Pneumothorax definition classification etiology pathogenesis pathophysiology clinical features diagnosis and management full details for md exams and complications with drugs doses
Reading File
search_medical_text
pneumothorax definition classification etiology types primary secondary spontaneous tension
search_medical_text
pneumothorax pathophysiology pathogenesis clinical features diagnosis chest X-ray CT findings
search_medical_image
pneumothorax chest X-ray tension pneumothorax imaging findings
GradeResponse
GradeResponse
GradeResponse
search_medical_text
pneumothorax management treatment chest tube needle decompression pleurodesis surgery drugs doses
Here is a comprehensive, exam-ready breakdown of Pneumothorax for MD-level preparation.
PNEUMOTHORAX — Complete MD Exam Guide
1. DEFINITION
Pneumothorax is the presence of air (gas) in the pleural space, resulting in partial or complete collapse of the lung.
(Harrison's Principles of Internal Medicine, 21st Ed., p. 8095)
2. CLASSIFICATION
A. Based on Etiology
| Type | Description |
|---|---|
| Primary Spontaneous Pneumothorax (PSP) | No underlying lung disease; typically tall, young males |
| Secondary Spontaneous Pneumothorax (SSP) | Complicates pre-existing lung disease (COPD, TB, etc.) |
| Traumatic Pneumothorax | Due to penetrating or blunt chest trauma; includes iatrogenic |
| Tension Pneumothorax | Pleural pressure is positive throughout the respiratory cycle — a life-threatening emergency |
B. Based on Size
| Size | BTS Definition | ACCP Definition |
|---|---|---|
| Small | Rim of air < 2 cm on CXR | Apex-to-cupola distance < 3 cm |
| Large | Rim of air ≥ 2 cm | Apex-to-cupola distance ≥ 3 cm |
C. Other Subtypes
- Iatrogenic: Complication of procedures (CVP line insertion, thoracentesis, mechanical ventilation, lung biopsy)
- Catamenial: Rare; occurs in women during menstruation (endometriosis of pleura/diaphragm)
- Neonatal: Associated with meconium aspiration, RDS
3. ETIOLOGY
Primary Spontaneous Pneumothorax (PSP)
- Rupture of subpleural blebs/bullae (apical, small air-filled cysts)
- Tall, thin males aged 20–40 years
- Smoking is the strongest risk factor (increases risk ~20x in heavy smokers)
- Connective tissue disorders: Marfan syndrome, Ehlers-Danlos syndrome
- High altitude, rapid changes in atmospheric pressure (diving, flying)
Secondary Spontaneous Pneumothorax (SSP)
| Disease | Mechanism |
|---|---|
| COPD / Emphysema | Most common cause; bullae rupture |
| Tuberculosis | Subpleural caseous nodule rupture |
| Pneumocystis jirovecii pneumonia (PCP) | Cystic lung changes in HIV |
| Cystic Fibrosis | Emphysematous bullae |
| Asthma | Air trapping, alveolar over-distension |
| Lung cancer | Tumor necrosis, pleural invasion |
| Interstitial Lung Disease (LAM, LCH) | Cystic changes |
| Necrotizing pneumonia / Lung abscess | Bronchopleural fistula |
| Marfan/Ehlers-Danlos | Connective tissue weakness |
Traumatic / Iatrogenic
- Penetrating trauma: stab wound, gunshot
- Blunt trauma: rib fracture lacerating lung parenchyma
- Iatrogenic: central line (subclavian > internal jugular), thoracentesis, mechanical ventilation (barotrauma), bronchoscopy with biopsy, transthoracic needle biopsy
4. PATHOGENESIS
PSP
- Subpleural bleb formation: Weak areas at lung apex develop blebs from ischemia, inflammatory changes in airways, and increased mechanical stress from the pressure gradient (highest at apex due to lung weight)
- Smoking: increases small airways inflammation → air trapping → bleb formation
- Blebs rupture → air enters pleural space
SSP
- Underlying disease creates bullae, cysts, or necrotic tissue that ruptures
- Bronchopleural fistula → continued air leakage
Tension Pneumothorax (One-way valve mechanism)
- A defect in visceral/parietal pleura acts as a one-way (ball-valve) mechanism
- Air enters the pleural space on inspiration but cannot escape on expiration
- Progressive accumulation of air → positive intrapleural pressure throughout respiratory cycle
- Leads to: lung collapse → mediastinal shift → contralateral lung compression → kinking of great vessels (SVC, IVC) → decreased venous return → reduced cardiac output → obstructive shock and death if untreated
5. PATHOPHYSIOLOGY
Air enters pleural space
↓
Lung collapses (↓ lung compliance)
↓
↓ Ventilation-Perfusion (V/Q) mismatch
↓
Intrapulmonary shunting → Hypoxemia
↓
Compensatory tachypnea, tachycardia
↓ (if tension)
Mediastinal shift → Compression of contralateral lung
↓
Kinking of SVC/IVC → ↓↓ Venous return
↓
↓ Cardiac output → Obstructive shock → Cardiorespiratory arrest
Key physiological changes:
- Intrapleural pressure shifts from negative (−5 cmH₂O) to positive (in tension)
- Lung compliance decreases
- FRC (Functional Residual Capacity) decreases
- Hypoxemia due to right-to-left shunt
- Hypercapnia in severe cases
6. CLINICAL FEATURES
Symptoms
| Symptom | PSP | Tension PTX |
|---|---|---|
| Chest pain | Sudden, pleuritic, ipsilateral | Severe |
| Dyspnea | Mild to moderate | Severe, rapidly worsening |
| Onset | At rest or light activity | Sudden, often in ventilated patients |
| Cough | Occasional | Present |
| Shock symptoms | Absent | Present (hypotension, altered sensorium) |
Signs
| Sign | Description |
|---|---|
| Tachycardia | Most common sign |
| Tachypnea | Rapid shallow breathing |
| Reduced chest expansion | On affected side |
| Tracheal deviation | Away from affected side (TENSION — late sign) |
| Hyperresonance to percussion | Affected side |
| Absent/decreased breath sounds | Affected side |
| Hypotension | Tension pneumothorax |
| JVP elevation | Tension (impaired venous return) |
| Cyanosis | Late sign, severe hypoxia |
| Subcutaneous emphysema | Air tracking into soft tissues |
| Pulsus paradoxus | May be present |
Classic triad of Tension PTX: Hypotension + Absent breath sounds (ipsilateral) + Tracheal deviation (contralateral) — also called Beck's triad equivalent for tension PTX
7. DIAGNOSIS
A. Chest X-ray (CXR) — First-line Investigation
- Visceral pleural line visible as a white line with absence of lung markings beyond it
- Lung collapse toward hilum
- Tension PTX: tracheal/mediastinal shift contralaterally, depression/inversion of ipsilateral hemidiaphragm
- Erect PA CXR is standard; expiratory films may enhance visualization
- Supine CXR (ICU): deep sulcus sign (hyperlucency of costophrenic angle)
B. CT Thorax — Gold Standard
- Most sensitive and specific
- Identifies underlying bullae, blebs, underlying lung disease
- Differentiates pneumothorax from large bullae
- Quantifies size accurately
- Guides management decisions (surgery)
C. Ultrasound (POCUS) — Bedside/ICU
- Absence of lung sliding (M-mode: "barcode/stratosphere sign" instead of "seashore sign")
- Absence of B-lines (comet-tail artifacts)
- Lung point sign: pathognomonic — transition point between normal and absent lung sliding
- Sensitivity: 100%, Specificity: 100% for lung point sign (GLGCA textbook on bedside ultrasonography, p. 12)
Ultrasound accuracy exceeds that of plain chest radiography in ICU settings
D. Other Investigations
| Investigation | Finding |
|---|---|
| ABG | Hypoxemia (↓PaO₂), possible hypocapnia (early), hypercapnia (late/severe) |
| ECG | Sinus tachycardia; in tension: right heart strain pattern |
| SpO₂ | Decreased |
Diagnostic Algorithm
Suspected Pneumothorax
↓
Hemodynamically UNSTABLE?
YES → Clinical diagnosis of TENSION PTX → Immediate needle decompression
NO ↓
CXR (erect PA)
↓
Confirmed PTX
↓
Primary or Secondary? Small or Large? Symptomatic?
↓
Management as below
8. MANAGEMENT
TENSION PNEUMOTHORAX — Medical Emergency
Do NOT wait for CXR — treat on clinical diagnosis
Step 1: Immediate Needle Decompression (Thoracocentesis)
- Site: 2nd intercostal space (ICS), midclavicular line (MCL) — OR — 4th/5th ICS, anterior axillary line
- Needle: 14–16 G IV cannula
- Converts tension to simple pneumothorax
- Hissing sound of escaping air confirms diagnosis
Step 2: Chest Tube (Intercostal Drain — ICD)
- Site: 4th–5th ICS, anterior or midaxillary line (safe triangle)
- Tube size: 28–32 Fr (large bore)
- Connected to underwater seal drain
- Definitive treatment
Step 3: Supportive
- High-flow O₂ (100% via non-rebreather mask) — accelerates reabsorption of pleural air
- IV access, fluid resuscitation for shock
- Monitoring
PRIMARY SPONTANEOUS PNEUMOTHORAX (PSP)
BTS (British Thoracic Society) Guidelines 2023
| Scenario | Management |
|---|---|
| Small (<2 cm) + Minimal symptoms | Conservative: observation, discharge with 2–4 week follow-up, avoid air travel/diving |
| Large (≥2 cm) OR symptomatic | Aspiration first (simple aspiration via 16–18G cannula at 2nd ICS MCL) |
| Aspiration failed / recurrent | Intercostal chest drain (ICD) + Heimlich valve / underwater seal |
| Persistent air leak >3–5 days | Surgical referral: Video-Assisted Thoracoscopic Surgery (VATS) |
Simple Aspiration Technique:
- 16–18G cannula at 2nd ICS MCL
- Aspirate up to 2.5 L of air
- If < 2.5 L aspirated and lung re-expands → successful → observe 4 hours → discharge
- If > 2.5 L required → ICD
SECONDARY SPONTANEOUS PNEUMOTHORAX (SSP)
SSP is more dangerous — always admit; conservative management not appropriate
| Scenario | Management |
|---|---|
| Small (<1 cm) + minimally symptomatic | Admit, high-flow O₂, observe 24 hours |
| >1 cm OR symptomatic | ICD insertion (28–32 Fr) |
| Persistent air leak | VATS or open thoracotomy |
| Treat underlying disease | COPD, TB, etc. |
INTERCOSTAL DRAIN (ICD) — Key Details
| Parameter | Detail |
|---|---|
| Site | 4th–5th ICS, anterior/midaxillary line (safe triangle: bordered by pectoralis major, latissimus dorsi, and 5th ICS) |
| Tube size | 28–32 Fr (large), 12–16 Fr small bore for simple PSP |
| Drain | Underwater seal drain; apply suction (−20 cmH₂O) if not expanding |
| Removal | After 24 h with no bubbling and CXR shows full expansion |
RECURRENCE PREVENTION — PLEURODESIS
| Method | Detail |
|---|---|
| Chemical pleurodesis | Talc slurry or poudrage (most effective), doxycycline, bleomycin via ICD |
| Surgical (VATS) | Bullectomy + mechanical pleurodesis / pleural abrasion / pleurectomy — gold standard for recurrence prevention |
Indications for surgery (VATS/Thoracotomy):
- 2nd ipsilateral pneumothorax (recurrence)
- 1st contralateral pneumothorax
- Bilateral simultaneous pneumothorax
- Persistent air leak > 5–7 days
- Incomplete lung expansion
- Tension pneumothorax
- Occupational risk (pilots, divers)
- Hemopneumothorax
DRUG DOSES (Exam-Critical)
| Drug | Indication | Dose | Route |
|---|---|---|---|
| 100% Oxygen | All pneumothorax; accelerates reabsorption 4x | 10–15 L/min via NRB mask | Inhalation |
| Morphine sulfate | Pain relief | 2–4 mg IV every 4–6 h (titrate to pain) | IV |
| Paracetamol | Analgesia | 1 g every 6–8 h | IV/Oral |
| Ibuprofen / NSAIDs | Mild analgesia | 400 mg TDS with food (avoid in SSP/renal issues) | Oral |
| Talc slurry | Chemical pleurodesis | 5 g in 50–100 mL NS via ICD | Intrapleural |
| Doxycycline | Chemical pleurodesis (alternative) | 500 mg in 50 mL NS via ICD | Intrapleural |
| Bleomycin | Chemical pleurodesis | 60 units in 100 mL NS via ICD | Intrapleural |
| Lidocaine (Lignocaine) | Pre-pleurodesis analgesia | 250 mg in 50 mL NS intrapleural before sclerosant | Intrapleural |
| Atropine | Pre-medication (vagal response during ICD) | 0.6 mg IV | IV |
| Diazepam/Midazolam | Sedation for procedure | 2–5 mg IV (titrate) | IV |
9. COMPLICATIONS
| Complication | Details |
|---|---|
| Tension pneumothorax | Life-threatening; obstructive shock; if untreated → cardiac arrest |
| Hemopneumothorax | Blood + air in pleural space; from torn vessels, needs large bore ICD |
| Hydropneumothorax | Fluid + air in pleural space |
| Pyopneumothorax | Pus + air; from infection; treat with ICD + antibiotics |
| Chronic/Persistent pneumothorax | Air leak > 5 days; bronchopleural fistula; surgical intervention needed |
| Re-expansion pulmonary edema | Rapid re-expansion of collapsed lung; unilateral PE; occurs when pneumothorax present >3 days; avoid rapid drainage |
| Recurrence | PSP: 30–50% recurrence rate; SSP: even higher |
| Respiratory failure | Especially SSP with poor respiratory reserve |
| Cardiovascular collapse | Tension pneumothorax with obstructive shock |
| Subcutaneous emphysema | Air tracking into soft tissues; can be extensive |
| Bronchopleural fistula | Persistent air leak; communication between bronchial tree and pleura |
| Empyema | Infection of pleural space post-ICD (iatrogenic complication) |
10. SPECIAL SCENARIOS
Pneumothorax in Mechanically Ventilated Patients
- Highest risk for tension pneumothorax (positive pressure ventilation forces air in)
- Diagnosis: ↓ SpO₂, ↑ peak airway pressure, hemodynamic deterioration
- Use ultrasound (POCUS) — most rapid diagnosis
- Immediate ICD (not aspiration)
Pneumothorax in Pregnancy
- Rare; managed with ICD to protect fetus from hypoxia
- VATS can be performed in 2nd trimester
Bilateral Pneumothorax
- Rare; simultaneous ICD bilaterally
- Surgical intervention required
11. IMAGING
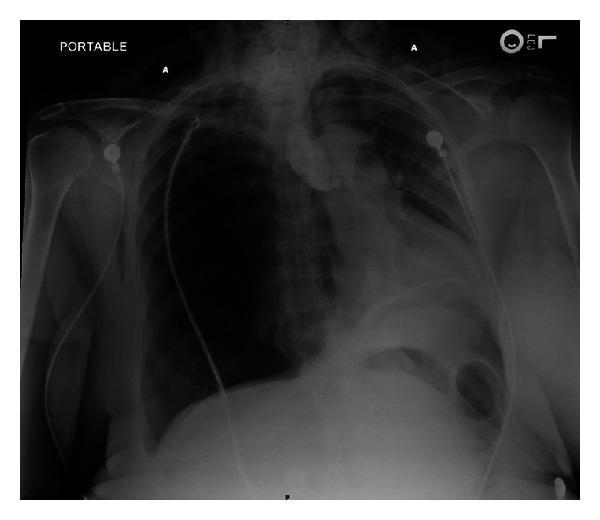
CXR showing tension pneumothorax: Right hemithorax complete radiolucency with absent lung markings, marked contralateral mediastinal shift (heart and trachea deviated to left), depression of right hemidiaphragm, and subcutaneous emphysema in soft tissues — classic findings of obstructive shock physiology requiring emergency needle decompression.
12. HIGH-YIELD EXAM MNEMONICS
| Mnemonic | Content |
|---|---|
| HATT | Hyperresonance, Absent breath sounds, Tracheal deviation, Tachycardia (signs of tension PTX) |
| Indications for VATS | 2nd ipsilateral, 1st contralateral, bilateral, persistent air leak, occupational risk |
| Safe triangle | Anterior: pectoralis major; Posterior: latissimus dorsi; Inferior: 5th ICS |
| First step in tension PTX | Needle at 2nd ICS MCL — do NOT wait for CXR |
13. SUMMARY TABLE
| Feature | PSP | SSP | Tension |
|---|---|---|---|
| Patient | Young, tall, thin male, smoker | Older, underlying lung disease | Any (esp. ventilated) |
| Symptoms | Mild dyspnea, pleuritic pain | Severe dyspnea | Severe + hemodynamic collapse |
| CXR | Visceral pleural line | Visceral pleural line + underlying disease | Mediastinal shift, diaphragm depression |
| Management | Observation/aspiration/ICD | ICD + treat underlying disease | Emergency needle decompression → ICD |
| Recurrence | 30–50% | Higher | N/A |
| First-line | Aspiration (if large/symptomatic) | ICD | Needle decompression immediately |
References:
- Harrison's Principles of Internal Medicine, 21st Edition, p. 8095
- BTS Guideline for Pleural Disease 2023
- Bedside General and Cardiac Ultrasonography in Critically Ill Patients (GLGCA, p. 12)
- ACCP (American College of Chest Physicians) Consensus Guidelines
This is a shared conversation. Sign in to Orris to start your own chat.