Macular rashes with itching over neck and forearm diagnosis and management
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Finding Sources
Searching Images
macular rash neck forearm contact dermatitis urticaria
I have comprehensive information. Let me compile the full response now, covering differential diagnosis and management of macular rash with itching over neck and forearm.
Macular Pruritic Rash over Neck and Forearm — Diagnosis & Management
Differential Diagnosis
Macular rashes with pruritus over the neck and forearm are most commonly caused by the following conditions:
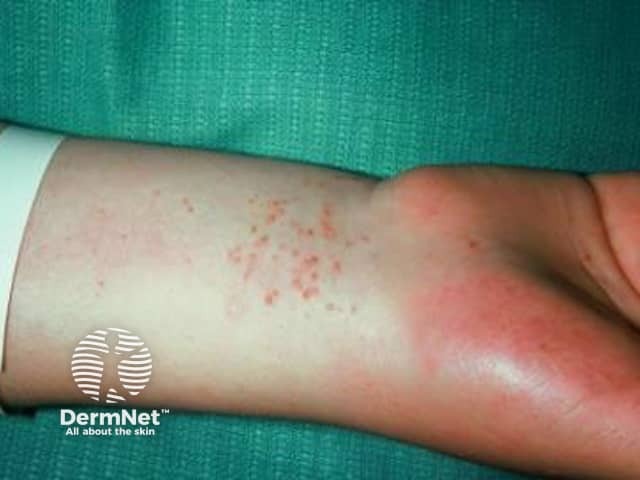
1. Allergic Contact Dermatitis (ACD) — Most Likely
Pathophysiology: Type IV (delayed-type) hypersensitivity mediated by sensitized T-lymphocytes (Th2-mediated). Requires prior sensitization; reaction appears hours to days after re-exposure.
Common allergens for neck/forearm distribution:
- Neck: Jewelry (nickel — the most common allergen, 19.5%), perfumes/cosmetics, clothing dyes, hair dye (p-phenylenediamine)
- Forearm: Watches/bracelets (nickel, cobalt), rubber/latex gloves, topical medications (neomycin, bacitracin), plants (Toxicodendron — poison ivy/oak/sumac), sunscreen chemicals
Clinical features:
- Erythematous macules/papules, vesicles on an erythematous base
- Streaky, linear, intensely pruritic lesions in the area contacting the allergen
- Eruption may appear within hours to days of exposure
- Distribution mirrors the contact area
Diagnosis: Careful exposure history; patch testing is the gold standard for identifying the causative allergen.
2. Irritant Contact Dermatitis (ICD)
Pathophysiology: Direct chemical/physical damage to the skin barrier — not immune-mediated. Given sufficient exposure, anyone can develop ICD.
Common irritants: Soaps, detergents, cleansers, hand sanitizers, water (repeated wet-work), industrial solvents.
Clinical features: Erythema, scaling, vesicles, bullae, crusting — identical to ACD in appearance. Both can coexist. Intensely pruritic.
Key distinction from ACD: ICD typically confined to irritant-exposed skin; ACD can spread beyond contact zone.
3. Urticaria (Hives)
Pathophysiology: Mast cell degranulation releasing histamine, bradykinin, kallikrein. Immunologic (IgE-mediated) or non-immunologic mechanisms.
Triggers:
- Drugs: Penicillin, aspirin, NSAIDs, narcotics
- Foods: Seafood, tree nuts, eggs, strawberries, lobster
- Infections: Rhinovirus, hepatitis, mononucleosis, coxsackievirus; Candida, dermatophytes
- Contact with textiles, animal dander, topical agents, plants
Clinical features:
- Raised, circumscribed, erythematous wheals — often annular and transient/migratory
- Any skin surface can be affected, including neck and forearms
- Acute (<4–6 weeks) vs. Chronic (>6 weeks; more common in women 40s–50s)
- In >50% of chronic urticaria, no etiology is found (idiopathic/autoimmune)
4. Pityriasis Rosea
- Begins as a "herald patch" then spreads as oval, salmon-pink macules in a Christmas-tree distribution on the trunk — but can affect neck and arms
- Mild pruritus, self-limiting (resolves in 6–8 weeks)
5. Atopic Dermatitis (Eczema)
- Chronic, relapsing pruritic macules/papules on flexural surfaces (cubital fossae of forearm) and neck
- Associated with personal/family history of atopy (asthma, rhinitis)
6. Drug Eruption / Morbilliform Rash
- Macular or maculopapular rash appearing 7–21 days after starting a new medication (antibiotics, anticonvulsants, NSAIDs)
- Symmetric, widespread — but can be localized early
Diagnostic Approach
| Step | Action |
|---|---|
| History | New exposures (jewelry, cosmetics, topical agents, plants, medications, foods), occupation, atopic history, timeline of rash |
| Physical exam | Morphology (macule vs. papule vs. wheal), distribution, linearity, border definition |
| Patch testing | Gold standard for ACD allergen identification |
| Skin prick / RAST | For suspected IgE-mediated urticaria (via allergy specialist) |
| Blood tests | CBC, ESR, IgE, thyroid antibodies in chronic urticaria workup |
| Skin biopsy | When diagnosis is unclear or refractory |
Management
Contact Dermatitis (Allergic & Irritant)
- Avoidance — identify and remove the causative agent (essential, primary treatment)
- Skin washing — wash skin and clothing with soap and water as soon as possible after exposure (especially plant allergens)
- Cool wet compresses — aluminum acetate (Domeboro/Burow's solution) for oozing/vesiculated lesions; cool soaks 10–15 min
- Topical corticosteroids:
- Low-potency (hydrocortisone) around orifices and face
- Mid-potency (triamcinolone 0.1% cream BD × 1 week) for neck and forearm
- Superpotent (clobetasol 0.05%) for plant-contact ACD
- Note: Topical steroids are ineffective on blistered areas
- Barrier protection — petrolatum ointment, protective gloves for ICD
- Oral antihistamines for pruritus:
- Sedating (hydroxyzine, diphenhydramine) — nighttime
- Non-sedating (cetirizine, loratadine, fexofenadine) — daytime preferred
- Systemic corticosteroids (oral prednisone) — for severe/extensive ACD (e.g., widespread poison ivy); short course only
- Treat secondary infection if present (antibacterial cream or systemic antibiotics)
Urticaria
- Avoidance of triggers — cornerstone of management
- Antihistamines (first-line):
- 2nd/3rd generation (cetirizine, loratadine, fexofenadine, levocetirizine, desloratadine) — daytime; can up-titrate to 4× normal daily dose
- 1st generation (diphenhydramine, hydroxyzine, doxepin) — nighttime
- H2 antagonists (famotidine, cimetidine) — adjunctive
- Leukotriene antagonists (montelukast) — adjunctive
- Oral corticosteroids — short-term only for severe acute urticaria
- Omalizumab (anti-IgE) — for chronic spontaneous urticaria unresponsive to antihistamines
- Extensive workup in chronic urticaria unresponsive to antihistamines (thyroid, autoimmune, infectious causes)
Potency Guide for Topical Steroids (Neck & Forearm)
| Skin Location | Recommended Potency | Example |
|---|---|---|
| Neck (thin skin) | Class 4–5 (mid-strength) | Triamcinolone 0.1% cream |
| Forearm | Class 3–4 | Betamethasone valerate 0.1% |
| Severely affected forearm (ACD) | Class 1–2 (superpotent, short course) | Clobetasol 0.05% cream |
When to Refer
- Persistent or recurrent rash despite treatment → Dermatology for patch testing
- Chronic urticaria >6 weeks unresponsive to antihistamines → Allergy/Immunology
- Suspected systemic cause (autoimmune, malignancy) → Internal Medicine/Rheumatology
Sources: Rosen's Emergency Medicine, 10e; Textbook of Family Medicine, 9e; Goldman-Cecil Medicine, 26e; Andrews' Diseases of the Skin; Dermatology 2-Volume Set, 5e
Similar type lesions
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Searching Images
miliaria rubra prickly heat rash neck papules erythematous
Excellent — the clinical picture is now clear. Here is the analysis:
Clinical Analysis of the Images
Image 1 (Light skin — neck/upper shoulder):
Multiple tiny, discrete erythematous papules and micropustules densely clustered over an erythematous base, affecting the neck and upper chest/shoulder. The lesions are 1–3 mm, uniform, and non-confluent with a "goosebump-like" studded appearance.
Image 2 (Dark skin — posterior neck):
Fine, subtle papular eruption with slight scaling over the posterior neck, partially obscured by a necklace. The skin appears mildly thickened/rough with hyperpigmentation.
Most Likely Diagnosis: Miliaria Rubra (Prickly Heat / Heat Rash)
The morphology, distribution (neck, upper trunk, clothed/occluded areas), and the dense studded papular/papulopustular pattern are classic for miliaria rubra.
Pathophysiology
Obstruction of the eccrine sweat duct at the mid-epidermal level → sweat retention within the duct → rupture into the malpighian layer → inflammatory papules and vesicles on an erythematous base. Triggered by maceration of the stratum corneum from excessive sweating under occlusive clothing, hot/humid conditions, or fever.
Types of Miliaria (Classification)
| Type | Level of Obstruction | Lesion | Pruritus | Distribution |
|---|---|---|---|---|
| Crystallina | Stratum corneum | Clear, fragile 1 mm vesicles | No | Face, trunk |
| Rubra (this case) | Mid-epidermis | Pruritic, erythematous 1–3 mm papules ± pustules | Yes, intense | Neck, upper trunk |
| Profunda | Dermo-epidermal junction | Non-pruritic white papules | No | Trunk, proximal limbs |
Miliaria rubra specifically affects the neck and upper trunk — matching both images precisely. — Dermatology 2-Volume Set, 5e, Table 39.15
Management
Immediate/Primary
- Remove from hot/humid environment — move to cool, air-conditioned space (most important step; lesions resolve spontaneously)
- Loose, light, breathable clothing — cotton preferred; avoid synthetic or occlusive fabrics
- Avoid vigorous activity that induces sweating until resolved
- Cool water baths/showers — pat dry gently; do not rub
Symptomatic Relief
- Antihistamines — for pruritus relief (hydroxyzine or cetirizine)
- Calamine lotion — soothing, antipuritic topical application
- Topical mild corticosteroids — low-potency (hydrocortisone 1% cream) to reduce inflammation; short course only
- Topical anhydrous lanolin — may help re-open blocked ducts
- Oral Vitamin C — has been described as beneficial adjunctively
For Recurrent/Severe Cases
- 1% salicylic acid solution applied TID — assists in desquamating keratin plug blocking sweat ducts; particularly useful in miliaria profunda
- Chlorhexidine in light cream — reduces Staphylococcus colonization (S. aureus secondary infection is a common complication of miliaria)
Prevention
- Acclimatization to heat gradually
- Avoid tight/occlusive clothing over neck, trunk, axillae
- Regular cool showers in hot climates
- Antiperspirants are not appropriate here (worsen duct occlusion)
Differential Diagnoses to Consider
| Condition | Distinguishing Feature |
|---|---|
| Folliculitis | Perifollicular pustules, hair follicle-centered; ± Staphylococcal |
| Allergic contact dermatitis | History of allergen contact (jewelry, cosmetics); more polymorphic |
| Viral exanthem | Systemic symptoms (fever, malaise); widespread distribution |
| Atopic dermatitis | Chronic, flexural, personal/family atopy history |
| Scabies | Burrows, nocturnal itch, interdigital/flexural; close contacts affected |
Key Clinical Note
The necklace visible in Image 2 is important — if there is also a possibility of contact dermatitis to jewelry metal (nickel/cobalt), this should be co-investigated. In that case, patch testing would be appropriate if lesions persist despite cooling measures.
Sources: Tintinalli's Emergency Medicine; Dermatology 2-Volume Set, 5e (Miliaria section, Table 39.15); Harriet Lane Handbook, 23e
This is a shared conversation. Sign in to Orris to start your own chat.