Systemic lupas erythematus
Reading File
search_medical_text
systemic lupus erythematosus pathophysiology clinical features diagnosis
search_medical_image
systemic lupus erythematosus malar rash butterfly rash
GradeResponse
GradeResponse
search_medical_text
SLE diagnostic criteria SLICC ACR classification management treatment
GradeResponse
Here is a comprehensive overview of Systemic Lupus Erythematosus (SLE):
Systemic Lupus Erythematosus (SLE)
Overview
SLE is a chronic, multisystem autoimmune disease characterized by the production of autoantibodies, immune complex deposition, and widespread inflammation affecting virtually any organ system. It follows a relapsing-remitting course and predominantly affects women of childbearing age (female:male ratio ~9:1).
Pathophysiology
SLE results from a breakdown in immune self-tolerance, leading to:
- Autoantibody production — particularly anti-double-stranded DNA (anti-dsDNA) and anti-Smith (anti-Sm)
- Immune complex formation and deposition — circulating complexes (DNA + anti-DNA) deposit in tissues (kidneys, skin, joints, vessels), activating the complement cascade
- Complement-mediated damage — leukocyte infiltration, procoagulant factor activation, and cytokine release cause end-organ injury
- Loss of apoptotic debris clearance — defective clearance of nuclear material serves as a persistent antigenic stimulus
Clinical Features
SLE is the "great imitator." Key manifestations by system:
| System | Features |
|---|---|
| Constitutional | Fatigue, fever, weight loss |
| Skin | Malar (butterfly) rash, discoid rash, photosensitivity, oral ulcers, alopecia |
| Musculoskeletal | Arthritis/arthralgia (non-erosive), myalgia |
| Renal | Lupus nephritis (hematuria, proteinuria, HTN, renal failure) |
| Cardiovascular | Pericarditis, Libman-Sacks endocarditis, accelerated atherosclerosis |
| Pulmonary | Pleuritis, interstitial lung disease, pulmonary HTN |
| Neuropsychiatric | Seizures, psychosis, cognitive dysfunction, stroke |
| Hematologic | Hemolytic anemia, leukopenia, lymphopenia, thrombocytopenia |
| Serositis | Pleuritis, pericarditis |
Classic Malar (Butterfly) Rash
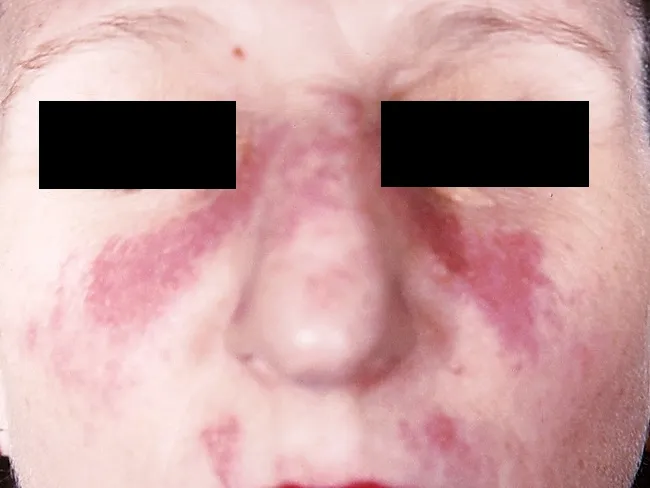
Bilateral erythematous rash across the malar eminences and nasal bridge, characteristically sparing the nasolabial folds. Exacerbated by sun exposure.
Diagnosis
EULAR/ACR 2019 Criteria (most current)
- Entry criterion: Positive ANA (≥1:80 by immunofluorescence) — present in >98% of SLE patients
- Scoring: Accumulate ≥10 points from weighted clinical and immunologic domains
- Specificity 97%, sensitivity 93%
SLICC Criteria (older, clinically useful)
- Requires ≥4 criteria (at least 1 clinical + 1 immunologic), OR lupus nephritis confirmed by biopsy + positive ANA or anti-dsDNA
- Specificity 97%, sensitivity 84% (Harrison's, p. 9974)
Key Autoantibodies
| Antibody | Significance |
|---|---|
| ANA | Screening test; >98% sensitive, low specificity |
| Anti-dsDNA | Highly specific; correlates with disease activity and nephritis |
| Anti-Sm | Highly specific; does not correlate with activity |
| Anti-Ro/La | Associated with neonatal lupus, subacute cutaneous lupus |
| Anti-phospholipid | Associated with thrombosis, recurrent miscarriage |
| Anti-histone | Drug-induced lupus |
Lupus Nephritis
A common and serious complication, present in 30% of patients at diagnosis. More common in Black, Asian, and Hispanic patients. Caused by deposition of immune complexes in mesangial, subendothelial, and subepithelial spaces, leading to complement activation and glomerular injury. (Harrison's, p. 8577)
ISN/RPS Classification (Classes I–VI) guides treatment intensity:
- Class III/IV (focal/diffuse proliferative) — most severe; requires aggressive immunosuppression
- Class V (membranous) — presents with nephrotic syndrome
- Biopsy is essential for classification
Management
General Principles
- Sun protection — essential for all SLE patients
- Regular monitoring — renal function, CBC, complement (C3/C4), anti-dsDNA
Drug Therapy
| Indication | Treatment |
|---|---|
| All SLE patients | Hydroxychloroquine (reduces flares, organ damage, mortality) |
| Mild-moderate disease | NSAIDs, low-dose glucocorticoids |
| Moderate-severe disease | Glucocorticoids + mycophenolate mofetil or azathioprine |
| Lupus nephritis (Class III/IV) | High-dose glucocorticoids + mycophenolate or cyclophosphamide |
| Refractory/severe disease | Belimumab (anti-BLyS), voclosporin, rituximab |
| Neuropsychiatric SLE | High-dose steroids ± immunosuppressants |
| Antiphospholipid syndrome | Anticoagulation (warfarin/heparin) |
Key Points on Hydroxychloroquine
- Reduces risk of flares, organ damage, thrombosis, and improves overall survival
- Should be used in virtually all SLE patients unless contraindicated
- Annual ophthalmologic screening required (risk of retinopathy)
Complications & Prognosis
- Renal failure — leading cause of morbidity in the first decade
- Cardiovascular disease — accelerated atherosclerosis; leading cause of death in later disease
- Infections — from immunosuppression
- Malignancy — slightly increased risk (especially lymphoma)
- Antiphospholipid syndrome — thrombosis, recurrent pregnancy loss
5-year survival is now >90% with modern therapy; 10-year survival ~80%. Mortality is higher in patients with severe renal or neuropsychiatric involvement.
Special Populations
- Pregnancy: SLE can flare during pregnancy; anti-Ro/La antibodies risk neonatal lupus and congenital heart block. Hydroxychloroquine is safe and should be continued.
- Drug-induced lupus: Caused by hydralazine, procainamide, isoniazid, minocycline; anti-histone antibodies are characteristic; resolves on drug cessation.
- Pediatric SLE: More severe renal and hematologic involvement compared to adults.
Key takeaway: SLE requires a multidisciplinary approach, long-term follow-up, and individualized therapy. Hydroxychloroquine is the cornerstone of all treatment regimens.
This is a shared conversation. Sign in to Orris to start your own chat.