Plantar wart causes and treatment
Reading File
search_medical_text
plantar wart etiology HPV causes pathophysiology
search_medical_text
plantar wart treatment management options
search_medical_image
plantar wart verruca plantaris clinical appearance
GradeResponse
GradeResponse
GradeResponse
Plantar Warts (Verruca Plantaris)
Causes & Pathophysiology
Plantar warts are cutaneous lesions caused by Human Papillomavirus (HPV) — a double-stranded DNA virus with over 100 known types. The subtypes most commonly responsible for plantar warts are HPV-1, HPV-2, and HPV-4.
How infection occurs:
- HPV enters through minor breaks or abrasions in the plantar skin (sole of the foot)
- Transmission is facilitated by direct contact with contaminated surfaces — communal showers, swimming pools, locker rooms, and gymnasiums are common sources
- Risk factors include walking barefoot in public areas, hyperhidrosis (sweaty feet), immunosuppression, and skin trauma
Pathophysiology:
- The virus infects keratinocytes in the basal epidermis, driving epidermal hyperplasia, papillomatosis, and hyperkeratosis
- Because plantar warts are endophytic (grow inward due to pressure from walking), they are covered by thick keratin and may be painful
- Paring the wart reveals a central core of keratinized debris and punctate bleeding points (thrombosed capillaries — the characteristic "black dots")
(Harrison's Principles of Internal Medicine, 21st ed., p. 1545)
Clinical Appearance
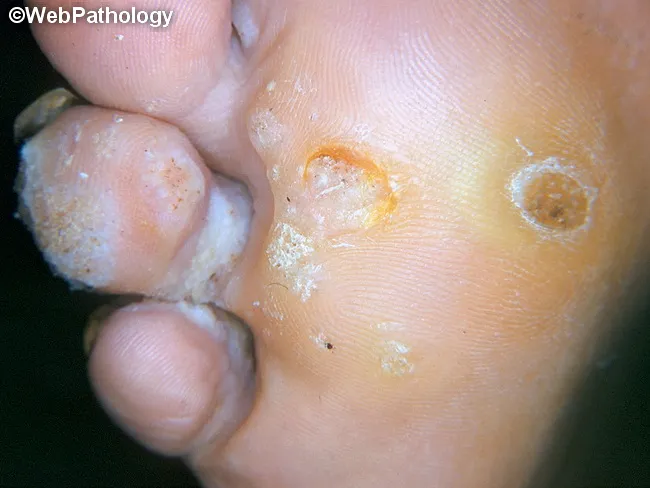
Verruca plantaris: endophytic, hyperkeratotic lesion with punctate black dots representing thrombosed capillaries. (webpathology.com)
Key Features That Distinguish Plantar Warts
| Feature | Plantar Wart | Callus/Corn |
|---|---|---|
| Black dots (thrombosed capillaries) | Present | Absent |
| Pain on lateral squeeze | Yes | No (pain with direct pressure) |
| Skin line interruption | Yes | No (lines continue through) |
| Endophytic growth | Yes | Yes |
| HPV etiology | Yes | No |
Treatment
No single therapy is universally effective. Importantly, most warts in immunocompetent individuals resolve spontaneously within 1–2 years, which should be factored into treatment decisions. (Harrison's, p. 1546)
| Treatment | Details | Effectiveness |
|---|---|---|
| Watchful waiting | Reasonable for asymptomatic warts in children | ~65% resolve in 2 years |
| Salicylic acid (keratolytic) | 17–40% topical preparations or plasters applied daily after soaking; requires consistent patient compliance over weeks | Equivalent to cryotherapy for many warts |
| Cryotherapy (liquid nitrogen) | In-office application every 2–3 weeks; causes blister formation and tissue destruction | Most convenient; first-line in office settings |
| Duct tape occlusion | Applied continuously, changed weekly; evidence is modest | Used in children or as adjunct |
| Intralesional bleomycin | Injected directly into resistant warts; reserved for recalcitrant lesions | Effective for refractory cases |
| Laser therapy (CO₂ or pulsed dye) | Vaporizes wart tissue; used for widespread or recalcitrant lesions | Effective but more expensive |
| Immunotherapy (imiquimod, intralesional Candida antigen) | Stimulates local immune response; useful in immunocompetent patients with resistant warts | Good for multiple/recurrent lesions |
| Surgical excision/curettage | Reserved for large, resistant warts; risk of scarring on the plantar surface | Effective but scar may be painful |
(Harrison's Principles of Internal Medicine, 21st ed., p. 1546)
Practical Tips
- Soak the foot in warm water for 5–10 minutes before applying salicylic acid; pare down dead tissue with an emery board
- Cryotherapy is the most practical first-line office treatment — apply for 10–20 seconds per cycle, 2–3 sessions usually needed
- Immunosuppressed patients (HIV, transplant recipients) tend to have more extensive, treatment-resistant disease and require aggressive management
- Prevention: wear footwear in communal areas, keep feet dry, avoid direct contact with others' warts
This is a shared conversation. Sign in to Orris to start your own chat.