PCR from saliva/CSF, or VZV IgM serology. This must be differentiated from Bell's palsy.
CLINICAL PHOTOGRAPH — HALLMARK SIGNS
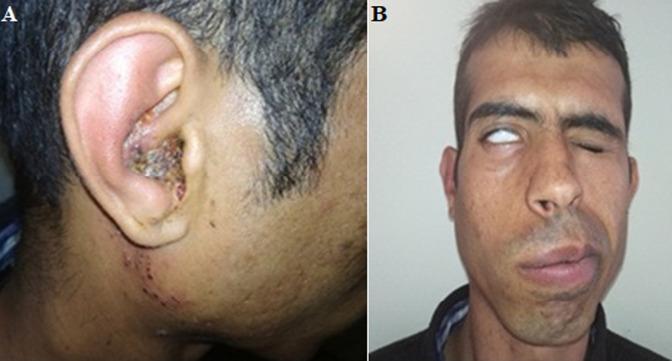
Image: Composite photograph of Ramsay Hunt Syndrome.
- Left (Image A): Right auricle showing inflammatory swelling with characteristic clustered vesicles and hemorrhagic crusting in the concha and EAC, extending to the preauricular region.
- Right (Image B): Ipsilateral LMN facial nerve palsy — facial asymmetry, drooping of right side, loss of nasolabial fold, and Bell's phenomenon (upward rolling of globe on attempted eye closure = lagophthalmos).
HOUSE-BRACKMANN GRADING SCALE FOR FACIAL PALSY
| Grade | Description | Gross Function |
|---|---|---|
| I | Normal | Normal |
| II | Mild dysfunction | Slight weakness on close inspection |
| III | Moderate dysfunction | Obvious but not disfiguring; complete eye closure with effort |
| IV | Moderately severe | Disfiguring asymmetry; incomplete eye closure |
| V | Severe dysfunction | Barely perceptible motion; incomplete closure |
| VI | Total paralysis | No movement |
DIFFERENTIAL DIAGNOSIS
| Condition | Differentiating Feature |
|---|---|
| Bell's Palsy | No vesicles, no SNHL/vertigo; idiopathic; better prognosis |
| Otitis Media with Facial Palsy | Purulent discharge, Type B tympanogram, no vesicles |
| Cholesteatoma | Bony erosion on CT, keratin debris |
| Malignant Otitis Externa | Elderly diabetic; pseudomonas; granulation tissue at EAC floor |
| Facial Nerve Schwannoma | Gradual onset; MRI shows mass |
| Parotid Malignancy | Parotid mass, progressive palsy |
| Lyme Disease (Borrelia burgdorferi) | Bilateral palsy; endemic area; positive Lyme serology (Harrison's 21st Ed.) |
| Sarcoidosis (Heerfordt syndrome) | Bilateral palsy, uveitis, parotitis |
| Guillain-Barré Syndrome | Bilateral, ascending paralysis |
| Melkersson-Rosenthal Syndrome | Recurrent facial palsy + facial edema + fissured tongue |
MANAGEMENT
FLOWCHART OF MANAGEMENT
PATIENT WITH ACUTE FACIAL PALSY + EAR PAIN/VESICLES
↓
Clinical Assessment (Triad + Audiovestibular)
↓
CONFIRM DIAGNOSIS (Clinical ± VZV PCR/MRI)
↓
┌───────────────────────────────────────────────┐
│ GENERAL MEASURES │
│ - Eye care (Lagophthalmos prevention) │
│ - Lubricant eye drops (Methylcellulose) │
│ - Eye pad/taping at night │
│ - Analgesics for otalgia │
└──────────────────┬────────────────────────────┘
↓
┌──────────────────────────────────────────────────────┐
│ ANTIVIRAL THERAPY │
│ (MOST IMPORTANT — Start within 72 hours) │
│ │
│ Acyclovir 800 mg 5×/day × 7–10 days (oral) │
│ OR │
│ Valacyclovir 1g TDS × 7 days (better bioavailability)│
│ OR │
│ Famciclovir 500 mg TDS × 7 days │
│ │
│ Severe: IV Acyclovir 10 mg/kg TDS × 7–10 days │
└──────────────────┬───────────────────────────────────┘
↓
┌──────────────────────────────────────────────────────┐
│ CORTICOSTEROIDS │
│ Prednisolone 1 mg/kg/day → taper over 10–14 days │
│ (Reduces neural edema, improves prognosis) │
│ Combined Antiviral + Steroid = Best outcome │
└──────────────────┬───────────────────────────────────┘
↓
┌────────────────────────────────────┐
│ AUDIOVESTIBULAR MANAGEMENT │
│ • SNHL: Betahistine, Vasodilators │
│ • Vertigo: Prochlorperazine, │
│ Cinnarizine │
│ • Vestibular rehab exercises │
└──────────────────┬─────────────────┘
↓
MONITOR RECOVERY WEEKLY
(House-Brackmann grading)
↓
┌────────────────────────────┐
↓ ↓
RECOVERY (>70%) No Recovery by 3 months
(Most within 6 months) → Consider Surgical Decompression
↓
ENoG: >90% degeneration within 14 days
EMG: Denervation potentials
↓
SURGICAL DECOMPRESSION of
Facial Nerve (Transpetrosal route)
— middle cranial fossa approach
DETAILED DRUG REGIMENS
| Drug | Dose | Route | Duration |
|---|---|---|---|
| Acyclovir | 800 mg 5×/day | Oral | 7–10 days |
| Valacyclovir | 1000 mg TDS | Oral | 7 days |
| Famciclovir | 500 mg TDS | Oral | 7 days |
| IV Acyclovir | 10 mg/kg TDS | IV | 7–10 days (immunocompromised/severe) |
| Prednisolone | 1 mg/kg/day | Oral | Taper over 10–14 days |
| Methylprednisolone | 1 mg/kg/day | IV | Severe cases |
| Carbamazepine/Gabapentin | Standard doses | Oral | Post-herpetic neuralgia |
| Lubricant drops | Methylcellulose 0.5% | Topical | PRN |
Eye Care (Critical — prevents exposure keratopathy)
- Artificial tear drops (Methylcellulose) — during day
- Lubricant eye ointment — at night
- Eye pad taping at night
- Tarsorrhaphy (temporary lateral lid suturing) — if corneal exposure severe
- Regular ophthalmology review
SURGICAL MANAGEMENT
Indications for Facial Nerve Decompression:
- ENoG > 90% degeneration within 14 days of onset
- No clinical or electrical recovery by 3 months
- Surgical decompression is controversial — evidence is limited
Surgical Approaches:
| Approach | Indication | Exposure |
|---|---|---|
| Middle Cranial Fossa (MCF) | Labyrinthine + tympanic segments | Preserves hearing |
| Transmastoid | Tympanic + vertical/mastoid segment | Limited proximal access |
| Translabyrinthine | Full exposure (IAC to stylomastoid) | Sacrifices hearing |
Other Surgical Procedures:
- Tarsorrhaphy — for lagophthalmos
- Gold weight implant in upper eyelid — for permanent lagophthalmos
- Hypoglossal-facial nerve anastomosis — for permanent complete palsy
- Gracilis free muscle transfer — for long-standing palsy with muscle atrophy
COMPLICATIONS
Short-term:
| Complication | Mechanism |
|---|---|
| Exposure keratopathy / Corneal ulceration | Lagophthalmos (incomplete eye closure) |
| Permanent SNHL | Cochlear nerve damage |
| Persistent vertigo | Vestibular nerve damage |
| Post-herpetic Neuralgia (PHN) | Incomplete viral clearance; chronic neuropathic pain |
| Secondary bacterial infection | Superinfection of vesicles |
Long-term:
| Complication | Details |
|---|---|
| Incomplete facial recovery | 30–50% of cases (vs. 10% in Bell's palsy) |
| Synkinesis | Aberrant regeneration — eye blinks when smiling (oro-ocular synkinesis) |
| Crocodile tears (Bogorad syndrome) | Aberrant regeneration of greater petrosal nerve → lacrimation while eating |
| Hemifacial spasm | Irregular facial twitching, post-nerve recovery |
| Contracture | Permanent facial tightening on affected side |
PROGNOSIS
| Prognostic Factor | Favorable | Unfavorable |
|---|---|---|
| Age | Young | Elderly (>60) |
| Degree of initial palsy | Incomplete (partial) | Complete palsy |
| Time to treatment | <72 hours | >72 hours |
| ENoG degeneration | <90% | >90% |
| Treatment | Antiviral + Steroid | Untreated |
| CN VIII involvement | Absent | Present |
| Immunostatus | Immunocompetent | Immunocompromised (HIV) |
Overall recovery statistics:
- Complete palsy + treated early: 70% full recovery
- Complete palsy + untreated: ~50% full recovery
- RHS vs Bell's palsy: RHS has significantly worse prognosis than Bell's palsy
- Recovery timeline: Most within 3–6 months; if no recovery by 1 year → permanent
COMPARISON: RAMSAY HUNT SYNDROME vs BELL'S PALSY
| Feature | Ramsay Hunt Syndrome | Bell's Palsy |
|---|---|---|
| Etiology | VZV reactivation | HSV-1 reactivation (mainly) |
| Site of lesion | Geniculate ganglion | Geniculate ganglion / intratemporal |
| Vesicles | Present (EAC, pinna, palate) | Absent |
| Otalgia | Severe, lancinating | Mild or absent |
| CN VIII | Often involved (SNHL, vertigo) | Not involved |
| CN IX, X | Occasionally | Not involved |
| Prognosis | Worse (30–50% incomplete recovery) | Better (10–15% incomplete recovery) |
| Treatment | Antiviral + Steroid | Steroid (± Antiviral for HSV) |
| MRI | Geniculate ganglion enhancement | May show facial nerve enhancement |
RECENT ADVANCES (Important for RGUHS)
1. Zoster Vaccine (Shingrix)
- Recombinant subunit vaccine (RZV — Shingrix) — 2 doses, highly effective (~97%) in preventing herpes zoster and RHS in adults ≥50 years
- Superior to older live-attenuated Zostavax vaccine
- Recommended for immunocompetent adults ≥50 years by CDC and WHO (2023 guidelines)
- Reduces incidence of post-herpetic neuralgia by >90%
2. Antiviral Updates
- Valacyclovir is preferred over Acyclovir due to superior oral bioavailability (3–5× higher)
- Combination antiviral + steroid proven superior to either alone (Murakami et al.)
- Early initiation (<72h) significantly improves outcomes
3. VZV PCR in Zoster Sine Herpete
- High-sensitivity VZV PCR from saliva is now the standard non-invasive diagnostic test for RHS without vesicles
- Changing the diagnostic paradigm — up to 16–18% of Bell's palsy cases may actually be VZV-mediated (detected by PCR)
4. MRI Advances
- 3T MRI with gadolinium — detects subtle geniculate ganglion enhancement as early as 48 hours
- Differentiates RHS from Bell's palsy, schwannoma, and other causes of facial palsy
- Predicts extent of nerve damage and correlates with prognosis
5. ENoG as Prognostic Tool
- ENoG performed between day 3–14 of complete palsy onset is most informative
-
90% degeneration → surgical decompression consideration
- Updated evidence suggests transcutaneous electrostimulation may help during recovery
6. Vestibular Rehabilitation
- Evidence-based vestibular rehabilitation exercises (Cawthorne-Cooksey, Brandt-Daroff) show significant improvement in RHS-related vestibular dysfunction
7. Facial Reanimation Surgery
- Selective neurorrhaphy, cross-facial nerve grafting, and dynamic reanimation using free gracilis muscle transfer — newer reconstructive options for permanent palsy
- Botulinum toxin (Botox) — used to treat synkinesis and hemifacial spasm post-recovery
8. Immunocompromised Patients (HIV/AIDS)
- RHS can present with multidermatome zoster and bilateral facial palsy
- IV Acyclovir + long-term oral antivirals recommended
- Higher rates of PHN and incomplete recovery
9. COVID-19 and RHS
- Recent case series (2021–2023) report reactivation of VZV (causing RHS) following COVID-19 infection and COVID-19 mRNA vaccination — proposed mechanism: immune dysregulation
- Not yet established as causative; monitoring ongoing
SUMMARY FLOWCHART: DIAGNOSTIC APPROACH
ACUTE PERIPHERAL FACIAL PALSY
↓
Is it LMN or UMN type?
↓ LMN
Check for Vesicles in EAC/Pinna?
↓ YES ↓ NO
RHS likely Other causes (Bell's, Otitis Media,
↓ Cholesteatoma, Tumor, Lyme, etc.)
Check: ↓
• CN VIII signs? VZV PCR (Zoster sine herpete?)
• Taste loss?
• Lacrimation?
• Hyperacusis?
↓
TOPOGNOSTIC TESTING
(Schirmer's, Stapedial reflex,
Electrogustometry)
↓
IMAGING: MRI Gadolinium
+ HRCT Temporal Bone
↓
ENoG + EMG (if complete palsy)
↓
CONFIRM RHS → START TREATMENT within 72h
KEY POINTS FOR VIVA / SHORT NOTES (RGUHS Focus)
- James Ramsay Hunt — described in 1907
- VZV — reactivates in geniculate ganglion (sensory ganglion of CN VII)
- Classic triad: Otalgia + Vesicles + LMN Facial Palsy
- Bell's phenomenon — eye rolls up when patient tries to close eye (lagophthalmos)
- House-Brackmann scale — grading facial palsy (Grade I=Normal, VI=Complete palsy)
- Schirmer's test — reduced if lesion is above/at geniculate ganglion (Greater Petrosal Nerve)
- ENoG — >90% degeneration = poor prognosis / consider surgical decompression
- Treatment: Acyclovir/Valacyclovir + Prednisolone — within 72 hours
- Prognosis of RHS is worse than Bell's palsy (50–70% full recovery vs. 85–90%)
- Zoster sine herpete — RHS without vesicles; diagnose with VZV PCR
- Shingrix vaccine — recombinant VZV vaccine; >97% effective; recommended ≥50 years
- Complications: PHN, synkinesis, crocodile tears, exposure keratopathy
- Corneal protection is a CLINICAL EMERGENCY — lagophthalmos → corneal ulcer → blindness
- MRI gadolinium — investigation of choice for imaging
REFERENCES
- Scott-Brown's Otorhinolaryngology, Head and Neck Surgery (8th Ed.) — Facial Nerve chapter
- Cummings Otolaryngology — Head and Neck Surgery (7th Ed., Flint et al.) — Ch. Facial Nerve, Herpes Zoster Oticus
- Stell and Maran's Head and Neck Surgery — Facial nerve and peripheral neuropathies
- Zakir Hussain's ENT — Ramsay Hunt Syndrome, Peripheral Facial Palsy
- Dhingra's Diseases of Ear, Nose and Throat (8th Ed.) — Facial nerve disorders, p. relevant chapters
- Hazarika's Textbook of ENT & Head-Neck Surgery — Ramsay Hunt Syndrome, facial palsy
- Bailey & Love's Short Practice of Surgery (28th Ed., p. 784) — Facial nerve palsy
- Harrison's Principles of Internal Medicine (21st Ed., p. 12502) — Differential diagnosis of facial palsy
- Murakami S et al. — "Treatment of Ramsay Hunt syndrome with acyclovir-prednisone: significance of early diagnosis and treatment" — Ann Neurol 1997
- Coulson S et al. — "Herpes zoster oticus (Ramsay Hunt syndrome)" — Cochrane Review
- CDC/WHO 2023 — Shingrix (RZV) vaccination guidelines
- Sweeney CJ, Gilden DH — "Ramsay Hunt syndrome" — JNNP 2001
- Recent articles (2021–2023) — VZV reactivation post-COVID-19 and mRNA vaccination
This comprehensive answer covers the pathophysiology, clinical features, investigations, management, complications, prognosis, and recent advances of Ramsay Hunt Syndrome as required for a 50-mark RGUHS University ENT examination, drawing from Scott-Brown, Cummings, Stell & Maran, Zakir Hussain, Dhingra, Hazarika, Bailey & Love, Harrison's, and current peer-reviewed literature.
This is a shared conversation. Sign in to Orris to start your own chat.