Epedimo- orchitis..explain me everything including treatment
Reading File
Finding Sources
Searching PubMed
"epididymo-orchitis" AND treatment
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Reading File
I now have comprehensive information from multiple authoritative textbooks. Let me compile the complete answer:
Epididymo-Orchitis — Complete Guide
Definition
Epididymitis = inflammation of the epididymis lasting < 6 weeks (acute).
Orchitis = inflammation of the testis.
Epididymo-orchitis = combined inflammation of both — the most common clinical presentation when bacterial infection spreads from the epididymis to the adjacent testis.
Anatomy Recap
The epididymis sits posterolaterally on the testis. Infection typically ascends from the lower urinary tract via the vas deferens or spermatic cord lymphatics, reaching the epididymis first, then the testis.
Etiology (Age-Based)
| Age Group | Common Organisms |
|---|---|
| Children (prepubertal) | Gram-negative rods (E. coli), often with congenital GU anomaly; also post-infectious (Mycoplasma pneumoniae, enteroviruses, adenoviruses) |
| Sexually active males < 35 yrs | Neisseria gonorrhoeae, Chlamydia trachomatis (>50% of cases) |
| Older males (> 35 yrs) | E. coli, Pseudomonas, Proteus spp. (urinary pathogens) |
| MSM (insertive anal sex) | E. coli and other coliform bacteria |
| Immunocompromised | Mycobacterium tuberculosis, cryptococcosis, toxoplasmosis, candidiasis |
Other/rare causes:
- Viral orchitis — especially mumps (occurs in 20–30% of postpubertal males with mumps); also Coxsackievirus, EBV, varicella, echovirus
- Chemical/reflux-induced (amiodarone, urine reflux into ejaculatory ducts)
- Systemic: Behçet syndrome, Henoch-Schönlein purpura, sarcoidosis
Mumps orchitis is unilateral in 70% of cases; contralateral involvement in 1–9 days. Bilateral involvement → risk of infertility.
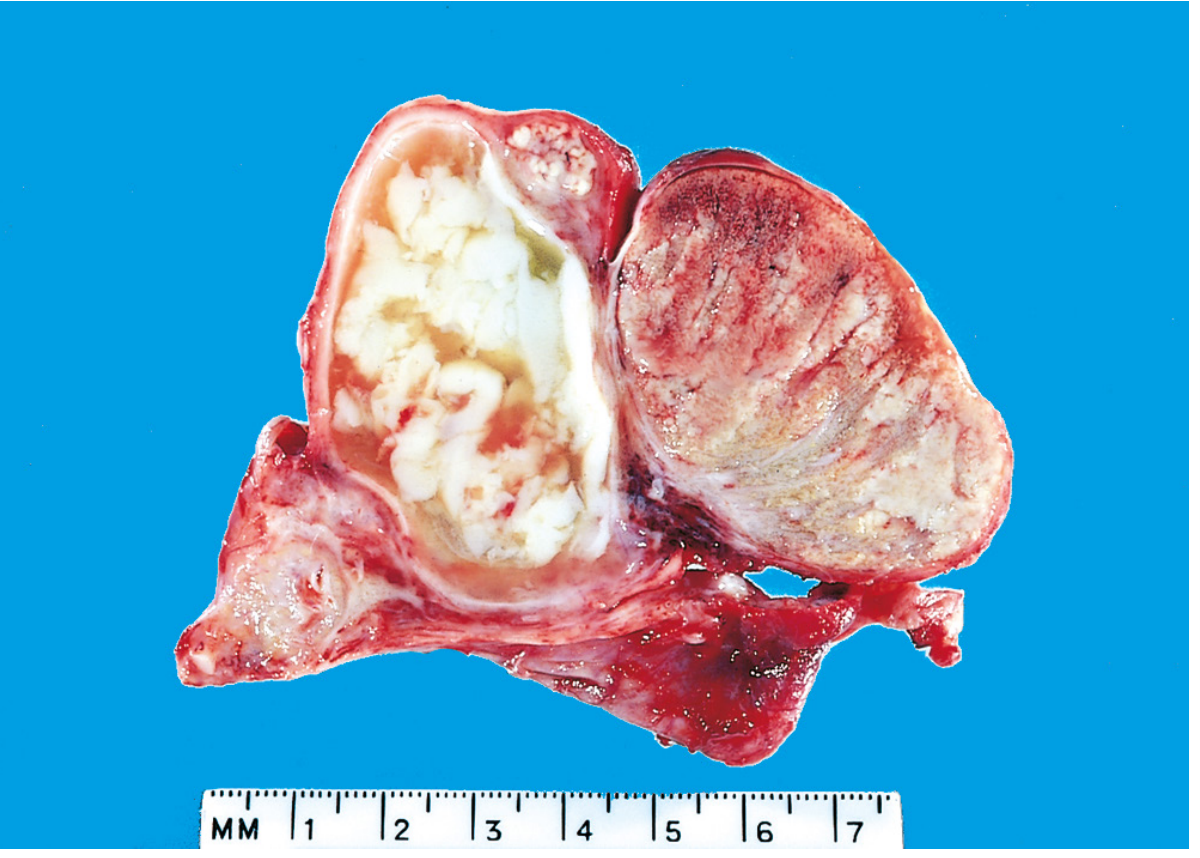
Pathology
Bacterial infection causes:
- Acute inflammation — congestion, edema, neutrophil infiltration
- Starts in interstitial connective tissue → spreads to tubules
- Can culminate in abscess formation or suppurative necrosis of the entire epididymis
- Spreads to testis → similar inflammatory reaction
- Fibrous scarring follows → may cause infertility
- Leydig cells are usually spared → androgen production preserved
Clinical Features
Symptoms
- Gradual onset scrotal pain (over 24–48 hours) — key distinction from torsion (sudden onset < 4–8 hours)
- Pain may radiate to the groin or flank
- Scrotal swelling and erythema
- Nausea/vomiting (from spermatic cord irritation)
- Urethral discharge (suggests STI)
- Dysuria, frequency (urethritis, cystitis, prostatitis may precede or coexist)
Signs
- Enlarged, red, tender scrotum
- Tender, enlarged epididymis (posterolateral) ± testis
- Cremasteric reflex intact (unlike torsion, where it is absent)
- Prehn sign positive — pain relief with scrotal elevation (suggestive of epididymitis, though not reliable for excluding torsion)
- Thickened spermatic cord (occasionally palpable)
- Reactive hydrocele may develop rapidly
Differential Diagnosis — Comparison Table
| Feature | Epididymo-Orchitis | Testicular Torsion | Appendage Torsion |
|---|---|---|---|
| Peak age | Adolescents, young adults | Neonates, adolescents | Prepubertal |
| Pain onset | Gradual, progressive | Sudden | Variable |
| Cremasteric reflex | Present | Absent | Present |
| Nausea/vomiting | Less likely | More likely | Less likely |
| Dysuria | More likely | Less likely | Less likely |
| Prehn sign | Positive | Negative | — |
Investigations
| Test | Finding |
|---|---|
| Urinalysis | WBCs, bacteria (pyuria/bacteriuria) |
| Urine culture | Identifies causative organism |
| Urethral swab + NAAT | For STI (gonorrhoea/chlamydia) |
| FBC | Leukocytosis |
| Scrotal Doppler Ultrasound | Gold standard imaging — sensitivity 92–100%; shows ↑blood flow to epididymis/testis (rules out torsion); may also show reactive hydrocele or abscess |
| Radionuclide scan | Alternative — uptake into center of testis rules out torsion |
Imaging caveat: In severe orchitis, testicular flow can be compromised — scrotal exploration should be considered in any equivocal case. A missed torsion = testicular loss.
In prepubertal boys diagnosed with epididymitis: Renal-bladder ultrasound (RBUS) + voiding cystourethrogram (VCUG) to exclude congenital anomalies (reflux, ectopic ureter).
Treatment
1. Supportive Care (All Cases)
- Bed rest
- Scrotal elevation (scrotal support/jockstrap)
- NSAIDs (e.g., ibuprofen) — reduce pain and inflammation duration
- Ice packs
- Analgesia
2. Antibiotic Therapy (Empiric — Based on Likely Etiology)
A. STI-likely (< 35 years, sexually active, gonorrhoea/chlamydia)
| Drug | Dose | Route | Duration |
|---|---|---|---|
| Ceftriaxone | 500 mg (or 250 mg per older guidelines) | IM single dose | Single dose |
| + Doxycycline | 100 mg | PO twice daily | 10–14 days |
European Association of Urology (EAU) guidelines: Ceftriaxone 500 mg IM + Doxycycline 200 mg as first dose.
B. MSM (insertive anal sex) — STI + enteric organisms
| Drug | Dose | Route | Duration |
|---|---|---|---|
| Ceftriaxone | 250–500 mg | IM single dose | Single dose |
| + Doxycycline | 100 mg | PO BD | 10 days |
| + Levofloxacin | 500 mg | PO daily | 10 days |
| OR Ofloxacin | 300 mg | PO BD | 10 days |
C. Enteric organisms likely (> 35 years, UTI-associated, no STI risk)
| Drug | Dose | Route | Duration |
|---|---|---|---|
| Levofloxacin | 500 mg | PO daily | 10 days |
| OR Ofloxacin | 300 mg | PO BD | 10 days |
(Ofloxacin is not currently available in the US or Canada)
D. If chlamydia only suspected (no gonorrhoea risk)
- Azithromycin 1 g PO single dose, OR
- Doxycycline 100 mg PO BD × 7 days
E. STI partners
- Sexual partners of confirmed STI cases must be treated to prevent reinfection.
3. Hospitalisation Indications (IV Antibiotics)
- Fever / systemic toxicity / sepsis
- Failure of outpatient therapy
- Immunocompromised patients
- Suspected tuberculosis (requires further evaluation ± admission)
4. Surgical Management
| Indication | Procedure |
|---|---|
| Scrotal abscess | Incision and drainage (I&D) ± antibiotics + urology consultation |
| Equivocal torsion | Emergent scrotal exploration |
| Chronic relapsing epididymitis / intractable scrotal pain | Epididymectomy / orchiectomy |
5. Special Cases
Viral orchitis (mumps):
- No specific antiviral therapy
- Supportive care: analgesics, ice, scrotal support
- MMR vaccination prevents mumps orchitis
Tuberculous epididymo-orchitis:
- Standard anti-TB therapy (RHEZ regimen)
- Almost always begins in epididymis → spreads to testis
- Produces caseating granulomatous inflammation
Immunocompromised patients:
- Broad coverage including antifungals if indicated
- Urology + Infectious disease referral
Complications
| Complication | Notes |
|---|---|
| Abscess formation | Requires surgical drainage |
| Infarction / gangrene | Rare, from severe vascular compromise |
| Infertility | From fibrous scarring of tubules (bilateral involvement especially in mumps) |
| Chronic epididymitis / chronic scrotal pain | May require epididymectomy |
| Fistula formation | Rare, in TB or severe infection |
Disposition
- Uncomplicated cases → discharge home with oral antibiotics, supportive care, and outpatient urology follow-up
- Complicated or equivocal → admission, IV antibiotics, urology consultation
Sources: Smith and Tanagho's General Urology 19e, p.234; Schwartz's Principles of Surgery 11e, p.1789; Tintinalli's Emergency Medicine, p.4041–4074; Rosen's Emergency Medicine; Robbins Pathologic Basis of Disease
This is a shared conversation. Sign in to Orris to start your own chat.