Endometrial thickness with different conditions
Reading File
search_medical_text
endometrial thickness normal and abnormal conditions ultrasound
search_medical_image
endometrial thickness ultrasound different conditions
GradeResponse
GradeResponse
Here is a comprehensive overview of endometrial thickness (ET) across different physiological and pathological conditions.
Endometrial Thickness — Clinical Reference Guide
Measurement Technique
ET is measured by transvaginal ultrasound (TVUS) at the thickest portion, from echogenic border to echogenic border, perpendicular to the midline in the longitudinal plane of the uterus. (Performance of an Ultrasound Examination of the Female Pelvis, p. 3)
1. Normal Physiological Variations
Premenopausal (by menstrual cycle phase)
| Phase | ET (mm) | Sonographic Appearance |
|---|---|---|
| Menstrual (Days 1–4) | 2–4 | Thin, irregular, echogenic debris |
| Proliferative / Early (Days 5–9) | 5–7 | Thin, hypoechoic, triple-line sign |
| Periovulatory (Days 10–14) | 8–12 | Classic triple-line (trilaminar) pattern |
| Secretory / Luteal (Days 15–28) | 10–16 | Thick, hyperechoic, uniform |
Postmenopausal
| Status | Normal ET (mm) | Action Threshold |
|---|---|---|
| Asymptomatic | ≤ 11 mm | Routine follow-up |
| Asymptomatic | > 11 mm | Consider biopsy |
| With postmenopausal bleeding (PMB) | ≤ 4–5 mm | Low risk of malignancy; biopsy may not be needed |
| With PMB | > 4–5 mm | Endometrial biopsy indicated |
The 4–5 mm threshold in symptomatic postmenopausal women is widely accepted (ACOG, RCOG guidelines) with a sensitivity of ~90–96% for endometrial carcinoma.
2. Pathological Conditions
| Condition | Typical ET (mm) | Key Features |
|---|---|---|
| Endometrial atrophy | < 4 | Thin, hyperechoic; most common cause of PMB |
| Endometrial polyp | Variable (focal thickening) | Echogenic, well-defined, with color Doppler feeding vessel |
| Submucosal fibroid | Variable | Hypoechoic, distorts cavity |
| Endometrial hyperplasia (simple) | 10–20 | Diffusely thickened, uniform, hyperechoic |
| Atypical endometrial hyperplasia (AEH) | ~8–20+ | Heterogeneous texture; may have posterior leiomyoma |
| Endometrial carcinoma | > 16–20 (often > 20) | Heterogeneous, irregular, +/- myometrial invasion |
| Endometritis | 4–10 | Irregular, with fluid/gas; clinical correlation needed |
| Retained products of conception (RPOC) | > 10–15 | Echogenic mass, hypervascularity on Doppler |
3. Special Clinical Scenarios
Hormone-Related Changes
| Scenario | ET |
|---|---|
| Hormone Replacement Therapy (HRT) — sequential | Up to 8 mm (end of progestogen phase) |
| HRT — continuous combined | ≤ 5 mm (stable) |
| Tamoxifen therapy | May appear up to 8–12 mm (artifactually thick due to subepithelial change — sonohysterography preferred) |
| OCP use | 4–8 mm (thinned, atrophic) |
| Clomiphene / Letrozole (ovulation induction) | ≥ 7 mm preferred for implantation |
Fertility / ART Context
| Status | Minimum ET for IVF | Optimal ET |
|---|---|---|
| IVF embryo transfer | ≥ 7 mm | 8–14 mm (triple-line pattern ideal) |
| ET < 7 mm | Associated with poor implantation | Cycle cancellation often considered |
4. Risk of Malignancy by ET (Postmenopausal Women with Bleeding)
| ET (mm) | Risk of Endometrial Cancer |
|---|---|
| ≤ 4 | ~1% |
| 5–8 | ~5–7% |
| 9–12 | ~10–12% |
| > 20 | Highly predictive of occult endometrial carcinoma |
An ET > 20 mm in patients with preoperative AEH is highly predictive of concurrent occult endometrial cancer (confirmed as stage pT1a G2 in the image below). (pmc_clinical_VQA)
Ultrasound Example: AEH vs. Endometrial Cancer
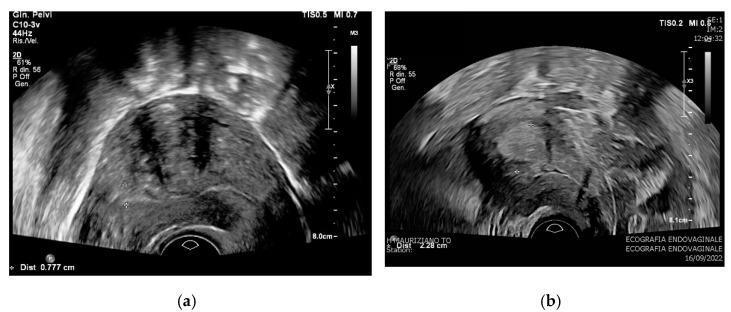
(a) ET = 7.77 mm — heterogeneous texture with posterior leiomyoma; preoperative diagnosis: AEH.
(b) ET = 22.8 mm — markedly thickened, echogenic, irregular; postoperative finding: stage pT1a G2 endometrial carcinoma.
Key Takeaways
- < 4 mm in a postmenopausal woman with bleeding = low malignancy risk (likely atrophy)
- > 4–5 mm with PMB = biopsy threshold
- > 20 mm = high suspicion for endometrial carcinoma regardless of symptoms
- Tamoxifen artificially thickens the apparent endometrium — sonohysterography is preferred in these patients
- In IVF, triple-line pattern with ET ≥ 8 mm is the goal for optimal implantation
Define menopause
search_medical_text
menopause definition diagnosis criteria
GradeResponse
Menopause is defined as the permanent cessation of menstruation resulting from the loss of ovarian follicular activity.
Clinical Definition
- Diagnosis: In a woman with an intact uterus, menopause is a clinical diagnosis based on the absence of menstruation for at least 12 consecutive months, with no other pathological or physiological cause. (Treatment of Symptoms of the Menopause, p. 6)
- The average age of natural menopause is 51 years (range: 45–55).
- Hormonal measurements (FSH, LH, estradiol, inhibin B, AMH) are not required to confirm the diagnosis in typical cases.
Clinical Spectrum
| Term | Definition |
|---|---|
| Perimenopause / Menopausal transition | Period leading up to menopause with irregular cycles + menopausal symptoms; begins years before the final period |
| Menopause | 12 months of amenorrhea after the final menstrual period (FMP) |
| Postmenopause | All time following the FMP |
| Premature menopause / POI | Menopause occurring before age 40 (premature ovarian insufficiency) |
| Early menopause | Menopause occurring between ages 40–45 |
| Surgical menopause | Abrupt menopause following bilateral oophorectomy |
| Induced menopause | Due to chemotherapy or pelvic radiation |
Hormonal Changes
| Hormone | Change at Menopause |
|---|---|
| Estradiol (E2) | Markedly decreased |
| FSH | Elevated (> 40 IU/L) |
| LH | Elevated |
| Inhibin B | Decreased |
| AMH | Very low / undetectable |
Hormonal testing is useful when the diagnosis is uncertain — e.g., in women who have had a hysterectomy (no menses to track), those under 40 (to diagnose POI), or those on hormonal contraception.
Common Symptoms
- Vasomotor: hot flushes, night sweats
- Genitourinary: vaginal dryness, dyspareunia, urinary urgency (GSM — genitourinary syndrome of menopause)
- Sleep disturbance, mood changes, cognitive symptoms
- Reduced libido
- Long-term: bone loss (osteoporosis), cardiovascular risk increase
What happens to the estrogen, progesterone, fish and lh levels in pcos
search_medical_text
PCOS estrogen progesterone FSH LH hormone levels
GradeResponse
I assume you meant FSH (not "fish") — here is a full breakdown of hormonal changes in PCOS.
Hormonal Changes in PCOS
Estrogen
- Estrone (E1) is elevated — due to peripheral conversion of androgens (androstenedione → estrone) in adipose tissue, particularly in overweight/obese women.
- Estradiol (E2) levels are typically in the low-to-normal follicular phase range, but there is a chronic, non-cyclic estrogen state — meaning estrogen is present continuously without the normal mid-cycle surge or luteal phase rise.
- There is no progesterone rise to oppose this estrogen, creating a state of unopposed estrogen — which increases the risk of endometrial hyperplasia and carcinoma.
Progesterone
- Decreased / Low — because ovulation does not occur (anovulation), the corpus luteum is not formed, so progesterone is not produced in the luteal phase.
- This results in irregular or absent menstruation (oligomenorrhea/amenorrhea).
FSH (Follicle-Stimulating Hormone)
- Low-normal or decreased relative to LH.
- FSH levels are insufficient to drive a dominant follicle to full maturity, leading to follicular arrest — multiple small antral follicles accumulate (the "polycystic" appearance on ultrasound).
LH (Luteinizing Hormone)
- Elevated — increased pulse frequency and amplitude of LH secretion from the pituitary.
- The classic finding is an elevated LH:FSH ratio (≥ 2:1 or ≥ 3:1), which is characteristic of PCOS, though not always present on a random measurement due to pulsatile secretion. (Harrison's Principles of Internal Medicine, 21st Ed., p. 11075)
- Elevated LH directly stimulates ovarian theca cells to produce excess androgens (testosterone, androstenedione).
Summary Table
| Hormone | Change in PCOS | Consequence |
|---|---|---|
| Estrone (E1) | Elevated | Unopposed estrogen effect on endometrium |
| Estradiol (E2) | Low-normal, non-cyclic | No mid-cycle LH surge; anovulation |
| Progesterone | Low (deficient) | Anovulation; irregular menses; endometrial hyperplasia risk |
| FSH | Low-normal / relatively low | Follicular arrest; no dominant follicle |
| LH | Elevated | Excess androgen production by theca cells |
| LH:FSH ratio | ≥ 2:1 (often ≥ 3:1) | Hallmark of PCOS |
| Testosterone | Mildly-moderately elevated | Hyperandrogenism (acne, hirsutism, alopecia) |
| Androstenedione | Elevated | Peripheral conversion to estrone |
| DHEAS | Mildly elevated (in ~50%) | Adrenal contribution to androgen excess |
| Insulin | Often elevated (insulin resistance) | Stimulates theca cells; reduces SHBG → more free testosterone |
The Core Hormonal Cascade in PCOS
↑ LH pulses
→ ↑ Theca cell androgen production (testosterone, androstenedione)
→ Peripheral conversion to estrone (↑ E1)
→ ↓ SHBG (especially with hyperinsulinemia) → ↑ free testosterone
→ Hyperandrogenism (clinical features)
→ Follicular arrest → anovulation → ↓ progesterone
→ Unopposed estrogen → endometrial hyperplasia risk
Causes for heavy menstrual bleeding and tender lateral fornix
search_medical_text
heavy menstrual bleeding causes differential diagnosis
search_medical_text
tender lateral fornix causes pelvic examination findings
GradeResponse
GradeResponse
The combination of heavy menstrual bleeding (HMB) + tender lateral fornix is a clinically significant pairing that points to a focused differential. The lateral fornix tenderness reflects pathology in the adnexa (ovaries, fallopian tubes, broad ligament, parametrium).
Top Diagnoses to Consider
1. Endometriosis / Adenomyosis (Most likely combined cause)
- Endometriosis causes HMB + dysmenorrhea + fornix tenderness — tender nodularity in the posterior/lateral fornix is a classic pelvic sign. (Endometriosis: Diagnosis and Management, p. 10)
- Adenomyosis (endometrial glands within myometrium) → bulky, tender uterus + heavy, painful periods.
- Ovarian endometrioma can cause adnexal/lateral fornix tenderness.
2. Pelvic Inflammatory Disease (PID)
- Adnexal tenderness (lateral fornix) + cervical motion tenderness are the hallmark examination findings of PID.
- Acute/subacute PID can cause menorrhagia due to endometritis.
- Associated features: purulent discharge, fever, raised CRP/WBC, history of STI.
3. Ectopic Pregnancy (Must exclude urgently)
- Lateral fornix/adnexal tenderness ± adnexal mass.
- Can present with abnormal uterine bleeding (usually not frank HMB, but irregular bleeding).
- Always check βhCG in any woman of reproductive age with pelvic pain + bleeding.
4. Ovarian Pathology
| Condition | HMB Mechanism | Fornix Tenderness |
|---|---|---|
| Ovarian cyst (functional/hemorrhagic) | Hormonal disruption | Ipsilateral lateral fornix |
| Ovarian torsion | Disrupts ovarian hormones | Acute, severe unilateral tenderness |
| Ovarian endometrioma | Endometriosis-related | Lateral/posterior fornix |
| Ovarian tumor | Estrogen-secreting tumors (granulosa cell) | Adnexal mass + tenderness |
5. Uterine Fibroids (Leiomyomata)
- Submucosal and intramural fibroids are a major cause of HMB.
- Large broad ligament or lateral fibroids can cause lateral fornix/adnexal tenderness on palpation.
6. Coagulopathy / Bleeding Disorders
- Von Willebrand disease (VWD), factor XI deficiency, platelet dysfunction, and hemophilia carriers are common and underdiagnosed causes of HMB. (Harrison's, p. 1837)
- Defined as blood loss > 80 mL/cycle; clinical predictors include clots > 1 inch, changing pads hourly, iron-deficiency anaemia.
- These would not explain lateral fornix tenderness — if present alongside bleeding, a concurrent pelvic pathology must be sought.
7. Parametritis / Pelvic Abscess
- Infection spreading to parametrium → lateral fornix tenderness.
- Can follow PID, instrumentation (IUD insertion, post-abortion), or appendicitis.
Differential Summary Table
| Condition | HMB | Lateral Fornix Tenderness | Key Distinguishing Features |
|---|---|---|---|
| Endometriosis | ✅ | ✅ | Dysmenorrhea, nodularity, infertility |
| Adenomyosis | ✅ | ✅ (uterine) | Bulky, globular, tender uterus |
| PID | ✅ | ✅ | Discharge, fever, CMT, STI history |
| Ectopic pregnancy | ✅ (irregular) | ✅ | +βhCG, amenorrhea, peritonism |
| Hemorrhagic ovarian cyst | ✅ | ✅ | Sudden onset, unilateral |
| Uterine fibroids | ✅ | ± | Palpable mass, bulk symptoms |
| Ovarian torsion | ± | ✅ (severe) | Acute, nausea/vomiting |
| Coagulopathy (VWD etc.) | ✅ | ❌ | No pelvic pathology, lifelong bleeding Hx |
| Endometrial polyp/hyperplasia | ✅ | ❌ | Thickened endometrium on TVUS |
| Pelvic abscess | ± | ✅ | Fever, systemic sepsis, post-procedure |
Immediate Priorities in Workup
- βhCG — exclude ectopic pregnancy first
- TVUS — assess endometrial thickness, adnexal masses, uterine morphology
- Swabs (cervical/vaginal) — exclude PID/STI
- FBC, ferritin — assess for iron-deficiency anaemia from HMB
- Coagulation screen + VWF antigen/activity — if HMB since menarche or no structural cause found
- CA-125 — if endometriosis or ovarian pathology suspected
- MRI pelvis — gold standard for adenomyosis, deep infiltrating endometriosis
Difference between cyclical and regular menstruate bleeding
search_medical_text
cyclical vs non-cyclical menstrual bleeding patterns definition abnormal uterine bleeding
GradeResponse
search_medical_text
regular menstruation definition normal cycle length duration frequency
GradeResponse
Here is a clear comparison between cyclical and regular menstrual bleeding — terms that are related but not identical.
Key Distinction
| Feature | Regular Bleeding | Cyclical Bleeding |
|---|---|---|
| Definition | Bleeding that occurs at predictable, consistent intervals | Bleeding that occurs in a pattern tied to the menstrual cycle (whether regular or not) |
| Ovulation required? | Yes — implies ovulatory cycles | Not necessarily — can occur in anovulatory cycles |
| Interval | 25–35 days (±2 days cycle-to-cycle) | Repeats at some interval, even if outside normal range |
| Driven by | Normal HPO axis cycling | Any recurring hormonal fluctuation |
In clinical practice, "regular" implies both cyclical and within normal parameters. "Cyclical" simply means the bleeding repeats in a pattern — it may still be irregular in timing.
Normal (Regular) Menstruation — Parameters
(Harrison's Principles of Internal Medicine, 21st Ed., p. 11037)
| Parameter | Normal Range |
|---|---|
| Cycle length | 25–35 days |
| Cycle-to-cycle variability | ±2 days |
| Duration of bleeding | 4–6 days |
| Luteal phase | 12–14 days (constant) |
| Main variability | Follicular phase length |
| Blood loss | 20–80 mL per cycle |
- Regular cycles become established 2–4 years after menarche.
- Cycle length shortens gradually after age 35.
- Anovulatory cycles increase as menopause approaches, making cycles erratic.
Types of Uterine Bleeding by Pattern
(Bailey & Love's Short Practice of Surgery, 28th Ed., p. 1605)
| Term | Description | Cyclical? | Regular? |
|---|---|---|---|
| Normal menstruation | Predictable, ovulatory, normal volume | ✅ | ✅ |
| Heavy menstrual bleeding (HMB/menorrhagia) | Cyclical but excessive (> 80 mL) | ✅ | ✅ (timing-wise) |
| Oligomenorrhoea | Cycles > 35 days apart | ✅ (loosely) | ❌ |
| Polymenorrhoea | Cycles < 25 days apart | ✅ | ❌ |
| Intermenstrual bleeding (IMB) | Bleeding between periods | ❌ | ❌ |
| Postcoital bleeding (PCB) | After intercourse | ❌ | ❌ |
| Anovulatory bleeding | Irregular, unpredictable, no ovulation | ❌/± | ❌ |
| Postmenopausal bleeding (PMB) | After 12 months of amenorrhoea | ❌ | ❌ |
| Breakthrough bleeding | On hormonal contraception | ± | ❌ |
Cyclical vs. Regular — Clinical Significance
Cyclical but Irregular
- Occurs in PCOS, perimenopause, thyroid dysfunction, hyperprolactinaemia
- Bleeding repeats, but intervals are unpredictable (e.g., every 45–90 days)
- Often anovulatory — no progesterone produced → unopposed estrogen
Regular but Abnormal Volume/Duration
- Normal cycle timing but too heavy (fibroids, adenomyosis, coagulopathy) or too light (Asherman's syndrome, OCP)
- Ovulation is occurring normally — the problem is structural or local
Neither Cyclical nor Regular
- IMB, PCB, PMB — always require investigation to exclude malignancy, infection, or polyps
Summary
- Regular = predictable timing (25–35 days) — implies ovulation and a functioning HPO axis.
- Cyclical = repeating pattern — does not require normal interval or ovulation.
- All regular bleeding is cyclical, but not all cyclical bleeding is regular.
- Any deviation from regular, cyclical, normal-volume bleeding should be categorised using the FIGO PALM-COEIN classification of abnormal uterine bleeding (AUB) for systematic evaluation.
This is a shared conversation. Sign in to Orris to start your own chat.