Meningococcal disease
Reading File
search_medical_text
meningococcal disease etiology pathophysiology Neisseria meningitidis serogroups
search_medical_text
meningococcal disease clinical presentation diagnosis management treatment
search_medical_image
meningococcal disease purpuric rash meningococcemia
GradeResponse
GradeResponse
GradeResponse
Meningococcal Disease
Etiology & Microbiology
Neisseria meningitidis is a Gram-negative diplococcus that is the causative agent. It is classified into 13 serogroups based on capsular polysaccharide; the clinically significant ones are A, B, C, W, X, and Y.
- Serogroup A: historically dominant in sub-Saharan Africa's "meningitis belt," with epidemic waves every 8-12 years
- Serogroups C (~60%) and B (~29%): responsible for most outbreaks in the US and Europe over the past 50 years
- Serogroups W135, X, C: emerging pathogens in Africa (e.g., a large serogroup C outbreak in Nigeria, 2016-2017)
Humans are the only natural reservoir. The organism colonizes the nasopharynx asymptomatically in ~10% of healthy adults (carrier state). Transmission is via respiratory droplets or direct contact.
Pathophysiology
Following nasopharyngeal colonization, the organism can invade the bloodstream (bacteremia/meningococcemia) and/or spread to the meninges. Key pathogenic mechanisms include:
- Endotoxin (lipooligosaccharide) release → massive systemic inflammatory response (cytokine storm with IL-1, IL-6, TNF-α)
- Disseminated intravascular coagulation (DIC) → microvascular thrombosis and hemorrhage → purpuric/petechial rash and purpura fulminans
- Hypovolemic shock (from vasodilation and capillary leak) — the most common cause of death
- Raised intracranial pressure — in meningitis predominant forms
Clinical Presentations
Meningococcal disease manifests in several overlapping syndromes:
| Syndrome | Key Features |
|---|---|
| Meningococcemia (bacteremia) | Fever, rash (petechiae → purpura), hypotension, DIC, shock |
| Meningococcal meningitis | Fever, headache, neck stiffness, photophobia, altered consciousness |
| Mixed (most common) | Features of both meningitis and septicemia |
| Purpura fulminans | Fulminant DIC, large ecchymoses, limb ischemia — highest mortality |
| Waterhouse-Friderichsen syndrome | Bilateral adrenal hemorrhage, adrenal insufficiency |
Rash is present in ~75% of bacteremic patients and is the cardinal sign — initially blanching maculopapular, rapidly progressing to non-blanching petechiae and purpura. This is a medical emergency.
Classic purpuric rash of meningococcemia:
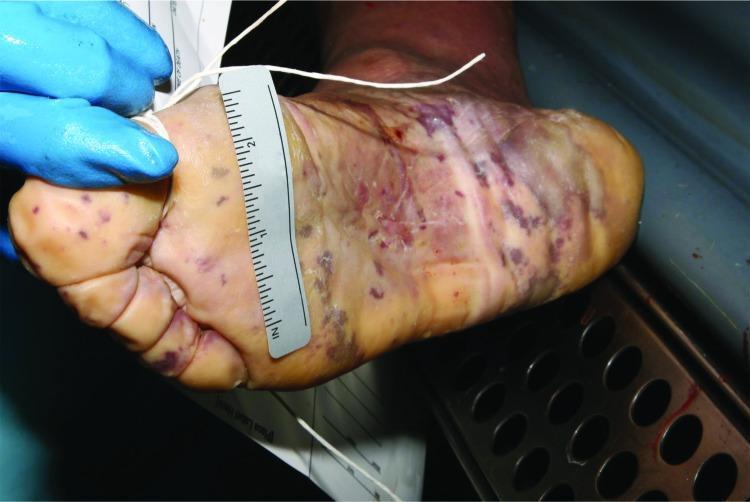
Plantar surface demonstrating widespread purpuric lesions — pinpoint petechiae and confluent ecchymoses typical of fulminant meningococcemia (purpura fulminans). Harrison's, p. 3690.
Diagnosis
Immediate clinical recognition is paramount — do not delay treatment for diagnostic workup.
- Blood cultures (before antibiotics if feasible, but never delay antibiotics)
- Lumbar puncture (LP): CSF shows cloudy fluid, elevated WBC (neutrophilic pleocytosis), elevated protein, low glucose; Gram stain and culture; PCR for N. meningitidis
- CBC: leukocytosis (or leukopenia in severe sepsis), thrombocytopenia
- Coagulation studies: PT/aPTT prolongation, elevated D-dimer, low fibrinogen (DIC)
- Serum lactate, electrolytes, LFTs, renal function
- Skin biopsy of petechiae: Gram stain and PCR can be diagnostic even after antibiotics
- Meningococcal PCR (blood/CSF): highly sensitive, unaffected by prior antibiotic therapy
If raised ICP is suspected (papilledema, focal neuro signs, GCS <12), perform CT head before LP. Do not delay antibiotics for CT.
Management
(Harrison's, p. 4617)
1. Stabilization (ABCs)
- Airway: secure if GCS is depressed due to shock or raised ICP
- Oxygen for hypoxia (pulmonary edema/oligemia in meningococcemia)
- IV access: aggressive fluid resuscitation for hypovolemic shock
- Vasopressors (norepinephrine) for refractory shock
2. Antibiotics — Start Immediately
- First-line: Benzylpenicillin (Penicillin G) IV/IM — if organism confirmed susceptible
- Empirical (before results): Ceftriaxone 2g IV q12h (adults) or 80–100 mg/kg/day in children — covers both meningitis and septicemia
- Alternative: Cefotaxime; Chloramphenicol in penicillin allergy
- Duration: typically 5–7 days for meningococcal meningitis/septicemia
3. Adjunctive Therapy
- Dexamethasone 0.15 mg/kg IV q6h × 4 days: given before or with the first antibiotic dose to reduce neurological sequelae in bacterial meningitis
- DIC management: fresh frozen plasma, platelets, cryoprecipitate as needed
- Adrenal insufficiency: consider hydrocortisone in hemodynamically unstable patients
- ICU admission for all severe cases
Prevention & Vaccination
Chemoprophylaxis (close contacts)
All household/close contacts (within 7 days of exposure) require prophylaxis within 24 hours:
- Rifampicin 600 mg PO q12h × 2 days (adults)
- Ciprofloxacin 500 mg PO single dose (preferred in many guidelines due to simplicity)
- Ceftriaxone 250 mg IM single dose (preferred in pregnancy)
Vaccines
| Vaccine Type | Serogroups Covered | Key Use |
|---|---|---|
| MenACWY (conjugate) | A, C, W, Y | Routine adolescent immunization; travelers to endemic areas |
| MenB (protein-based) | B | Adolescents/young adults; outbreak control |
| MenA conjugate (MenAfriVac) | A | Mass vaccination campaigns in sub-Saharan Africa |
High-risk groups requiring vaccination: asplenic patients, complement deficiencies (C5-C9, properdin), HIV, college freshmen in dormitories, military recruits, Hajj pilgrims, travelers to the meningitis belt.
Complications & Prognosis
- Mortality: 10–15% overall; up to 40–60% in fulminant meningococcemia
- Neurological sequelae (in survivors of meningitis): hearing loss (~10%), cognitive impairment, seizures
- Limb loss: ischemic necrosis from purpura fulminans may require amputation
- Waterhouse-Friderichsen syndrome: adrenal crisis
- Obstructive hydrocephalus, subdural empyema (rare)
Early antibiotic therapy and aggressive ICU management are the key determinants of outcome. Delayed recognition is the leading preventable cause of death. (Harrison's, p. 4617)
This is a shared conversation. Sign in to Orris to start your own chat.