45 f kco bk slab d3 due to ankle sprain fall while walking to bathroom with walker , fall on olecranon and coccyx. Swelling and pain in olecranon, no head injury but reports feeling of shaking of head. How to manage first few days, hospital too far away. Best position to keep elbow for olecranon stability
olecranon fracture conservative management splinting position elbow
coccyx coccygeal injury fall management conservative treatment
olecranon undisplaced fracture elbow position immobilization 90 degrees splint
concussion head injury shaking sensation management without hospital
45F, KCO DM, Fell with Walker — Multi-Site Injury Management (Remote Setting)
- Olecranon injury (possible fracture — swelling + pain)
- Coccyx injury
- Head symptom — "shaking sensation" (possible concussion/BPPV, no direct head strike documented)
- Background: DM, ankle sprain (pre-existing)
1. Olecranon — Elbow Injury
Best Position for Stability
Immobilize at 90° elbow flexion (right-angle position), forearm in neutral rotation (thumb pointing up), with a posterior slab/splint or firm folded padding + bandage.
- At 90°, the pull of triceps on the olecranon fragment is minimized
- Allows the fracture gap (if present) to remain reduced under least tension
- Do NOT extend the elbow — triceps pull will distract any fracture fragment
- Use a folded magazine/cardboard as a posterior slab
- Apply behind the upper arm and forearm (posterior surface)
- Secure with crepe bandage or cloth
- Use a broad arm sling over clothing to maintain the 90° position
- The arm should rest across the chest, NOT hanging down
Olecranon — First Few Days Management
| Action | Detail |
|---|---|
| RICE | Rest, Ice (10–15 min every 2 hrs, cloth-wrapped), no direct ice on skin (especially diabetic) |
| Elevation | Keep arm elevated on a pillow when resting to reduce swelling |
| Analgesia | Paracetamol 500–1000 mg every 6–8 hrs (preferred in DM) |
| NSAID | Ibuprofen 400 mg TDS with food if no contraindication (check renal function — caution in DM) |
| No weight-bearing | Do not lean on elbow or use arm to push up |
| Wound check | Inspect skin over olecranon daily — thin skin here is prone to pressure injury |
- Skin tenting, open wound, or bone visible
- Numbness or tingling in ring/little fingers (ulnar nerve)
- Loss of ability to feel or move fingers
- Rapidly increasing swelling with tightness (compartment syndrome)
2. Coccyx Injury
| Action | Detail |
|---|---|
| Seating | Use a donut cushion or coccyx cut-out cushion; avoid sitting on hard surfaces |
| Position of comfort | Lying slightly to one side or prone (if tolerable) reduces direct pressure |
| Analgesia | Same as above — paracetamol ± ibuprofen |
| Bowel care | Avoid straining; stool softener (lactulose or isabgol) if needed — straining worsens pain |
| Activity | Limit sitting duration; walking short distances is acceptable |
| Duration | Significant pain typically 6–12 weeks; full resolution 3–6 months |
3. "Shaking Sensation in Head" — Possible Concussion
Watch Closely for the Following (Concussion Red Flags — Evacuate Urgently):
- Loss of consciousness (even brief)
- Worsening headache over hours
- Repeated vomiting (>2 episodes)
- Confusion, difficulty recognizing people, slurred speech
- One pupil larger than the other
- Weakness or numbness in arms/legs
- Seizure
- Cannot be woken up
If BPPV suspected (room spinning when moving head):
- Epley manoeuvre can be performed at home
- Avoid sudden head movements
- Sleep with head slightly elevated (2 pillows)
General:
- Complete cognitive rest for 24–48 hrs (no screens, no bright light, no exertion)
- Monitor hourly for the first 6 hours
- No sedating medications
4. Diabetes-Specific Considerations
| Concern | Action |
|---|---|
| Wound healing | Inspect all injury sites daily; any skin break is high risk |
| Blood glucose | Stress + pain elevates glucose; check BS more frequently |
| Renal caution | Avoid prolonged NSAIDs if eGFR compromised |
| Circulation | Ice use — always use a cloth barrier; limit to 15 min sessions |
| Infection risk | Any puncture or abrasion needs careful antiseptic care |
Summary — Priority Order
- Immobilize elbow at 90° NOW in a posterior slab/sling
- Monitor neurological status hourly for first 6 hours (concussion watch)
- Coccyx cushion + analgesia
- Arrange X-ray of elbow and coccyx at earliest opportunity — undisplaced fractures managed conservatively, but displaced olecranon fractures require surgical fixation and cannot wait indefinitely
- Document blood glucose and adjust diabetic medications if intake is reduced due to pain
Reports tingling of little and ring finger with hand during fall and a few hrs post it. But able to move all fingers now
ulnar nerve injury olecranon fracture cubital tunnel neuropraxia management
ulnar nerve anatomy olecranon groove cubital tunnel
Ulnar Nerve — Critical Update
Why This Happens
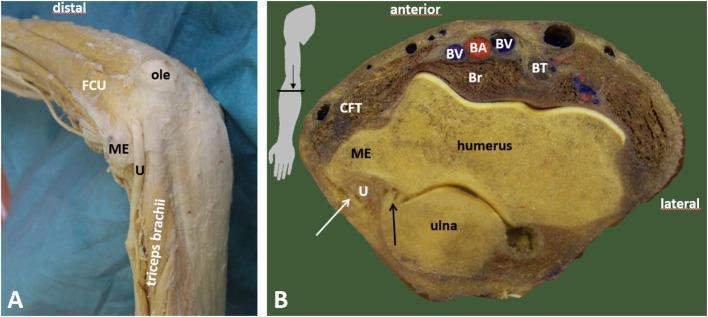
What the Current Status Means
| Feature | Interpretation |
|---|---|
| Tingling during fall + few hours after | Ulnar nerve was traumatized — neuropraxia (nerve bruising, no structural disruption) most likely |
| Movement of all fingers now normal | Motor fibers intact — reassuring, no axonotmesis or complete injury currently |
| Tingling has resolved | Suggests the acute compression/stretch phase has passed |
What to Watch For — Serial Neurological Checks (Every Few Hours)
- Lightly touch the little finger and the ulnar (medial) half of the ring finger
- Compare with the same fingers on the other hand
- Any new numbness = worrying sign
- Finger spread test: Ask her to spread all 5 fingers wide apart and hold against resistance. Weakness of the little/ring finger = ulnar intrinsic weakness
- Froment's sign: Ask her to hold a piece of paper between thumb and index finger. If the thumb bends at the tip joint to grip, that is a positive Froment's sign — ulnar motor weakness
- Overall grip should feel near-normal for her
Position of Elbow — Updated Guidance
This changes the immobilization recommendation slightly.
- Elbow flexion beyond 90° increases pressure in the cubital tunnel and worsens ulnar nerve compression
- Keep elbow at exactly 90° or very slightly less (80–85°) — do NOT flex more than 90°
- A broad arm sling holding the forearm horizontally across the chest achieves this naturally
- Avoid resting the medial side of the elbow on any hard surface (e.g., armrest, mattress edge) — this compresses the nerve directly
Red Flags — Evacuate Without Delay If:
- Tingling returns or worsens in ring/little finger
- She cannot spread fingers or grip weakens
- New claw deformity of ring/little finger (they curl and she cannot straighten them)
- Wrist drop (rare with ulnar injury but indicates broader nerve involvement)
- Swelling at the elbow increases significantly — can increase nerve compression
Summary of Change
- This raises the suspicion for a displaced or comminuted fracture rather than a simple undisplaced one — displaced fragments are more likely to injure the adjacent ulnar nerve
- X-ray and orthopedic review is now more urgent — within 24 hours if any way possible, not just "at earliest convenience"
- If tingling returns or motor signs appear, this becomes a surgical emergency (nerve decompression may be needed)
Reports tingling of little and ring finger with hand during fall and a few hrs post it. But able to move all fingers now
- Resolved tingling = neuropraxia (nerve bruising) — reassuring for now
- Elbow must stay at 90° or slightly less — never flex beyond 90°
- No pressure on the medial elbow at any time
- Repeat neuro checks every few hours — finger spread, little finger sensation, Froment's sign
- X-ray within 24 hours — ulnar nerve involvement raises concern for a displaced fracture that needs imaging urgently
Same pt
olecranon fracture X-ray displaced undisplaced classification
olecranon fracture classification displaced surgical indications tension band wiring
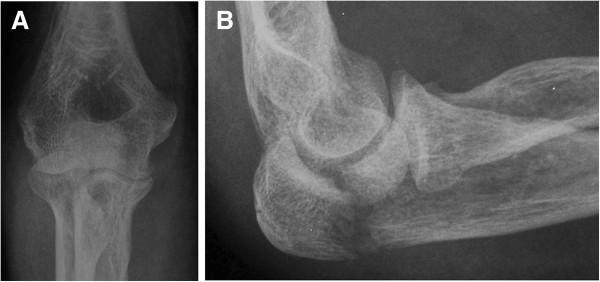
X-Ray Interpretation — Same Patient
Image Analysis
- Lateral projection of the elbow
- The olecranon tip shows disruption of the posterior cortex
- There is visible soft tissue swelling over the posterior elbow
- The image quality through the screen makes fine detail difficult but the bony contour of the olecranon is irregular
- This is the more informative view
- The olecranon region shows a fracture line at the proximal olecranon
- There is apparent displacement — the proximal fragment appears shifted
- The articular surface of the trochlear notch needs careful assessment
- No obvious comminution visible at this resolution, but cannot be fully excluded
- The distal humerus and radial head appear intact on this view
Classification (Mayo System)
What This Means Clinically
| Finding | Implication |
|---|---|
| Displaced fracture (>2 mm) | Conservative management is NOT sufficient |
| Extensor mechanism likely disrupted | Triceps pull will widen the gap further with time |
| Ulnar nerve tingling already documented | Displaced fragment is close to or impinging on ulnar nerve |
| Diabetic patient | Delayed surgery carries infection risk; prolonged immobilization causes stiffness |
Immediate Action Plan — Revised
This fracture needs surgery. The question is timing and logistics.
- Maintain posterior slab at 90° — do not change position, do not attempt any manipulation
- Do NOT attempt closed reduction at a remote facility
- Strict nil manipulation of the elbow
- Repeat neuro check — document finger spread, little finger sensation NOW and log it
- Analgesia: Paracetamol + short course ibuprofen (with food, monitor renal function given DM)
- NPO (nothing by mouth) status — anticipate she may need general/regional anesthesia soon
- This patient needs transfer to a facility with orthopedic surgical capability as soon as possible — ideally within 12–24 hours
- The ulnar nerve involvement makes this more urgent, not elective
- During transport: arm in posterior slab + broad arm sling, supported on a pillow, no pressure on medial elbow
- Formal AP + true lateral elbow X-ray (undistorted, not through a screen)
- Orthopedic review for tension band wiring or plate fixation
- Ulnar nerve assessment and possible nerve decompression at time of surgery if still symptomatic
Bottom Line
This is a displaced olecranon fracture with transient ulnar nerve involvement in a diabetic patient. It cannot be managed conservatively long-term. Surgical fixation is required. Stabilize, protect the elbow at 90°, monitor the ulnar nerve, and arrange urgent transfer.
Where exactly is the fracture. Can you explain with reference and normal
olecranon anatomy normal X-ray lateral view trochlear notch coronoid process
olecranon fracture site proximal ulna labeled diagram
Step 1 — Normal Elbow Lateral X-Ray (Reference)
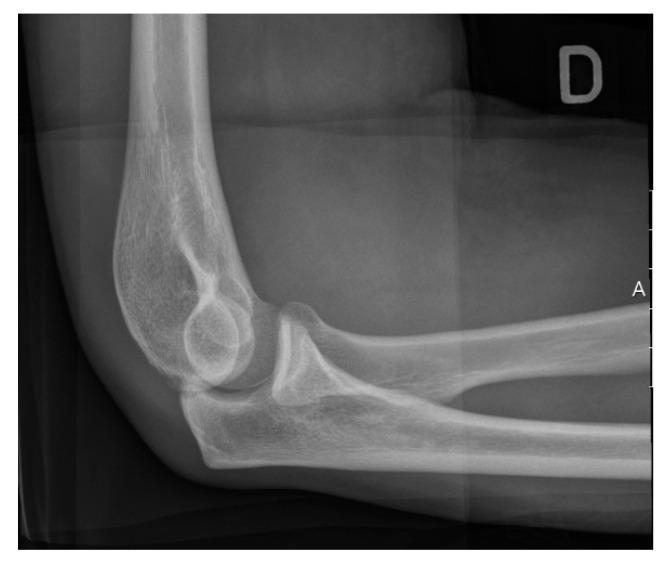
POSTERIOR (back)
│
[OLECRANON TIP] ← the bony point you feel at the back of the elbow
│
[TROCHLEAR NOTCH] ← the curved C-shaped articular surface that grips the humerus
│
[CORONOID PROCESS] ← small bony projection at the front
│
ANTERIOR (front)
- Tip (non-articular) — where the triceps muscle inserts
- Articular portion — the trochlear notch, which wraps around the humerus to form the hinge of the elbow
Step 2 — Where Exactly Is the Fracture in Your Patient?
OLECRANON TIP
│
┌─────────┴──────────┐
│ FRACTURE LINE │ ← HERE — at the base/waist of the olecranon
└─────────┬──────────┘ just proximal to the trochlear notch
│
ULNAR SHAFT
- The fracture is at the base (waist) of the olecranon — the junction between the olecranon tip and the beginning of the trochlear notch
- This is the most common site for olecranon fractures (transverse fracture at the olecranon waist)
- The proximal fragment (tip of olecranon + triceps attachment) is pulled upward and backward by the triceps muscle
- The distal fragment (rest of ulna + forearm) stays in place
- This creates the gap visible on your X-ray
Step 3 — Why This Location Matters
| Structure at this site | Consequence of fracture here |
|---|---|
| Triceps insertion | Pulls proximal fragment away — widens gap with any arm movement |
| Trochlear notch articular surface | Fracture line may enter the joint — affects elbow mechanics |
| Ulnar nerve groove (just medial) | Explains the ring/little finger tingling your patient had |
| Elbow hinge axis | Loss of stability = cannot extend elbow against gravity |
Step 4 — Surgical Fix at This Exact Site
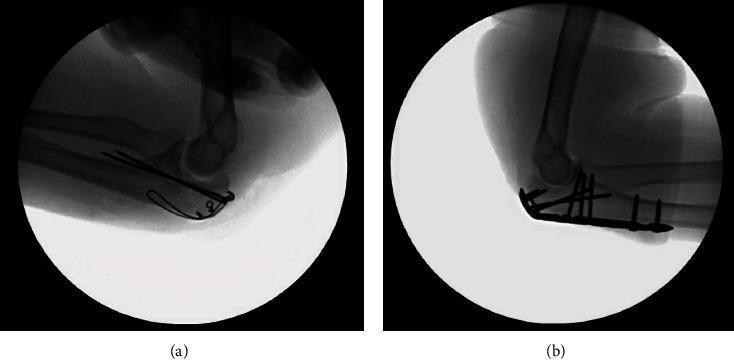
- Tension band wiring (TBW): Two K-wires driven down the olecranon into the ulnar shaft + a figure-of-8 wire that converts triceps pull into compression across the fracture — standard for simple transverse fractures like this
- Plate fixation: Used if comminuted or fracture extends further down — provides more rigid fixation
Summary in Plain Terms
The pointed bony tip at the back of the elbow (olecranon) has broken off at its base. The triceps muscle, which attaches to this tip, is pulling the broken piece upward. The gap this creates is visible on the X-ray and is why she cannot extend her elbow against resistance. The ulnar nerve, which runs in a groove right next to this fracture site, was irritated by the injury — explaining the ring and little finger tingling. Surgery is needed to put the fragment back and hold it with wires or a plate.
Can you explain the ap oblique view with reference
normal elbow AP anteroposterior X-ray labeled medial epicondyle lateral epicondyle olecranon radial head
olecranon fracture AP view X-ray proximal ulna displacement
Reference — AP View of Displaced Olecranon Fracture (Mayo Type IIA)

What You Are Looking at on an AP/Oblique Elbow View
HUMERUS (shaft coming down)
│
┌─────────┴─────────┐
│ │
LATERAL MEDIAL
EPICONDYLE EPICONDYLE
│ │
CAPITULUM TROCHLEA
│ │
RADIAL HEAD OLECRANON / CORONOID
│ │
RADIUS SHAFT ULNA SHAFT
Normal AP Landmarks — What Each Structure Looks Like
| Structure | Appearance on AP |
|---|---|
| Distal humerus | Flared bone ending in two rounded bumps (epicondyles) |
| Lateral epicondyle | Outer bony prominence |
| Medial epicondyle | Inner bony prominence — ulnar nerve runs just behind here |
| Capitulum | Smooth round knuckle on lateral side — articulates with radial head |
| Trochlea | Spool-shaped structure on medial side — articulates with olecranon/coronoid |
| Radial head | Circular flat disc-shaped structure on lateral side |
| Olecranon | Seen end-on in AP — appears as a dense white oval/shadow overlying the distal humerus in the center |
| Coronoid process | Small projection just below the trochlea |
| Ulna shaft | Straight line continuing downward from the olecranon |
Your Patient's AP/Oblique View — Structure by Structure
✅ What is Normal / Intact
- Distal humerus — intact, no fracture line visible through the humeral shaft
- Medial and lateral epicondyles — visible and appear intact
- Radial head — visible on the lateral side, no obvious fracture
- Capitulum-radial head articulation — appears maintained, no dislocation
- Joint space — the humero-ulnar joint space is preserved
🔴 Where the Fracture Is
On YOUR patient's AP/oblique:
HUMERUS
│
[TROCHLEA]
│
════════════ ← FRACTURE LINE visible here
│ transverse, at the olecranon base
[PROXIMAL ← this fragment is shifted
FRAGMENT] slightly laterally and superiorly
↑↑
(pulled by triceps)
│
[ULNA SHAFT] ← distal fragment, stays in place
-
Fracture line — there is a clear lucent (dark) line cutting across the proximal ulna just at the base of the olecranon, where it begins to form the trochlear notch. This is most visible in the central/medial part of the proximal ulna on the AP view.
-
Proximal fragment displacement — the olecranon tip fragment appears to have a subtle lateral and proximal shift compared to the ulnar shaft below — this is the classic finding on AP in a displaced fracture, matching the reference image (A) above exactly.
-
Disrupted cortical line — on the medial border of the proximal ulna, the normally smooth continuous white cortical line is interrupted and stepped at the fracture site.
-
No widening of humero-ulnar joint — the joint itself is not dislocated, meaning this is a stable elbow (consistent with Mayo Type II, not Type III).
-
No radial head fracture visible — important to note, as radial head fractures often accompany elbow injuries (the "terrible triad"). Not seen here, but a true lateral view at a proper facility will confirm.
Side-by-Side Comparison Summary
| Feature | Reference (Mayo IIA) | Your Patient |
|---|---|---|
| Fracture line location | Base of olecranon, transverse | Same — base of olecranon |
| Proximal fragment | Displaced laterally + superiorly | Same pattern |
| Elbow joint | Stable, no dislocation | Stable, joint space maintained |
| Radial head | Intact | Appears intact |
| Comminution | None (IIA = non-comminuted) | Not clearly seen — needs proper lateral view to confirm |
| Humeral shaft | Intact | Intact |
Why the Oblique View is Less Ideal Than a True Lateral
- The olecranon is not seen in pure profile
- The fracture gap may be underestimated (it could be wider than it appears)
- Comminution may be hidden by overlapping bone
- A true lateral view (which you already have in image 1) and a true AP at a proper facility will give the full picture before surgical planning
Bottom Line on the AP/Oblique
The AP/oblique view confirms a transverse fracture at the base of the olecranon with the proximal fragment shifted away from the ulnar shaft — driven by triceps pull. The elbow joint is stable with no dislocation. This is consistent with Mayo Type IIA — displaced, non-comminuted, stable — which is the classic indication for tension band wiring at surgery.