The nature of pain in acute diseases of the gastrointestinal tract.
nature of pain in acute gastrointestinal diseases mechanisms types
visceral parietal referred pain abdomen acute abdomen characteristics
Nature of Pain in Acute Diseases of the Gastrointestinal Tract
1. Fundamental Mechanisms of Abdominal Pain
| Stimulus | Example |
|---|---|
| Ischaemia | Mesenteric ischaemia, strangulated bowel |
| Muscle spasm / smooth muscle distension | Biliary colic, intestinal obstruction |
| Stretching or irritation of peritoneum | Perforation, inflammation |
2. Types of Abdominal Pain
A. Visceral (Autonomic) Pain
- Transmitted via sympathetic afferent fibres (T1–L2 nerve roots)
- Deep, dull, poorly localised, often felt in the midline regardless of the side of the lesion
- Frequently accompanied by autonomic features: nausea, vomiting, sweating, restlessness
- Arises from hollow organ distension, smooth muscle spasm, or ischaemia
- Classic example: early appendicitis — crampy periumbilical pain before peritoneal involvement
B. Parietal (Somatic) Pain
- Arises when an inflamed organ comes into contact with the parietal peritoneum
- Transmitted via spinal somatic nerves — sharp, well-localised, and constant
- Localises to the segmental dermatome of the affected abdominal wall region
- Aggravated by movement, coughing, or deep breathing (peritonism)
- Classic example: acute appendicitis — pain migrates from periumbilical to right iliac fossa (McBurney's point) once the parietal peritoneum is involved
C. Referred Pain
- Felt at a site remote from the diseased organ, sharing the same nerve root supply
- Mechanism: convergence of visceral and somatic afferents on the same spinal cord segment
- Key examples:
| Condition | Referred Pain Site |
|---|---|
| Acute cholecystitis / biliary colic | Right shoulder tip, right subscapular region |
| Ruptured spleen / diaphragmatic irritation | Left shoulder (Kehr's sign) |
| Pancreatitis | Back (mid-scapular / lumbar band) |
| Renal / ureteric colic | Groin, scrotum, or inner thigh |
| Peptic ulcer perforation | Shoulder tip (diaphragmatic spread) |
3. Sensitisation and Progression of Pain
- Peripheral sensitisation: Inflammatory mediators (prostaglandins, bradykinin, substance P) lower the threshold of nociceptor transducers, intensifying afferent signalling.
- Recruitment of silent afferents: Afferents normally inactive at baseline become activated, broadening the pain field.
- These acute mechanisms can also trigger central sensitisation, explaining referred hyperalgesia and allodynia around the affected area (e.g., cutaneous tenderness overlying an inflamed appendix or gallbladder).
4. Character of Pain by Condition
| Condition | Onset | Character | Location | Radiation |
|---|---|---|---|---|
| Biliary colic | Sudden | Severe, constant, colicky | Epigastrium / RUQ | Right shoulder, back |
| Acute cholecystitis | Gradual | Constant, aching | RUQ | Right shoulder blade — Murphy's sign positive |
| Acute pancreatitis | Sudden | Severe, boring, constant | Epigastrium | Band-like to the back; relieved by leaning forward |
| Appendicitis | Gradual | Initially dull → sharp | Periumbilical → RIF | None typical |
| Perforated peptic ulcer | Sudden ("like a blow") | Knife-like, agonising | Epigastrium | Shoulder tip (peritoneal spread) |
| Intestinal obstruction | Colicky, intermittent | Crescendo–decrescendo waves | Central abdomen | None |
| Mesenteric ischaemia | Sudden | Severe, out of proportion to signs | Periumbilical | None |
| Acute diverticulitis | Gradual | Constant, dull | LIF | None |
| Renal/ureteric colic | Sudden | Severe, colicky | Loin | Groin, genitalia |
5. Clinical Significance of Pain Features
- Onset: Sudden ("thunderclap") onset suggests perforation or vascular catastrophe; gradual onset suggests inflammation.
- Character: Colicky (waxing/waning) pain implies hollow viscus obstruction (bowel, ureter, bile duct); constant pain implies inflammation or ischaemia.
- Murphy's sign: On deep inspiration, the descending inflamed gallbladder contacts the examining hand, worsening pain and causing the patient to arrest breathing — reflects parietal peritoneal involvement in acute cholecystitis (Bailey and Love's, p. 1074).
- Psoas sign: In retrocaecal appendicitis, the inflamed appendix irritates the psoas muscle; children adopt hip flexion to relieve psoas stretch.
- Rebound tenderness (Blumberg's sign): Release of hand pressure suddenly worsens pain — indicates parietal peritoneal irritation.
- Pain–signs disparity: Severe pain with minimal tenderness is the hallmark of mesenteric ischaemia and demands urgent investigation.
6. Neuroanatomical Basis of Pain Localisation
- Foregut derivatives (stomach to mid-duodenum, liver, biliary tree, spleen, pancreas): pain referred to the epigastrium
- Midgut derivatives (mid-duodenum to mid-transverse colon, including appendix): pain referred to the periumbilical region
- Hindgut derivatives (mid-transverse colon to rectum): pain referred to the hypogastrium/suprapubic region
specific sym of pulmonary embolism
pulmonary embolism symptoms clinical presentation signs
pulmonary embolism symptoms signs clinical features
pulmonary embolism dyspnea pleuritic chest pain hemoptysis tachycardia syncope massive submassive
pulmonary embolism symptoms frequency dyspnea chest pain signs examination findings
Specific Symptoms of Pulmonary Embolism
Classification by Severity
| Category | Prevalence | Key Features |
|---|---|---|
| Massive (high-risk) | 5–10% | Systemic hypotension, ≥50% pulmonary vasculature occluded |
| Submassive (intermediate-risk) | 20–25% | RV dysfunction, normal BP, elevated cardiac biomarkers |
| Low-risk | 65–75% | Normal RV, normal BP, excellent prognosis |
Specific Symptoms
Respiratory Symptoms
- Dyspnea — the most common symptom; may be sudden in onset; present even at rest
- Pleuritic chest pain — sharp, stabbing, worsened by inspiration; occurs with peripheral emboli causing pulmonary infarction and pleural irritation
- Haemoptysis — blood-streaked sputum; signals pulmonary infarction (peripheral emboli)
- Cough — non-productive; less specific
Cardiovascular Symptoms
- Tachycardia (HR >100 bpm) — one of the most consistent signs; included in the Wells score (Bailey and Love's, 28th Ed., p. 345)
- Syncope / presyncope — hallmark of massive PE; reflects acute reduction in cardiac output and cerebral hypoperfusion
- Hypotension / cardiogenic shock — defines massive (high-risk) PE
- Cyanosis — in severe cases with massive occlusion
Other Symptoms
- Anxiety and sense of impending doom — common in large emboli due to sudden haemodynamic compromise
- Leg pain and swelling — from concurrent deep vein thrombosis (DVT), which is the source in ~70% of cases
Signs on Examination
| Sign | Mechanism |
|---|---|
| Tachycardia | Compensatory response to reduced cardiac output |
| Tachypnoea | Hypoxaemia, stimulation of pulmonary stretch receptors |
| Low O₂ saturation (SpO₂ <94%) | V/Q mismatch and intrapulmonary shunting |
| Pleural rub | Infarction-related pleural inflammation |
| Raised JVP / right heart strain signs | Acute cor pulmonale from RV pressure overload |
| Loud P2 (pulmonary component of S2) | Pulmonary hypertension |
| S3 / S4 gallop (right-sided) | RV failure |
| Leg oedema, warmth, erythema | Co-existing DVT |
| Hypotension | Massive PE; RV failure reducing LV preload |
Wells Score Clinical Features
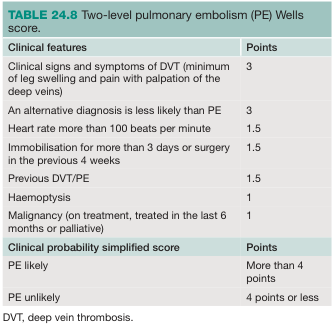
Key Points
- No single symptom is pathognomonic — PE is notoriously non-specific in presentation
- The classic triad of dyspnea + chest pain + haemoptysis occurs in fewer than 20% of patients
- Massive PE presents with dyspnea, syncope, hypotension, and cyanosis
- Peripheral (small) PE tends to present with pleuritic chest pain and haemoptysis (infarction pattern)
- Central (large) PE tends to present with dyspnea, syncope, and haemodynamic collapse
- A high index of suspicion, combined with risk factor assessment and the Wells score, is the cornerstone of diagnosis
myocardial infarction in detailed
myocardial infarction pathophysiology etiology types STEMI NSTEMI
myocardial infarction clinical presentation symptoms signs diagnosis ECG
myocardial infarction management treatment thrombolysis PCI reperfusion therapy
myocardial infarction ECG changes STEMI ST elevation
Myocardial Infarction — Detailed Review
Definition
Classification
By ECG Pattern
| Type | ECG Finding | Mechanism |
|---|---|---|
| STEMI | ST-segment elevation in ≥2 contiguous leads | Complete occlusion of a coronary artery (transmural ischaemia) |
| NSTEMI | No ST elevation; troponin elevated | Partial occlusion or severe stenosis (subendocardial ischaemia) |
| Unstable Angina | No ST elevation; troponin normal | Partial occlusion; no myocyte necrosis |
By Depth (Histological)
- Transmural MI — full thickness of myocardial wall; usually STEMI
- Subendocardial MI — inner layer only; usually NSTEMI
Universal Classification (Type 1–5)
| Type | Cause |
|---|---|
| Type 1 | Spontaneous — atherosclerotic plaque rupture/erosion with thrombosis |
| Type 2 | Supply-demand mismatch (e.g., anaemia, tachyarrhythmia, hypotension) |
| Type 3 | Sudden cardiac death before biomarkers obtained |
| Type 4a/4b | Peri-PCI MI / stent thrombosis |
| Type 5 | Peri-CABG MI |
Aetiology & Risk Factors
Primary Cause
Risk Factors
| Modifiable | Non-modifiable |
|---|---|
| Hypertension | Age (♂ >45, ♀ >55) |
| Dyslipidaemia (↑LDL, ↓HDL) | Male sex |
| Diabetes mellitus | Family history of premature CAD |
| Smoking | Genetic predisposition |
| Obesity / metabolic syndrome | Prior MI or CAD |
| Physical inactivity | |
| Cocaine / stimulant use |
Pathophysiology
- Atherosclerotic plaque develops in coronary arteries over years (lipid-rich core with fibrous cap)
- Plaque rupture or erosion → exposure of subendothelial collagen and lipid core
- Platelet adhesion and aggregation → thrombus formation
- Coronary artery occlusion → cessation of oxygen delivery distal to the lesion
- Ischaemia → within seconds: impaired contractility; within minutes: electrical instability
- Irreversible necrosis begins after ~20–40 minutes of sustained ischaemia (subendocardium first, propagating outward — the "wavefront phenomenon")
- Reperfusion injury can occur if flow is restored late
Zones of Injury (from centre outward):
- Zone of necrosis — dead tissue, no function
- Zone of injury — viable but injured myocytes (ST elevation on ECG)
- Zone of ischaemia — reversible ischaemia (T-wave changes on ECG)
Clinical Presentation
Symptoms
- Chest pain — the cardinal symptom
- Crushing, squeezing, pressure-like ("elephant sitting on chest")
- Central/retrosternal, may radiate to left arm, jaw, neck, back, epigastrium
- Lasting >20 minutes (differentiates from stable angina)
- Not relieved by nitrates
- Dyspnoea — from acute LV failure / pulmonary oedema
- Diaphoresis (profuse sweating) — autonomic activation
- Nausea and vomiting — especially in inferior MI (vagal stimulation)
- Palpitations — arrhythmias
- Syncope — from haemodynamic compromise or arrhythmia
- Sense of impending doom
Atypical Presentations (common in elderly, women, diabetics)
- Epigastric pain / "indigestion"
- Isolated jaw or arm pain
- Fatigue and weakness only
- Silent MI (no pain) — particularly in diabetics
Signs on Examination
| Sign | Significance |
|---|---|
| Tachycardia | Sympathetic activation; heart failure |
| Bradycardia + hypotension | Inferior MI with vagal activation (Bezold-Jarisch reflex) |
| S3 gallop | LV failure / reduced compliance |
| S4 gallop | Reduced LV compliance (common in MI) |
| Pansystolic murmur | Mitral regurgitation (papillary muscle dysfunction) or VSD (mechanical complication) |
| Pulmonary crackles | Pulmonary oedema / LV failure |
| Raised JVP, hypotension | RV infarction (especially inferior MI) |
| Pericardial rub | Post-MI pericarditis (Dressler's syndrome, days–weeks later) |
Diagnosis
1. ECG
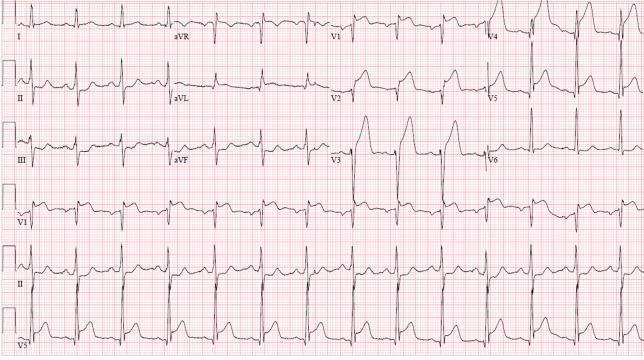
| Phase | ECG Finding |
|---|---|
| Hyperacute (minutes) | Tall, peaked (hyperacute) T-waves |
| Acute (hours) | ST-segment elevation (STEMI); ST depression (NSTEMI) |
| Hours–days | T-wave inversion |
| Days–weeks | Pathological Q-waves (>40 ms wide, >25% R-wave height) |
| Old/chronic | Persistent Q-waves; T-wave changes |
| Territory | Leads | Artery |
|---|---|---|
| Anterior | V1–V4 | LAD |
| Anterolateral | V1–V6, I, aVL | Proximal LAD |
| Lateral | I, aVL, V5–V6 | LCx |
| Inferior | II, III, aVF | RCA (80%) or LCx |
| Posterior | ST depression V1–V2 + tall R | RCA/LCx |
| Right ventricular | V4R–V6R elevation | Proximal RCA |
2. Cardiac Biomarkers
| Biomarker | Rises | Peaks | Returns to Normal | Notes |
|---|---|---|---|---|
| High-sensitivity Troponin I/T | 1–3 h | 12–24 h | 7–14 days | Gold standard; serial measurements at 0 and 1–3 h |
| CK-MB | 3–6 h | 12–24 h | 48–72 h | Useful for reinfarction detection |
| Myoglobin | 1–2 h | 4–8 h | 24 h | Sensitive but non-specific |
| LDH | 24–48 h | 3–6 days | 8–14 days | Rarely used now |
3. Imaging
- Echocardiography: Regional wall motion abnormalities (RWMA); LV function; mechanical complications
- Coronary angiography: Definitive identification of culprit lesion; performed urgently in STEMI
- Chest X-ray: Pulmonary oedema, cardiomegaly; not diagnostic for MI
Management
Immediate (First 10 Minutes)
- MONA mnemonic:
- Morphine (cautiously; may mask symptoms, use judiciously)
- Oxygen (only if SpO₂ <90%)
- Nitrates (sublingual GTN; avoid in RV infarction / hypotension / PDE5 inhibitor use)
- Aspirin 300 mg loading dose (chewed)
Reperfusion Strategy (Management of ACS, p. 10)
| Strategy | Indication | Time Target |
|---|---|---|
| Primary PCI (PPCI) | STEMI — preferred | Door-to-balloon ≤90 min (≤60 min if direct presentation) |
| Fibrinolysis | STEMI if PPCI not feasible within 120 min | Administer within 10 min of decision |
| Urgent angiography ± PCI | NSTE-ACS with very high-risk features | Immediate |
| Early angiography | NSTE-ACS with high-risk features | Within 24 hours |
Antiplatelet & Anticoagulation (Acute Phase)
- Dual antiplatelet therapy (DAPT): Aspirin + P2Y₁₂ inhibitor (ticagrelor, prasugrel, or clopidogrel)
- Anticoagulation: Unfractionated heparin (UFH) or low molecular weight heparin (LMWH) or fondaparinux
Secondary Prevention (Long-term)
| Drug Class | Agent | Benefit |
|---|---|---|
| Antiplatelet | Aspirin + P2Y₁₂ (12 months DAPT) | Prevent stent thrombosis / recurrent MI |
| Beta-blocker | Metoprolol, carvedilol | Reduce mortality; prevent arrhythmia |
| ACE inhibitor / ARB | Ramipril, valsartan | Reduce LV remodelling; especially if EF <40% |
| Statin (high-intensity) | Atorvastatin 80 mg | Plaque stabilisation; LDL reduction |
| Aldosterone antagonist | Eplerenone | If EF <35% + heart failure or diabetes |
| Lifestyle | Smoking cessation, diet, exercise, cardiac rehab | Reduce recurrence |
Complications
Early (Hours–Days)
| Complication | Notes |
|---|---|
| Arrhythmias | VF/VT most common cause of early death; AF also common |
| Cardiogenic shock | Massive LV failure; mortality >50%; requires IABP/Impella + urgent revascularisation |
| Acute LV failure / pulmonary oedema | Diuretics, vasodilators, ventilatory support |
| Right ventricular infarction | Complicates inferior MI; treat with fluids, avoid nitrates/diuretics |
| Mechanical complications | Free wall rupture (tamponade), VSD, papillary muscle rupture (acute MR) |
Late (Days–Weeks)
| Complication | Notes |
|---|---|
| Post-MI pericarditis (Dressler's syndrome) | Autoimmune; fever, pleuritic chest pain, pericardial rub; treat with NSAIDs/colchicine |
| LV aneurysm | Persistent ST elevation; mural thrombus; risk of embolism |
| Heart failure / cardiomyopathy | LV remodelling; start ACEi + beta-blocker |
| Ventricular thrombus | Anticoagulate for 3–6 months |
| Arrhythmias (chronic) | Consider ICD if EF <35% after 40 days |
Prognosis
- In-hospital mortality for STEMI with PPCI: ~5%
- 30-day mortality (untreated STEMI): ~30%
- Key determinants: time to reperfusion, infarct size, LV ejection fraction, age, comorbidities
- TIMI and GRACE scores are used for risk stratification in ACS
Summary Algorithm
Chest pain / suspected ACS
↓
ECG within 10 min
↓
┌─────────────────────┐
│ ST elevation or LBBB│ → STEMI → Primary PCI (≤90 min) or Fibrinolysis
└─────────────────────┘
↓ (no ST elevation)
Serial troponins (0h, 1–3h)
↓
┌───────────┐ ┌──────────┐
│ Troponin ↑│ │Troponin N│
└───────────┘ └──────────┘
NSTEMI Unstable angina
↓ ↓
Risk stratify (GRACE score)
↓
Angiography ± PCI (timing by risk)
atypical type
atypical myocardial infarction presentation silent MI women elderly diabetic
Atypical Presentations of Myocardial Infarction
Who Presents Atypically?
| Population | Reason |
|---|---|
| Elderly | Reduced pain perception; multiple comorbidities masking symptoms |
| Women | Different pain pathways; smaller vessel disease more common |
| Diabetics | Autonomic neuropathy impairs pain signalling — "silent MI" |
| Post-cardiac transplant | Denervated heart — no anginal pain |
| Patients on analgesics / opioids | Pain perception blunted |
Atypical Symptom Patterns
1. Epigastric / GI Presentation
- Pain in upper abdomen mimicking peptic ulcer, gastritis, or indigestion
- Nausea, vomiting, belching
- Most common in inferior MI (diaphragmatic surface irritation + vagal stimulation)
- Frequently misdiagnosed and sent home with antacids
2. Jaw / Dental Pain
- Isolated jaw ache or toothache without chest pain
- Referred pain via shared cervical and trigeminal pathways
- Patients often see a dentist before a cardiologist
3. Arm / Shoulder Pain Only
- Left arm heaviness, aching, or numbness without chest involvement
- Can occur in isolation, especially in women
4. Back Pain
- Interscapular or mid-back pain
- May mimic musculoskeletal pain or aortic dissection
- Common in posterior MI
5. Neck / Throat Tightness
- Sensation of throat constriction or choking
- Mistaken for anxiety, GERD, or oesophageal spasm
6. Dyspnoea Alone (Anginal Equivalent)
- Sudden breathlessness without chest pain
- Reflects acute LV dysfunction / flash pulmonary oedema
- Common in elderly women and diabetics
7. Fatigue / Weakness
- Profound, unexplained fatigue — especially in women
- May precede MI by days to weeks (prodromal symptom)
- Often dismissed as viral illness or stress
8. Syncope / Collapse
- Loss of consciousness due to arrhythmia or haemodynamic compromise
- No preceding chest pain
- Common in massive MI or MI complicated by VT/VF
9. Silent MI (Completely Asymptomatic)
- Patient has no symptoms at all; MI discovered incidentally on ECG (Q-waves) or imaging
- Accounts for up to 20–30% of all MIs
- Strongly associated with diabetes mellitus (autonomic neuropathy)
10. Acute Confusion / Delirium
- Seen in the very elderly
- MI reduces cardiac output → cerebral hypoperfusion → confusion
- No chest pain reported
Comparison: Classic vs. Atypical MI
| Feature | Classic | Atypical |
|---|---|---|
| Pain location | Central/retrosternal | Jaw, arm, back, epigastrium, or absent |
| Character | Crushing, pressure | Aching, burning, indigestion-like |
| Duration | >20 min | Variable |
| Associated symptoms | Diaphoresis, dyspnoea | Nausea, fatigue, syncope, dyspnoea alone |
| Who | Middle-aged men | Women, elderly, diabetics |
| Risk of missed diagnosis | Low | High |
Clinical Importance
- Atypical MI carries higher mortality than classic MI — primarily due to delayed diagnosis and treatment
- A high index of suspicion must be maintained in at-risk groups
- ECG + high-sensitivity troponin should be obtained in any patient with unexplained dyspnoea, syncope, epigastric pain, or fatigue — especially if risk factors are present
- The phrase "rule out MI" exists precisely because atypical presentations are common and dangerous
In women presenting with acute MI, the most common symptom is not chest pain — it is fatigue, followed by dyspnoea and jaw/arm discomfort. Chest pain occurs in only ~57% of women vs. ~70% of men.