vertebral roatation surgery
Reading File
search_medical_text
vertebral rotation surgery scoliosis derotation techniques
search_medical_text
spinal deformity correction surgical approaches vertebral derotation outcomes
search_medical_image
vertebral rotation scoliosis surgical correction
GradeResponse
GradeResponse
GradeResponse
Vertebral Rotation Surgery
Vertebral rotation surgery refers to surgical procedures aimed at correcting axial vertebral rotation (AVR) — the rotational deformity of vertebrae around the long axis of the spine, most commonly seen in scoliosis and other 3-dimensional spinal deformities.
Why Vertebral Rotation Matters
Scoliosis is not simply a lateral curve — it is a 3-dimensional deformity involving:
- Coronal plane: lateral curvature (measured by Cobb angle)
- Sagittal plane: loss of normal kyphosis/lordosis
- Axial/transverse plane: vertebral rotation — often the most functionally significant component, causing rib hump and trunk imbalance
Correcting rotational deformity is a key goal of modern spinal deformity surgery.
Indications for Surgery
| Condition | Surgical Trigger |
|---|---|
| Adolescent Idiopathic Scoliosis (AIS) | Cobb angle >45–50°, progressive curve |
| Congenital Scoliosis | Progressive curves, vertebral anomalies |
| Neuromuscular Scoliosis | Functional impairment, cardiopulmonary compromise |
| Adult Degenerative Scoliosis | Pain, neurological deficit, progression |
Brace treatment is ineffective for rigid structural curves, particularly in congenital scoliosis (Bailey & Love's, p. 542).
Surgical Techniques for Vertebral Derotation
1. Rod Rotation (Cotrel-Dubousset Technique)
- Classic technique: a pre-contoured rod is placed in the coronal plane then rotated 90°
- Converts the lateral curve into sagittal contour
- Achieves indirect vertebral derotation
- Limitation: incomplete axial derotation, can cause "adding-on" or flat back
2. Direct Vertebral Rotation (DVR)
The modern gold standard for axial derotation.
- Vertebral Column Manipulator (VCM) or similar device attached to pedicle screws at the apex
- Applies a controlled rotational force en bloc across multiple apical vertebral levels
- Corrects the apical vertebral rotation directly in the transverse plane
- Superior to rod rotation for 3D correction
See intraoperative image below demonstrating DVR using a VCM construct:
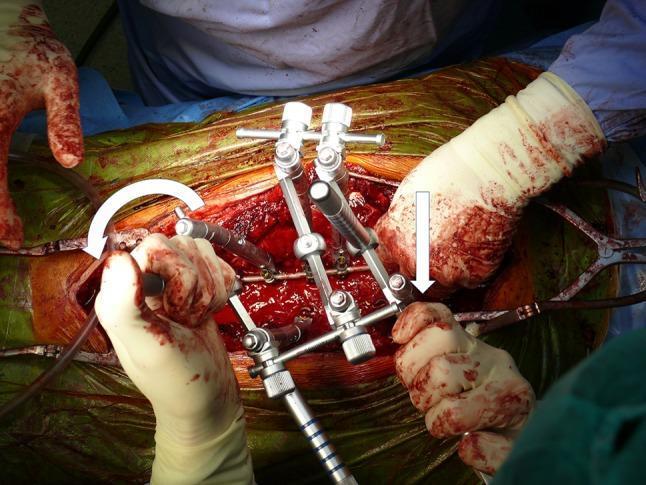
3. Apical Vertebral Derotation (AVD)
- Individual derotation maneuvers applied sequentially to each vertebra using derotation handles on pedicle screws
- More precise control per level compared to en bloc techniques
- Commonly combined with DVR
4. Hemivertebra Excision
- Used in congenital scoliosis with a fully segmented hemivertebra
- Excision of the anomalous vertebra removes the asymmetric growth driver
- Followed by short-segment fusion
- Bailey & Love's (p. 542) identifies this as a primary surgical option for progressive congenital curves
5. Posterior Instrumented Correction and Fusion (PICF)
- Standard approach for most scoliosis types
- Pedicle screws inserted bilaterally across multiple levels
- Rod contouring + rotation + compression/distraction maneuvers applied
- Fusion achieved with bone graft/allograft
6. Growing Rod Constructs (Pediatric Patients)
- Magnetically Controlled Growing Rods (MCGR): non-invasive lengthening via external magnet
- Used in skeletally immature children to control curve while allowing spinal growth
- Definitive fusion deferred until near skeletal maturity (Bailey & Love's, p. 542)
Surgical Approach
| Approach | Use Case |
|---|---|
| Posterior (most common) | AIS, neuromuscular, most deformities |
| Anterior | Thoracolumbar/lumbar curves, disc release for rigid curves |
| Combined anterior-posterior | Severe/rigid curves (>70–80°), revision cases |
| Lateral (XLIF/OLIF) | Adult degenerative scoliosis, disc space correction |
Instrumentation
- Pedicle screws: the workhorse — provide 3-column fixation and enable rotational correction
- Hooks and wires: older adjuncts, still used in select cases
- Rods: titanium or cobalt-chrome; shape pre-contoured to desired sagittal profile
- Cross-links: add construct rigidity
Intraoperative Monitoring
- Neuromonitoring (SSEP + MEP): mandatory during derotation maneuvers to detect spinal cord compromise
- Wake-up test: if neuromonitoring changes occur
- Fluoroscopy / intraoperative CT (O-arm): confirm screw placement and deformity correction
Complications
| Complication | Rate / Notes |
|---|---|
| Neurological deficit | <1% with modern monitoring |
| Screw malposition | 5–15%; most clinically silent |
| Infection (deep) | 1–4%; higher in neuromuscular patients |
| Pseudarthrosis / non-union | 2–5%; risk increases with longer constructs |
| Proximal/distal junctional kyphosis | 5–40% depending on definition; long-term concern |
| Implant failure | Rod breakage, especially at lumbosacral junction |
| Crankshaft phenomenon | Growth around a fused spine in immature patients |
Outcomes
- Modern posterior instrumented fusion with DVR achieves 50–70% correction of Cobb angle and significant improvement in axial rotation
- Patient-reported outcomes (SRS-22, ODI scores) show substantial quality-of-life improvement
- Fusion rates >95% with current techniques
- Long-term: most AIS patients lead normal, active lives post-surgery
Summary
The goal of vertebral rotation surgery is 3-dimensional deformity correction — not just reducing the lateral Cobb angle but restoring axial alignment and trunk balance. Direct Vertebral Rotation (DVR) using pedicle screw-based constructs is the current standard, with hemivertebra excision and growing rods reserved for congenital and pediatric cases respectively.
This is a shared conversation. Sign in to Orris to start your own chat.