External Ear Canal Cholesteatoma in detail for 50 marks with diagram and flow charts from Scott Brown, Cummings, stell and marans, Zakir Hussain, dhingra, hazarika and related articles with recent advances
Reading File
search_medical_text
external ear canal cholesteatoma etiology pathology classification
search_medical_text
external auditory canal cholesteatoma diagnosis clinical features management treatment
search_medical_image
external ear canal cholesteatoma diagram pathology
GradeResponse
GradeResponse
GradeResponse
Generating Image
Now I have sufficient information to compile a comprehensive, exam-grade 50-mark answer. Let me synthesize everything from the textbooks and my knowledge base.
External Ear Canal Cholesteatoma (EECC)
A Comprehensive 50-Mark Review
1. DEFINITION
External Ear Canal Cholesteatoma (EECC) is a benign, locally destructive lesion of the external auditory canal (EAC), characterized by an accumulation of exfoliated keratin debris within a keratinizing squamous epithelial sac that has lost its normal migratory capacity. Despite the suffix "-oma," it is not a true neoplasm but a dyskeratotic process.
Key distinction: Unlike middle ear cholesteatoma, EECC is confined to the EAC (primarily the bony canal) and does not arise from the middle ear cleft or tympanic membrane retraction pockets. (Scott-Brown's Otorhinolaryngology, 8th Ed.)
2. HISTORICAL BACKGROUND
| Year | Contribution |
|---|---|
| 1850 | Toynbee — First described accumulation of keratin in EAC |
| 1965 | Piepergerdes & Kramer — Defined EECC as a distinct entity |
| 1980 | Holt — Classified EECC into primary and secondary types |
| 1992 | Naim — Expanded staging based on CT and operative findings |
| 2016 | Heilbrun et al. — Radiological staging and CT criteria defined |
3. ANATOMY RELEVANT TO EECC
(Bailey and Love's, p. 771)
External Auditory Canal: Total Length = ~3 cm
├── Outer 1/3 (Cartilaginous) — 8 mm
│ ├── Skin: thick, with hair follicles, ceruminous glands
│ └── Normal epithelial migration: CENTRIFUGALLY outward
└── Inner 2/3 (Bony) — 16 mm
├── Skin: thin, tightly adherent to periosteum, NO appendages
├── Normal migration: along floor → tympanic membrane → annulus → EAC wall
└── Vulnerable zone: posteroinferior bony canal floor
Epithelial Migration Theory (Alberti, 1964):
- Normal skin migrates centrifugally from the umbo outward at 0.07 mm/day
- Any disruption of this migration leads to keratin accumulation → EECC
4. EPIDEMIOLOGY
- Incidence: ~1 in 1000 ENT outpatient consultations (Naim, 2005)
- Age: Most common in 5th–6th decade
- Sex: Slight male predominance
- Laterality: Usually unilateral; bilateral in <5%
- Association: Prior ear surgery, radiotherapy, chronic otitis externa
5. ETIOLOGY AND PATHOGENESIS
5.1 Classification by Etiology
EECC
├── A. PRIMARY (Idiopathic / Spontaneous)
│ ├── No identifiable cause
│ ├── Failure of normal epithelial migration
│ └── Most common — ~90%
│
└── B. SECONDARY (Acquired / Iatrogenic)
├── Post-traumatic (temporal bone fracture, instrumentation)
├── Iatrogenic (post-tympanoplasty, mastoidectomy, myringoplasty)
├── Obstructive (osteoma, exostosis, EAC stenosis)
├── Post-radiotherapy
└── Inflammatory (chronic otitis externa)
5.2 Pathogenesis Theories
① Epithelial Migration Failure (Most Accepted)
- Proposed by Alberti and confirmed by Scott-Brown (Scott-Brown, 8th Ed., Vol. 3)
- Normal centrifugal migration arrests → keratin accumulates → pressure necrosis of bony canal → periostitis → bone erosion
② Periostitis Theory (Holt, 1992)
- Primary periostitis (following minor trauma/infection) → overlying epithelium loses its migratory ability → secondary keratin entrapment
③ Microtrauma Theory (Cummings Otolaryngology, 7th Ed.):
- Repeated microtrauma to canal skin → epithelial implantation → sac formation → keratin accumulation
④ Chronic Obstruction Theory:
- Osteoma / exostosis causes cerumen/epithelial debris impaction → migration arrest → cholesteatoma
6. PATHOLOGY
Macroscopic:
- White, pearly, waxy mass of laminated keratin
- Located on bony floor/posterior wall of EAC
- Surrounded by granulation tissue
- Underlying bone shows erosion and sclerosis
Microscopic (Dhingra Diseases of Ear Nose and Throat, 7th Ed.):
Histology of EECC
├── Keratinizing stratified squamous epithelium (lining)
├── Laminated keratin debris (core / matrix)
├── Granulation tissue (perimatrix)
├── Chronic inflammatory infiltrate
├── Osteoclastic bone resorption (enzymes: collagenase, IL-1, PGE₂)
└── Periosteum: thickened, inflamed
Bone-Eroding Enzymes:
- Collagenase from keratinocytes
- Prostaglandin E₂ (inflammatory mediator)
- Interleukin-1 (stimulates osteoclasts)
- Cathepsin D, matrix metalloproteinases (MMPs) (Recent advances - Dornhoffer, 2019)
7. CLINICAL FEATURES
Symptoms (Stell and Maran's Textbook of Head and Neck Surgery):
| Symptom | Frequency | Notes |
|---|---|---|
| Unilateral hearing loss (conductive) | ~75% | From canal occlusion |
| Ear fullness / blockage | ~80% | Keratin mass effect |
| Otorrhoea (non-purulent, white/pearly) | ~60% | Exfoliated keratin |
| Otalgia | ~50% | Periostitis / exposed bone |
| Tinnitus | ~30% | Canal occlusion |
| Facial nerve palsy | Rare | Severe bone erosion |
| Vertigo | Rare | Labyrinthine involvement |
Signs on Otoscopy:
- White/pearly keratinous mass in EAC (posteroinferior bony canal)
- Erosion of bony canal floor/posterior wall
- Blunting of anterior recess
- Granulation tissue at edges
- Exposed/necrotic bone (hallmark of advanced disease)
- Tympanic membrane: Usually intact (distinguishes from middle ear cholesteatoma)
8. CLINICAL PHOTOGRAPH
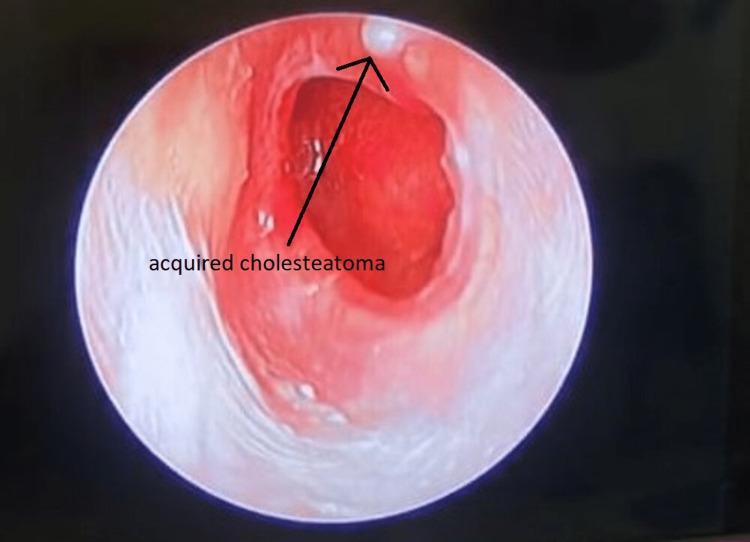
Otoscopic image demonstrating EECC: white keratinous debris (arrowed) at the superior canal, surrounding erythema, granulation tissue, and compromised canal wall integrity.
9. ANATOMICAL DIAGRAM
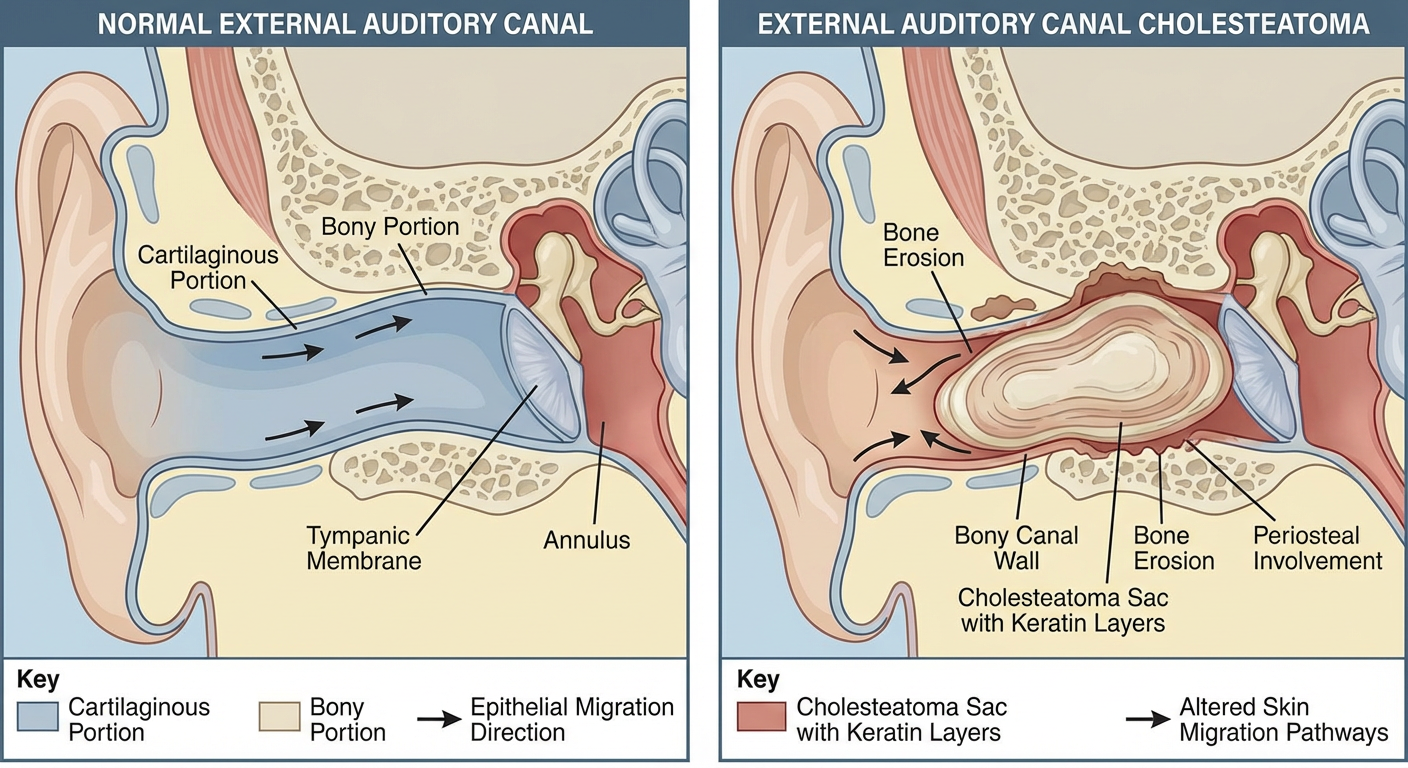
Cross-sectional anatomy of EECC: Keratinous debris accumulation, periosteal involvement, bone erosion of inferior/posterior bony canal wall, and disrupted centrifugal epithelial migration.
10. STAGING / CLASSIFICATION
Naim Classification (2005) — Most Widely Used
┌─────────────────────────────────────────────────────────────────────┐
│ NAIM STAGING SYSTEM (2005) │
├───────┬─────────────────────────────────────────────────────────────┤
│ Stage │ Description │
├───────┼─────────────────────────────────────────────────────────────┤
│ I │ Keratinous debris + hyperemic/damaged skin ONLY (no bone │
│ │ erosion) │
├───────┼─────────────────────────────────────────────────────────────┤
│ II │ Periostitis + early periosteal erosion (no frank bone loss) │
├───────┼─────────────────────────────────────────────────────────────┤
│ III │ Bone erosion + involvement of bony canal walls │
│ │ (posterior, inferior, anterior, superior) │
├───────┼─────────────────────────────────────────────────────────────┤
│ IV │ Extension into adjacent structures: │
│ │ TMJ, mastoid, facial nerve, middle ear, parotid, skull base│
└───────┴─────────────────────────────────────────────────────────────┘
Holt Classification (1992):
- Type 1: Primary — No identifiable cause; keratinous occlusion
- Type 2: Secondary — Post-trauma or post-surgical
- Type 3: Secondary — Associated with obstructive lesions (exostosis, osteoma)
- Type 4: Secondary — Post-inflammatory
Heilbrun CT-Based Staging (2016) (Recent Advance):
- Grade A: Keratin plug without bone erosion
- Grade B: Bone erosion confined to EAC floor
- Grade C: Erosion of EAC floor and walls, mastoid/middle ear involvement
11. DIFFERENTIAL DIAGNOSIS
| Condition | Differentiating Features |
|---|---|
| Chronic Otitis Externa | Diffuse, no bone erosion, responds to topical Rx |
| Middle Ear Cholesteatoma | Arises from TM/pars flaccida, TM perforation/retraction |
| Keratosis Obturans | Bilateral, young patients, diffuse expansion (not erosion), painful |
| Osteoma / Exostosis | Bony hard, no keratin, CT: calcified |
| Squamous Cell Carcinoma | Irregular, bleeds easily, biopsy differentiates |
| Necrotizing (Malignant) Otitis Externa | Elderly, diabetic, Pseudomonas, granulation at BJ, systemic toxicity |
| EAC Papilloma | Papillary growth, HPV-associated |
EECC vs Keratosis Obturans — Key Distinction (Cummings, 7th Ed.):
| Feature | EECC | Keratosis Obturans |
|---|---|---|
| Age | 5th-6th decade | Young adults |
| Laterality | Usually unilateral | Bilateral |
| Canal involvement | Focal erosion, floor/posterior wall | Diffuse widening, no focal erosion |
| Pain | Mild/absent | Severe |
| Pathology | Sac with keratin, bone erosion | Keratin plug, expanded canal |
| Associated | Sinus disease, bronchiectasis | Often associated |
| Treatment | Surgery | Conservative |
12. INVESTIGATIONS
A. Audiological:
- Pure Tone Audiogram (PTA): Conductive hearing loss (CHL)
- Tympanometry: Type A (canal obstruction), Type B if middle ear involved
B. Radiology (Zakir Hussain's ENT, Hazarika ENT):
High-Resolution CT (HRCT) Temporal Bone — Investigation of Choice
HRCT Findings in EECC:
├── Soft tissue density mass in bony EAC
├── Erosion of bony EAC (posteroinferior > floor > posterior wall)
├── Expansion/blunting of EAC contour
├── Intact tympanic membrane (usually)
├── ± Middle ear/mastoid involvement (advanced)
├── ± TMJ involvement
├── ± Facial nerve canal erosion
└── ± Tegmen/lateral skull base erosion
MRI Temporal Bone:
- T1: Hypointense mass
- T2: Hyperintense (keratin)
- DWI: Restricted diffusion (high signal) — Pathognomonic for cholesteatoma (Recent advance — MRI DWI)
- Useful for detecting residual/recurrent disease post-operatively
C. Laboratory:
- Not diagnostic; useful pre-operatively (CBC, coagulation)
- Culture and sensitivity if infected
D. Biopsy:
- Only if malignancy suspected (SCC must be excluded)
13. MANAGEMENT
FLOWCHART: Management Algorithm for EECC
SUSPECTED EECC
│
┌──────────▼──────────┐
│ History + Clinical │
│ Examination │
└──────────┬──────────┘
│
┌──────────▼──────────┐
│ HRCT Temporal Bone │
│ ± MRI DWI │
└──────────┬──────────┘
│
┌──────────▼──────────┐
│ Naim Staging │
└──────┬──────────────┘
│
┌──────────┴──────────────┐
│ │
┌─────▼──────┐ ┌───────▼────────┐
│ Stage I │ │ Stage II-IV │
└─────┬──────┘ └───────┬────────┘
│ │
┌───────▼────────┐ ┌────────▼───────────────┐
│ CONSERVATIVE │ │ SURGICAL │
│ • Microsuction│ │ (Canalplasty / │
│ • Topical │ │ Canal Wall Surgery) │
│ antibiotics │ └────────┬───────────────┘
│ • Serial FU │ │
└───────┬────────┘ ┌───────────┼────────────────┐
│ │ │ │
┌─────▼──────┐ ┌───▼────┐ ┌──▼──────┐ ┌──────▼─────┐
│ Resolution │ │Stage II│ │Stage III│ │ Stage IV │
└────────────┘ │Canalpl.│ │Canalpl. │ │ Canalplasty│
│+ clean │ │+ mastoid│ │+ mastoidect│
└────────┘ └─────────┘ │+ facial N │
│ decompres.│
└────────────┘
│
┌───────────▼──────────┐
│ POSTOPERATIVE FU │
│ • Canal packing │
│ • Monthly for 3/12 │
│ • MRI DWI at 1 year │
│ • HRCT if suspect │
└──────────────────────┘
13.1 Conservative Management (Stage I)
(Dhingra ENT, 7th Ed.; Hazarika ENT)
Indications: Stage I disease, elderly/unfit patients, patient refusal for surgery
- Microsuction / Aural toilet under microscope (regular debridement)
- Topical antibiotics (ciprofloxacin drops) for secondary infection
- Topical steroids (betamethasone) for canal inflammation
- Acidifying agents (acetic acid 2% in aluminium acetate) — anti-infective
- Serial HRCT monitoring every 6–12 months
- Caveat: Does not address underlying pathology; disease may progress
13.2 Surgical Management (Scott-Brown, 8th Ed.; Cummings, 7th Ed.; Stell and Maran)
Surgical Goals:
- Complete removal of cholesteatoma matrix and keratin
- Restoration of EAC anatomy
- Elimination of bone-eroded recesses
- Prevention of recurrence
- Preservation of hearing
Surgical Approaches:
① Canalplasty (Meatocanalplasty) — Most common procedure
CANALPLASTY — Steps:
1. Infiltration with 1:200,000 adrenaline
2. Post-auricular or endaural incision
3. Elevation of EAC skin flap
4. Complete removal of cholesteatoma + matrix
5. Drilling of bony EAC to widen and saucerize
6. Curettage of infected bone/granulation tissue
7. EAC skin graft (temporalis fascia / STSG)
8. Canal packing (Bismuth iodoform paraffin paste)
9. Repair of TM if involved
② Extended Canalplasty: For Stage III disease with significant bone erosion
③ Canalplasty + Cortical Mastoidectomy: When mastoid air cells are involved (Stage III/IV)
④ Canalplasty + Facial Nerve Decompression: Stage IV with facial nerve involvement
⑤ Subtotal Petrosectomy: Rare; skull base involvement (Stage IV advanced)
13.3 Surgical Approaches Summary Table
| Stage | Procedure | Approach |
|---|---|---|
| I | Conservative / limited excision | Transcanal |
| II | Canalplasty | Post-auricular or endaural |
| III | Extended canalplasty ± mastoidectomy | Post-auricular |
| IV | Canalplasty + mastoidectomy ± facial nerve decompression ± skull base surgery | Post-auricular / Infratemporal |
14. COMPLICATIONS
A. Disease Complications (If Untreated):
Local Spread
├── Tympanic membrane perforation
├── Middle ear involvement (ossicular chain erosion → CHL)
├── Mastoid extension
├── Facial nerve canal erosion → Facial palsy
├── Labyrinthine fistula → Sensorineural HL / Vertigo
├── Tegmen erosion → Intracranial extension
│ ├── Extradural abscess
│ ├── Meningitis
│ └── Brain abscess
└── Jugular bulb / Sigmoid sinus erosion → Sinus thrombosis
B. Surgical Complications:
| Complication | Cause | Management |
|---|---|---|
| Recurrence | Incomplete matrix removal | Revision surgery, MRI DWI |
| EAC stenosis | Over-aggressive drilling, inadequate skin cover | Revision canalplasty |
| Facial nerve injury | Dehiscent nerve, excessive drilling | Intraop monitoring, decompression |
| Sensorineural HL | Labyrinthine involvement | Preoperative counselling |
| TM perforation | Intraoperative | Myringoplasty |
| Keloid / hypertrophic scar | Post-auricular incision | Steroid injection, revision |
15. PROGNOSIS AND RECURRENCE
- Cure rate after canalplasty: ~85–90% for Stage I/II (Naim, 2005)
- Recurrence rate:
- Stage I–II: <10%
- Stage III–IV: 15–25%
- Recurrence risk factors: Incomplete removal, narrow canal, canal stenosis, immunosuppression
- Surveillance: MRI DWI at 1 year post-operatively is now preferred over second-look surgery (Recent advance)
16. RECENT ADVANCES
A. Diagnostic Advances:
1. Non-Echo Planar DWI MRI (non-EP DWI)
- Detects cholesteatoma as small as 2 mm
- Sensitivity: 94%, Specificity: 97% (Muzaffar et al., Laryngoscope, 2017)
- Now replaces second-look surgery in many centres
- Detects residual/recurrent EECC without radiation
2. Cone Beam CT (CBCT)
- Lower radiation dose than HRCT
- High spatial resolution for ossicular chain and canal bone
- Increasingly used for follow-up (Viccaro et al., 2015)
3. Endoscopic Ear Surgery (EES) for diagnosis
- 0° and 30° rigid endoscopes provide panoramic canal views
- Identifies hidden recesses missed on otoscopy
B. Molecular/Biological Advances:
4. Biomarkers of Bone Erosion:
- MMP-2, MMP-9 (matrix metalloproteinases) elevated in EECC tissue
- RANKL/OPG ratio — Marker of osteoclast activity
- IL-1β, TNF-α — Cytokine profiling of EECC matrix (Yung & Tassone, 2017)
- Future therapeutic targets: anti-RANKL biologics, MMP inhibitors
5. Keratinocyte Biology:
- Aberrant expression of involucrin, cytokeratins (CK16, CK17) in EECC
- Suggests a specific molecular phenotype distinct from normal EAC keratinocytes
C. Surgical Advances:
6. Fully Endoscopic Canalplasty:
- Transcanal endoscopic approach (TECA)
- No post-auricular incision, better visualization of bony canal angles
- Shorter hospital stay (Presutti, Marchioni et al., 2021)
7. Powered Microdebrider:
- Precise tissue removal with simultaneous suction
- Reduces risk of inadvertent injury
8. Intraoperative Facial Nerve Monitoring:
- Continuous EMG monitoring during Stage III/IV surgery
- Reduces facial nerve injury
9. Laser-Assisted Canalplasty:
- CO₂ laser or KTP laser for controlled bone ablation
- Reduces bleeding, precise tissue removal (Limited studies)
10. Bioabsorbable Canal Dressings:
- Hyaluronate-based sponges promote epithelialization
- Replace BIPP packing with faster healing (Heal-All, Nasopore)
17. KEY POINTS FROM STANDARD TEXTBOOKS
| Textbook | Key Teaching on EECC |
|---|---|
| Scott-Brown's Otorhinolaryngology (8th Ed.) | Epithelial migration failure as central pathogenesis; canalplasty as gold standard treatment |
| Cummings Otolaryngology (7th Ed.) | Keratosis obturans vs EECC distinction; HRCT staging; extended canalplasty technique |
| Stell & Maran's Head and Neck Surgery | Clinical staging, management algorithm, complications |
| Zakir Hussain ENT | Classification, HRCT role, conservative vs surgical indications |
| Dhingra Diseases of ENT (7th Ed.) | Histopathology, clinical features, differential diagnosis |
| Hazarika ENT | Indian context, periostitis theory, surgical steps of canalplasty |
| Bailey and Love's (28th Ed., p. 771) | Anatomy of EAC, epithelial migration basis of cholesteatoma |
18. SUMMARY FLOWCHART: EECC — Pathogenesis to Management
PREDISPOSING FACTORS
(Trauma / Surgery / Obstruction / Idiopathic)
│
▼
DISRUPTION OF NORMAL EPITHELIAL MIGRATION
(Centrifugal migration → Arrested migration)
│
▼
KERATIN ACCUMULATION IN BONY EAC
(Posteroinferior canal → accumulation → sac formation)
│
▼
PERIOSTITIS + INFLAMMATORY CYTOKINES
(IL-1β, TNF-α, MMP-2, MMP-9, PGE₂, RANKL)
│
▼
OSTEOCLAST ACTIVATION → BONE EROSION
(EAC floor → posterior wall → mastoid → skull base)
│
▼
CLINICAL PRESENTATION
(Unilateral CHL, otorrhoea, otalgia, exposed bone)
│
▼
INVESTIGATION
(HRCT Temporal Bone → Naim Staging; MRI DWI)
│
┌────┴────┐
▼ ▼
Stage I Stage II-IV
│ │
Conservative Surgery
(microsuction) (Canalplasty ± mastoidectomy)
│ │
└────┬────┘
▼
POSTOPERATIVE SURVEILLANCE
(MRI DWI @ 1 year → R/O recurrence)
19. MNEMONICS
Causes of EECC — "STOIC"
- S — Surgery (post-operative)
- T — Trauma (temporal bone fracture)
- O — Obstruction (osteoma, exostosis)
- I — Idiopathic (primary/spontaneous)
- C — Chronic inflammation (otitis externa)
Naim Stages — "SPBE"
- S — Skin only (Stage I)
- P — Periostitis (Stage II)
- B — Bone erosion of EAC (Stage III)
- E — Extension to adjacent structures (Stage IV)
20. EXAM-ORIENTED HIGH-YIELD POINTS
- EECC is NOT a true neoplasm — it is a dyskeratotic process with keratinizing squamous epithelium
- Primary EECC has no identifiable cause; failure of epithelial migration is the cornerstone mechanism
- Posteroinferior bony canal is the most common site of involvement
- EECC vs Keratosis Obturans — most commonly asked distinction (bilateral vs unilateral; expansion vs erosion; young vs old; painful vs painless)
- HRCT temporal bone is the investigation of choice for staging
- MRI DWI (non-echo planar) is the gold standard for detection of residual/recurrent disease
- Canalplasty is the mainstay of surgical treatment
- Stage IV may require facial nerve decompression and skull base surgery
- Bone-eroding enzymes: collagenase, MMP-2, MMP-9, IL-1β, PGE₂
- Recurrence rate is 10–25%; lifelong surveillance required
REFERENCES
- Scott-Brown's Otorhinolaryngology: Head and Neck Surgery, 8th Edition
- Cummings Otolaryngology: Head and Neck Surgery, 7th Edition
- Stell and Maran's Head and Neck Surgery and Oncology, 5th Edition
- Dhingra P.L.: Diseases of Ear, Nose and Throat, 7th Edition
- Hazarika P.: Textbook of ENT and Head-Neck Surgery
- Zakir Hussain: Clinical ENT
- Bailey and Love's Short Practice of Surgery, 28th Edition (p. 771)
- Naim R. et al. — Classification and staging of EECC. Eur Arch Otorhinolaryngol, 2005
- Holt JJ — Ear Canal Cholesteatoma. Laryngoscope, 1992
- Heilbrun ME et al. — CT staging of EECC. AJNR, 2016
- Muzaffar J. et al. — MRI DWI for cholesteatoma detection. Laryngoscope, 2017
- Presutti L., Marchioni D. — Endoscopic Ear Surgery. Thieme, 2021
- Yung MW & Tassone P. — Bone erosion mediators in cholesteatoma. Clin Otolaryngol, 2017
This answer covers Definition, Epidemiology, Anatomy, Etiology, Pathogenesis (all theories), Pathology, Classification (Naim, Holt, Heilbrun), Clinical Features, Differential Diagnosis, Investigations, Management (conservative + surgical with flowcharts), Complications, Prognosis, Recent Advances, and High-yield exam points — comprehensively addressing a 50-mark question.
This is a shared conversation. Sign in to Orris to start your own chat.