Treatment of swelling in testis
Reading File
search_medical_text
testicular swelling scrotal swelling causes diagnosis treatment
search_medical_text
epididymo-orchitis hydrocele varicocele testicular torsion management
search_medical_image
scrotal swelling testicular anatomy diagram
GradeResponse
GradeResponse
GradeResponse
Here is a comprehensive overview of testicular (scrotal) swelling — its causes, diagnosis, and treatment:
Testicular / Scrotal Swelling
Common Causes
| Condition | Key Features | Acuity |
|---|---|---|
| Testicular Torsion | Acute severe pain, absent cremasteric reflex, elevated testicle | Surgical emergency |
| Epididymo-Orchitis | Pain + fever, history of STI/UTI, dysuria | Urgent (antibiotics) |
| Hydrocele | Painless fluid accumulation, transilluminates | Elective |
| Varicocele | "Bag of worms" feel, left-sided, may cause subfertility | Elective |
| Inguinal Hernia | Bowel in scrotum, reducible, may have cough impulse | May be urgent if strangulated |
| Epididymal Cyst | Soft, separate from testis, transilluminates | Elective |
| Testicular Cancer | Hard, painless lump, non-transilluminable, constitutional symptoms | Urgent referral |
| Trauma / Haematocele | History of injury, tender, may not transilluminate | Urgent if haematocele |
Diagnosis
Clinical Assessment
- History: onset (acute vs. gradual), pain, fever, sexual history, trauma
- Examination: side, consistency, tenderness, position, transillumination, cremasteric reflex
Investigations
- Scrotal Ultrasound (Doppler): First-line imaging — assesses blood flow (rules out torsion), identifies hydrocele, varicocele, masses (STI Guidelines, p. 101)
- Ultrasound is primarily used to rule out torsion in acute painful swelling
- A negative ultrasound does not rule out epididymitis and should not override clinical judgment
- Urinalysis / Urine culture: For suspected infection
- STI swabs / NAAT (urine or urethral): If epididymo-orchitis suspected
- Tumour markers: AFP, β-hCG, LDH — if testicular cancer suspected
- Radionuclide scan: Most accurate for epididymitis but rarely available
Note: Bilateral testicular pain/swelling should raise suspicion for systemic causes (e.g., mumps orchitis, vasculitis, lymphoma).
Treatment by Condition
🔴 Testicular Torsion (Surgical Emergency)
- Immediate surgical exploration — do NOT wait for imaging if clinical suspicion is high
- Manual detorsion can be attempted while awaiting theatre (usually "open book" — rotate outward)
- Orchiopexy of both testes (bilateral fixation) once viability confirmed
- Orchidectomy if testicle non-viable (>6 hours ischemia — salvage rate drops significantly)
- Window of salvage: >90% if within 6 hrs, <10% after 24 hrs
🟠 Epididymo-Orchitis
Likely STI-related (age <35 yrs, sexually active):
- Ceftriaxone 500 mg IM single dose + Doxycycline 100 mg BD × 10–14 days
- Treat sexual partners; abstain during treatment
Likely enteric/urinary organisms (age >35 yrs, instrumentation, UTI):
- Ofloxacin 200 mg BD × 14 days OR Levofloxacin 500 mg OD × 10 days
Supportive measures:
- Scrotal support / elevation
- NSAIDs (e.g., ibuprofen 400 mg TDS) for pain/inflammation
- Rest and hydration
🟡 Hydrocele
(Paediatric Urology Guidelines, p. 26)
| Type | Management |
|---|---|
| Congenital communicating (children) | Observe until age 1–2 yrs; surgical repair (herniotomy/ligation of processus vaginalis) if persists |
| Primary/Idiopathic (adult) | Aspiration (temporary; high recurrence) OR surgical hydrocelectomy (Lord's/Jaboulay procedure) |
| Secondary (from infection, trauma, tumour) | Treat underlying cause first |
Aspiration + sclerotherapy (e.g., with tetracycline, polidocanol) is an option in patients unfit for surgery.
🟡 Varicocele
- Indications for treatment: subfertility, chronic dull pain, testicular atrophy in adolescents
- Options:
- Surgical ligation (subinguinal microsurgical approach — gold standard)
- Laparoscopic ligation
- Percutaneous embolization (radiological, less invasive)
- No treatment needed if asymptomatic and fertility is not a concern
🟡 Epididymal Cyst
- Usually no treatment needed if asymptomatic
- Surgical excision if large, symptomatic, or causing anxiety — though risk of epididymal damage exists
🔴 Testicular Cancer
- Urgent orchidectomy via inguinal approach (never scrotal) for diagnosis and primary treatment
- Further management depends on histology (seminoma vs. non-seminoma) and staging:
- Stage I: Surveillance / adjuvant radiotherapy (seminoma) / BEP chemotherapy (NSGCT)
- Advanced: BEP chemotherapy ± retroperitoneal lymph node dissection (RPLND)
🟡 Inguinal Hernia with Scrotal Extension
- Elective surgical repair (open or laparoscopic) for reducible hernias
- Emergency surgery for irreducible/strangulated hernia
Clinical Image — Massive Scrotal Swelling
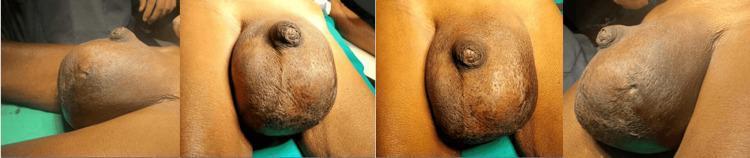
Key Clinical Pearls
- Acute painful scrotal swelling = testicular torsion until proven otherwise — time is testicle
- Doppler ultrasound is the investigation of choice but should never delay surgical exploration when torsion is clinically suspected
- A hard, painless testicular lump in a young man = cancer until proven otherwise
- Transillumination differentiates fluid-filled (hydrocele/cyst) from solid lesions
This is a shared conversation. Sign in to Orris to start your own chat.