Pneumonia in children
Reading File
search_medical_text
pneumonia in children etiology clinical presentation diagnosis
search_medical_image
pediatric pneumonia chest X-ray
GradeResponse
GradeResponse
search_medical_text
pediatric pneumonia management antibiotic treatment guidelines
GradeResponse
The retrieval gave limited results on management specifics. I'll synthesize a comprehensive answer using the retrieved content alongside established clinical knowledge.
Pneumonia in Children
Overview
Pneumonia is one of the leading causes of morbidity and mortality in children worldwide. It refers to infection/inflammation of the lung parenchyma and is broadly classified as community-acquired pneumonia (CAP), hospital-acquired pneumonia, or aspiration pneumonia.
Etiology by Age Group
| Age Group | Common Pathogens |
|---|---|
| Neonates (0–4 weeks) | Group B Streptococcus, gram-negative enteric bacteria (E. coli), Listeria |
| Infants (1–3 months) | Chlamydia trachomatis, RSV, parainfluenza, S. pneumoniae |
| 1 month – 5 years | RSV, influenza, parainfluenza, Streptococcus pneumoniae, Haemophilus influenzae |
| School-age (>5 years) | Mycoplasma pneumoniae, Chlamydophila pneumoniae, S. pneumoniae, influenza |
Key point: Viral pneumonia is the most common cause in children under 5. Bacteria become more prominent with increasing age.
Clinical Presentation
Symptoms:
- Fever (may be absent in neonates/young infants)
- Cough (productive or dry)
- Tachypnea — the most sensitive sign
- Dyspnea, grunting, nasal flaring
- Chest pain (older children)
- Poor feeding, lethargy, irritability (infants)
WHO Tachypnea Thresholds:
| Age | Tachypnea Threshold |
|---|---|
| < 2 months | ≥ 60 breaths/min |
| 2–12 months | ≥ 50 breaths/min |
| 1–5 years | ≥ 40 breaths/min |
| > 5 years | ≥ 30 breaths/min |
Signs on examination:
- Dullness to percussion
- Decreased breath sounds or bronchial breathing
- Crackles (fine/coarse)
- Reduced chest expansion on affected side
- Intercostal, subcostal, or suprasternal retractions
As noted in guidelines on HIV-infected children, wheezing makes acute bacterial pneumonia less likely, suggesting viral, atypical bacterial (Mycoplasma), or reactive airway disease instead (Prevention and Treatment of Opportunistic Infections in Children with and Exposed to HIV, p. 32).
Diagnosis
Clinical Diagnosis
Pneumonia is often diagnosed clinically based on fever + respiratory symptoms + signs of consolidation. Chest radiograph supports but is not always required for outpatient management.
Chest X-Ray (CXR)
Bacterial pneumonia: Lobar/segmental consolidation, air bronchograms
Viral/atypical pneumonia: Bilateral interstitial/perihilar infiltrates, hyperinflation, ground-glass opacities
Viral/atypical pneumonia: Bilateral interstitial/perihilar infiltrates, hyperinflation, ground-glass opacities
Below is a representative pediatric CXR showing bilateral patchy interstitial and alveolar opacities in viral pneumonia:
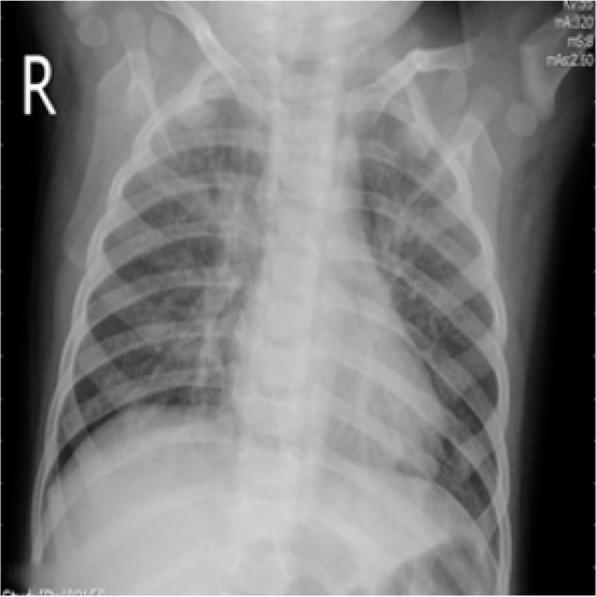
Laboratory Workup
- CBC: leukocytosis with left shift suggests bacterial infection; lymphocytosis more consistent with viral
- CRP / Procalcitonin: elevated in bacterial pneumonia; useful to guide antibiotic decisions
- Blood cultures: low yield (~5%) but important for severe/hospitalized cases
- Nasopharyngeal PCR panel: differentiates viral from bacterial and identifies specific pathogens (e.g., influenza, RSV, Mycoplasma)
- Pleural fluid culture: if pleural effusion present
- Urine antigen tests: for S. pneumoniae (useful in older children/adults)
Molecular diagnostic testing can differentiate viral from bacterial pneumonia and has the potential to decrease hospitalizations and empiric antibiotic use (Prevention and Treatment of OIs in Children with HIV, p. 32).
Severity Assessment
Signs of severe pneumonia (require hospitalization):
- SpO₂ < 92% on room air
- Severe respiratory distress (marked retractions, grunting)
- Age < 6 months
- Toxic appearance, altered mental status
- Inability to maintain oral hydration
- Bilateral or multilobar involvement
- Parapneumonic effusion or empyema
Management
Outpatient (Mild CAP)
| Age / Suspected Pathogen | First-Line Treatment |
|---|---|
| < 5 years (viral most likely) | Supportive care; no antibiotics unless bacterial signs |
| Any age, bacterial CAP | Amoxicillin 90 mg/kg/day ÷ 2–3 doses (high-dose) |
| Atypical (Mycoplasma) | Azithromycin 10 mg/kg day 1, then 5 mg/kg days 2–5 |
| Influenza pneumonia | Oseltamivir (start within 48 hours) |
Inpatient (Moderate–Severe CAP)
- Ampicillin IV (if fully immunized, no MRSA risk)
- Ceftriaxone IV (broader coverage; preferred if H. influenzae or resistant S. pneumoniae suspected)
- Add azithromycin if atypical pneumonia suspected (school-age children)
- Vancomycin or clindamycin: add if MRSA pneumonia suspected (preceding influenza, skin infections, cavitation on CXR)
Supportive Care
- Supplemental oxygen to maintain SpO₂ ≥ 95%
- IV fluids if not tolerating oral intake
- Antipyretics/analgesics (paracetamol/ibuprofen)
- Chest physiotherapy: not routinely recommended
- Bronchodilators: only if concurrent wheeze/bronchospasm
Complications
| Complication | Features |
|---|---|
| Parapneumonic effusion / Empyema | Fever persisting > 48–72 hrs on antibiotics; pleural tapping/drainage required |
| Lung abscess | Cavitary lesion; prolonged antibiotics needed |
| Pneumatocele | Usually resolves spontaneously; more common after Staph aureus |
| Respiratory failure | Requires PICU, mechanical ventilation |
| Septicemia | Multi-organ dysfunction; aggressive resuscitation |
Special Populations
- HIV-infected children: Must consider Pneumocystis jirovecii pneumonia (PCP) if not on combination ART, and tuberculosis even if on ART. Lymphoid interstitial pneumonitis (LIP) presents with chronic cough, mild tachypnea, and recurrent bacterial superinfections.
- Neonates: Group B Strep and gram-negatives dominate; IV antibiotics mandatory.
- Immunocompromised: Broaden coverage to include fungal (Aspergillus), viral (CMV), and atypical pathogens.
Differential Diagnosis
- Bronchiolitis (RSV, mainly < 2 years)
- Asthma exacerbation
- Foreign body aspiration
- Pulmonary tuberculosis
- Heart failure with pulmonary edema
- Acute chest syndrome (sickle cell disease)
Prevention
- Pneumococcal vaccines (PCV13/PCV15/PCV20): significantly reduce S. pneumoniae pneumonia burden
- Influenza vaccine: annual, for all children ≥ 6 months
- Hib vaccine: prevents H. influenzae type b pneumonia
- RSV prophylaxis (palivizumab/nirsevimab): for high-risk infants (prematurity, congenital heart disease)
- Breastfeeding, smoke-free environments, good nutrition
Summary: Pneumonia in children is predominantly viral in young children and bacterial/atypical in older children. Tachypnea is the key clinical sign. Treatment is guided by age, severity, and likely pathogen — with high-dose amoxicillin as the cornerstone of outpatient bacterial CAP therapy. Hospitalization is warranted for hypoxia, severe distress, or failure to improve.
National health mission
search_medical_text
National Health Mission India objectives components programs
GradeResponse
search_medical_text
National Rural Health Mission NRHM primary healthcare India
GradeResponse
The medical database has minimal content on health policy/administration. I'll provide a comprehensive answer from established knowledge.
National Health Mission (NHM), India
Overview
The National Health Mission (NHM) is India's flagship public health program, launched by the Government of India in 2013, subsuming the earlier National Rural Health Mission (NRHM) (2005) under its umbrella. It aims to achieve universal access to equitable, affordable, and quality healthcare — particularly for the most vulnerable populations.
Nodal Ministry: Ministry of Health and Family Welfare, Government of India
Funding Pattern: Centre–State ratio of 60:40 (general states), 90:10 (special category / NE states)
Funding Pattern: Centre–State ratio of 60:40 (general states), 90:10 (special category / NE states)
Structure of NHM
NHM has two sub-missions:
| Sub-Mission | Focus Area |
|---|---|
| National Rural Health Mission (NRHM) | Rural populations across all states |
| National Urban Health Mission (NUHM) | Urban poor, slum dwellers (launched 2013) |
Goals / Objectives
- Reduce Maternal Mortality Rate (MMR) to < 100 per 1,00,000 live births
- Reduce Infant Mortality Rate (IMR) to < 25 per 1,000 live births
- Reduce Under-5 Mortality Rate (U5MR) to < 23 per 1,000 live births
- Reduce Total Fertility Rate (TFR) to 2.1
- Prevent and control communicable and non-communicable diseases
- Achieve universal access to public health services
- Improve health infrastructure and human resources
Key Components
1. Health System Strengthening
- Upgradation of Sub-Centres (SC), Primary Health Centres (PHC), Community Health Centres (CHC), and District Hospitals
- Operationalizing 24×7 delivery services at PHCs
- Establishing First Referral Units (FRUs)
2. Human Resources
- Accredited Social Health Activist (ASHA): Village-level female community health worker; acts as a link between the community and the health system. One ASHA per 1,000 population in rural areas.
- Auxiliary Nurse Midwife (ANM): Deployed at sub-centres
- Multi-Purpose Workers (MPW)
- Appointment of contractual staff — specialists, MOs, nurses
3. Reproductive, Maternal, Newborn, Child and Adolescent Health (RMNCH+A)
Key interventions under this integrated strategy:
- Janani Suraksha Yojana (JSY): Cash incentive for institutional deliveries to reduce home births and maternal mortality
- Janani Shishu Suraksha Karyakram (JSSK): Free entitlements — delivery, C-section, transport, medicines, diet for pregnant women and sick newborns
- Pradhan Mantri Surakshit Matritva Abhiyan (PMSMA): Free antenatal checkups on the 9th of every month
- LaQshya: Labour room and maternity OT quality improvement
- Home Based Newborn Care (HBNC): ASHA visits newborns at home; 7 visits in the first 42 days
- Rashtriya Bal Swasthya Karyakram (RBSK): Child health screening and early intervention for 4 Ds — Defects, Deficiencies, Diseases, Developmental delays
- Adolescent health (RKSK): Rashtriya Kishor Swasthya Karyakram — covers nutrition, mental health, ARSH, substance abuse
4. Immunization
- Universal Immunization Programme (UIP) strengthened under NHM
- Introduction of new vaccines: Pentavalent, Rotavirus, Pneumococcal Conjugate Vaccine (PCV), Inactivated Polio Vaccine (IPV), Measles-Rubella (MR)
- Mission Indradhanush: Intensified immunization drive to reach unvaccinated/partially vaccinated children
- U-WIN: Digital immunization tracking platform
5. Disease Control Programs
NHM integrates several National Disease Control Programmes (NDCPs):
| Program | Target Disease |
|---|---|
| RNTCP / NTEP | Tuberculosis |
| NVBDCP | Malaria, Dengue, Filaria, Kala-azar, Japanese Encephalitis |
| NACP | HIV/AIDS |
| NLEP | Leprosy |
| NPCB | Blindness |
| NPCDCS | Non-communicable diseases (cancer, CVD, stroke, diabetes) |
| NMHP | Mental Health |
| NPHCE | Elderly health care |
6. Urban Health (NUHM)
- Urban Primary Health Centres (U-PHC): one per 50,000 urban population
- Urban Community Health Centres (U-CHC)
- Mahila Arogya Samiti (MAS): Urban equivalent of ASHA groups
- Focus on slum dwellers, migrant workers, homeless populations
7. Infrastructure & Quality
- Indian Public Health Standards (IPHS): Defined standards for facilities at every level
- Kayakalp Award: Recognizes public health facilities for cleanliness and infection control
- NQAS (National Quality Assurance Standards): Certification for public health facilities
- Mera Aspataal: Patient satisfaction measurement system
8. Health Information & Technology
- HMIS (Health Management Information System): Web-based data reporting
- MCTS / RCH Portal: Mother and Child Tracking System
- eSanjeevani: National telemedicine platform
- Ayushman Bharat Digital Mission (ABDM): Digital health IDs (ABHA)
Flagship Schemes Under / Linked to NHM
| Scheme | Purpose |
|---|---|
| Ayushman Bharat – PM-JAY | Health insurance cover of ₹5 lakh/family/year for BPL families |
| Ayushman Bharat – HWC | 1.5 lakh Health and Wellness Centres for comprehensive primary care |
| PM Poshan (MDM) | Nutrition for school children |
| Poshan Abhiyaan | Reducing malnutrition |
ASHA — Backbone of NHM
- Over 10 lakh ASHAs deployed across India
- Roles: Mobilize communities for immunization, ANC registration, institutional delivery, DOTS for TB, family planning counseling
- Receive performance-based incentives
- Awarded the WHO Director-General's Global Health Leaders Award (2022)
Achievements / Impact
- Significant decline in MMR: from 254 (2004–06) to 97 (2018–20)
- IMR declined from 58 (2005) to 28 (2020)
- Institutional deliveries rose from ~40% (2005) to >90% (2021)
- Polio eradication (certified 2014)
- Substantial reduction in malaria and leprosy burden
Challenges
- Shortage of specialists and healthcare workers in rural areas
- Uneven implementation across states
- High out-of-pocket expenditure still persists
- Urban–rural healthcare divide
- Weak referral linkages between tiers
- Inadequate infrastructure in tribal/hilly areas
In summary, NHM is the cornerstone of India's public health delivery system, integrating maternal and child health, immunization, disease control, and urban health under one framework, with ASHA workers and community participation as its driving force.
This is a shared conversation. Sign in to Orris to start your own chat.