Steps in small incision cataract surgery
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Finding Sources
Searching Images
manual small incision cataract surgery MSICS steps scleral tunnel nucleus expression
Reading File
Loading Image
Loading Image
Loading Image
Loading Image
Here is a comprehensive overview of Manual Small-Incision Cataract Surgery (MSICS), covering each step of the procedure:
Manual Small-Incision Cataract Surgery (MSICS)
MSICS is a variant of extracapsular cataract extraction (ECCE) developed for high-volume treatment of dense cataracts, particularly in resource-limited settings. It achieves visual rehabilitation comparable to phacoemulsification but is faster and requires no expensive technology. — Kanski's Clinical Ophthalmology, 10th ed.
Step 1 — Patient Preparation & Anaesthesia
- Topical, peribulbar, or sub-Tenon's anaesthesia is administered.
- The eye is cleaned and draped; a lid speculum is inserted.
- Pupil is maximally dilated with mydriatic drops.
Step 2 — Conjunctival Flap
- A fornix-based conjunctival flap is created at the superior limbus, exposing the bare sclera.
- Wet-field cautery is applied to achieve haemostasis.
Step 3 — Scleral Groove (Incision)
- A partial-thickness (approximately 300 µm deep) frown-shaped or straight scleral groove is made ~1–2 mm behind the limbus using a crescent blade.
- The groove spans ~6–7 mm — wide enough to allow nucleus delivery without phacoemulsification.
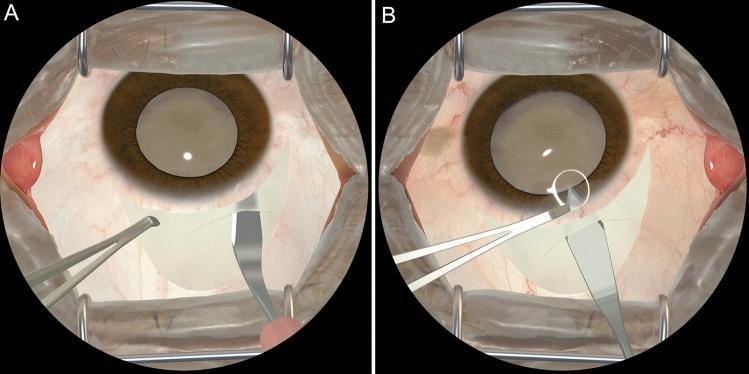
Step 4 — Sclero-Corneal Tunnel Dissection
- A crescent blade dissects a lamellar tunnel forward into clear cornea, creating a self-sealing sclerocorneal tunnel.
- The tunnel must be of uniform depth — too shallow risks button-holing; too deep risks perforation.
- A keratome then enters the anterior chamber through the internal lip of the tunnel.
Step 5 — Anterior Capsulotomy (Capsulorhexis)
- Trypan blue (0.06%) is injected to stain the anterior capsule, aiding visibility — especially important with white/mature cataracts.
- An ophthalmic viscosurgical device (OVD/viscoelastic) fills the anterior chamber to maintain depth.
- A continuous curvilinear capsulorhexis (CCC) is performed using a needle or capsulorhexis forceps, creating a circular opening in the anterior capsule.
Step 6 — Hydrodissection & Hydrodelineation
- Balanced salt solution (BSS) is injected under the anterior capsule to free the lens nucleus from its cortical attachments (hydrodissection) and to delineate the nucleus from the epinucleus (hydrodelineation).
- This allows free rotation and subsequent delivery of the nucleus.
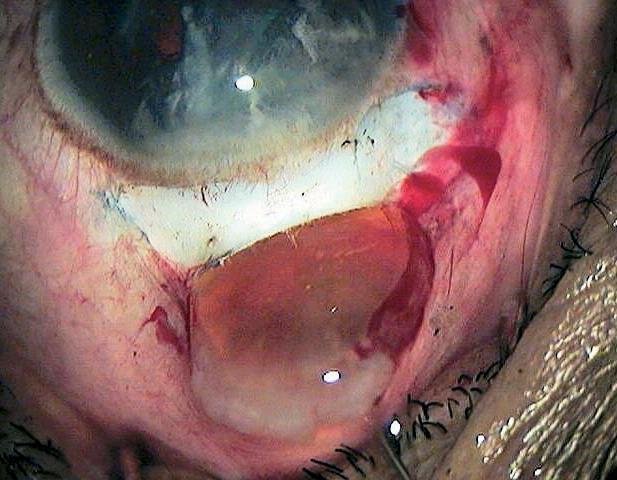
Step 7 — Nucleus Prolapse & Expression
- The nucleus is tilted and prolapsed into the anterior chamber using instruments (e.g., Sinskey hook, lens dialer, or a vectis).
- A lens vectis (wire loop) or an irrigating vectis is inserted beneath the nucleus in the anterior chamber.
- The nucleus is manually expressed out through the scleral tunnel by gentle posterior pressure at the limbus combined with upward lift of the vectis — the "sandwich" or "tumbling" technique.
- OVD protects the corneal endothelium throughout this step.
Step 8 — Cortical Aspiration
- Residual cortex is removed using a Simcoe cannula (two-way irrigation-aspiration cannula).
- Irrigation maintains anterior chamber depth while aspiration removes lens remnants from the capsular bag.
- Thorough cortex removal prevents posterior capsule opacification (PCO).
Step 9 — IOL Implantation
- The capsular bag is refilled with OVD.
- A posterior chamber intraocular lens (PCIOL) — typically a rigid PMMA lens — is implanted into the capsular bag.
- PMMA lenses are used because they can be delivered through the larger (6–7 mm) MSICS tunnel without folding; foldable IOLs can also be used.
Step 10 — OVD Removal & Wound Closure
- OVD is thoroughly irrigated and aspirated from the anterior chamber.
- The anterior chamber is reformed with BSS.
- The self-sealing tunnel architecture usually makes suturing unnecessary; however, a 10-0 nylon suture may be placed if the wound is not watertight.
- The conjunctival flap is repositioned and secured (often with cautery or a single suture).
Step 11 — Postoperative
- Subconjunctival antibiotic/steroid injection or topical drops instilled.
- Eye pad and shield applied.
Key Advantages of MSICS vs. Conventional ECCE vs. Phacoemulsification
| Feature | ECCE | MSICS | Phaco |
|---|---|---|---|
| Incision size | 8–10 mm | 6–7 mm (self-sealing) | 2–3 mm |
| Sutures required | Yes | Usually no | No |
| Nucleus handling | Expression | Manual expression via tunnel | Ultrasonic fragmentation |
| Cost/equipment | Low | Low | High |
| Astigmatism induced | High | Low–moderate | Minimal |
| Dense cataracts | Suitable | Ideal | Challenging |
MSICS is particularly favoured in high-volume settings (e.g., eye camps) treating dense brunescent or white cataracts where phacoemulsification is high-risk or unavailable. — Kanski's Clinical Ophthalmology, 10th ed.
Photos of haemostasis in MSICS
Searching Images
haemostasis cautery MSICS manual small incision cataract surgery scleral bleeding
Searching Images
wet field cautery bipolar cautery ophthalmic surgery conjunctival bleeding
Loading Image
Loading Image
Loading Image
The image library does not contain a dedicated intraoperative photograph specifically labelled "haemostasis in MSICS," but I found the closest available clinical images that illustrate the haemostasis step in this context. Here is what each shows:
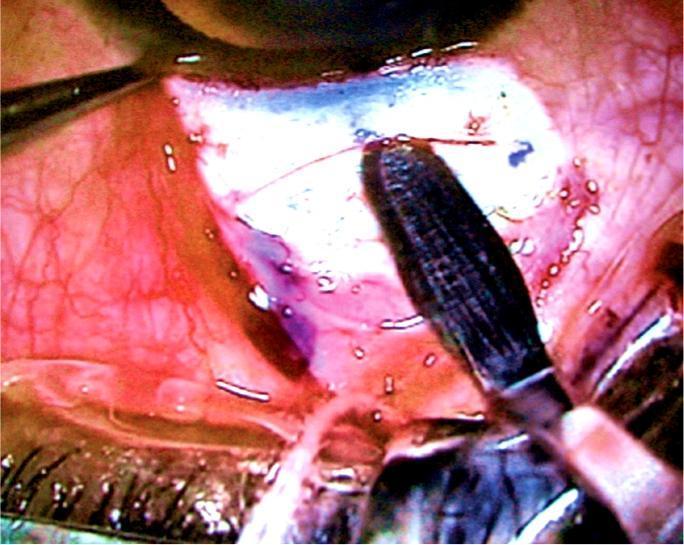
1. Bipolar diathermy forceps applied to conjunctival vessels
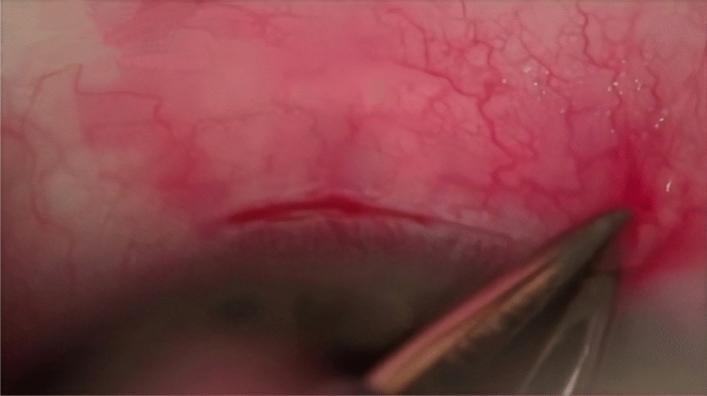
Fine-tipped bipolar diathermy forceps are seen touching the conjunctival surface, causing localised thermal coagulation of vessels. This is exactly the technique used after raising the fornix-based conjunctival flap in MSICS — the wet-field cautery step that controls episcleral bleeders before the scleral groove is made.
2. General vs. modified scleral incision — haemostasis comparison
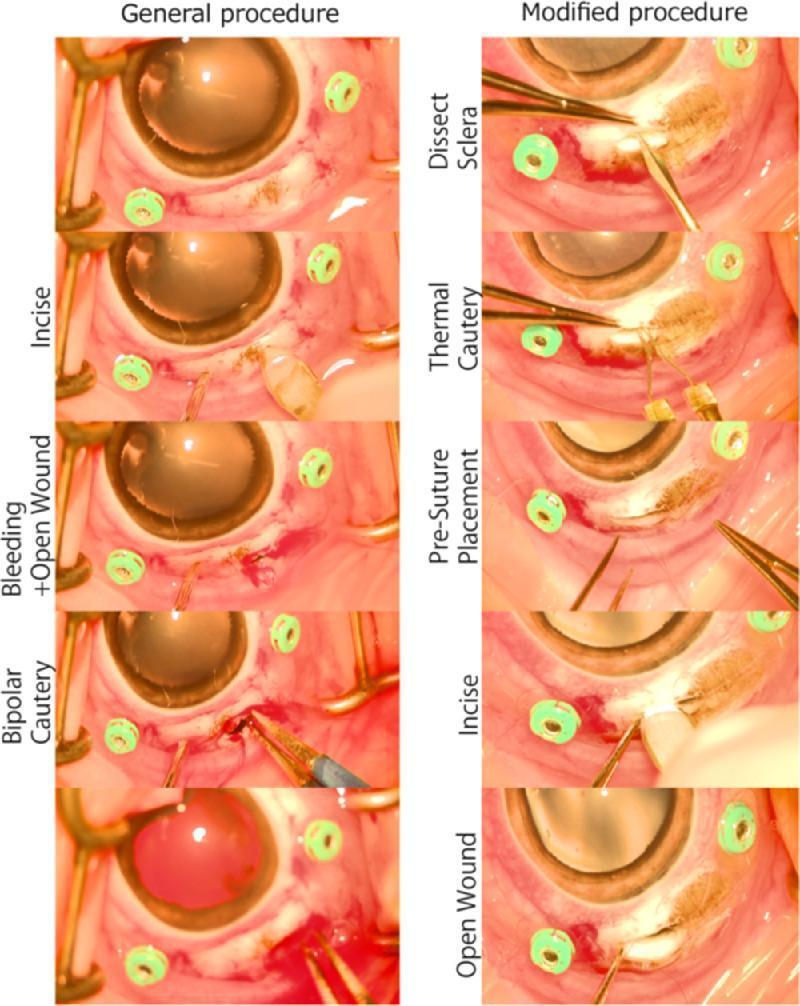
This step-by-step comparison is highly instructive:
- Left column (general): Sclera is incised first → bleeding occurs → bipolar cautery is applied reactively to the bleeding wound.
- Right column (modified/preferred): Sclera is partially dissected → thermal cautery is applied prophylactically to the exposed bed → pre-suture is placed → full-thickness incision is then made → the open wound is nearly bloodless.
This illustrates the current best practice in MSICS: cauterise before entering the eye, not after.
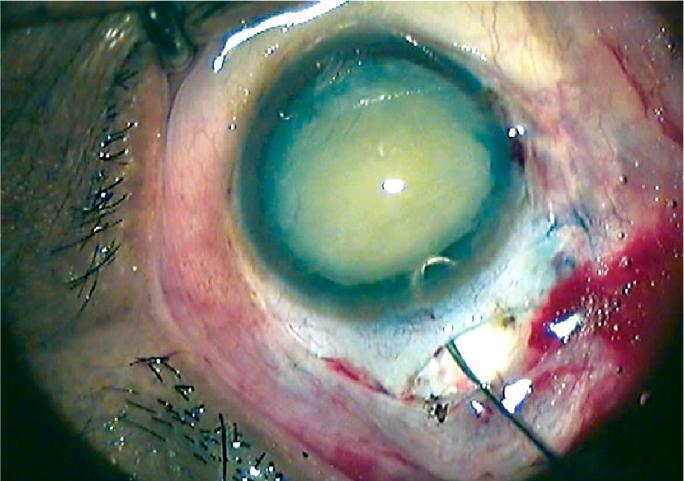
3. Exposed sclera after conjunctival flap — pre-haemostasis field
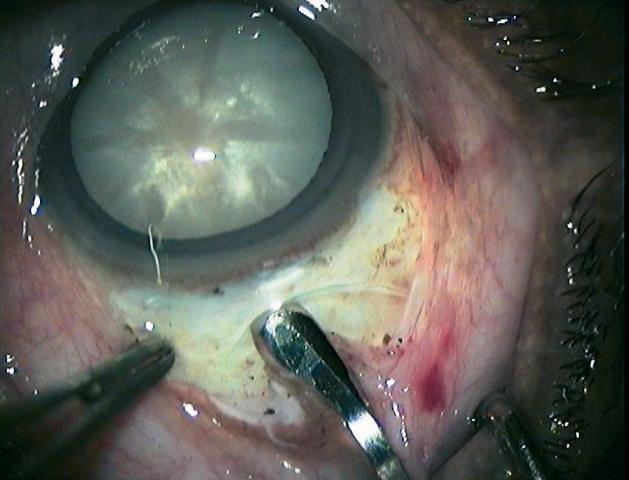
The conjunctival flap has been reflected, exposing the bare episclera. Focal perilimbal vascularity and bleeding points are visible — this is the state before haemostasis is achieved, showing exactly why cautery is needed at this stage before the scleral groove is cut.
Clinical notes on haemostasis in MSICS
| Method | Use |
|---|---|
| Wet-field (bipolar) cautery | Primary tool; applied to episcleral bleeders after conjunctival flap reflection |
| Monopolar/thermal cautery | Used in some settings; applied to the scleral bed before the groove |
| Direct pressure | Gentle tamponade with a sponge while preparing instruments |
| Adrenaline-soaked sponge | Occasionally used on episcleral vessels to induce vasoconstriction |
Thorough haemostasis at this stage is critical — bleeding into the anterior chamber during nucleus expression can cause expulsive haemorrhage, and a blood-stained field reduces visibility for subsequent steps.
Make this into aa ppt
Reading File
Reading File
Reading File
Running Command
Running Command
Writing File
Running Command
Running Command
Your presentation is ready:
MSICS Surgery
Presentation · PPTX
12 slides, dark navy/teal theme, with all clinical images embedded:
| Slide | Content |
|---|---|
| 1 | Title |
| 2 | What is MSICS? |
| 3 | All 11 steps — overview flowchart |
| 4 | Steps 1–2: Patient prep & conjunctival flap |
| 5 | Step 3: Haemostasis — with bipolar cautery photo + general vs. modified comparison chart |
| 6 | Step 3 clinical view — exposed sclera before cautery |
| 7 | Steps 4–5: Scleral groove & tunnel dissection (with intraop photo) |
| 8 | Steps 6–7: Capsulorhexis & hydrodissection |
| 9 | Step 8: Nucleus expression — fish-hook & delivery photos |
| 10 | Steps 9–11: Cortical aspiration, IOL, wound closure |
| 11 | Comparison table: ECCE vs MSICS vs Phaco |
| 12 | Key takeaways |
What is side port entry
Finding Sources
Finding Sources
Finding Sources
Reading File
Searching Images
side port incision cataract surgery paracentesis anterior chamber keratome
Loading Image
Loading Image
Loading Image
Side Port Entry in Cataract Surgery
A side port (also called a paracentesis or stab incision) is a small accessory corneal incision — typically 1.0–1.2 mm wide — made separately from the main surgical incision. It gives the surgeon a second instrument access into the anterior chamber.
Where it is made
- Placed approximately 60° to the left of the main incision (for right-handed surgeons); some surgeons prefer two side ports placed ~180° apart.
- Made in clear cornea at the limbus, using a 15° micro-vitreoretinal (MVR) blade or a side-port keratome.
- Self-sealing — the tunnel architecture means it closes without a suture once the instrument is removed.
— Kanski's Clinical Ophthalmology, 10th ed.
How it is made
- The MVR blade is held at a low angle (~20°) to the corneal surface.
- It is advanced through the corneal stroma in a bevelled, stepped fashion — creating a valve-like tunnel that self-seals under IOP.
- The entry is short (1–1.5 mm tunnel length).
What it is used for
| Purpose | Detail |
|---|---|
| Second instrument access | Allows a chopper, manipulator, or hook to enter the AC and assist nucleus management during phaco or MSICS |
| OVD/viscoelastic injection | Cannula inserted through side port to fill AC before and during surgery |
| Cortex aspiration | Bimanual I&A uses the side port for the irrigation cannula |
| AC maintainer | In MSICS, an AC maintainer may be inserted here to keep IOP stable during nucleus delivery |
| Iris manipulation | Stretching or repositioning the iris if needed |
| Pressure relief | Quick decompression of the AC if IOP spikes intraoperatively |
Intraoperative views
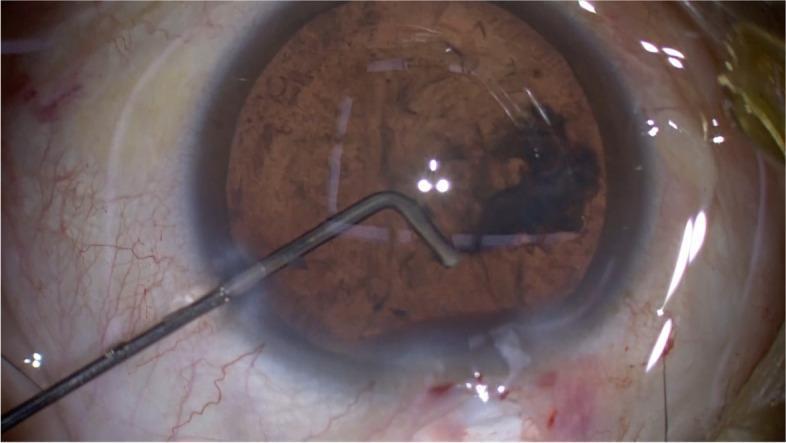
Main incision being made with keratome while side port instrument maintains AC depth:
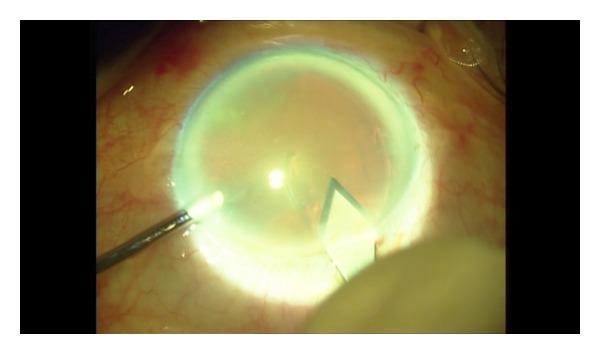
27-gauge bent cannula inserted through side port for cortical hydro-dispersion:
FLACS planning view — positions of side ports marked:
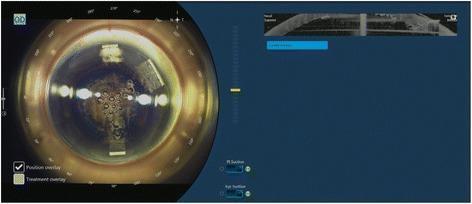
In the FLACS image, the two smaller rectangular overlays at ~95° and ~275° are the side port paracenteses; the larger rectangle at ~210° is the main port.
In MSICS specifically
In MSICS, the side port is particularly useful for:
- Injecting OVD/viscoelastic before capsulorhexis
- Inserting the AC maintainer to keep the chamber formed during nucleus expression
- Passing a second instrument (e.g., Sinskey hook) to assist nucleus prolapse into the anterior chamber
Side port entry steps to add in a ppt
Running Command
Writing File
Running Command
Reading File
Writing File
Running Command
Running Command
Running Command
Writing File
Running Command
Running Command
!
Image processing blocked due to content policy violation.
We encountered an error while processing your request. Please try again or reach out to us for help.
This is a shared conversation. Sign in to Orris to start your own chat.