Peri oral skin lesion and redness
Reading File
Checking Date & Time
Asking for Preferences
Asking for Preferences
Finding Sources
Searching PubMed
perioral dermatitis treatment
Searching Images
perioral dermatitis clinical photo rash around mouth
Reading File
Reading File
Loading Image
Perioral Dermatitis
Perioral dermatitis (also called periorificial dermatitis) is a common inflammatory acneiform eruption confined to the skin around the mouth in adults, with a strong female predominance (ages 20–35).
Clinical Features
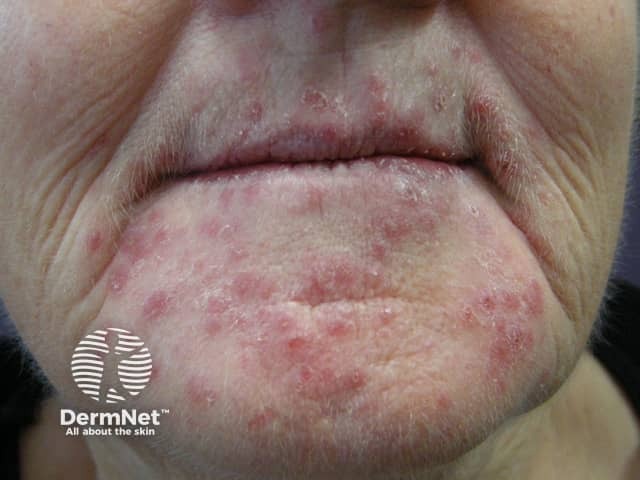
- Morphology: Discrete small inflammatory papules and pustules on an erythematous, sometimes scaling base
- Distribution: Symmetrically around the mouth — a hallmark clear zone of ~5 mm between the vermilion border and the eruption (lip margin is spared)
- Symptoms: Usually asymptomatic; may cause mild burning or itching; no significant pruritus
- Variants:
- Periorificial dermatitis — when the nose, eyes, or groin are also involved
- Granulomatous perioral dermatitis — larger, coalescing granulomatous papules; more severe; rarely scars
- Facial Afro-Caribbean Eruption (FACE) — a granulomatous sarcoidal variant with additional involvement of upper eyelids and ear helices
Pathogenesis & Triggers
The exact cause is not fully understood, but several triggers are established:
| Trigger | Notes |
|---|---|
| Fluorinated topical corticosteroids | Most common identified cause (creams, ointments, inhalers) |
| Fluoride in dentifrices | Implicated in some cases |
| Inhaled corticosteroids | Can cause perinasal distribution |
| Demodex mites | Suspected role in some cases (responds to antiparasitic agents) |
| Cosmetic/occlusive products | Lip balms, heavy moisturizers |
Histologically, it resembles rosacea — perifollicular and perivascular lymphohistiocytic infiltrate, with variable perifollicular granulomas.
Differential Diagnosis
| Condition | Distinguishing Feature |
|---|---|
| Acne vulgaris | Comedones present; no lip-sparing zone |
| Rosacea | Flushing, telangiectasia; mid-face distribution |
| Contact/irritant dermatitis | Pruritus; exposure history |
| Seborrheic dermatitis | Greasy scale; nasolabial fold involvement |
| Demodex folliculitis | May overlap; responds to ivermectin |
Treatment
Step 1 — Remove the trigger
- Discontinue topical or inhaled fluorinated corticosteroids
- Avoid occlusive cosmetics and fluoride toothpaste if implicated
Step 2 — Pharmacotherapy
| Agent | Route | Notes |
|---|---|---|
| Doxycycline | Oral | First-line in adults |
| Metronidazole | Topical | Effective; well tolerated |
| Azelaic acid | Topical | Anti-inflammatory |
| Adapalene | Topical | Retinoid; useful adjunct |
| Ivermectin | Topical | Especially if Demodex suspected |
| Tacrolimus 0.1% or Pimecrolimus 1% | Topical | Calcineurin inhibitors — prevent rebound flare after stopping steroids |
| Erythromycin | Oral | Preferred in children |
Critical point: Do NOT use topical corticosteroids to treat perioral dermatitis — they will initially suppress but ultimately worsen the eruption (steroid-induced perioral dermatitis).
Sources: Fitzpatrick's Dermatology, p. 1484; Andrews' Diseases of the Skin, p. 296
Perioral dermatitis with itching and redness also spread to limbs what is the treatment
Finding Sources
Finding Sources
Searching PubMed
perioral dermatitis disseminated treatment doxycycline
Reading File
Finding Sources
Searching PubMed
perioral dermatitis systemic treatment tetracycline
Reading File
Important Clinical Note First
The presentation you describe — perioral dermatitis + itching + spread to limbs — warrants a diagnostic pause. Classic perioral dermatitis is typically confined to the face, minimally itchy, and does not spread to limbs. Extension to the extremities and trunk is atypical and shifts the differential. The textbooks specifically note that truncal and extremity involvement is uncommon and, when present, suggests the granulomatous/disseminated periorificial variant, or an alternative diagnosis should be considered.
Reassessing the Differential
Before treating, consider these alternative or co-existing diagnoses:
| Condition | Key features |
|---|---|
| Disseminated/granulomatous periorificial dermatitis | Face + trunk + limbs; more common in children but reported in adults |
| Atopic dermatitis | Pruritic; flexural; perioral involvement possible |
| Contact/irritant dermatitis | Exposure history; itching prominent |
| Seborrheic dermatitis | Greasy scale; scalp/nasolabial involvement |
| Demodex folliculitis | Perifollicular; face + body possible |
| Rosacea | Flushing; telangiectasia; less body involvement |
| Lupus miliaris disseminatus faciei | Granulomatous; can extend beyond face |
Treatment — Stepped Approach
Step 1 — Eliminate triggers (mandatory first step)
- Stop all topical/inhaled fluorinated corticosteroids — these are the most common cause and perpetuate the eruption
- Discontinue fluoride toothpaste if suspected
- Remove occlusive cosmetics, heavy moisturizers, lip balms
In mild steroid-induced cases, stopping the steroid alone may resolve the eruption.
Step 2 — Topical therapy (mild–moderate disease, face-limited)
| Agent | Formulation | Notes |
|---|---|---|
| Metronidazole | 0.75–1% gel or cream | First-line topical |
| Azelaic acid | 15–20% cream | Anti-inflammatory + antibiotic |
| Ivermectin | 1% cream | Especially if Demodex suspected |
| Clindamycin | 1% gel/lotion | Topical antibiotic |
| Erythromycin | 2% gel | Alternative topical antibiotic |
| Sodium sulfacetamide | Lotion | Useful adjunct |
| Pimecrolimus 1% or Tacrolimus 0.1% | Cream/ointment | Calcineurin inhibitors — bridge during steroid withdrawal to prevent rebound flare |
⚠️ Never use topical corticosteroids — they provide initial relief but worsen and prolong the condition.
Step 3 — Systemic therapy (moderate–severe, disseminated, refractory)
For adults with involvement spreading to limbs or refractory facial disease:
| Agent | Dose | Notes |
|---|---|---|
| Doxycycline | 50–100 mg once or twice daily | First-line systemic in adults; typically 6–12 weeks |
| Tetracycline | 500 mg twice daily | Alternative; avoid in pregnancy |
| Azithromycin | Weekly pulsed dosing | If tetracyclines not tolerated |
| Oral ivermectin | Weight-based dosing | For disseminated/Demodex-driven cases |
| Prednisone + dapsone | Combination | Reserved for severe granulomatous disseminated variant |
| Cyclosporine | Short course | Reported in resistant cases |
Step 4 — Address the itching
Pruritus is not a classic feature of perioral dermatitis. If itching is prominent, consider:
- Oral antihistamines (e.g. cetirizine, fexofenadine) for symptomatic relief
- Topical tacrolimus/pimecrolimus — reduce inflammation without steroid risk
- Re-evaluate for atopic or contact dermatitis as an alternative or co-existing diagnosis
Summary Treatment Algorithm
Spread to limbs + itching?
↓
Rule out atopic/contact dermatitis
↓
Stop all steroids + triggers
↓
Oral doxycycline 100 mg/day (adults)
+ Topical metronidazole or ivermectin to face
+ Pimecrolimus/tacrolimus during steroid withdrawal
↓
Refractory/granulomatous disseminated?
→ Consider oral ivermectin, dapsone ± short-course prednisone, or cyclosporine
Sources: Fitzpatrick's Dermatology, p. 1484–1485; Andrews' Diseases of the Skin, p. 296–297
This is a shared conversation. Sign in to Orris to start your own chat.