All over body with itching
Reading File
search_medical_text
prurigo nodularis multiple papules nodules all over body itching
search_medical_text
papular urticaria scabies nodular lesions arms itching differential diagnosis
search_medical_image
prurigo nodularis papules arms itching
GradeResponse
GradeResponse
GradeResponse
Clinical Assessment
Most likely diagnosis: Prurigo Nodularis (PN)
The images show multiple discrete, dome-shaped papules and nodules distributed over the extensor surface of the arms, several with white/crusted tops consistent with excoriation — a classic presentation.
Morphology from the Images
| Feature | Observation |
|---|---|
| Lesion type | Dome-shaped firm papules/nodules |
| Surface | Some with white/hyperkeratotic tops (excoriated/crusted) |
| Distribution | Extensor arms, spreading proximally and distally |
| Background skin | Post-inflammatory hyperpigmentation |
| Symptom | Intense generalized pruritus |
Diagnosis: Prurigo Nodularis
Prurigo nodularis is a chronic inflammatory skin disease driven by an itch-scratch cycle. Repeated scratching induces nerve proliferation and chronic skin changes, perpetuating the itch.
Pathophysiology: Intense pruritus → scratching → trauma → epidermal hyperplasia, dermal fibrosis, nerve proliferation → more itch (self-perpetuating cycle).
Key clinical features:
- Multiple firm, dome-shaped nodules (5–20 mm) on extensor surfaces
- Severe, intractable pruritus
- Post-inflammatory hyperpigmentation common in darker skin types
- Sparing of the mid-back ("butterfly sign") is characteristic but not always present
Reference Image (Prurigo Nodularis)
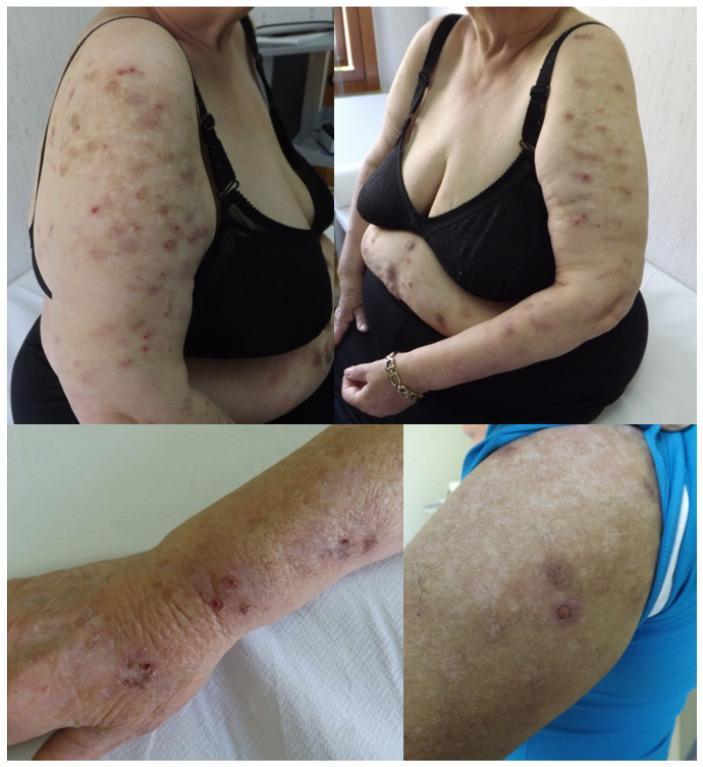
Differential Diagnoses to Consider
| Condition | Distinguishing Features |
|---|---|
| Nodular scabies | Burrows in web spaces/genitalia; household contacts affected; responds to scabicides |
| Papular urticaria | Urticarial base, insect bite history, transient lesions |
| Lichen planus | Violaceous flat-topped papules, Wickham striae, oral lesions |
| Hypertrophic lichen planus | Thick plaques on shins, overlapping features with PN |
| Pemphigoid nodularis | Rare; blister formation; IgG/C3 on IF |
Important: In any new or severe case of PN, screen for underlying systemic triggers (see below), especially given the widespread distribution.
Workup — Screen for Underlying Causes
| Category | Tests |
|---|---|
| Renal | BUN, creatinine (CKD is a major cause) |
| Hepatic | LFTs, HBsAg, anti-HCV (cholestatic itch) |
| Haematologic | CBC, peripheral smear (polycythemia vera, lymphoma) |
| Endocrine | TFTs (thyroid disease), FBS (diabetes) |
| Infectious | HIV serology (PN is a well-known HIV-associated dermatosis — Harrison's, p. 5916) |
| Atopic | IgE, eosinophil count (atopic diathesis) |
| Iron stores | Serum ferritin, iron studies |
Management
Step 1 — General Measures
- Emollients (thick moisturizers) liberally and frequently
- Trim fingernails short; cotton gloves at night
- Avoid hot water baths
Step 2 — Topical Therapy
- High-potency topical corticosteroids (clobetasol propionate 0.05%) under occlusion to individual nodules
- Topical calcineurin inhibitors (tacrolimus 0.1%) for maintenance
- Topical capsaicin (0.025–0.075%) — desensitizes C-fibers; burning sensation initially
Step 3 — Intralesional Therapy
- Intralesional triamcinolone acetonide (10–40 mg/mL) for individual thick nodules — highly effective
Step 4 — Systemic Therapy (for widespread/refractory cases)
| Drug | Dose | Notes |
|---|---|---|
| Antihistamines | Cetirizine/hydroxyzine | Adjunct for itch relief |
| Gabapentin/pregabalin | 300–1800 mg/day | For neuropathic itch component |
| Naltrexone (low-dose) | 4.5 mg/night | Opioid antagonist for refractory pruritus |
| Dupilumab | 300 mg SC every 2 weeks | IL-4/IL-13 blockade; FDA-approved for PN (2022) |
| Thalidomide/lenalidomide | Specialist use | For severe refractory PN |
| Narrowband UVB phototherapy | 2–3×/week | Effective for widespread disease |
Step 5 — Address Underlying Cause
Treating the trigger (e.g., correcting iron deficiency, managing CKD, treating HIV) can lead to significant improvement.
Summary
This presentation is highly consistent with Prurigo Nodularis. The priority is:
- Rule out nodular scabies (treat empirically with permethrin if clinical suspicion)
- Screen for HIV, CKD, hepatic disease, and haematologic malignancy
- Start topical high-potency steroids ± intralesional triamcinolone for thickest lesions
- Add gabapentin or dupilumab for widespread/refractory disease
(Harrison's Principles of Internal Medicine, 21st Ed., p. 5916)
This is a shared conversation. Sign in to Orris to start your own chat.