Newborn phenomenon of hemangioma in eye
Reading File
search_medical_text
infantile hemangioma periocular eyelid newborn
search_medical_image
periocular infantile hemangioma eyelid newborn
GradeResponse
GradeResponse
Periocular Infantile Hemangioma in Newborns
Overview
Infantile hemangioma (IH) is the most common benign vascular tumor of infancy, occurring in approximately 4–10% of infants. When it involves the periocular region (eyelids, orbit, or surrounding structures), it carries unique clinical significance due to the risk of vision-threatening complications.
Natural History / "Phenomenon"
IH follows a characteristic triphasic course:
| Phase | Timing | Description |
|---|---|---|
| Proliferative | Birth – 12 months (peak 3–5 mo) | Rapid growth; lesion enlarges quickly |
| Plateau | 12–18 months | Growth stabilizes |
| Involution | 18 months – 10 years | Gradual spontaneous regression (~50% by age 5, ~70% by age 7) |
Key point: Most IHs are not visible at birth — they appear within the first 2–4 weeks of life as a faint macule or telangiectatic patch, then proliferate rapidly. This is why they are called a "newborn phenomenon."
Classification by Depth
| Type | Appearance | Eye Relevance |
|---|---|---|
| Superficial | Bright red, "strawberry" surface | Eyelid skin |
| Deep | Bluish, subcutaneous | Orbital / retrobulbar |
| Mixed | Combined superficial + deep | Common in periocular region |
Periocular Location — Why It Matters
The periocular site is considered high-risk because of potential complications:
-
Amblyopia (most feared complication)
- Deprivation amblyopia — eyelid hemangioma causes ptosis occluding the visual axis
- Anisometropic amblyopia — mass effect induces astigmatism, disrupting refractive development
- Strabismic amblyopia — orbital involvement displaces the globe
-
Proptosis — retrobulbar (orbital) hemangiomas can push the eye forward
-
Optic nerve compression — large orbital lesions may cause disc edema and permanent vision loss
-
Exposure keratopathy — incomplete eyelid closure damages the cornea
Clinical Features
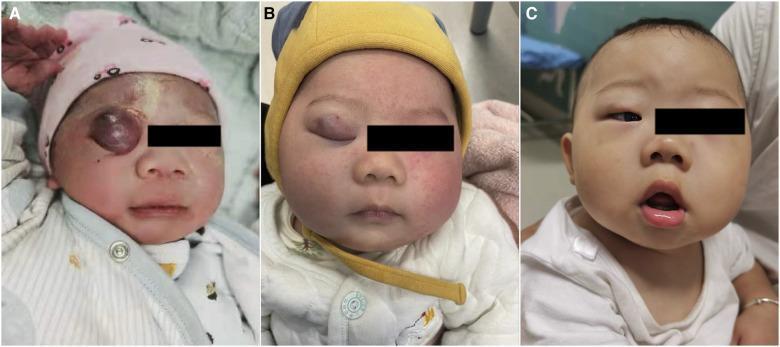
- Appears as a raised, well-circumscribed, purplish-red vascular mass on the upper eyelid
- Upper eyelid involved more commonly than lower
- May extend into the orbit (deep component not visible externally)
- Associated findings: PHACE syndrome (Posterior fossa malformations, Hemangiomas, Arterial anomalies, Cardiac defects, Eye anomalies) in large facial/periocular IH
Diagnosis
- Primarily clinical based on characteristic appearance and growth pattern
- Ultrasound with Doppler: high-flow vascular lesion; useful to assess depth
- MRI orbit: gold standard for orbital extension; shows T2-bright lobulated mass with flow voids
- Ophthalmologic evaluation: visual acuity testing, refraction (cycloplegic), cover testing, fundus exam
Management
Treatment is indicated when there is visual axis compromise, amblyopia risk, or rapid growth.
First-Line: Oral Propranolol
- Beta-blocker; works via vasoconstriction, reduced angiogenesis, and induction of apoptosis
- Dose: 1–3 mg/kg/day in divided doses
- Duration: typically continued until 12–18 months of age
- Monitor: hypoglycemia, bradycardia, bronchospasm
Other Options
| Treatment | Use Case |
|---|---|
| Topical timolol (0.5% gel) | Small, superficial, non-vision-threatening lesions |
| Intralesional corticosteroids | Localized, well-defined lesions; risk of central retinal artery occlusion |
| Intralesional sclerosants (e.g., lauromacrogol) | Combined with propranolol as shown in the image above |
| Systemic corticosteroids | Second-line if propranolol contraindicated |
| Surgical excision | Residual fibrofatty tissue post-involution; rarely primary treatment |
| Amblyopia therapy | Patching of the fellow eye to stimulate visual development |
Prognosis
- With early treatment, the majority of periocular IHs respond well — the image above demonstrates near-complete resolution at 6 months.
- Amblyopia is preventable with early detection and treatment; untreated cases can lead to permanent visual loss.
- Residual skin changes (telangiectasia, fibrofatty tissue, redundant skin) may persist after involution in ~40% of cases.
- Regular ophthalmologic follow-up is essential through early childhood to monitor for and treat amblyopia.
Key Takeaway
Periocular infantile hemangioma is a benign but potentially vision-threatening newborn vascular tumor. Early identification and prompt treatment — primarily with oral propranolol — are critical to preserving visual development and preventing amblyopia.
This is a shared conversation. Sign in to Orris to start your own chat.