Meningococoal disease
Reading File
search_medical_text
meningococcal disease Neisseria meningitidis epidemiology pathophysiology clinical features diagnosis management
search_medical_text
meningococcal meningitis septicemia treatment antibiotics complications prevention vaccination
search_medical_image
meningococcal purpuric rash petechiae meningococcemia
GradeResponse
GradeResponse
GradeResponse
Here is a comprehensive overview of meningococcal disease:
Meningococcal Disease
Etiology
Meningococcal disease is caused by Neisseria meningitidis, a gram-negative diplococcus. It is transmitted via respiratory droplets and close contact. The organism is classified into serogroups based on its polysaccharide capsule; the clinically important ones are:
| Serogroup | Key Features |
|---|---|
| A | Major cause of epidemic disease in sub-Saharan Africa ("meningitis belt") |
| B | Predominant in Europe, Americas, Australasia; hardest to vaccinate against |
| C | Common in Europe and the Americas |
| W | Increasing global prevalence; higher case fatality |
| Y | Common in North America, associated with pneumonia |
| X | Emerging in Africa |
Epidemiology
- Humans are the only reservoir; 5–25% of the population carry the organism asymptomatically in the nasopharynx.
- Peak incidence: infants < 1 year, toddlers, and adolescents/young adults (dormitory settings — universities, military).
- Outbreaks occur in the "meningitis belt" (sub-Saharan Africa), particularly serogroup A.
- Case fatality rate: 10–15% overall; up to 40–50% in fulminant meningococcemia (purpura fulminans).
Pathophysiology
- Nasopharyngeal colonization → invasion of mucosal barrier
- Bacteremia → release of lipopolysaccharide (LPS/endotoxin)
- Massive cytokine cascade → systemic inflammatory response
- Endothelial damage → disseminated intravascular coagulation (DIC), microvascular thrombosis
- Meningeal seeding → meningitis; adrenal infarction → Waterhouse-Friderichsen syndrome
Clinical Presentations
Meningococcal disease presents in several overlapping forms:
1. Meningococcal Meningitis
- Headache, photophobia, neck stiffness (meningism)
- Fever, nausea/vomiting
- Altered consciousness
- Kernig's and Brudzinski's signs
2. Meningococcemia (Septicemia)
- High fever, rigors
- Petechial/purpuric rash — the hallmark; begins as pinpoint petechiae, rapidly progressing to non-blanching purpura
- Hypotension, shock
- Multi-organ failure
3. Purpura Fulminans (Fulminant Meningococcemia)
- Most severe form: rapidly spreading ecchymoses, DIC, adrenal hemorrhage
- High mortality even with treatment
4. Other (less common)
- Pneumonia, septic arthritis, pericarditis, conjunctivitis
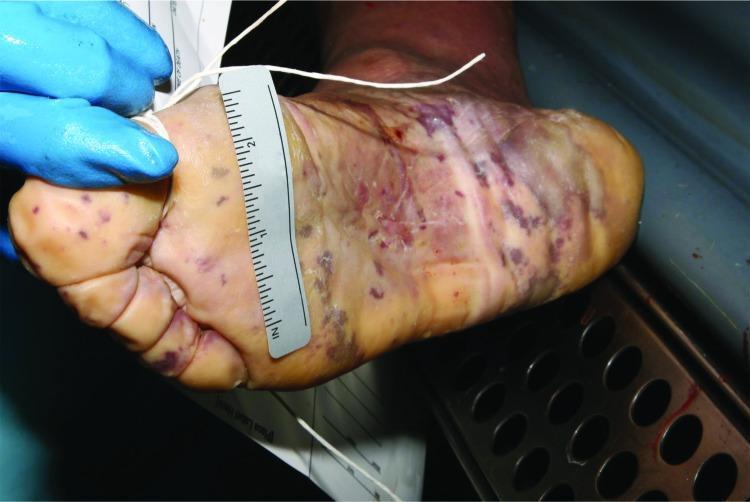
The Classic Rash
The non-blanching petechial/purpuric rash is a medical emergency — presence on glass test (does not blanch under pressure) mandates immediate action.
Diagnosis
Investigations (to be done urgently, without delaying treatment)
| Test | Purpose |
|---|---|
| Blood cultures (x2) | Isolate organism, sensitivities |
| PCR (blood/CSF) | Rapid detection; positive even after antibiotics |
| Lumbar puncture (if no contraindication) | CSF analysis, culture, PCR |
| FBC, CRP, clotting, U&E, LFTs, lactate | Assess severity, DIC |
| Meningococcal throat swab | Strain typing for public health/contact management |
| CT head | Before LP if focal neurology, papilloedema, or GCS < 13 |
CSF findings in bacterial meningitis:
- Turbid/purulent appearance
- Raised WBC (predominantly neutrophils, > 1000 cells/µL)
- Raised protein (> 1 g/L)
- Low glucose (CSF:serum glucose < 0.4)
Per the NICE Guideline on Bacterial Meningitis and Meningococcal Disease, a bacterial throat swab should be taken in all suspected meningococcal cases to guide management of cases, contacts, and outbreaks. (NICE, p. 69)
Management
Immediate Pre-Hospital / Emergency
- If meningococcal disease is suspected and the patient cannot be transferred immediately, administer IM/IV Benzylpenicillin (or Ceftriaxone if penicillin allergy) before transfer.
- Secure IV access, resuscitation fluids for shock.
- Isolate (droplet precautions) until 24h of antibiotics.
Definitive Antibiotic Treatment
| Scenario | Preferred Agent | Duration |
|---|---|---|
| Meningococcal meningitis | IV Ceftriaxone 2g BD | 7 days (3–5 days may suffice) |
| Meningococcal septicemia | IV Ceftriaxone 2g BD | 7 days |
| Penicillin allergy | IV Chloramphenicol or Meropenem | 7 days |
| Resource-limited settings | Single dose IM Ceftriaxone or oily Chloramphenicol | — |
Harrison's (p. 4618): "Both meningococcal meningitis and meningococcal septicemia are conventionally treated for 7 days, although courses of 3–5 days may be equally effective... Cultures usually become sterile within 24 h of initiation of appropriate antibiotic chemotherapy."
Adjunctive Treatment
- Dexamethasone IV (0.15 mg/kg QDS for 4 days) — reduces neurological sequelae; best given before or with first dose of antibiotics.
- ICU care for shock: vasopressors (norepinephrine), mechanical ventilation, renal replacement therapy.
- DIC management: FFP, platelet transfusion as needed.
- Treat Waterhouse-Friderichsen syndrome (adrenal insufficiency) with hydrocortisone.
Complications
| Short-term | Long-term |
|---|---|
| Septic shock, multi-organ failure | Sensorineural hearing loss (most common) |
| DIC, purpura fulminans | Neurological deficits (cognitive, motor) |
| Waterhouse-Friderichsen syndrome | Limb amputation (from ischemic necrosis) |
| Raised intracranial pressure, herniation | Skin scarring |
| Hydrocephalus | Psychological/PTSD |
Prevention
Vaccination
| Vaccine | Target | Examples |
|---|---|---|
| MenACWY | Serogroups A, C, W, Y | Menveo, Nimenrix — routine adolescent immunization in many countries |
| MenB | Serogroup B | Bexsero, Trumenba — recommended for infants and high-risk groups |
| MenA (polysaccharide conjugate) | Serogroup A | MenAfriVac — mass campaigns in African meningitis belt |
Chemoprophylaxis for Close Contacts
Close contacts (household members, kissing contacts) should receive prophylaxis within 24 hours of case identification:
- Ciprofloxacin 500mg single dose PO (adults) — preferred in most guidelines
- Rifampicin 600mg BD for 2 days (alternative)
- Ceftriaxone 250mg IM single dose (pregnant women)
Risk Factors for Severe/Invasive Disease
- Complement deficiencies (C5–C9, properdin) — recurrent disease
- Asplenia or functional hyposplenism
- HIV infection
- Age extremes (infants, elderly)
- Crowded living conditions
Key Points Summary
- Any non-blanching rash + fever = meningococcal disease until proven otherwise — treat immediately.
- Do not delay antibiotics to perform investigations; LP can follow once stable.
- Ceftriaxone is the antibiotic of choice; dexamethasone reduces sequelae.
- Hearing loss is the most common long-term complication — arrange formal audiological assessment post-recovery.
- Notify public health authorities; trace and provide prophylaxis to close contacts within 24 hours.
This is a shared conversation. Sign in to Orris to start your own chat.