Ventriculomegaly in fetus
Reading File
Finding Sources
Finding Sources
Searching PubMed
fetal ventriculomegaly diagnosis outcome
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Reading File
Loading Image
Reading File
Reading File
Loading Image
I now have all the information needed for a comprehensive answer.
Fetal Ventriculomegaly
Definition and Grading
Ventriculomegaly (VM) is defined as dilation of one or both lateral ventricles with an atrial width ≥10 mm, measured on the axial plane at the level of the parieto-occipital sulcus. It is a sign, not a diagnosis — it has a broad differential and reflects a variety of underlying pathologies.
| Grade | Measurement |
|---|---|
| Mild (borderline) | 10–12 mm |
| Moderate | 12.1–14.9 mm |
| Severe | ≥15 mm |
Note: The terms ventriculomegaly and hydrocephaly are sometimes used interchangeably in the literature, but VM is preferred because it identifies the sonographic finding independently of etiology. "Hydrocephaly" is typically reserved for ventricles >15 mm.
Incidence
- Overall incidence: 1–2 per 1,000 births
- Mild/borderline VM: 1.4 per 1,000 (low-risk) to 22 per 1,000 (high-risk) populations
- Males are more commonly affected than females
Ultrasound Appearance
Mild VM (borderline) — axial view, atria 11.5 mm and 10.5 mm:
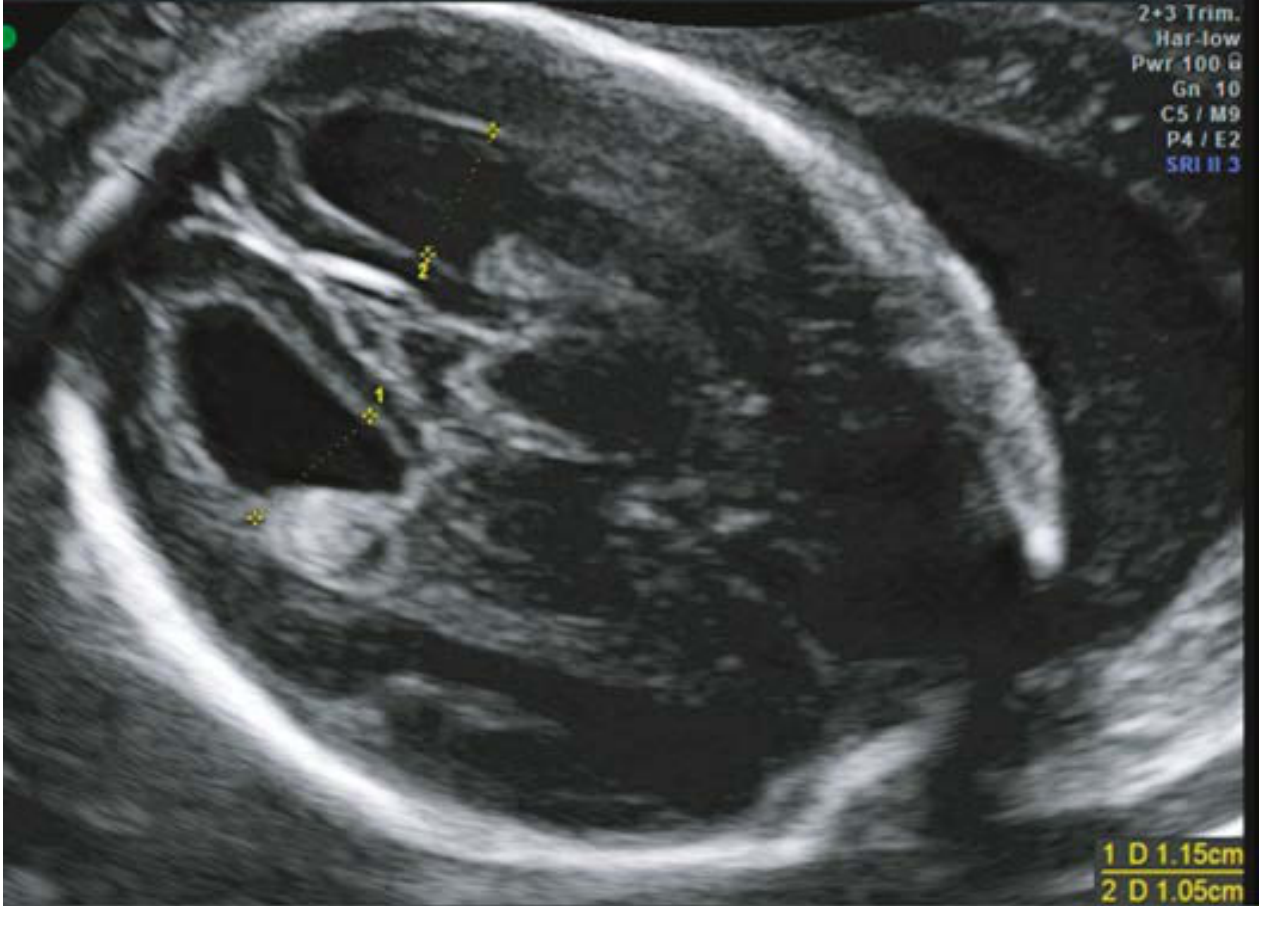
Axial US: Bilateral borderline ventriculomegaly (1.15 cm and 1.05 cm). The choroid plexus may appear dangling (dependent).
Severe VM — axial view with minimal residual brain mantle:
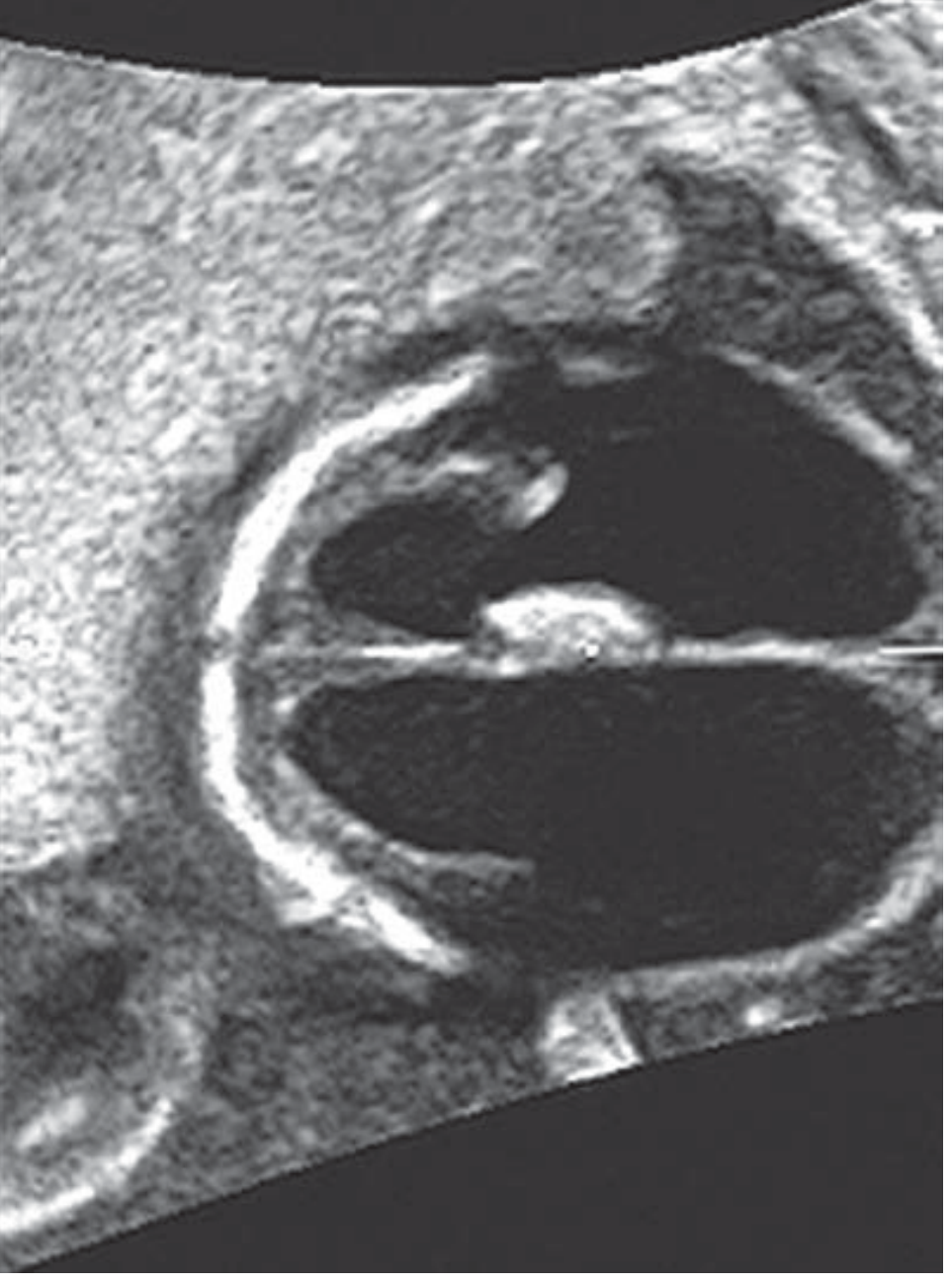
Axial US: Bilateral severe ventriculomegaly (25 mm and 30 mm) with minimal residual brain tissue.
Differential Diagnosis (Box 19.2)
Obstructive Causes
- Aqueductal stenosis (AS) — most common cause, accounts for 30–40% of all fetal VM
- Chiari II malformation (myelomeningocele-related)
- Dandy-Walker malformation
- Intracranial tumor
Structural Brain Anomalies
- Agenesis of the corpus callosum (ACC) — classic: teardrop-shaped dilated atria (colpocephaly), steer-horn configuration on coronal view
- Septo-optic dysplasia
- Schizencephaly (wedge-shaped gray matter-lined cleft extending to ventricle)
- Porencephaly / encephalomalacia / hemorrhage
Chromosomal / Genetic
- Trisomy 21 (most common aneuploidy), followed by trisomies 18 and 13
- X-linked (L1CAM mutation at Xq28) — consider in males; associated with adducted thumbs
Infections (TORCH)
- CMV — periventricular calcifications, echogenic lining of ventricle
- Toxoplasmosis — bilateral severe VM with reduced brain parenchyma
- Zika virus (in endemic areas)
Other
- Ischemia/hemorrhage (e.g., monochorionic twin demise)
- Idiopathic
Key Causes in Detail
1. Aqueductal Stenosis
The most common single cause. Narrowing of the Sylvian aqueduct connecting the 3rd and 4th ventricles leads to non-communicating hydrocephalus. ~75% is idiopathic; other causes: L1CAM mutation, CMV, hemorrhage. Features: severe bilateral VM >15 mm, dangling choroid plexus, macrocephaly, dilated 3rd ventricle, normal posterior fossa, abducted thumbs in X-linked form. Incidence: 3–15 per 10,000 births; X-linked form 1:30,000 males.
2. Arnold-Chiari II Malformation
Open spinal defect (myelomeningocele) with herniation of cerebellar vermis and brainstem through foramen magnum. VM/hydrocephaly occurs in 80–90% of cases. Classic cranial signs: "lemon" sign (frontal bone scalloping) and "banana" sign (compressed cerebellum), seen in >95% of cases at 16–24 weeks. Elevated maternal serum AFP.
3. Dandy-Walker Malformation
Developmental arrest of the hindbrain at 4–6 weeks. Features: large posterior fossa cyst communicating with 4th ventricle, absent/hypoplastic vermis, splayed cerebellar hemispheres, elevated tentorium. VM present in 70–80% of cases. Incidence: 1:30,000; accounts for 4–12% of infantile hydrocephaly. Associated anomalies in 60% of prenatally diagnosed cases.
Workup / Prenatal Evaluation
Imaging
- Detailed anatomic ultrasound survey — neurosonography (assess corpus callosum, CSP, vermis, posterior fossa)
- Fetal echocardiogram — cardiac anomalies are common associations
- Fetal MRI — recommended, especially when:
- Dedicated neurosonography is unavailable
- Additional CNS anomalies are suspected
- Third-trimester assessment for cortical, white matter, or hemorrhagic abnormalities (MRI is superior)
- A 2020 international multicenter study supported MRI in every fetus with prenatal VM; if isolated on neurosonography, low risk of associated anomaly
Genetic / Laboratory
- Amniocentesis: karyotype ± chromosomal microarray
- Amniotic fluid PCR: CMV, toxoplasmosis
- If X-linked hydrocephaly suspected in males: L1CAM gene mutation (Xq28)
- Zika serology if in endemic area
- Maternal serum AFP if spinal dysraphism suspected
Consultations
- Genetic counseling
- Pediatric neurology
Obstetric Management
| Situation | Management |
|---|---|
| Mild isolated VM | Vaginal delivery not contraindicated; serial US to monitor progression |
| No macrocephaly | Trial of labor in vertex presentation |
| Macrocephaly / cephalopelvic disproportion | Cephalocentesis controversial (may worsen prognosis); CS reserved for obstetric indications |
| Before viability | Option of pregnancy termination should be offered |
Neonatal Management
- Neonatology, pediatric neurology, and neurosurgery evaluation
- Postnatal head ultrasound and/or MRI
- Serial head circumference measurements
- Surgical management (VP shunt) for progressive VM
Prognosis
Isolated Mild VM (10–12 mm)
- Likely represents a normal variant in many cases
- Resolution before 24 weeks in 62% of cases
- >90% of neonates have a normal postnatal evaluation when truly isolated
- Pooled prevalence of neurodevelopmental delay in isolated mild VM: 4.9% (RR 3.5 vs. general population)
- Overall aneuploidy rate for mild VM: ~3%; infection rate: ~0.4%
Associated/Progressive VM
- Prognosis is determined by the underlying etiology (e.g., trisomy 21, ACC, aqueductal stenosis)
- In utero progression of VM is associated with increased neurologic sequelae
- Associated structural/chromosomal malformations present in ~41% of mild-moderate VM cases
| Finding | Implication |
|---|---|
| Isolated mild, resolves | Excellent prognosis |
| Isolated mild, stable | Generally favorable; small risk of neurodevelopmental delay |
| Mild + other anomalies | Prognosis depends on associated finding |
| Moderate-severe | Worse outcomes; depends on etiology |
| Severe with minimal mantle | Poor; differentiate from hydranencephaly by MRI |
Key Points Summary
- Measure atrial width at the level of the parieto-occipital sulcus; ≥10 mm = VM
- VM is a sign — always search for the underlying cause
- Aqueductal stenosis is the most common single etiology (30–40%)
- MRI adds significant diagnostic value, especially for cortical and white matter abnormalities
- Isolated mild VM has an excellent prognosis; associated or progressive VM carries significantly worse outcomes
- Serial surveillance ultrasound is mandatory once VM is detected
— Creasy & Resnik's Maternal-Fetal Medicine: Principles and Practice, Chapters 19–20
Ventriculomegaly in brain of fetus
The previous response already covered fetal ventriculomegaly comprehensively — including definition/grading, incidence, ultrasound imaging, differential diagnosis, workup, obstetric and neonatal management, and prognosis.
Is there a specific aspect you'd like me to go deeper on? For example:
- Neuroanatomy of the ventricular system and CSF pathways
- MRI findings in specific subtypes (aqueductal stenosis, ACC, Dandy-Walker)
- Genetic counseling and recurrence risks
- Postnatal neurosurgical management (shunting, ETV)
- A specific etiology in more detail (e.g., CMV, Chiari II, X-linked hydrocephalus)
This is a shared conversation. Sign in to Orris to start your own chat.