Expiratory wheezing
Reading File
search_medical_text
expiratory wheezing causes diagnosis management
search_medical_image
wheezing airway obstruction pathophysiology
GradeResponse
GradeResponse
Expiratory Wheezing
Pathophysiology
Wheezing is a high-pitched, musical respiratory sound produced by turbulent airflow through narrowed airways. Expiratory wheezing specifically occurs because airways naturally narrow during expiration (reduced elastic recoil + positive pleural pressure compresses airways), making obstruction more audible — or exclusively audible — during this phase.
Two key patterns (Harrison's, p. 7848):
- Polyphonic wheezing — multiple pitches simultaneously, from diffuse small airway narrowing (classic in asthma, COPD)
- Monophonic wheezing — single pitch, from a fixed obstruction of one airway (e.g., endobronchial tumor, foreign body)
Etiology
| Category | Conditions |
|---|---|
| Obstructive lung disease | Asthma, COPD, bronchiectasis |
| Cardiac | Congestive heart failure ("cardiac asthma" — peribronchial edema) |
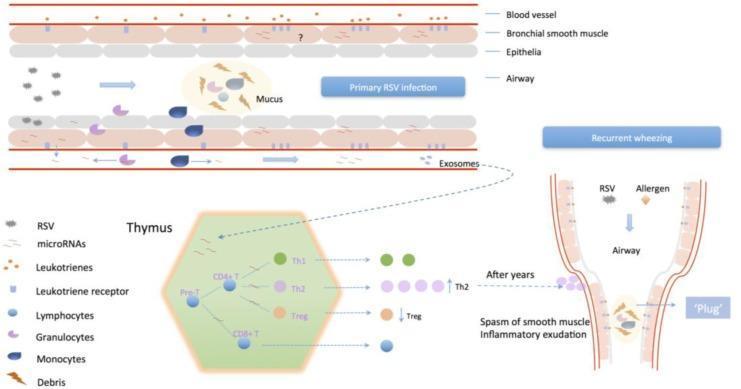
| Infectious | Bronchiolitis (RSV, esp. in infants), acute bronchitis, pneumonia |
| Structural/mechanical | Endobronchial tumor, foreign body aspiration, tracheobronchomalacia |
| Allergic/immunologic | Anaphylaxis, hypersensitivity pneumonitis, ABPA |
| Other | Vocal cord dysfunction (mimicker), GERD-induced bronchospasm, medications (beta-blockers, NSAIDs in aspirin-exacerbated respiratory disease) |
Key teaching point (Harrison's, p. 7848): "Clinicians must take care not to attribute all wheezing to asthma."
Clinical Features
- Expiratory-only wheezing suggests mild-to-moderate obstruction; airflow is adequate to generate sound
- Biphasic (inspiratory + expiratory) suggests severe obstruction or upper airway involvement
- Silent chest in an asthmatic = critical obstruction — too little airflow to generate wheeze (ominous sign)
- Associated symptoms guide etiology:
- Episodic + atopy history → asthma
- Chronic productive cough + smoking → COPD
- Orthopnea + peripheral edema → CHF
- Fever + URI prodrome in infant → bronchiolitis
- Acute onset after meal/play in child → foreign body
Diagnosis
History
- Onset (acute vs. chronic), triggers (allergens, exercise, cold air, NSAIDs), smoking, occupational exposures, atopy, cardiac history
Physical Exam
- Confirm wheeze is truly expiratory (auscultate full respiratory cycle)
- Accessory muscle use, prolonged expiratory phase, hyperinflation
Investigations
| Test | Indication |
|---|---|
| Spirometry (pre/post-bronchodilator) | Confirm obstructive pattern; reversibility suggests asthma |
| Peak expiratory flow (PEF) | Bedside severity assessment, monitoring |
| Chest X-ray | Hyperinflation (asthma/COPD), pulmonary edema (CHF), foreign body |
| CT chest (HRCT) | Bronchiectasis, air trapping, endobronchial lesion |
| Bronchoscopy | Suspected foreign body, tumor, structural lesion |
| Allergy testing / IgE | Atopic workup |
| BNP/NT-proBNP + echo | CHF differentiation |
| Methacholine challenge | Airway hyperresponsiveness when spirometry normal |
Management
Management is directed at the underlying cause:
Asthma
- Acute: SABA (albuterol) via inhaler/nebulizer, systemic corticosteroids, ipratropium, Mg²⁺ sulfate (IV) in severe cases
- Chronic: Stepwise GINA approach — low-dose ICS → ICS/LABA → add-ons (LAMA, biologic for eosinophilic/type 2)
COPD
- Acute exacerbation: SABA ± SAMA, systemic steroids, antibiotics (if purulent/infective trigger), O₂ titrated to SpO₂ 88–92%
- Chronic: LAMA ± LABA, ICS in frequent exacerbators, pulmonary rehab
Cardiac Asthma (CHF)
- IV diuretics (furosemide), nitrates, treat underlying heart failure — bronchodilators have limited role
Bronchiolitis (infants)
- Supportive: hydration, nasal suctioning, O₂ if needed; bronchodilators generally not recommended per AAP guidelines
Foreign Body
- Urgent bronchoscopic removal
Anaphylaxis
- IM epinephrine (0.3–0.5 mg, 1:1000), supine, airway support, IV antihistamines/steroids
Red Flags Requiring Urgent Action
- Silent chest (absent wheeze with respiratory distress)
- SpO₂ < 92% despite supplemental O₂
- Inability to speak in full sentences
- Cyanosis, altered mentation, paradoxical breathing
- New-onset wheeze in elderly (consider CHF, malignancy)
- Unilateral wheeze (foreign body or tumor until proven otherwise)
This is a shared conversation. Sign in to Orris to start your own chat.