What are the factors affecting the pulse rate
Reading File
search_medical_text
factors affecting pulse rate heart rate
search_medical_text
physiological determinants of heart rate autonomic nervous system
GradeResponse
GradeResponse
Retrieval was limited, so I'll synthesize a comprehensive answer from established medical knowledge.
Factors Affecting Pulse Rate
Pulse rate (heart rate) is influenced by a wide range of physiological, pathological, pharmacological, and environmental factors.
1. Age
- Neonates: 120–160 bpm
- Children: 80–120 bpm
- Adults: 60–100 bpm (normal range)
- Elderly: Resting rate may decrease slightly; maximum achievable heart rate declines (~220 − age)
2. Autonomic Nervous System (ANS)
The ANS is the primary regulator of beat-to-beat heart rate:
| Division | Effect on Heart Rate | Mediator |
|---|---|---|
| Sympathetic | Increases HR (positive chronotropy) | Norepinephrine → β1 receptors |
| Parasympathetic (Vagus) | Decreases HR (negative chronotropy) | Acetylcholine → M2 receptors |
At rest, vagal tone predominates, keeping resting HR below the intrinsic SA node rate (~100 bpm).
3. Physical Activity & Exercise
- Exercise increases sympathetic drive and decreases vagal tone → HR rises
- Trained athletes have lower resting HR (sometimes 40–50 bpm) due to increased vagal tone and cardiac hypertrophy (athletic bradycardia)
4. Emotional State & Stress
- Anxiety, fear, excitement, and pain activate the sympathoadrenal axis → elevated HR
- Deep relaxation and meditation increase vagal tone → lower HR
5. Body Temperature
- Fever/hyperthermia: Each 1°C rise in core temperature increases HR by approximately 10–15 bpm (direct effect on SA node automaticity)
- Hypothermia: Decreases HR; extreme hypothermia can cause bradycardia and cardiac arrest
6. Medications & Drugs
| Drug/Substance | Effect |
|---|---|
| Beta-blockers (propranolol) | ↓ HR |
| Atropine (anticholinergic) | ↑ HR |
| Digoxin | ↓ HR (increases vagal tone) |
| Caffeine, nicotine | ↑ HR |
| Opioids | ↓ HR |
| Sympathomimetics (epinephrine) | ↑ HR |
| Calcium channel blockers (verapamil) | ↓ HR |
| Thyroid hormone (excess) | ↑ HR |
7. Blood Pressure & Hemodynamic Status
- Hypotension/hemorrhage/dehydration: Triggers baroreceptor reflex → sympathetic activation → tachycardia (compensatory)
- Hypertension: Can stimulate baroreceptors → reflex bradycardia
8. Respiratory Cycle (Sinus Arrhythmia)
- HR increases during inspiration (inhibition of vagal tone) and decreases during expiration
- This respiratory sinus arrhythmia is normal and more pronounced in children and athletes
9. Hormonal Factors
| Hormone | Effect |
|---|---|
| Epinephrine/Adrenaline | ↑ HR |
| Thyroid hormones (T3, T4) | ↑ HR (hyperthyroidism → tachycardia) |
| Cortisol | ↑ HR |
| Estrogen/Progesterone | Moderate effects; HR rises in pregnancy |
10. Posture & Position
- Moving from lying → sitting → standing activates orthostatic reflexes → slight HR increase (sympathetic activation to maintain BP)
- Orthostatic tachycardia is pronounced in POTS (Postural Orthostatic Tachycardia Syndrome)
11. Pathological Conditions
| Condition | Effect |
|---|---|
| Fever, infection, sepsis | ↑ HR (tachycardia) |
| Anemia | ↑ HR (compensatory) |
| Hyperthyroidism | ↑ HR |
| Heart failure | ↑ HR (compensatory) |
| Heart block (AV block) | ↓ HR (bradycardia) |
| Hypothyroidism | ↓ HR |
| Raised intracranial pressure | ↓ HR (Cushing's reflex) |
| Myocardial infarction | Variable |
12. Sex
- Women tend to have a slightly higher resting HR than men on average, partly due to smaller heart size and hormonal differences
13. Pain
- Acute pain typically causes tachycardia via sympathetic activation
- Severe visceral pain (e.g., inferior MI, vasovagal syncope) can cause bradycardia via vagal activation
14. Blood Gas & Metabolic Factors
- Hypoxia: ↑ HR (peripheral chemoreceptor stimulation)
- Hypercapnia: Initially ↑ HR; severe hypercapnia → bradycardia
- Acidosis: Can depress SA node function → bradycardia
- Electrolyte imbalances (e.g., hyperkalemia): Bradycardia; hypokalemia → tachyarrhythmias
Summary Table
| Category | Increases HR | Decreases HR |
|---|---|---|
| ANS | Sympathetic activation | Parasympathetic/vagal activation |
| Exercise | Yes | Trained state (resting) |
| Temperature | Fever, heat | Hypothermia |
| Drugs | Epinephrine, atropine, caffeine | Beta-blockers, digoxin, opioids |
| Hormones | Thyroid hormones, epinephrine | — |
| Pathology | Anemia, sepsis, hyperthyroidism | AV block, hypothyroidism, ↑ICP |
| Posture | Standing (orthostasis) | Supine position |
| Emotions | Stress, anxiety, pain | Relaxation, meditation |
Answers the following
search_medical_text
tachycardia bradycardia definition causes
search_medical_text
sinus arrhythmia pulse deficit arterial pulse recording
GradeResponse
GradeResponse
Generating Image
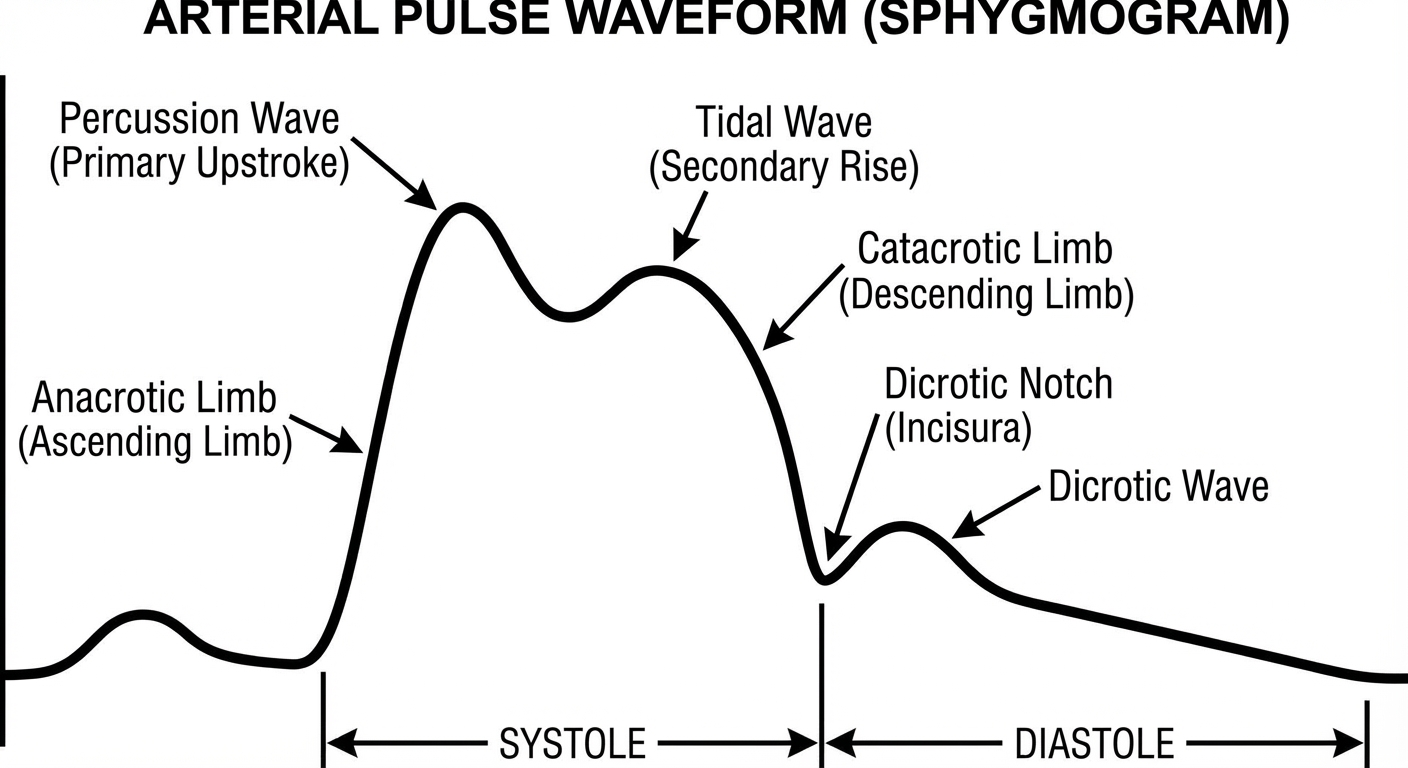
Explanation of components:
| Component | Description |
|---|---|
| Anacrotic limb | Rapid upstroke due to ejection of blood from the left ventricle into the aorta during systole |
| Percussion wave | The primary peak; represents the maximum pressure during ventricular systole |
| Tidal wave | A secondary smaller rise on the descending limb; due to reflection of pulse wave from the periphery |
| Dicrotic notch (Incisura) | A notch on the descending limb caused by the closure of the aortic valve at the end of systole |
| Dicrotic wave | A small wave just after the dicrotic notch; due to elastic recoil of the aortic wall during diastole |
| Catacrotic limb | The descending limb; represents the fall in pressure during diastole |
Q6. Effect of Exercise on Heart Rate
During exercise:
- Anticipatory rise — even before exercise begins, HR increases due to cortical stimulation of the sympathetic nervous system
- During exercise: Increased muscle activity → rise in CO₂ and lactic acid → stimulation of chemoreceptors → sympathetic activation → HR increases significantly
- Circulating epinephrine from adrenal medulla further increases HR
- Withdrawal of vagal (parasympathetic) tone contributes to rise
- Rise in body temperature during exercise directly stimulates the SA node
After exercise: HR gradually returns to resting level — faster recovery in trained individuals.
In trained athletes: Resting HR is lower (40–60 bpm) due to increased vagal tone and greater stroke volume (cardiac hypertrophy). The maximum HR achievable = ~220 − age.
Q7. Effect of Standing from Supine Position on Heart Rate
When a person stands up from a lying (supine) position:
- ~500–700 mL of blood pools in the lower limb veins due to gravity
- Venous return to the heart decreases → cardiac output falls → blood pressure drops transiently
- Baroreceptors in the aortic arch and carotid sinus detect the drop in BP
- Baroreceptor reflex is activated → sympathetic stimulation increases, vagal tone decreases
- Result: Heart rate increases by 10–20 bpm to compensate and maintain BP and cardiac output
Normal response: HR rises and BP is quickly restored within a few seconds.
Abnormal response: If this compensation fails, it results in orthostatic (postural) hypotension with symptoms of dizziness or syncope — seen in dehydration, autonomic neuropathy, or prolonged bed rest.
In POTS (Postural Orthostatic Tachycardia Syndrome), HR rises by >30 bpm upon standing without an adequate BP response.
This is a shared conversation. Sign in to Orris to start your own chat.