Patient having complain with red patches over body suddenly
Reading File
search_medical_text
sudden red patches on skin differential diagnosis causes
search_medical_text
erythematous skin rash acute onset evaluation management
search_medical_image
red patches skin rash erythema
GradeResponse
GradeResponse
GradeResponse
Here is a comprehensive clinical overview of a patient presenting with sudden red patches over the body:
Sudden Red Patches Over the Body — Clinical Approach
Key Definitions
| Term | Meaning |
|---|---|
| Macule | Flat color change < 1 cm |
| Patch | Flat color change > 1 cm |
| Erythema | Redness due to vascular dilatation (blanches on pressure) |
| Purpura/Petechiae | Red spots that do NOT blanch — indicates bleeding into skin |
First Step: Press a glass on the red patch. If it blanches → vascular/inflammatory. If it does NOT blanch → hemorrhagic (medical emergency).
Differential Diagnosis
🔴 Non-Blanching (Urgent — Rule Out First)
| Condition | Key Features |
|---|---|
| Meningococcemia | Fever, petechiae → purpura, meningeal signs, sepsis |
| Vasculitis (e.g., HSP/IgA vasculopathy) | Palpable purpura, lower limbs, joint pain, abdominal pain |
| Thrombocytopenic purpura (ITP/TTP) | Widespread petechiae, low platelet count |
| Disseminated Intravascular Coagulation (DIC) | Critically ill patient, multi-organ failure |
| Rocky Mountain Spotted Fever | Tick exposure, starts at wrists/ankles, spreads centrally |
🔶 Blanching Red Patches (Inflammatory / Allergic)
| Condition | Key Features |
|---|---|
| Urticaria (Hives) | Raised, itchy wheals, migratory, resolves within 24 hrs |
| Drug Reaction / Morbilliform rash | Starts trunk, spreads outward, recent new medication |
| Viral Exanthem | Fever + rash (measles, rubella, roseola, EBV, COVID-19) |
| Erythema Multiforme | Target lesions, palms/soles involved, triggered by HSV or drugs |
| Scarlet Fever | Sandpaper texture, strawberry tongue, follows strep throat |
| Contact Dermatitis | Localized to exposed area, intense itching, allergen history |
| Psoriasis (acute guttate) | Drop-like red plaques with silvery scale, post-strep |
| Systemic Lupus Erythematosus | Malar (butterfly) rash, photosensitivity, joint pain |
| Lyme Disease (Erythema Migrans) | Expanding ring/bullseye lesion after tick bite (Harrison's, p. 5381) |
| Cellulitis | Unilateral, warm, tender, spreading erythema with fever |
⚠️ Severe Cutaneous Adverse Reactions (SCARs) — Emergencies
Per Management of Immune-Related Adverse Events (p. 4):
- Stevens-Johnson Syndrome (SJS) — mucosal involvement, skin detachment < 10%
- Toxic Epidermal Necrolysis (TEN) — > 30% skin detachment, life-threatening
- DRESS Syndrome — Drug Reaction with Eosinophilia and Systemic Symptoms; fever, lymphadenopathy, organ involvement
- AGEP (Acute Generalized Exanthematous Pustulosis) — pustular rash, fever
Clinical Image
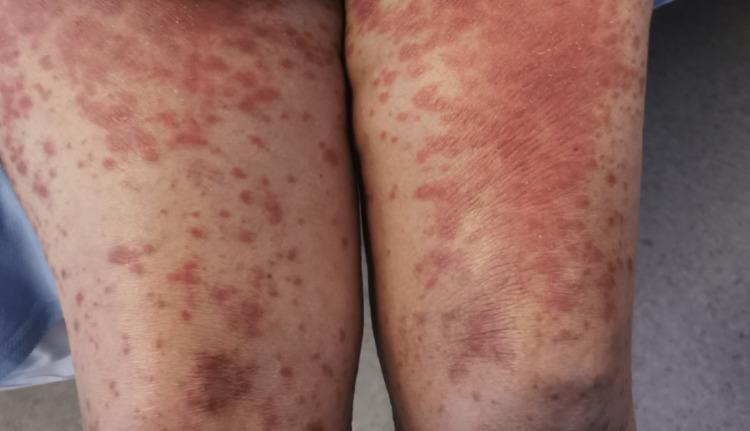
Widespread erythrodermic maculopapular eruptions with confluent red patches, surface scale, excoriation marks, and post-inflammatory hyperpigmentation — consistent with severe inflammatory dermatosis or drug eruption.
Initial Evaluation
History (must ask):
- Duration and onset (sudden vs gradual)
- Distribution — where did it start? Where is it now?
- Blanching or non-blanching?
- Fever, chills, malaise (systemic illness?)
- Recent new medications (within 2–8 weeks)
- Recent infections (URI, sore throat, viral illness)
- Tick/insect bite exposure
- Travel history
- Itching vs burning vs painless
- Mucosal involvement (mouth, eyes, genitals)?
Physical Exam:
- Vital signs (fever → infectious/inflammatory; hypotension → sepsis)
- Morphology of lesion (macule, papule, vesicle, purpura)
- Distribution (localized vs generalized, centripetal vs centrifugal)
- Mucosal exam (SJS/TEN red flag)
- Lymphadenopathy, hepatosplenomegaly
Investigations:
| Test | Purpose |
|---|---|
| CBC with differential | Thrombocytopenia, eosinophilia, infection |
| CRP, ESR | Inflammation |
| Blood cultures | Meningococcemia, sepsis |
| LFTs, renal function | DRESS syndrome, systemic involvement |
| Skin biopsy | When diagnosis unclear |
| ANA, anti-dsDNA | If SLE suspected |
| Throat swab / ASOT | If scarlet fever / guttate psoriasis |
| Coagulation profile | DIC |
Management Principles
| Category | Management |
|---|---|
| Non-blanching / purpuric | URGENT — admit, blood cultures, IV antibiotics (ceftriaxone if meningococcemia suspected), hematology consult |
| Drug reaction (mild) | Withdraw offending drug, antihistamines, topical steroids |
| SJS/TEN | STOP causative drug immediately, ICU/burns unit, supportive care, ophthalmology consult |
| Urticaria | Antihistamines (cetirizine/loratadine), epinephrine if anaphylaxis |
| Viral exanthem | Supportive care, antipyretics |
| Cellulitis | Antibiotics (amoxicillin-clavulanate or cloxacillin; IV if severe) |
| SLE | Hydroxychloroquine, steroids, rheumatology referral |
| Contact dermatitis | Avoid allergen, topical corticosteroids |
Red Flag Signs Requiring Immediate Action
- 🚨 Non-blanching rash + fever → rule out meningococcemia
- 🚨 Mucosal erosions + skin peeling → SJS/TEN
- 🚨 Rash + hypotension/tachycardia → anaphylaxis or sepsis
- 🚨 Rash + thrombocytopenia + neurological signs → TTP
Clinical Pearl: The combination of fever + non-blanching rash should be treated as meningococcemia until proven otherwise — do not delay antibiotics waiting for investigations.
Sudden red patches on skin.Advice treatment
search_medical_text
urticaria hives treatment management antihistamines
search_medical_image
urticaria hives wheals red patches legs
GradeResponse
GradeResponse
Clinical Assessment
Looking at the image, the findings are:
- Large, confluent erythematous (red) patches covering the lower leg
- Central pallor / pale areas within the red patches (classic "wheal with central clearing")
- Well-demarcated, irregular borders
- No visible blistering, skin peeling, or purpura
Most Likely Diagnosis: Acute Urticaria (Hives)
The image is highly consistent with acute urticaria — raised erythematous wheals with central pallor, sudden onset, on the lower extremity.
Reference image for comparison:
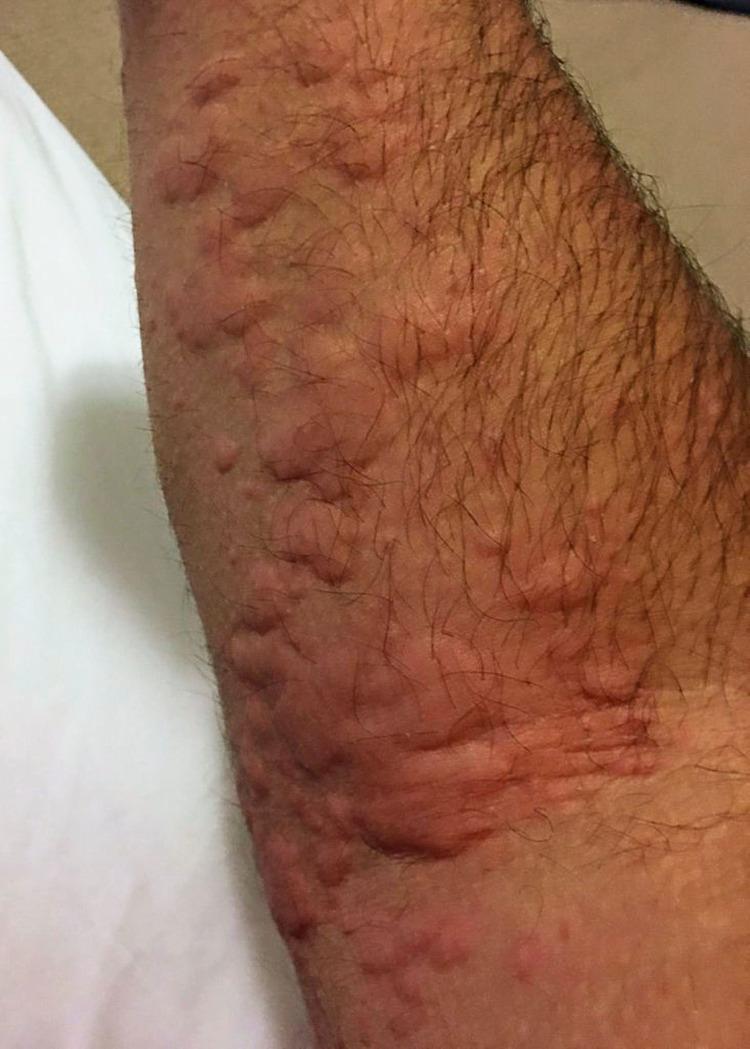
Treatment Plan
Step 1 — First-Line: Antihistamines
| Drug | Dose | Route | Frequency |
|---|---|---|---|
| Cetirizine 10 mg | 10 mg | Oral | Once daily |
| Loratadine 10 mg | 10 mg | Oral | Once daily |
| Fexofenadine 120/180 mg | 180 mg | Oral | Once daily |
| Chlorpheniramine (if sedation acceptable) | 4 mg | Oral | 3–4× daily |
If response is inadequate after 2 weeks, up-dose non-sedating antihistamines up to 4× the standard dose before adding other agents.
Step 2 — If Severe or Rapidly Spreading: Short-Course Oral Corticosteroids
| Drug | Dose | Duration |
|---|---|---|
| Prednisolone | 0.5–1 mg/kg/day | 3–5 days (taper) |
| Methylprednisolone | 16–32 mg/day | 3–5 days |
Steroids are not for long-term use in urticaria — use only for acute flares.
Step 3 — If Anaphylaxis Signs Present (Throat tightness, Hypotension, Dyspnea) 🚨
- Epinephrine (Adrenaline) 0.3–0.5 mg IM (anterolateral thigh) — IMMEDIATELY
- Call emergency services
- IV fluids, oxygen, antihistamines IV
Topical Supportive Care
- Calamine lotion — apply to affected areas for soothing effect
- Cold compress — reduces local swelling and itch
- Avoid hot showers (worsens histamine release)
Identify and Remove the Trigger
Ask the patient about:
| Category | Examples |
|---|---|
| Foods | Shellfish, nuts, eggs, strawberries, food additives |
| Drugs | Aspirin, NSAIDs, ACE inhibitors, antibiotics (penicillin) |
| Infections | Recent URTI, viral illness, parasites |
| Physical triggers | Cold, heat, pressure, exercise |
| Insect bite/sting | Bee, wasp, mosquito |
| Contact | Latex, cosmetics, plants |
Follow-Up & When to Refer
| Scenario | Action |
|---|---|
| Resolves within 6 weeks | Acute urticaria — no further workup needed |
| Persists > 6 weeks | Chronic urticaria — refer to dermatologist/allergist |
| Recurrent episodes | Allergy testing, IgE levels, CBC, thyroid function |
| Associated angioedema | Urgent evaluation — consider C1-esterase inhibitor deficiency |
⚠️ Important: Check if the wheals blanche on pressure — urticaria blanches. If they do NOT blanche, reconsider vasculitis or purpura and investigate further. Always monitor for signs of angioedema (lip/tongue swelling, throat tightening) which requires emergency management.
This is a shared conversation. Sign in to Orris to start your own chat.