Explain me antianginal drugs with its mechanism of action and side effects with diagrams
Reading File
Finding Sources
Finding Sources
Searching Images
antianginal drugs mechanism of action diagram
Reading File
Finding Sources
Finding Sources
Searching Images
nitrate mechanism angina vasodilation smooth muscle
Reading File
Reading File
Searching Images
calcium channel blocker mechanism cardiac angina
Reading File
Searching Images
beta blocker mechanism of action heart rate angina
Generating Image
Generating Image
Generating Image
Here is a comprehensive guide to antianginal drugs — their mechanisms of action and side effects.
Antianginal Drugs
Pathophysiology Overview
Angina pectoris results from an imbalance between myocardial oxygen demand and supply. Antianginal drugs work by either:
- Reducing demand (↓ heart rate, contractility, wall tension)
- Increasing supply (coronary/peripheral vasodilation)
Overall Mechanism Summary
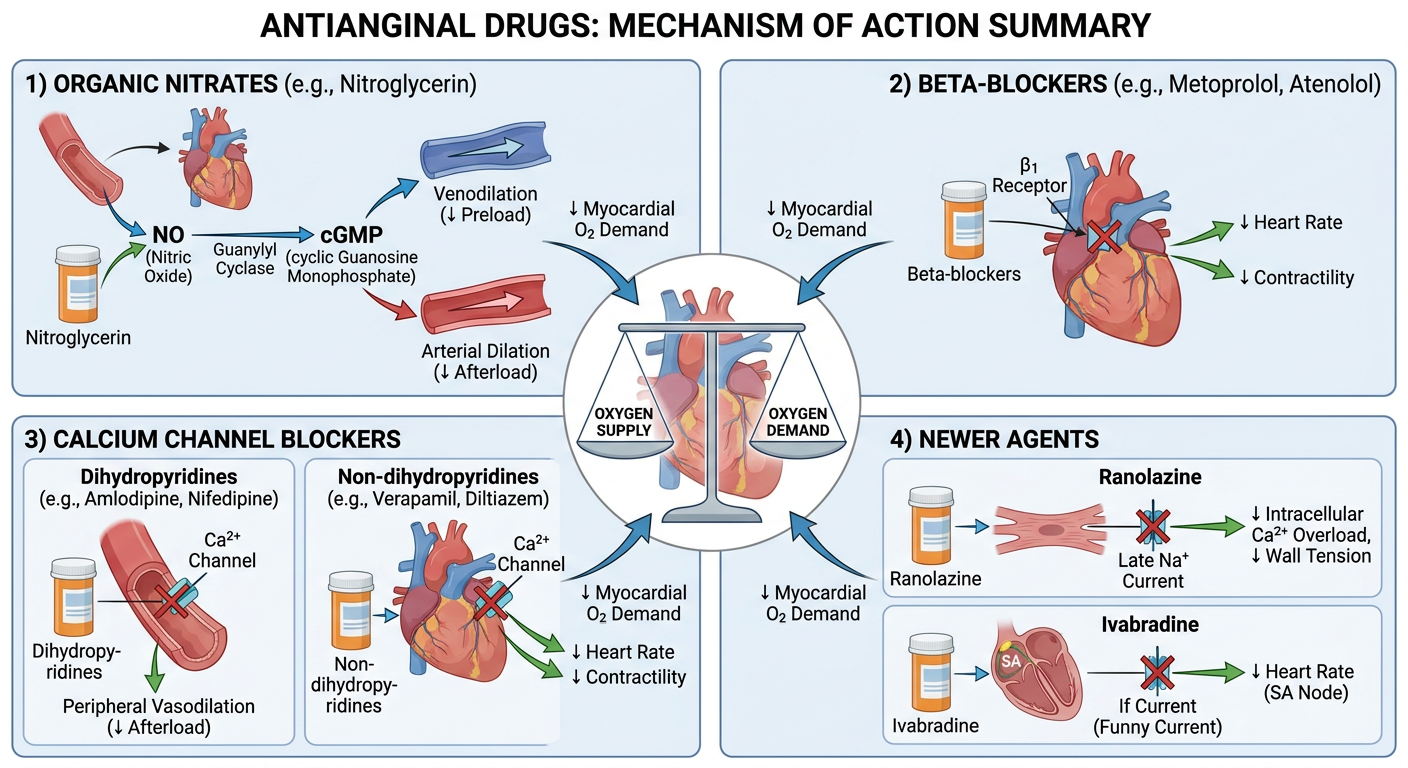
1. Organic Nitrates
Drugs: Nitroglycerin (GTN), Isosorbide dinitrate (ISDN), Isosorbide mononitrate (ISMN), Amyl nitrite
Mechanism of Action
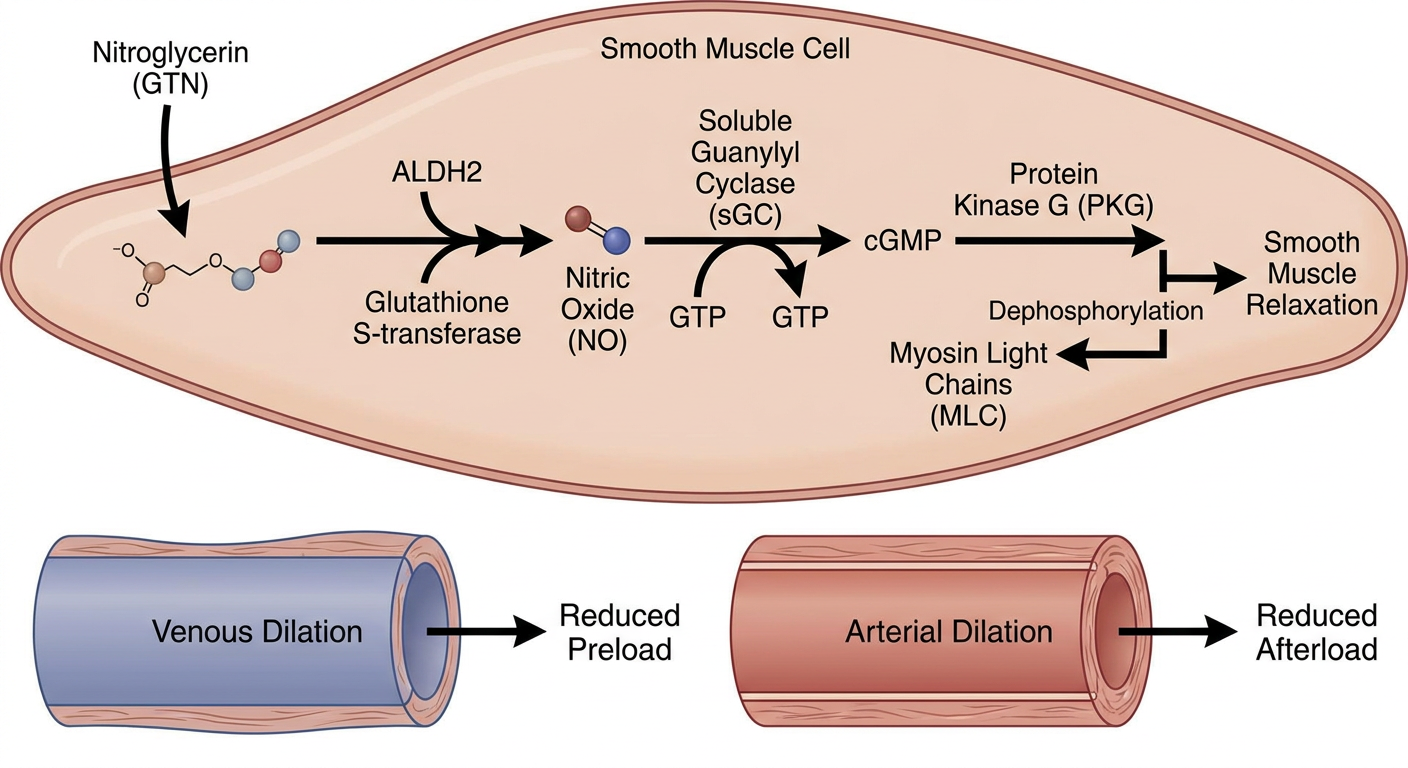
Nitroglycerin must be bioactivated enzymatically:
- ALDH2 (mitochondrial aldehyde dehydrogenase isoform 2) and glutathione S-transferase denitrate nitroglycerin → releases nitric oxide (NO)
- NO combines with the heme group of soluble guanylyl cyclase (sGC) → activates it
- sGC converts GTP → cGMP (cyclic GMP)
- cGMP activates protein kinase G (PKG)
- PKG dephosphorylates myosin light chains → smooth muscle relaxation → vasodilation
Net hemodynamic effects:
| Effect | Result |
|---|---|
| Venodilation (dominant) | ↓ Venous return → ↓ Preload → ↓ Wall tension → ↓ O₂ demand |
| Arterial dilation | ↓ Afterload → ↓ Cardiac work |
| Coronary redistribution | Improves flow to ischemic subendocardium |
| Weak negative inotropy | via NO |
Pharmacokinetics:
- Oral bioavailability is low (<10–20%) due to extensive hepatic first-pass metabolism
- Sublingual route preferred for rapid effect (onset 1–3 min, duration 15–30 min)
- Isosorbide mononitrate has 100% bioavailability (oral)
Side Effects
| Side Effect | Mechanism |
|---|---|
| Headache (most common) | Cerebral vasodilation |
| Flushing | Cutaneous vasodilation |
| Hypotension / syncope | Excessive vasodilation |
| Reflex tachycardia | Baroreceptor response to hypotension |
| Tolerance | Depletion of sulfhydryl groups needed for ALDH2; requires nitrate-free interval (8–12 h/day) |
| Severe hypotension with PDE-5 inhibitors | Both increase cGMP — dangerous combination; wait ≥6 h between use |
| Methemoglobinemia (with large doses) | Rare |
2. Beta-Adrenoceptor Blockers (β-Blockers)
Drugs: Metoprolol, Atenolol (cardioselective β₁); Propranolol (non-selective β₁/β₂)
Mechanism of Action
By blocking β₁-adrenoceptors on the heart:
- ↓ Heart rate (negative chronotropy)
- ↓ Contractility (negative inotropy)
- ↓ AV conduction velocity
→ All three reduce myocardial oxygen demand, especially during exertion (the main trigger for effort angina)
Hemodynamic effects:
- ↓ Heart rate × ↓ Systolic pressure = reduced rate-pressure product (key determinant of O₂ demand)
- Prolonged diastolic filling time → improved coronary perfusion
- Not vasodilators; do not benefit vasospastic/Prinzmetal angina (may worsen it by allowing unopposed α-vasoconstriction)
Side Effects
| Side Effect | Notes |
|---|---|
| Bradycardia / heart block | Especially non-selective agents |
| Bronchospasm | β₂ blockade — contraindicated in asthma |
| Fatigue, lethargy | CNS effects |
| Cold extremities | ↓ peripheral perfusion |
| Impotence | Peripheral vascular effect |
| Masking of hypoglycemia | Blocks tachycardia warning sign in diabetics |
| Rebound angina | On abrupt withdrawal — must taper |
| Negative inotropy | Worsens decompensated heart failure |
3. Calcium Channel Blockers (CCBs)
Drugs:
- Dihydropyridines (DHPs): Amlodipine, Nifedipine, Felodipine
- Non-dihydropyridines (Non-DHPs): Verapamil (phenylalkylamine), Diltiazem (benzothiazepine)
Mechanism of Action
Block voltage-gated L-type calcium channels (Ca²⁺ channels):
| Drug Class | Primary Target | Effect |
|---|---|---|
| Dihydropyridines | Vascular smooth muscle >> heart | Peripheral arterial vasodilation → ↓ afterload |
| Verapamil | Heart > vessels | ↓ HR, ↓ contractility, ↓ AV conduction; less vasodilation |
| Diltiazem | Heart and vessels equally | Intermediate effects |
How it helps angina:
- DHPs: ↓ afterload → ↓ O₂ demand; first-line for vasospastic (Prinzmetal) angina
- Non-DHPs: ↓ HR + contractility → ↓ O₂ demand (similar to β-blockers)
- All: coronary vasodilation → ↑ O₂ supply
Side Effects
Dihydropyridines:
| Side Effect | Cause |
|---|---|
| Peripheral edema | Vasodilation causing precapillary dilation > postcapillary |
| Flushing, headache | Vasodilation |
| Reflex tachycardia | With short-acting nifedipine (less with amlodipine) |
| Gingival hyperplasia | (especially nifedipine) |
Non-dihydropyridines (Verapamil/Diltiazem):
| Side Effect | Cause |
|---|---|
| Bradycardia / AV block | Direct cardiac effect |
| Constipation | (especially verapamil — smooth muscle relaxation in GI) |
| Negative inotropy | May worsen systolic heart failure |
| Contraindicated with β-blockers | Risk of complete heart block |
Side Effects Comparison
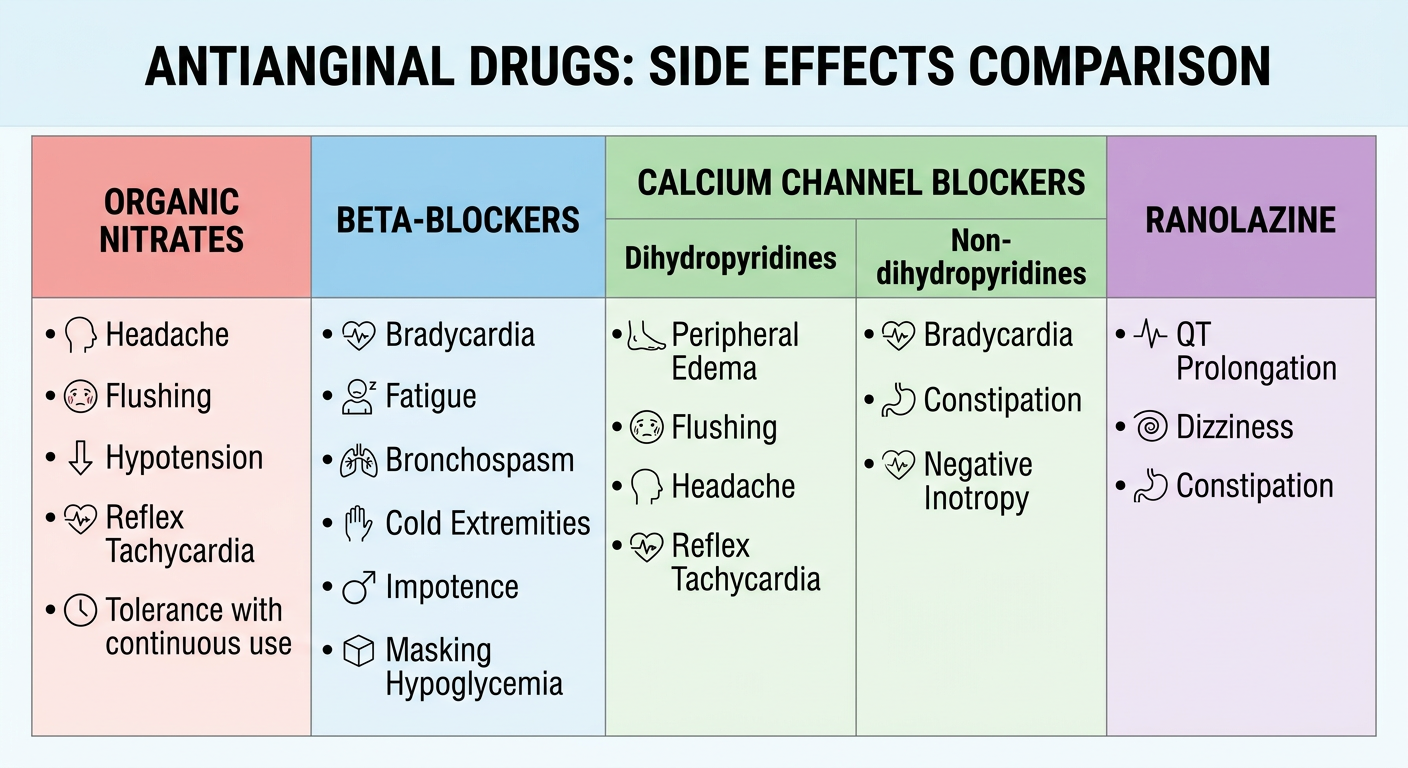
4. Newer / Second-Line Antianginal Agents
Ranolazine
- Mechanism: Inhibits the late sodium current (late I_Na) → ↓ intracellular Na⁺ → ↓ Na⁺/Ca²⁺ exchanger activity → ↓ intracellular Ca²⁺ → reduces diastolic tension and cardiac work
- Does not affect heart rate or blood pressure significantly
- Side effects: QT prolongation (though no torsades reported), dizziness, constipation, nausea; may inhibit metabolism of digoxin and simvastatin
Ivabradine
- Mechanism: Selectively blocks the hyperpolarization-activated I_f ("funny") current in the SA node → ↓ heart rate only
- No negative inotropic or vasodilator effects
- Similar efficacy to CCBs and β-blockers for angina
- Side effects: Visual disturbances (phosphenes — flickering lights), bradycardia
Nicorandil
- Mechanism: Dual — K⁺ channel activator (hyperpolarizes smooth muscle) + nitrate-like NO donor → vasodilation of coronary and peripheral vessels
- Side effects: Headache (like nitrates), hypotension, oral/GI ulceration
Trimetazidine (metabolic agent)
- Mechanism: Partially inhibits fatty acid oxidation (inhibits LC-3KAT enzyme) → myocardium shifts to glucose oxidation which consumes less oxygen per ATP → metabolic efficiency in ischemia
- Not approved in the USA; available in Europe and Asia
- Side effects: Parkinsonism-like symptoms, GI effects
Summary Table
| Drug Class | Key Mechanism | Reduces | Angina Type | Key Side Effect |
|---|---|---|---|---|
| Organic Nitrates | NO → cGMP → vasodilation | Preload (primarily) | Effort + Vasospastic | Headache, tolerance |
| β-Blockers | ↓ HR, contractility | O₂ demand | Effort only | Bronchospasm, bradycardia |
| DHP CCBs | Block L-Ca²⁺ in vessels | Afterload | Effort + Vasospastic | Edema, flushing |
| Non-DHP CCBs | Block L-Ca²⁺ in heart | HR + contractility | Effort + Vasospastic | AV block, constipation |
| Ranolazine | Block late I_Na | Diastolic tension | Effort (add-on) | QT prolongation |
| Ivabradine | Block I_f in SA node | HR only | Effort (add-on) | Visual phosphenes |
| Nicorandil | K⁺ activation + NO | Pre/afterload | Effort + Vasospastic | Headache, ulcers |
Key Clinical Point: β-blockers and short-acting dihydropyridine CCBs should not be combined (risk of severe bradycardia). However, β-blockers + long-acting DHPs (amlodipine) is a safe and effective combination. Never combine nitrates + PDE-5 inhibitors (sildenafil, tadalafil) due to severe hypotension risk.
Source: Katzung's Basic and Clinical Pharmacology, 16th Edition, Chapter 12: Vasodilators & the Treatment of Angina Pectoris
Can you generate flashcards for it
Asking for Preferences
Reading File
Running Command
Running Command
Writing File
Running Command
Running Command
Your credits are exhausted. Your daily credits reset tomorrow, or you can purchase a top-up for more.
This is a shared conversation. Sign in to Orris to start your own chat.