Quantification of pneumothorax full details
Reading File
search_medical_text
pneumothorax quantification methods size estimation formulas
search_medical_text
pneumothorax light criteria BTS guidelines classification management
search_medical_image
pneumothorax chest X-ray measurement quantification
GradeResponse
GradeResponse
GradeResponse
search_medical_text
pneumothorax size calculation Light index Collins method radiograph interpleural distance
search_medical_text
spontaneous pneumothorax small large classification treatment algorithm chest drain aspiration
Here is a comprehensive overview of pneumothorax quantification covering all major methods, formulas, guidelines, and clinical applications.
Pneumothorax Quantification
Why Quantification Matters
The size of a pneumothorax determines:
- Whether conservative management, aspiration, or chest drain insertion is required
- Monitoring of progression or resolution
- Classification as small vs. large per guidelines (BTS, ACCP)
Imaging Modalities for Quantification
| Modality | Role | Notes |
|---|---|---|
| Chest X-ray (CXR) | First-line; most quantification formulas based on this | PA erect preferred |
| CT Thorax | Most accurate; gold standard for size | Detects occult pneumothoraces; better size estimation |
| Ultrasound | Diagnosis, not quantification | Sensitivity ~89%, specificity ~99%; identifies lung point |
CT scanning exceeds both ultrasound and CXR for detecting small ("occult") pneumothoraces and determining size (Bedside General and Cardiac Ultrasonography, p. 12).
Quantification Methods
1. Light Index (Most Widely Used)
Proposed by Richard Light, this formula estimates the percentage of hemithorax volume occupied by air.
Formula: $$% \text{ Pneumothorax} = \left(1 - \frac{L^3}{H^3}\right) \times 100$$
Where:
- L = diameter of the collapsed lung (cm) — measured at the hilum level on CXR
- H = diameter of the hemithorax (cm) — measured at the same level
Basis: Lung and hemithorax are modeled as spheres. A pneumothorax >20% is considered large by ACCP criteria.
2. Collins Method (Average Interpleural Distance)
Measures the average interpleural distance at three points on CXR:
- Apex of lung to cupola of pleura
- Upper zone (mid-lung level)
- Lower zone (base)
Formula: $$\text{Size (%)} = 4.2 + [4.7 \times (A + B + C)]$$
Where A, B, C = interpleural distances (cm) at apex, mid, and base.
Threshold: >2 cm = large pneumothorax (BTS definition at the hilum level).
3. Rhea Index
Measures average of multiple interpleural distances (intrapleural distances between parietal and visceral pleura at defined levels) annotated on CXR. As shown in the image below, measurements are taken at multiple points bilaterally:
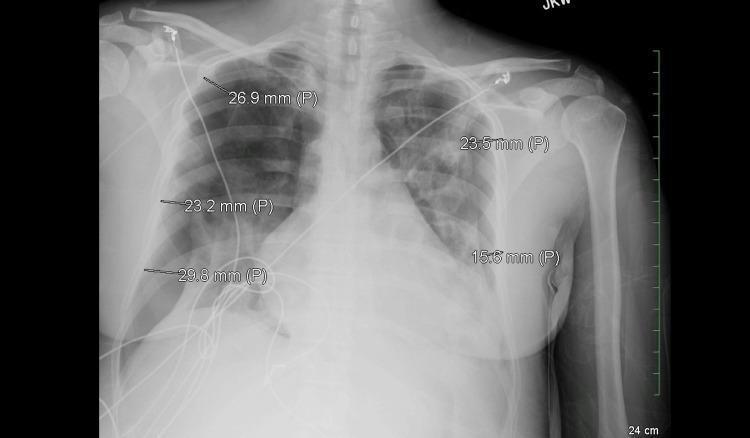
Formula: $$% \text{ Pneumothorax} = \frac{(D_1 + D_2 + D_3)}{3} \times K$$
Where D₁, D₂, D₃ are interpleural distances (mm/cm) at specified levels; K is a correction factor derived from the original validation study.
4. BTS Method (Interpleural Distance at Hilum)
The British Thoracic Society (2010) uses a single, simplified measurement:
Measure the interpleural distance at the level of the hilum on a PA CXR.
| Measurement | Classification |
|---|---|
| < 2 cm | Small pneumothorax |
| ≥ 2 cm | Large pneumothorax |
This single measurement correlates to approximately 50% of the hemithorax volume being occupied by air, because of the cubic relationship between radius and volume.
5. Deep Sulcus Sign (Supine CXR)
In ICU/supine patients, air collects anteriorly and basally, producing the deep sulcus sign:
- Hyperlucency in the costophrenic angle
- Deepening of the lateral sulcus
- Quantification is unreliable on supine films; CT is preferred
Comparison of Quantification Methods
| Method | Formula Used | CXR Measurements | Threshold: Large |
|---|---|---|---|
| Light Index | 1 − (L³/H³) × 100 | Lung & hemithorax diameter | >20% (ACCP) |
| Collins | 4.2 + 4.7×(A+B+C) | 3 interpleural distances | >2 cm (BTS) |
| Rhea Index | Mean of distances × K | 3 interpleural distances | Variable |
| BTS (Hilum) | Single distance | 1 measurement at hilum | ≥2 cm |
| CT volumetric | Direct 3D segmentation | CT slices | Most accurate |
Clinical Classification by Size
ACCP (American College of Chest Physicians) Classification:
- Small: <20% of hemithorax volume (Light Index)
- Large: ≥20% of hemithorax volume
BTS (British Thoracic Society 2010) Classification:
- Small: Interpleural rim <2 cm at hilum
- Large: Interpleural rim ≥2 cm at hilum
⚠️ The BTS and ACCP use different measurement thresholds for "large," which can create confusion. BTS 2 cm ≈ ACCP 50% by volume (not 20%), making the ACCP threshold more liberal for intervention.
Management Decisions Based on Size
| Scenario | Small (<2 cm / <20%) | Large (≥2 cm / ≥20%) |
|---|---|---|
| Primary spontaneous (PSP) | Discharge + outpatient follow-up | Aspiration or chest drain |
| Secondary spontaneous (SSP) | Admit + oxygen ± aspiration | Chest drain insertion |
| Traumatic | Observe if stable | Chest drain |
| Tension | Immediate needle decompression regardless of size | Chest drain after decompression |
BTS 2010 guidelines for spontaneous pneumothorax management are summarized in a decision algorithm (Bailey and Love's Short Practice of Surgery, 28th Ed., p. 1001).
CT-Based Quantification
CT is the most precise modality:
- Manual volumetry: Trace pleural outline on each slice, calculate volume
- Semi-automated segmentation: Software-assisted; used in research/surgical planning
- Percentage formula from CT: $$% = \left(1 - \frac{V_{lung}}{V_{hemithorax}}\right) \times 100$$
CT is mandatory when:
- CXR is equivocal
- Patient is supine/ICU
- Occult or loculated pneumothorax suspected
- Pre-surgical planning (e.g., VATS bullectomy)
Ultrasound-Based Assessment
Ultrasound cannot reliably quantify pneumothorax size, but it:
- Identifies the lung point (pathognomonic of pneumothorax, 100% specific)
- Rules out pneumothorax via comet tail artifacts (B-lines)
- Has pooled sensitivity 89%, specificity 99% vs. ~30–75% for CXR in ICU/ED patients (Bedside Ultrasonography, p. 12)
The lung point location can be used as a rough proxy for size: a more lateral lung point indicates a larger pneumothorax.
Summary: Key Formulas at a Glance
| Formula | Equation |
|---|---|
| Light Index | % = [1 − (L/H)³] × 100 |
| Collins | % = 4.2 + 4.7(A + B + C) |
| BTS threshold | ≥2 cm at hilum = large |
| CT volumetric | % = [1 − (V_lung / V_hemithorax)] × 100 |
Clinical Pearl: The Light Index and Collins method are validated for PA CXR in spontaneous pneumothorax. CT volumetry is the reference standard. In practice, the BTS single-measurement rule (2 cm at hilum) is the most widely applied bedside tool due to its simplicity and reproducibility.
This is a shared conversation. Sign in to Orris to start your own chat.