Tendon transfer definition types application and disadvantages structures everything for to answer 10 marks question with appropriate illustrative diagrams
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
Searching Images
tendon transfer surgery hand orthopedic diagram
Reading File
Searching Images
opponensplasty radial nerve palsy tendon transfer procedure illustration
Loading Image
Loading Image
Loading Image
Loading Image
Loading Image
This answer covers every component examiners expect for a 10-mark question. Here's a quick orientation:
What's covered:
- Definition — precise surgical definition sourced from Rockwood & Green's
- Principles — 9 key prerequisites using the SEEMS SAFE mnemonic for easy recall
- Types — by mechanism (direct, pulley, free muscle) and by goal (motor, tenodesis, stabilization)
- Applications — with full tables for:
- Radial nerve palsy (wrist drop) — PT→ECRB, FCU→EDC, PL→EPL
- Median nerve palsy — opponensplasty options (FDS, EIP, ADM, PL)
- Ulnar nerve palsy — anti-claw procedures
- Other conditions (foot drop, elbow flexion, CP, polio)
- Structures involved — donor tendons table with nerve supply, normal action, and use; fixation methods (Pulvertaft weave, end-to-side, bone anchor)
- Disadvantages — 11 specific limitations
- 4 intraoperative/postoperative photographs illustrating real surgical scenarios
The mark allocation table at the end maps the answer to the 10-mark rubric so you can allocate writing space in an exam accordingly.
Free flap in orthopaedics Tendon transfer definition types application and disadvantages structures everything for to answer 10 marks question with appropriate illustrative diagrams
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Searching Images
free flap microvascular reconstruction orthopaedic open fracture lower limb
Reading File
Searching Images
free fibula flap vascularized bone graft tibia reconstruction diagram
Loading Image
Loading Image
Loading Image
Loading Image
Loading Image
Loading Image
Excellent — I now have all the content and images needed. Here is the full comprehensive 10-mark answer on both topics.
PART 1: FREE FLAP IN ORTHOPAEDICS
Definition
A free flap (free tissue transfer) is a block of tissue — which may include skin, fascia, muscle, bone, or a combination — that is completely detached from its donor site along with its vascular pedicle (artery + vein), then transferred to a distant recipient site where the pedicle vessels are microsurgically anastomosed to local recipient vessels, restoring perfusion to the transplanted tissue.
"A free flap is where a block of tissue is isolated on its pedicle... but at this point, instead of maintaining the pedicle in continuity, it is divided and anastomosed to recipient vessels within the desired location." — Rockwood & Green's Fractures in Adults, 10th ed.
Why Free Flaps in Orthopaedics?
Free flaps are indicated when local and regional flap options are unavailable or insufficient, particularly in:
- Complex open fractures (Gustilo IIIB/IIIC) with large soft tissue defects
- Chronic osteomyelitis with dead space and poor local vascularity
- Post-tumour resection bone/soft tissue gaps
- Degloving injuries
- Failed previous local flap coverage
The orthoplastic approach — combined simultaneous management by orthopaedic and plastic surgeons — has become the standard of care. Flap survival is significantly better when reconstruction is performed within 72 hours of injury (Godina's principle, 1986).
Classification / Types of Free Flaps
A. By Tissue Composition
| Type | Components | Example Flaps |
|---|---|---|
| Fasciocutaneous | Skin + fascia | Anterolateral thigh (ALT), radial forearm, SCIP flap |
| Myocutaneous | Muscle + skin | Latissimus dorsi, rectus abdominis |
| Muscle-only | Muscle (+ skin graft later) | Gracilis, rectus abdominis |
| Osseocutaneous / Vascularized bone | Bone ± soft tissue | Free fibula, iliac crest, scapula |
| Free functioning muscle transfer | Innervated muscle for motor function | Gracilis (for elbow flexion/finger flexion) |
B. By Perforator Pattern
| Type | Description |
|---|---|
| Axial pattern | Based on a named artery (e.g., radial forearm — radial artery) |
| Perforator flap | Based on musculocutaneous perforators without sacrificing the parent muscle (e.g., ALT — descending branch of lateral circumflex femoral artery) |
Commonly Used Free Flaps in Orthopaedics
1. Anterolateral Thigh (ALT) Flap — Workhorse for lower limb
- Pedicle: Descending branch of lateral circumflex femoral artery
- Size: Up to 25 × 35 cm skin paddle; pedicle length 8–12 cm
- Landmarks: ASIS to lateral border of patella; perforators at midpoint within 4 cm circle
- Advantages: Large, reliable, thin, pliable; low donor morbidity; simultaneous harvest possible
- Used for: Gustilo IIIB tibial fracture soft tissue cover
2. Latissimus Dorsi Flap — Largest muscle flap
- Pedicle: Thoracodorsal artery (branch of subscapular artery)
- Provides large volume — excellent for filling dead space in osteomyelitis cavities
- Requires additional skin graft
- Used for: Open tibial fractures, osteomyelitis, shoulder defects
3. Rectus Abdominis Flap
- Pedicle: Deep inferior epigastric artery
- Large muscle, easy harvest
- Used for: Tibial defects, large soft tissue gaps
4. Gracilis Flap — Free functioning muscle transfer
- Pedicle: Medial circumflex femoral artery (entering proximal third of muscle)
- Innervated by anterior branch of obturator nerve → connected to recipient motor nerve
- Used for: Elbow flexion restoration (brachial plexus injury), finger flexion, facial reanimation
- Muscle must be placed under proper tension and re-educated
5. Free Fibula Flap — Gold standard vascularized bone graft
- Pedicle: Peroneal artery (sacrificed — preoperative angiogram mandatory)
- Harvest: 2 cm distal to fibula neck → 6 cm proximal to lateral malleolus (protect ankle syndesmosis and peroneal nerve)
- Up to 25 cm of cortical bone available; can carry overlying skin paddle (5 cm width)
- Used for: Large tibial/femoral bone defects, pathological fractures through osteomyelitis, tumour reconstruction, congenital pseudarthrosis
6. Radial Forearm Flap
- Pedicle: Radial artery (Allen test mandatory preop to confirm ulnar supply)
- Thin, pliable, long pedicle, reliable
- Donor: Skin grafted; visible scar, risk to radial nerve cutaneous branches
7. Scapular / Parascapular Flap
- Pedicle: Circumflex scapular artery (branch of subscapular artery)
- Used for: Lateral ankle/foot coverage
8. SCIP (Superficial Circumflex Iliac Artery Perforator) Flap
- Thin and long; donor scar in groin/lower abdomen — closed primarily for flaps ≤8 cm width
- Used for: Foot defects (thin, durable coverage)
Structures of a Free Flap
FREE FLAP — COMPONENTS
═══════════════════════════════════════════
┌──────────────────────────┐
│ TISSUE BLOCK │ ← Skin / Fascia / Muscle / Bone
│ │
│ Feeding ARTERY ────────┼──→ Microsurgical anastomosis
│ Draining VEIN(S) ──────┼──→ to recipient vessels
│ │
│ (± NERVE) ─────────────┼──→ Coapted for motor/sensory function
└──────────────────────────┘
DONOR SITE
(closed primarily or skin grafted)
═══════════════════════════════════════════
ANASTOMOSIS TYPES:
• End-to-end (most common)
• End-to-side (when recipient vessel must be preserved)
Recipient vessels in the lower limb:
- Posterior tibial artery/vein
- Anterior tibial artery/vein
- Peroneal artery/vein
Prerequisites for Free Flap Surgery ("WPES")
| Requirement | Detail |
|---|---|
| Well-prepared patient | Medically optimized; no inotropic support (causes vasospasm); CT angiogram of limb |
| Plan B ready | If first flap fails, second option must not be compromised by first |
| Equipped theatre | Operating microscope, microsurgical instruments, experienced scrub team |
| Safe postoperative monitoring | Flap temperature, colour, turgor, Doppler; intensive in first 48–72 hours |
Timing of Free Flap
| Window | Evidence |
|---|---|
| < 72 hours | Lowest failure rate (Godina 1986) |
| 3–7 days | "No man's land" — zone of injury established, local vessels compromised |
| > 7 days | Significantly higher failure rates |
Current orthoplastic consensus: definitive fixation and flap coverage should be simultaneous or as close together as possible.
Postoperative Monitoring
- Clinical: colour, turgor, temperature, capillary refill, pin-prick bleeding
- Handheld Doppler (most common adjunct)
- Implantable Doppler, laser Doppler, thermography
- Dangling protocol: progressive limb dependency over 3–5 days to prevent venous congestion
- Salvageable vascular problems arise mostly in first 24–48 hours; continue monitoring to day 4
Complications / Disadvantages of Free Flaps
| Complication | Details |
|---|---|
| Flap failure (partial/complete) | Quoted up to 20% in literature — arterial or venous thrombosis |
| Donor site morbidity | Scarring, weakness (LD donor: shoulder girdle), vascular sacrifice (radial artery) |
| Prolonged surgery | Often 6–12+ hours; risk of hypothermia, coagulopathy, deep vein thrombosis |
| Venous congestion | Commonest early complication; treated by re-exploration and thrombectomy |
| Arterial insufficiency | Vasospasm or anastomotic thrombosis → ischaemia |
| Requires specialist team | Not available in all centres — limits access |
| Re-exploration risk | Patients must consent to potential return to theatre |
| Donor site healing | Radial forearm (visible scar + cold intolerance), ALT (scar, nerve injury) |
| Complex rehabilitation | Lengthy bed rest, "dangling" protocol, prolonged physiotherapy |
| Infection | Despite vascularized tissue, infection remains possible — especially in osteomyelitis beds |
| Flap bulk | May require secondary thinning/revision surgery |
Illustrative Diagrams
Fig. 1 — ALT free flap for Gustilo IIIC open tibia fracture: complete limb salvage sequence
(A) Gustilo IIIC open fracture of lower leg with massive soft tissue loss. (B) Post-debridement with plate fixation and ALT free flap harvested. (C) Cross-leg flap pedicle stabilized with external fixator. (D) Patient ambulating with Ilizarov frame. (E) AP radiograph showing bone healing. (F) Long-term functional outcome at 8 years.
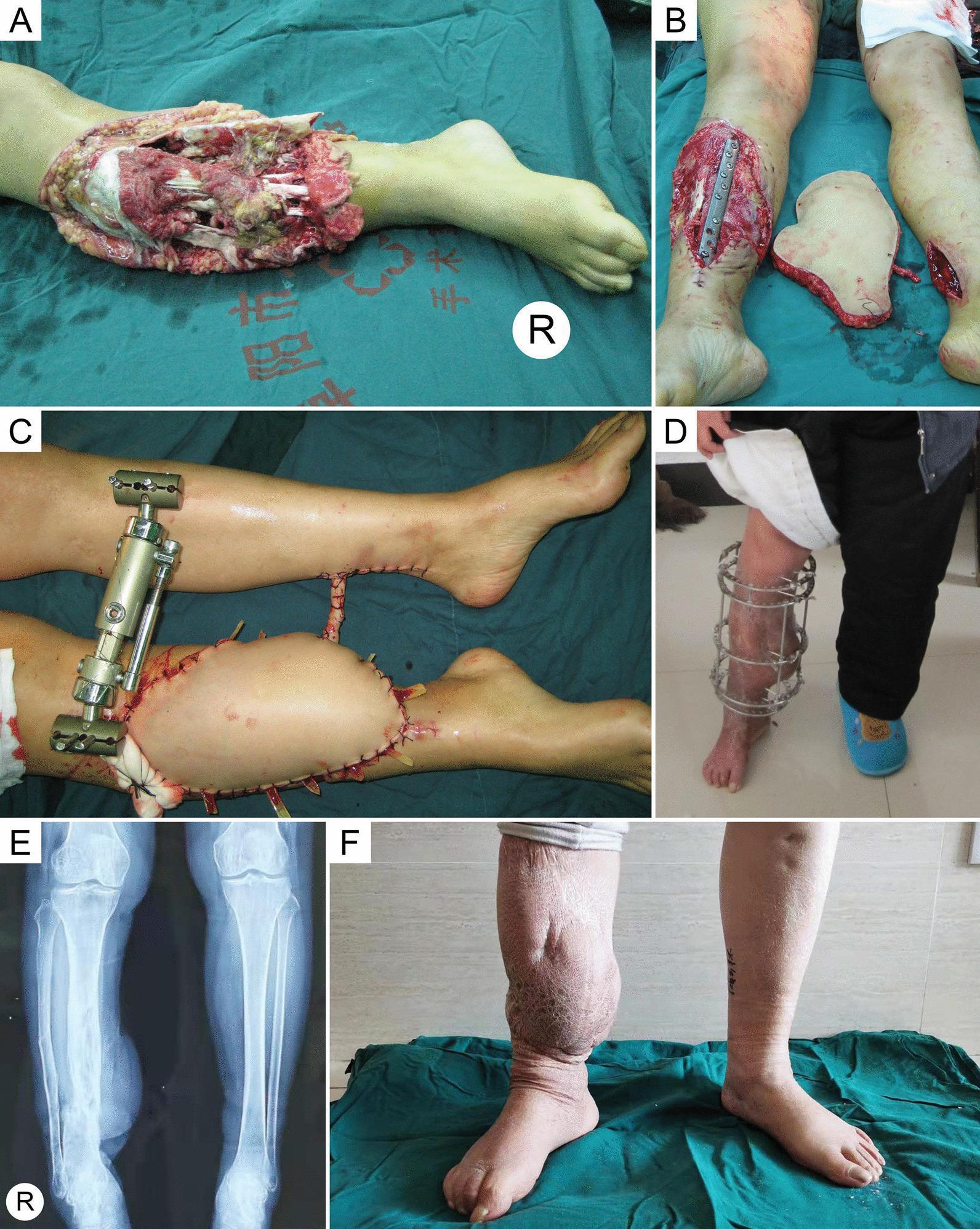
Fig. 2 — Free fibula flap for tibial reconstruction: surgical steps and radiograph
(A) Marking donor leg. (B) Dissecting down to fibula — superficial peroneal nerve protected. (C) Fibula cut proximally and distally with peroneal pedicle. (D) Flap mobilized. (E) AP X-ray of pathological open tibial fracture through chronic osteomyelitis. (F) Tibial defect with cement spacer. (G) Free fibula graft inset. (H) Final clinical outcome. (I) AP radiograph with fibula in situ.
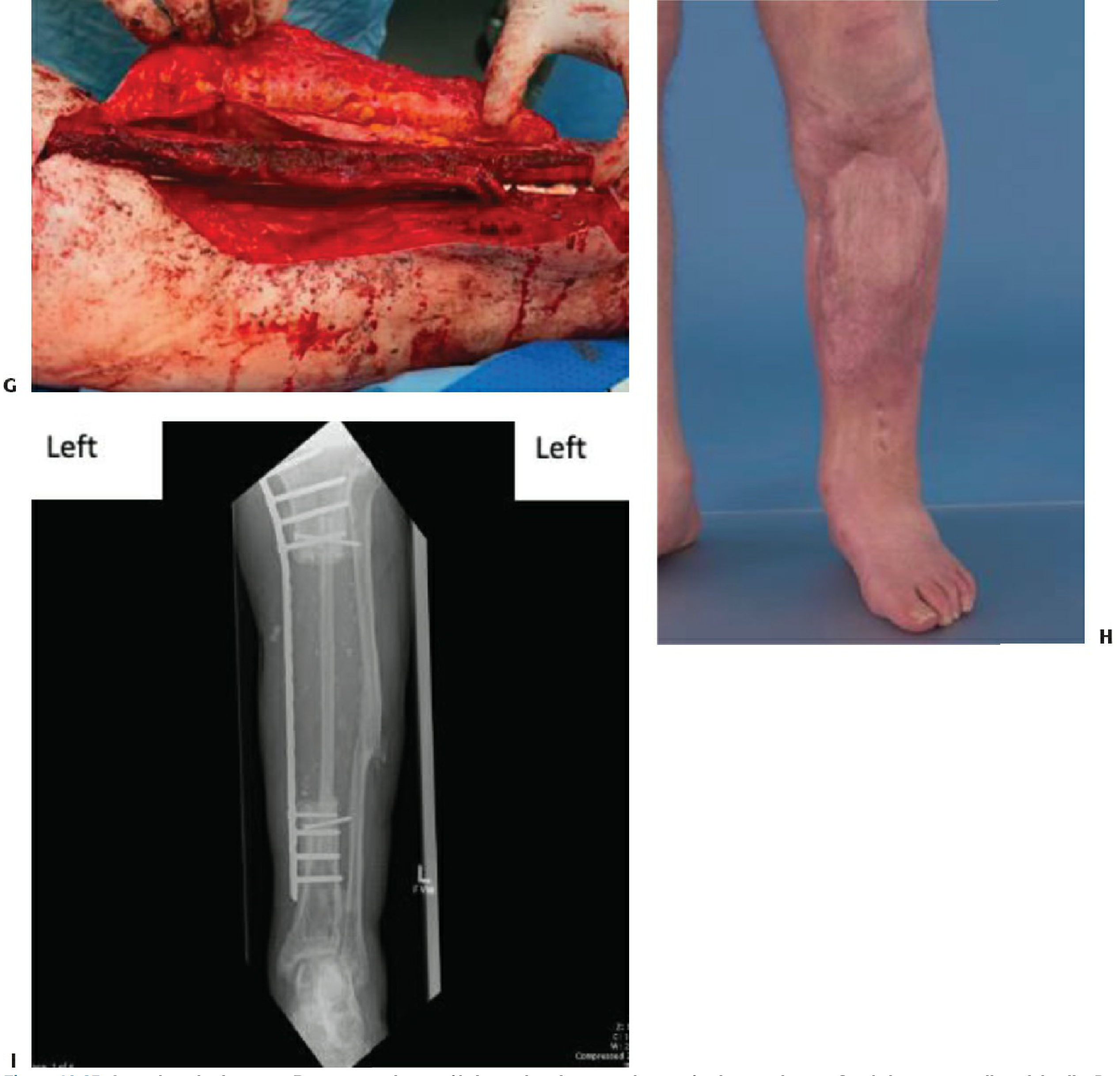
Fig. 3 — Rectus abdominis free muscle flap for open tibial fracture coverage (A: debridement; B: muscle flap; C: skin graft)
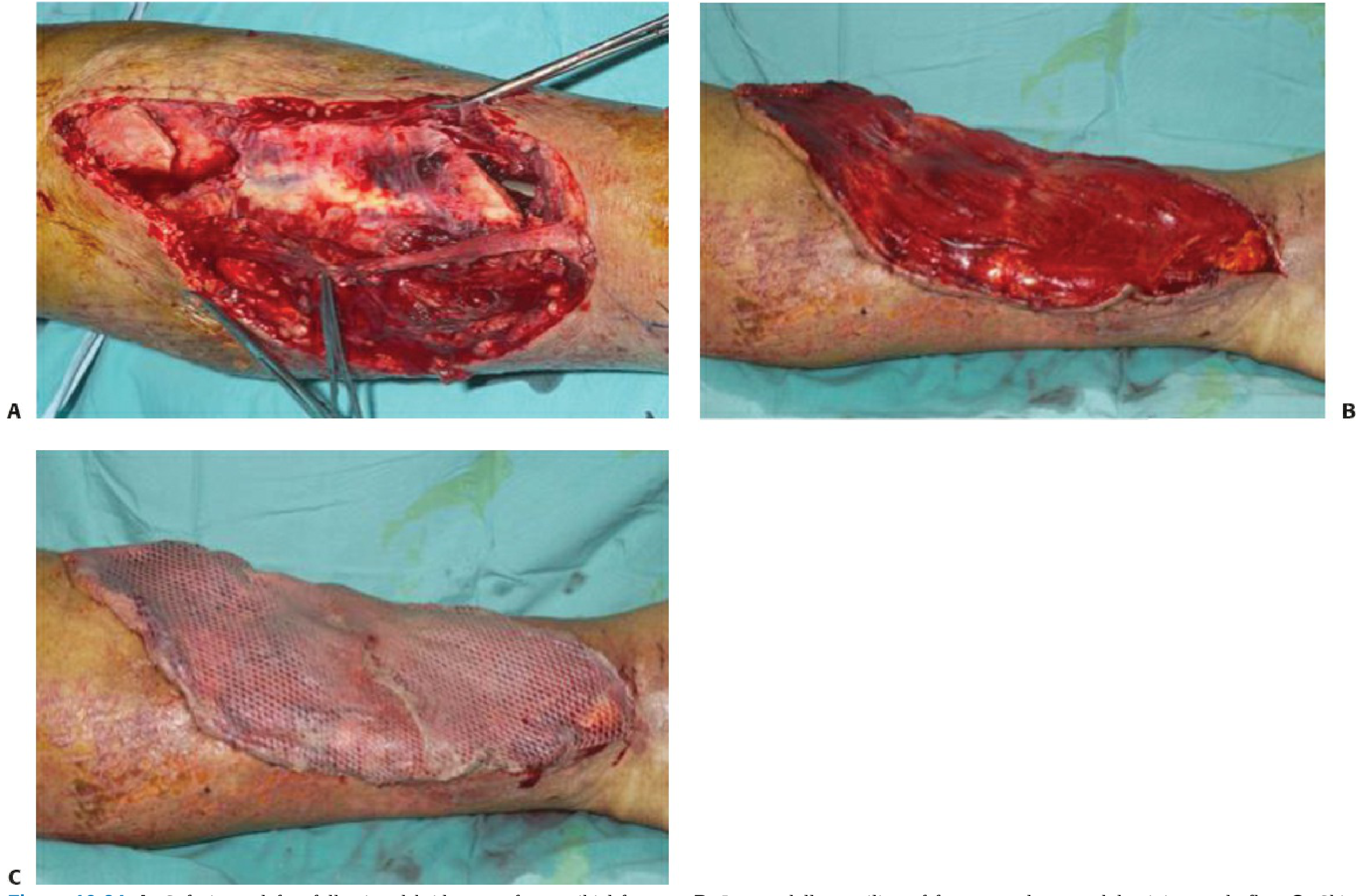
Fig. 4 — Free gracilis muscle flap for open ankle/hindfoot defect, with skin graft coverage
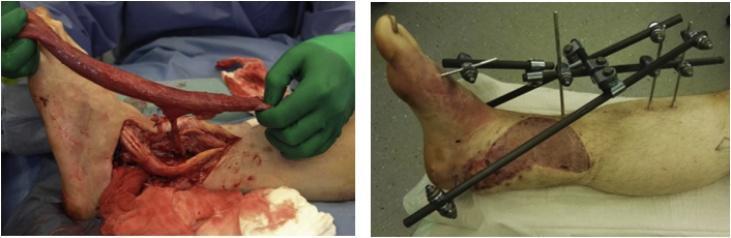
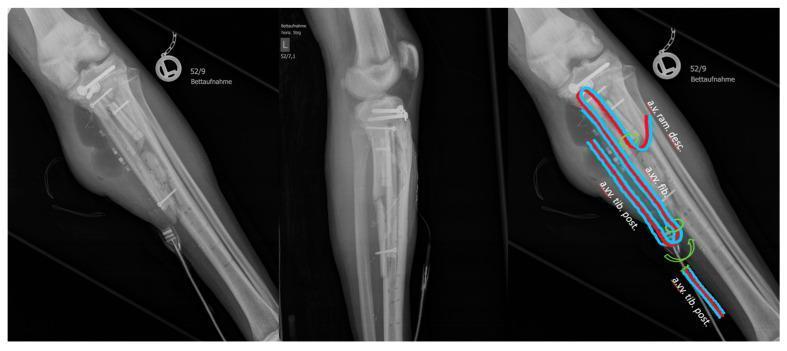
Fig. 5 — Double-loop flow-through free flap radiograph with vascular diagram overlay
(Posterior tibial, fibular vessels, and descending ramus anastomoses illustrated — red = arterial, blue = venous, green circles = anastomotic sites)
PART 2: TENDON TRANSFER (RECAP + ADDITIONAL DETAIL)
Definition
Tendon transfer is a reconstructive procedure in which a functioning, expendable muscle–tendon unit is detached from its original insertion and redirected to restore the function of a paralyzed or absent muscle.
"Tendon transfer involves transfer of a healthy muscle and tendon to replace the function of a paralyzed muscle." — Rockwood & Green's Fractures in Adults, 10th ed.
Principles — "SEEMS SAFE"
| Principle | |
|---|---|
| S | Soft tissue equilibrium (full passive ROM must be present) |
| E | Expendable donor (must not sacrifice a critical movement) |
| E | Excursion match (amplitude of donor ≈ that required at recipient) |
| M | Motor strength MRC grade 5 ideal (grade lost after transfer) |
| S | Synergistic muscles preferred (easier re-education) |
| S | Single function per transfer |
| A | Alignment — straight line of pull |
| F | Firm fixation (Pulvertaft weave — end-to-side preferred) |
| E | Expendable function not compromised at donor site |
Types of Tendon Transfer
| Category | Type | Example |
|---|---|---|
| By mechanism | Direct | FCU → EDC |
| Pulley | FDS ring → APB via pisiform pulley (opponensplasty) | |
| Free functioning muscle | Gracilis for elbow flexion | |
| By purpose | Motor restoration | Paralysed muscle replaced |
| Tenodesis | Tendon fixed to bone — passive motion drives distal joint | |
| Static stabilization | Prevent deformity |
Applications
Radial Nerve Palsy ("Wrist Drop") — Most tested clinically
| Function Lost | Donor | Recipient |
|---|---|---|
| Wrist extension | Pronator teres (PT) | ECRB |
| Finger extension | FCU or FCR | EDC |
| Thumb extension | Palmaris longus (PL) | EPL |
Median Nerve Palsy — Opponensplasty
Goal: Restore thumb opposition (abductor pollicis brevis).
- FDS ring finger (most common) — via pisiform pulley
- EIP, ADM (Huber), PL — all into APB
Ulnar Nerve Palsy — Anti-Claw
- Prevents MCP hyperextension in ring/little fingers
- Procedures: Brand (ECRB + tendon graft), Zancolli (FDS lasso), Bunnell
Other Applications
| Condition | Transfer |
|---|---|
| Elbow flexion loss (brachial plexus) | Steindler flexorplasty / pectoralis transfer |
| Foot drop | Tibialis posterior through interosseous membrane to dorsum |
| Shoulder (axillary nerve) | Trapezius to greater tuberosity |
| Cerebral palsy | FCU → ECRB (wrist extension) |
Structures Involved
| Structure | Role |
|---|---|
| Donor muscle-tendon unit | Source of active power |
| Subcutaneous tunnel | Route of transfer (must be straight) |
| Pulley or bone tunnel | Redirects line of pull |
| Recipient tendon | Target insertion (Pulvertaft weave or end-to-side) |
| Bone anchor | Insertional transfers |
Common donor tendons:
| Tendon | Nerve | Used For |
|---|---|---|
| Pronator teres | Median | → ECRB (wrist extension) |
| FCR | Median | → EDC (finger extension) |
| FCU | Ulnar | → EDC (finger extension) |
| Palmaris longus | Median | → EPL / opponensplasty |
| FDS ring | Median | → APB (opposition) |
| EIP | Radial | → EPL (thumb extension) |
| Brachioradialis | Radial | → FPL (thumb flexion) |
Disadvantages
| Disadvantage | Detail |
|---|---|
| One MRC grade lost | Routine strength loss after transfer |
| Donor morbidity | Weakens original action |
| Single function only | Multiple operations for complex deficits |
| Re-education required | Prolonged physiotherapy; non-synergistic = harder |
| Not restorative | No sensation; not normal anatomy |
| Strict prerequisites | Fails if passive ROM limited, tissue scarred |
| Tensioning errors | Over/under-tension leads to failure |
| Adhesions | Tendon may stick along its tunnel |
| Delayed rehab | 6–12 weeks immobilization then months physiotherapy |
| No donor available | May need free functioning muscle transfer instead |
Illustrative Diagrams — Tendon Transfer
Fig. 6 — FCR → EDC and PL → EPL for posterior interosseous nerve palsy (Pulvertaft weave at wrist)
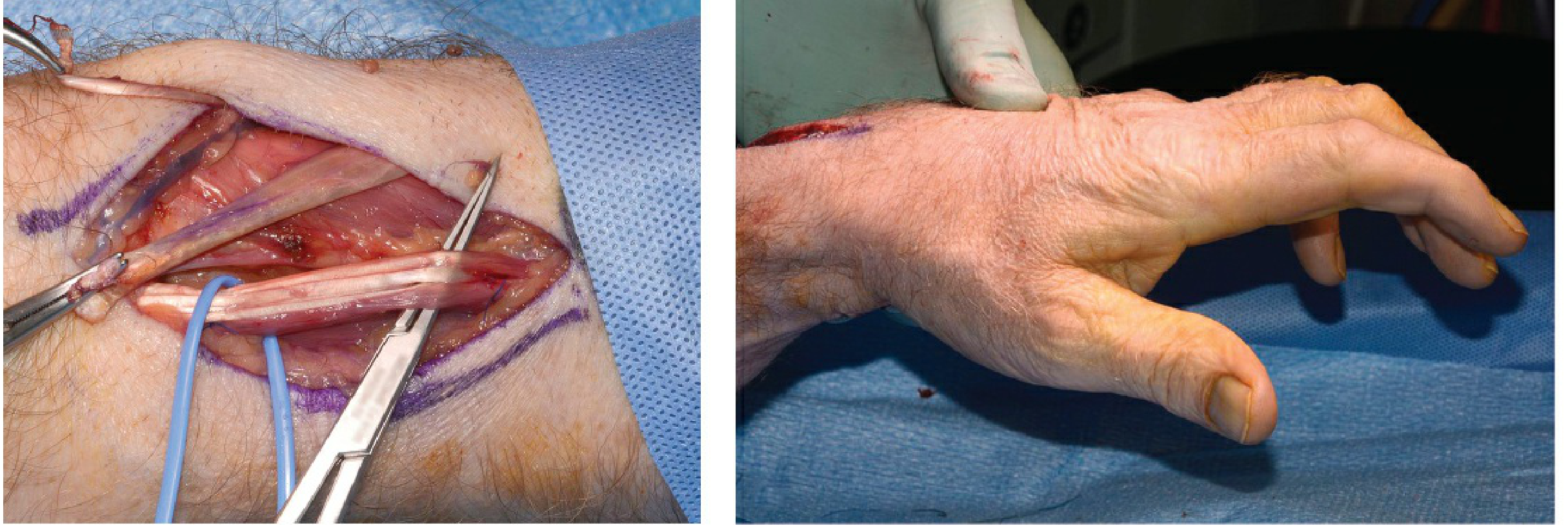
Figure 6. FCR woven into EDC and PL woven into EPL with multiple locking sutures (A) restoring finger and thumb extension (B). — Rockwood & Green's Fractures in Adults, 10th ed.
Summary Comparison Table
| Feature | Free Flap | Tendon Transfer |
|---|---|---|
| Purpose | Soft tissue / bone reconstruction | Motor function restoration |
| Indications | Open fractures, osteomyelitis, tumour | Nerve palsy, paralysis |
| Vascular requirement | Microsurgical anastomosis | Not applicable |
| Key structure | Pedicle artery + vein | Expendable muscle–tendon |
| Key complication | Flap failure, venous congestion | Strength loss, re-education failure |
| Specialist requirement | Microvascular surgery, orthoplastic team | Hand/reconstructive surgeon |
| Timing | Ideally within 72 hours | After nerve recovery plateau (6–12 months) |
10-Mark Answer Allocation
| Component | Marks |
|---|---|
| Free Flap: Definition + classification | 2 |
| Free Flap: Types with examples (ALT, LD, fibula, gracilis) | 2 |
| Free Flap: Complications/disadvantages | 1 |
| Tendon Transfer: Definition + principles | 2 |
| Tendon Transfer: Applications (radial/median/ulnar) | 2 |
| Tendon Transfer: Disadvantages | 1 |
| Total | 10 |
Sources:
- Rockwood and Green's Fractures in Adults, 10th ed. 2025 — Chapter 19 (Soft tissue coverage) & Chapter 20 (Nerve injuries / Tendon transfer)
- Miller's Review of Orthopaedics, 9th ed. — Nerve injuries and tendon transfers
- Current Surgical Therapy, 14th ed. — Muscle and tendon transfer
This is a shared conversation. Sign in to Orris to start your own chat.