Arm, truk fungal infection which is treatment
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Loading Image
Fungal Infection of the Arm & Trunk (Tinea Corporis)
Tinea corporis ("ringworm") is a dermatophyte infection of the glabrous (relatively hairless) skin of the body — commonly the arms, trunk, legs, and face. The causative organisms are Trichophyton rubrum (most common), T. interdigitale, Microsporum canis, and Epidermophyton floccosum.
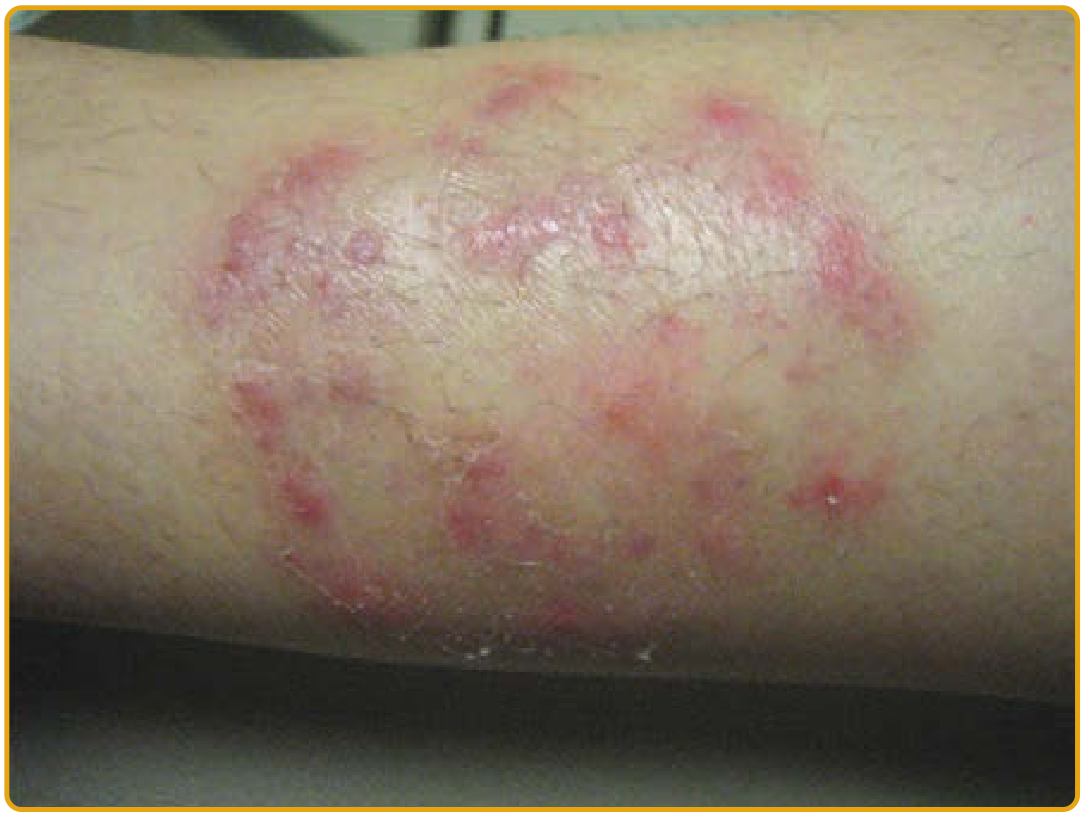
Clinical Features
- Erythematous, scaly plaques with an annular (ring-shaped) appearance
- Active, raised, scaly border with central clearing
- Itchy (pruritic)
- Deep inflammatory nodules/granulomas can occur if inappropriately treated with topical corticosteroids
Diagnosis
- KOH preparation of skin scrapings: reveals fungal hyphae
- Culture or histology (PAS stain) if needed
Treatment
1. Topical Antifungals — First Line for Mild/Limited Disease
Apply twice daily for 2–4 weeks (continue 1 week beyond clinical resolution):
| Drug Class | Examples |
|---|---|
| Allylamines | Terbinafine 1% cream/gel (most effective; can be once daily × 7 days) |
| Imidazoles | Clotrimazole 1%, Miconazole 2%, Ketoconazole 2% cream |
| Other | Tolnaftate, Butenafine, Ciclopirox |
Terbinafine 1% cream once daily for 7 days is highly effective for tinea corporis. — Textbook of Family Medicine 9e
2. Oral Antifungals — For Widespread, Inflammatory, or Recalcitrant Disease
| Drug | Dose | Notes |
|---|---|---|
| Terbinafine | 250 mg once daily × 2–4 weeks | Most effective oral agent; fungicidal |
| Itraconazole | 100–200 mg/day | Check for drug interactions (CYP450); avoid in heart failure |
| Griseofulvin | 500 mg/day (microsize) | Older agent; approved for skin/hair/nail dermatophytosis; SE: GI upset, headache |
| Fluconazole | 150 mg once weekly | Alternative option |
Oral antifungal agents are reserved for widespread or more inflammatory eruptions. — Fitzpatrick's Dermatology
All oral agents may cause hepatotoxicity. Should not be used in pregnant or breastfeeding women. — Harrison's Principles of Internal Medicine 22E
Special Situations
| Situation | Management |
|---|---|
| Tinea incognito (steroid-modified tinea) | Stop corticosteroid; treat with topical/oral antifungal |
| Extensive/recurrent disease | Oral terbinafine or itraconazole |
| Immunocompromised host | Oral therapy preferred; longer duration |
| Follicular involvement (Majocchi granuloma) | Oral antifungals required (topicals ineffective) |
Key Points
- Do NOT use topical corticosteroids alone — worsens infection and causes tinea incognito
- Nystatin is not active against dermatophytes (only useful for Candida)
- Keep skin dry and clean — fungal infections thrive in moisture
- Treat close contacts and shared fomites (towels, clothing) to prevent reinfection
Sources: Harrison's Principles of Internal Medicine 22E, Fitzpatrick's Dermatology, Goldman-Cecil Medicine, Textbook of Family Medicine 9e
This is a shared conversation. Sign in to Orris to start your own chat.