third generation orthopaedic nails
Reading File
search_medical_text
third generation orthopaedic intramedullary nails design features
search_medical_text
intramedullary nail generations evolution femur tibia humerus
search_medical_image
intramedullary nail orthopaedic fixation generations
GradeResponse
GradeResponse
GradeResponse
The retrieval touched on third-generation hindfoot nails and general IMN use but didn't fully cover the generational evolution. Let me fill this comprehensively from retrieved sources and my own knowledge.
Third Generation Orthopaedic Nails
Historical Evolution of Intramedullary Nails
The concept of intramedullary fixation was pioneered by Gerhard Küntscher in the 1940s. Nails have evolved through three broadly recognized generations:
| Generation | Era | Key Features |
|---|---|---|
| 1st Generation | 1940s–1960s | Solid/slotted cloverleaf cross-section (Küntscher nail); no interlocking; required canal reaming; treated only isthmic fractures |
| 2nd Generation | 1970s–1980s | Proximal/distal interlocking screws; expanded indications to comminuted, proximal, and distal fractures; still required reaming |
| 3rd Generation | 1990s–present | Advanced locking mechanisms, multiplanar/angular stability, cannulated designs, multiple entry options, unreamed variants, nail-specific targeting jigs |
Third Generation Nails: Defining Features
Third generation nails represent a fundamental advance in biomechanical design and clinical versatility:
1. Locking Screw Geometry
- Multiple locking hole configurations: static, dynamic, oblique, and spiral blade options
- Angular stable interlocking (e.g., LISS-like locking within the nail) reduces toggle at the nail-screw interface
- Distal locking in two planes (AP and lateral) for rotational and length control
2. Nail Geometry and Material
- Hollow/cannulated shaft allowing guidewire-assisted insertion
- Optimized cross-sections (titanium alloy: Ti-6Al-4V) — lighter, more elastic modulus match to cortical bone
- Variable diameter along the length (proximal flare for metaphyseal fill)
- Antegrade and retrograde options for the same bone (e.g., femur)
3. Unreamed vs. Reamed Design
- Third generation introduced validated unreamed variants (e.g., Unreamed Tibial Nail — UTN), preserving endosteal blood supply
- Reamed versions allow larger diameter nails with improved rotational stability
4. Targeting and Instrumentation
- Nail-specific aiming arms and jigs for accurate distal locking, especially in long nails
- Radiolucent jig designs to reduce fluoroscopy time
Third Generation Nails by Anatomical Site
Femoral Nails
- Antegrade (piriformis or trochanteric entry): e.g., Synthes Expert Femoral Nail, TRIGEN INTERTAN, Stryker T2 Femoral Nail
- Retrograde femoral nails: inserted through the knee; useful in obesity, bilateral femur fractures, polytrauma
- Cephalomedullary nails (e.g., Gamma3, PFNA — Proximal Femoral Nail Antirotation): treat peritrochanteric and subtrochanteric fractures; feature a helical blade or lag screw into the femoral head
Tibial Nails
- e.g., Synthes Expert Tibial Nail, Stryker T2 Tibial Nail
- Proximal locking in multiple planes addresses metaphyseal (proximal and distal) tibia fractures
- Suprapatellar entry option minimizes soft tissue disruption
Humeral Nails
- Antegrade (supraspinatus fossa) and retrograde (olecranon fossa) entry points
- Flexible/stacked nails (e.g., Ender nails) were second-generation; third generation adds interlocking for rotational stability
Hindfoot Fusion Nails (Third Generation)
- Fuse both the ankle (tibiotalar) and subtalar joints simultaneously in a single construct
- Inserted via open or arthroscopic technique (Bailey & Love's, p. 594)
- Indications: end-stage ankle and hindfoot arthritis, Charcot arthropathy, failed ankle arthroplasty
Key Biomechanical Concepts
| Concept | Relevance |
|---|---|
| Load sharing | Nail bears load cyclically; fracture healing gradually transfers load to bone |
| Static locking | All holes filled; prevents shortening and rotation — used for comminuted fractures |
| Dynamic locking | One end free; allows controlled axial micromotion promoting callus formation; used after early healing for delayed/non-union |
| Dynamization | Conversion from static to dynamic locking after 6–8 weeks to stimulate fracture healing |
| Nail-bone interface toggle | Third generation angular stable locking reduces this, improving stability in osteoporotic bone |
Clinical Advantages of Third Generation Nails
- Broader fracture indications: proximal, diaphyseal, and distal metaphyseal fractures
- Reduced operative time with improved targeting jigs
- Lower infection risk with unreamed/minimally invasive insertion
- Superior rotational control via multiplanar locking
- Applicable in osteoporosis — helical blade designs achieve better purchase than screws in cancellous bone (PFNA)
Example Implant: Fractured Gamma Nail
Below is a clinical photograph illustrating an explanted short Gamma intramedullary nail with fatigue fracture at the lag screw aperture — the mechanical weak point in earlier cephalomedullary designs, addressed in third generation redesigns:
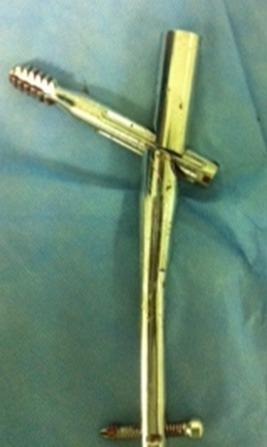
Explanted short Gamma nail fractured at the cephalic screw aperture. Third generation redesigns (Gamma3, PFNA) addressed this failure mode through geometry optimization and helical blade technology.
Summary
Third generation intramedullary nails are characterized by cannulated design, multiplanar interlocking, angular stability, material optimization (titanium), and expanded anatomical and fracture-type indications. They have largely replaced plating for diaphyseal long bone fractures and are the gold standard for peritrochanteric hip fractures via cephalomedullary designs. Ongoing fourth-generation concepts include smart nails with embedded sensors for real-time load monitoring and bioresorbable coatings for infection prophylaxis.
This is a shared conversation. Sign in to Orris to start your own chat.