EXPAIN COMPLICATION SEEN IN RESPIRATORY SYSTEM IN PED
Reading File
search_medical_text
respiratory complications in pediatrics children
search_medical_text
pediatric respiratory diseases pneumonia bronchiolitis asthma complications
search_medical_image
pediatric respiratory system complications diagram
GradeResponse
GradeResponse
GradeResponse
Based on retrieved sources and comprehensive clinical knowledge, here is a detailed explanation of respiratory system complications in pediatrics (PED):
Respiratory System Complications in Pediatrics
Why Children Are Uniquely Vulnerable
Children — especially those under 2 years — have distinct anatomical and physiological features that predispose them to more severe respiratory complications:
- Smaller airway diameter → minor edema causes significant obstruction
- Horizontal ribs & compliant chest wall → less efficient breathing mechanics, prone to fatigue
- Immature immune system → higher susceptibility to infections
- Higher respiratory rate → faster decompensation when compromised
- Higher oxygen consumption per kg → desaturate faster than adults
Major Respiratory Complications in Pediatrics
1. 🫁 Pneumonia
| Feature | Details |
|---|---|
| Common pathogens | S. pneumoniae, RSV, Mycoplasma, H. influenzae |
| Complications | Parapneumonic effusion, empyema, lung abscess, necrotizing pneumonia, pneumothorax, sepsis |
| Target SpO₂ | >92% (per WHO/GINA guidelines) |
| Severe signs | Grunting, nasal flaring, subcostal retractions, cyanosis |
Complications of pneumonia include:
- Parapneumonic effusion/Empyema: exudative fluid in pleural space; may require chest drain
- Necrotizing pneumonia: cavitation and lung tissue destruction; increasingly common with S. aureus (MRSA)
- Lung abscess: collection of pus within parenchyma
- Pneumothorax: especially in ventilated patients or those with Staph infection
- Septicemia & septic shock: systemic spread
2. 🌬️ Bronchiolitis
- Most common lower respiratory tract infection in infants <2 years
- Predominantly caused by RSV (Respiratory Syncytial Virus)
Complications:
- Apnea — especially in premature infants and neonates (<6 weeks)
- Respiratory failure requiring mechanical ventilation
- Secondary bacterial infection (otitis media, pneumonia)
- Recurrent wheeze / asthma development later in childhood
- Pulmonary hypertension in severe/prolonged cases
Oxygenation target for acute lower respiratory tract infection (bronchiolitis): SpO₂ ≥ 90–92% (Management of Pediatric Patients With Oxygen in the Acute Care Setting, p. 8)
3. 🤧 Asthma
- Most common chronic respiratory disease in children
Complications:
- Status asthmaticus — severe, prolonged bronchospasm unresponsive to initial therapy; life-threatening
- Air trapping & hyperinflation → pneumothorax, pneumomediastinum
- Respiratory arrest if untreated
- Steroid-related complications with long-term therapy (growth suppression, adrenal suppression)
- Exercise limitation & school absenteeism — long-term quality-of-life impact
- Fixed airflow obstruction if poorly controlled over years
Oxygen target in asthma: >90% (NHLBI 2007) or 94–98% (British Guideline 2019) (Management of Pediatric Patients With Oxygen, p. 8)
4. 😴 Obstructive Sleep Apnea (OSA)
- Common in children with adenotonsillar hypertrophy
Complications:
- Nocturnal hypoxemia (desaturations)
- Pulmonary hypertension → cor pulmonale if chronic
- Neurocognitive deficits: poor attention, behavioral issues, learning difficulties
- Growth failure (disrupted growth hormone secretion)
- Post-adenotonsillectomy respiratory complications: 21.6% of children with mild-to-moderate OSA required supplemental oxygen post-op; risk significantly higher in those with AHI >5 and severe OSA
Children with comorbidities had a 15.7% complication rate vs 6.7% in non-comorbid children after adenotonsillectomy (Day Case Paediatric Adenotonsillectomy, p. 12)
5. 💨 Croup (Laryngotracheobronchitis)
- Caused by parainfluenza virus; peaks in 6 months–3 years
Complications:
- Severe upper airway obstruction → stridor at rest, cyanosis
- Bacterial tracheitis (secondary superinfection with S. aureus) — life-threatening
- Respiratory failure in severe cases
6. 🧫 Pertussis (Whooping Cough)
- Caused by Bordetella pertussis; most dangerous in infants
Complications:
- Apnea and sudden death in infants <6 months
- Pneumonia (most common cause of death)
- Pulmonary hypertension — severe and often fatal in neonates
- Seizures (from hypoxia or direct toxin effect)
- Subconjunctival hemorrhage, rib fractures (from coughing)
- Encephalopathy
7. 🌊 Cystic Fibrosis (CF)
- Autosomal recessive; CFTR gene mutation
Respiratory Complications:
- Recurrent pulmonary infections (Pseudomonas aeruginosa, S. aureus, Burkholderia cepacia)
- Bronchiectasis — permanent airway dilation and destruction
- Hemoptysis — mild to massive
- Pneumothorax
- Cor pulmonale — from chronic hypoxia and pulmonary hypertension
- Respiratory failure — leading cause of death in CF
- Allergic bronchopulmonary aspergillosis (ABPA)
- Nasal polyps & chronic sinusitis
8. 🫧 Respiratory Distress Syndrome (RDS) / Neonatal
- Primarily in premature neonates (<34 weeks); surfactant deficiency
Complications:
- Intraventricular hemorrhage (IVH)
- Pulmonary interstitial emphysema (PIE)
- Pneumothorax, pneumomediastinum
- Bronchopulmonary dysplasia (BPD) — chronic lung disease of prematurity
- Pulmonary hypertension
- Retinopathy of prematurity (from oxygen therapy)
9. 🦠 Bronchopulmonary Dysplasia (BPD)
- Chronic lung disease following prematurity/mechanical ventilation
Complications:
- Recurrent respiratory infections
- Reactive airway disease / asthma-like symptoms
- Pulmonary hypertension
- Neurodevelopmental delay
- Growth failure
10. ⚡ Acute Respiratory Distress Syndrome (ARDS) in Children
- Can follow sepsis, pneumonia, trauma, near-drowning
Complications:
- Multi-organ dysfunction syndrome (MODS)
- Ventilator-induced lung injury (VILI)
- Pulmonary fibrosis (long-term)
- Neurocognitive impairment post-recovery
- High mortality if severe
Summary Table of Key Complications by Condition
| Condition | Life-Threatening Complications | Chronic Complications |
|---|---|---|
| Pneumonia | Empyema, sepsis, necrotizing pneumonia | Bronchiectasis |
| Bronchiolitis | Apnea, respiratory failure | Recurrent wheeze, asthma |
| Asthma | Status asthmaticus, arrest | Fixed obstruction, steroid side effects |
| OSA | Nocturnal hypoxemia | Cor pulmonale, neurocognitive delay |
| Croup | Bacterial tracheitis, respiratory failure | — |
| Pertussis | Apnea, PH, pneumonia (infant death) | — |
| Cystic Fibrosis | Hemoptysis, respiratory failure | Bronchiectasis, cor pulmonale |
| RDS (Neonatal) | Pneumothorax, IVH | BPD, pulmonary HTN |
| ARDS | MODS, death | Pulmonary fibrosis |
High-Risk Groups for Worse Complications
- Infants <2 years and premature neonates
- Children with congenital heart disease
- Immunocompromised patients (oncology, HIV, transplant)
- Children with neuromuscular disease (poor cough)
- Those with comorbid conditions (complication rate: 15.7% vs 6.7% in healthy children)
Sources:
- Day Case Paediatric Adenotonsillectomy, p. 12
- Management of Pediatric Patients With Oxygen in the Acute Care Setting, p. 8
- Clinical knowledge (Harrison's Principles, Nelson Textbook of Pediatrics)
WITH PHYSIOTHERAPY TREATMENT
search_medical_text
physiotherapy treatment pediatric respiratory complications children
search_medical_text
chest physiotherapy techniques bronchiolitis asthma pneumonia pediatric
search_medical_image
pediatric chest physiotherapy techniques airway clearance
GradeResponse
GradeResponse
GradeResponse
Here is a comprehensive explanation of physiotherapy treatment for each major respiratory complication seen in pediatrics:
Physiotherapy Treatment for Pediatric Respiratory Complications
Core Principles of Pediatric Respiratory Physiotherapy
- Treatment must be age-appropriate — techniques differ for neonates, infants, toddlers, and older children
- Positioning is a cornerstone of all pediatric respiratory PT
- Airway clearance is the primary goal in most conditions
- Treatment must be timed appropriately — not during acute distress, not immediately after feeds
- Play-based techniques are used for toddlers and preschoolers
- Family/caregiver education is essential for home management
Airway Clearance Techniques (ACT) — Foundation of Pediatric Respiratory PT
1. Chest Percussion (Clapping)
- Rhythmic manual tapping on chest wall using cupped hands or two fingers (in neonates)
- Loosens mucus from bronchial walls
- Applied over affected lung segments in postural drainage positions
2. Chest Vibration
- Gentle rapid vibrations applied to chest wall during exhalation
- Mobilizes secretions toward larger airways for clearance
- Used in conjunction with percussion
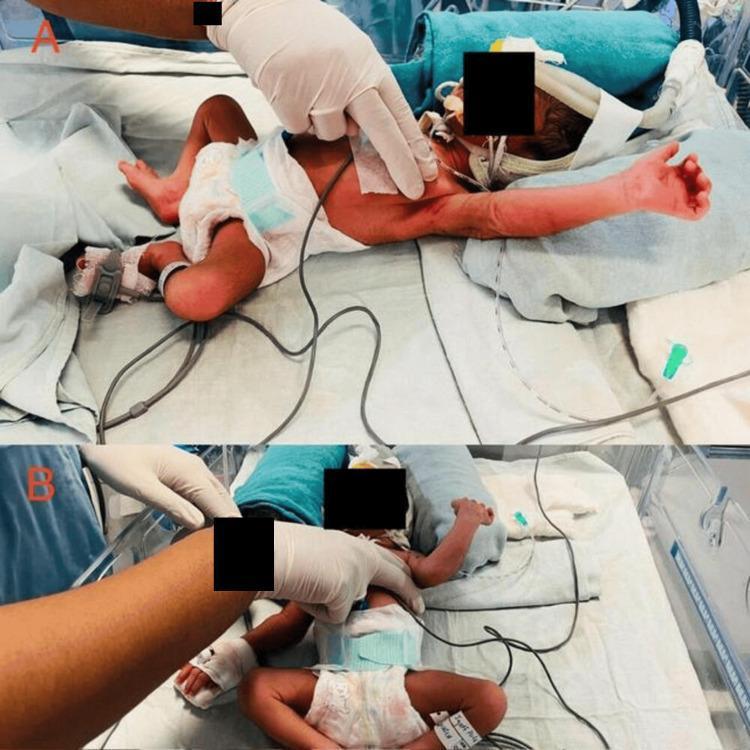
Physiotherapy by Condition
🫁 1. PNEUMONIA
Goals: Mobilize secretions, improve ventilation, prevent atelectasis, restore functional capacity
| Technique | Application |
|---|---|
| Postural Drainage | Position child to use gravity to drain affected lobe (e.g., head-down tilt for lower lobes) |
| Percussion & Vibration | Applied over consolidated segments to loosen secretions |
| Active Cycle of Breathing Technique (ACBT) | For older children (>6 years): breathing control → thoracic expansion exercises → forced expiration technique (FET/huffing) |
| Deep Breathing Exercises | Diaphragmatic breathing, incentive spirometry (older children) |
| Early Mobilization | Sitting out of bed, ambulation as tolerated — reduces complications |
| Positioning | Upright/semi-recumbent to maximize lung expansion; side-lying with affected side up to improve V/Q matching |
| Suctioning | For infants unable to clear secretions independently |
| Oxygen therapy | Target SpO₂ >92%; monitor during all PT sessions |
🌬️ 2. BRONCHIOLITIS (RSV)
Goals: Maintain airway patency, support oxygenation, reduce work of breathing
Note: Routine chest PT (percussion/postural drainage) is NOT recommended in mild bronchiolitis per current evidence. It does not reduce severity or hospital stay.
| Technique | Application |
|---|---|
| Positioning | Semi-upright (30–45°) to reduce work of breathing and improve diaphragmatic excursion |
| Nasal Suctioning | Saline drops + bulb/mechanical suction to clear nasal passages before feeds |
| High-Flow Nasal Cannula (HFNC) support | Physiotherapist assists with positioning and monitoring |
| Slow Expiration with Open Glottis in Infants (ELTGOL) | Used in some centers to assist passive airway clearance |
| Rhinopharyngeal Retrograde Clearance (RRC) | Gentle technique to clear upper airway secretions in infants |
| Apnea monitoring | Positioning to prevent apnea (prone monitoring in NICU, supine in community) |
🤧 3. ASTHMA
Goals: Reduce bronchospasm, improve ventilation, correct breathing pattern, improve exercise tolerance
| Phase | Physiotherapy Techniques |
|---|---|
| Acute attack | Positioning (high sitting/tripod position), controlled breathing, pursed-lip breathing, reassurance |
| Subacute/Stable | Breathing retraining (Buteyko technique, diaphragmatic breathing) |
| Active Cycle of Breathing Technique (ACBT) to clear mucus plugs | |
| Postural drainage if mucus plugging is present | |
| Airway clearance with Flutter/Acapella devices (older children) | |
| Exercise training — graded aerobic exercise to improve cardiorespiratory fitness | |
| Inspiratory muscle training (IMT) — strengthens diaphragm and accessory muscles | |
| Relaxation techniques — reduce anxiety-driven hyperventilation | |
| Long-term | Education on trigger avoidance, inhaler technique, action plans |
Key breathing technique — ACBT:
- Breathing control (relaxed tidal breathing)
- Thoracic expansion exercises (deep breaths ± percussion)
- Forced Expiration Technique (FET/Huffing) — forced exhalation with open glottis to mobilize mucus
😴 4. OBSTRUCTIVE SLEEP APNEA (OSA)
Goals: Reduce upper airway obstruction, improve muscle tone, optimize breathing during sleep
| Technique | Application |
|---|---|
| Positional therapy | Side-lying or semi-prone sleep positioning to prevent tongue base obstruction |
| Myofunctional therapy | Oropharyngeal exercises to strengthen tongue, palate, and pharyngeal muscles — shown to reduce AHI by ~50% |
| Post-adenotonsillectomy respiratory PT | Breathing exercises, early mobilization, SpO₂ monitoring post-op |
| CPAP adherence support | Education and desensitization techniques for mask tolerance in children |
| Weight management exercise | For obese children with OSA |
💨 5. CROUP
Goals: Reduce airway edema effects, minimize distress, support breathing
| Technique | Application |
|---|---|
| Calm positioning | Upright in parent's arms — reduces anxiety and respiratory effort |
| Minimize distress | Avoid unnecessary procedures; crying worsens obstruction |
| Cool mist/humidity | Traditionally used (evidence limited but clinically practiced) |
| Breathing retraining | Post-acute phase breathing exercises for any residual restriction |
🧫 6. PERTUSSIS (Whooping Cough)
Goals: Airway clearance, prevent secondary complications, support oxygenation
| Technique | Application |
|---|---|
| Positioning | Semi-upright to reduce aspiration risk post-coughing episodes |
| Gentle airway suctioning | For infants unable to clear thick secretions |
| Apnea management | Positioning + stimulation; PT input in PICU monitoring |
| Postural drainage (gentle) | For secondary pneumonia with consolidation |
| Oxygen monitoring | SpO₂ monitoring during all sessions given risk of hypoxia |
🌊 7. CYSTIC FIBROSIS (CF)
Goals: Twice-daily airway clearance lifelong, preserve lung function, optimize exercise capacity
This is the condition with the most structured and evidence-based physiotherapy program in pediatrics.
| Technique | Application |
|---|---|
| Postural Drainage & Percussion (PD&P) | Traditional technique; modified in infants (no head-down tilt <6 months) |
| Active Cycle of Breathing Technique (ACBT) | Gold standard in older children |
| Autogenic Drainage (AD) | Self-regulated breathing at different lung volumes to mobilize secretions from periphery to central airways |
| Positive Expiratory Pressure (PEP) mask | Creates back-pressure during expiration; keeps airways open; highly effective |
| Oscillating PEP (Flutter/Acapella/Aerobika) | Combines PEP with oscillations to loosen mucus |
| High-Frequency Chest Wall Oscillation (HFCWO/Vest) | Inflatable vest that delivers oscillations to chest wall; popular in North America |
| Exercise | Critical — aerobic exercise as effective as formal ACT; promotes mucus clearance, maintains fitness |
| Inspiratory Muscle Training | Addresses respiratory muscle weakness |
| Inhalation therapy coordination | Bronchodilator → hypertonic saline/DNase → ACT → inhaled antibiotics (in correct order) |
CF Airway Clearance Progression by Age:
| Age | Recommended ACT |
|---|---|
| 0–2 years | Modified PD&P by caregiver; infant PEP |
| 2–5 years | PEP mask, play-based breathing games |
| 5–12 years | ACBT, Flutter/Acapella, PEP |
| >12 years | ACBT, AD, HFCWO vest, exercise |
🫧 8. NEONATAL RDS / BRONCHOPULMONARY DYSPLASIA (BPD)
Goals: Improve gas exchange, prevent ventilator-induced injury, promote lung development
| Technique | Application |
|---|---|
| Positioning | Prone positioning (in monitored NICU) — improves oxygenation by 10–30% |
| Developmental positioning | Midline, flexed posture to promote neurodevelopment and breathing efficiency |
| Gentle percussion & vibration | Two-finger technique (see image above) for secretion clearance in ventilated neonates |
| Endotracheal suctioning | Coordinated with PT to optimize clearance; avoid over-suctioning |
| Minimal handling protocol | Cluster care; avoid unnecessary stimulation causing desaturation |
| Kangaroo care | Skin-to-skin with parent — improves SpO₂ and respiratory stability |
| Post-NICU follow-up | Breathing exercises, developmental PT as child grows |
⚡ 9. ARDS (Pediatric)
Goals: Optimize lung recruitment, prevent VILI, rehabilitate post-acute
| Phase | Technique |
|---|---|
| Acute (ventilated) | Prone positioning (lung-protective; reduces mortality); positioning changes every 2–4 hours |
| Subacute | Passive and active limb exercises; early mobilization protocol |
| Recovery | Breathing retraining, progressive aerobic exercise, inspiratory muscle training |
| Post-PICU rehabilitation | Address muscle weakness, exercise intolerance, neurocognitive rehabilitation |
Summary: Physiotherapy Techniques Quick Reference
| Technique | Conditions Used |
|---|---|
| Postural Drainage & Percussion | Pneumonia, CF, BPD |
| ACBT (Huffing/FET) | Asthma, CF, Pneumonia |
| PEP / Oscillating PEP (Flutter, Acapella) | CF, Bronchiectasis |
| HFCWO Vest | CF (older children) |
| Nasal Suctioning | Bronchiolitis, Pertussis, Neonates |
| Prone Positioning | ARDS, RDS/BPD (NICU) |
| Upright/Semi-recumbent Positioning | Asthma, Bronchiolitis, Pneumonia |
| Breathing Retraining (Buteyko, Diaphragmatic) | Asthma, Post-ARDS |
| Inspiratory Muscle Training | Asthma, CF, BPD |
| Exercise Therapy | CF, Asthma, OSA |
| Myofunctional Therapy | OSA |
| Kangaroo Care | Neonatal RDS |
General Physiotherapy Precautions in Pediatrics
- ❌ Avoid head-down tilt in infants <6 months (reflux/aspiration risk)
- ❌ Avoid percussion over bare skin, spine, kidneys, or surgical sites
- ❌ Do not perform PT immediately post-feeds (30–45 min wait)
- ❌ Avoid during acute severe bronchospasm without bronchodilator pre-treatment
- ✅ Always monitor SpO₂ before, during, and after PT sessions
- ✅ Stop if child shows signs of distress, significant desaturation, or tachycardia
Sources:
- Management of Pediatric Patients With Oxygen in the Acute Care Setting, p. 8
- Day Case Paediatric Adenotonsillectomy, p. 12
- Clinical knowledge: Nelson Textbook of Pediatrics, ACPCF Guidelines, ERS/ATS Pediatric Respiratory Guidelines
This is a shared conversation. Sign in to Orris to start your own chat.