Davidson principle and practice latest edition ischemia of heart notes for hkmle
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Reading File
I have enough rich content to compile comprehensive HKMLE-focused notes on Ischemic Heart Disease. Let me now produce the full structured notes.
❤️ Ischaemic Heart Disease (IHD) — HKMLE Notes
Based on Braunwald's Heart Disease, Robbins & Kumar Basic Pathology, Harrison's Principles of Internal Medicine 22e
1. DEFINITION & OVERVIEW
IHD = a group of syndromes caused by an imbalance between myocardial oxygen supply and demand, almost always due to coronary atherosclerosis (>90% of cases).
Synonyms: Coronary artery disease (CAD), coronary heart disease (CHD)
Key concept: Myocardial cells depend exclusively on mitochondrial oxidative phosphorylation → strictly dependent on continuous oxygenated blood flow.
2. CLINICAL SYNDROMES
| Syndrome | Mechanism | Reversible? |
|---|---|---|
| Stable angina | Fixed stenosis → demand ↑ | Yes |
| Unstable angina | Plaque rupture + thrombus | Yes (no necrosis) |
| Prinzmetal/Variant angina | Coronary vasospasm | Yes |
| NSTEMI | Partial/subendocardial infarct | No (necrosis) |
| STEMI | Complete occlusion → transmural infarct | No (necrosis) |
| Sudden cardiac death (SCD) | Fatal ventricular arrhythmia | No |
| Chronic IHD with CHF | Accumulated ischemic damage | Progressive |
Acute Coronary Syndrome (ACS) = Umbrella term for: Unstable angina + NSTEMI + STEMI (+ SCD)
3. PATHOGENESIS
A. Fixed Atherosclerotic Stenosis
- < 70% occlusion → usually asymptomatic at rest
- ≥ 70% occlusion → exertional angina (inadequate hyperaemic response)
- ≥ 90% occlusion → symptoms at minimal exertion or rest
B. Acute Plaque Change (the critical mechanism for ACS)
Sequence in typical MI:
- Plaque erosion or rupture → exposes subendothelial collagen + necrotic plaque contents
- Platelet adhesion and aggregation → platelet plug
- Activation of coagulation cascade → fibrin-rich thrombus
- Vasospasm triggered by platelet mediators (thromboxane A2, serotonin)
- Within minutes to hours → complete occlusion → STEMI
C. Other Causes of IHD (minority)
- Coronary vasospasm (Prinzmetal; healthy vessels possible)
- Embolism from mural thrombi (AF) or valve vegetations
- Demand ischaemia: tachycardia, hypertension, hypotension, anaemia, hypoxia
- Small vessel disease: vasculitis, amyloid, sickle cell
4. ANGINA PECTORIS
Clinical Features (Harrison's)
- Typical patient: Male >50 yrs, female >60 yrs
- Character: Heaviness, pressure, squeezing, smothering (rarely "pain")
- Location: Central, substernal — patient places hand over sternum (Levine's sign = clenched fist over sternum)
- Radiation: Left arm (ulnar aspect), jaw, back, interscapular region, neck, epigastrium
- NOT above mandible, NOT below umbilicus, NOT trapezius (trapezius radiation → pericarditis)
- Duration: 2–5 minutes
- Triggers: Exertion, emotion, cold, heavy meals, sexual activity
- Relief: Rest (1–5 min), sublingual nitrates
Three Variants
| Type | Cause | ECG during attack | Treatment |
|---|---|---|---|
| Stable angina | Fixed stenosis, demand ↑ | ST depression | Nitrates, beta-blockers, CCBs |
| Prinzmetal (Variant) | Coronary vasospasm | ST elevation | Vasodilators (nitrates, CCBs) |
| Unstable angina | Plaque rupture + thrombus | ST depression / normal | ACS management (heparin, aspirin, PCI) |
Canadian Cardiovascular Society (CCS) Grading of Angina
| Class | Description |
|---|---|
| I | Angina only with strenuous activity; ordinary activity doesn't cause angina |
| II | Slight limitation — angina on walking >2 blocks on level, climbing >1 flight |
| III | Marked limitation — angina on walking 1–2 blocks, climbing 1 flight |
| IV | Inability to carry on any activity without discomfort; angina at rest |
5. MYOCARDIAL INFARCTION
Definition (2018 Universal Definition)
"Acute myocardial injury detected by abnormal cardiac biomarkers in the setting of evidence of acute myocardial ischaemia"
Risk Factors
- Age (10% MI <40 yrs; 45% MI <65 yrs)
- Male sex (women protected pre-menopause; post-menopausal risk equalises)
- Hypertension, diabetes, dyslipidaemia, smoking, obesity, family history
Coronary Artery Territory
| Artery | Territory Supplied | ECG Leads |
|---|---|---|
| LAD | Anterior LV, anterior 2/3 septum, apex | V1–V4 |
| RCA | Posterior LV, posterior septum, SA node, AV node | II, III, aVF |
| LCx | Lateral wall LV | I, aVL, V5–V6 |
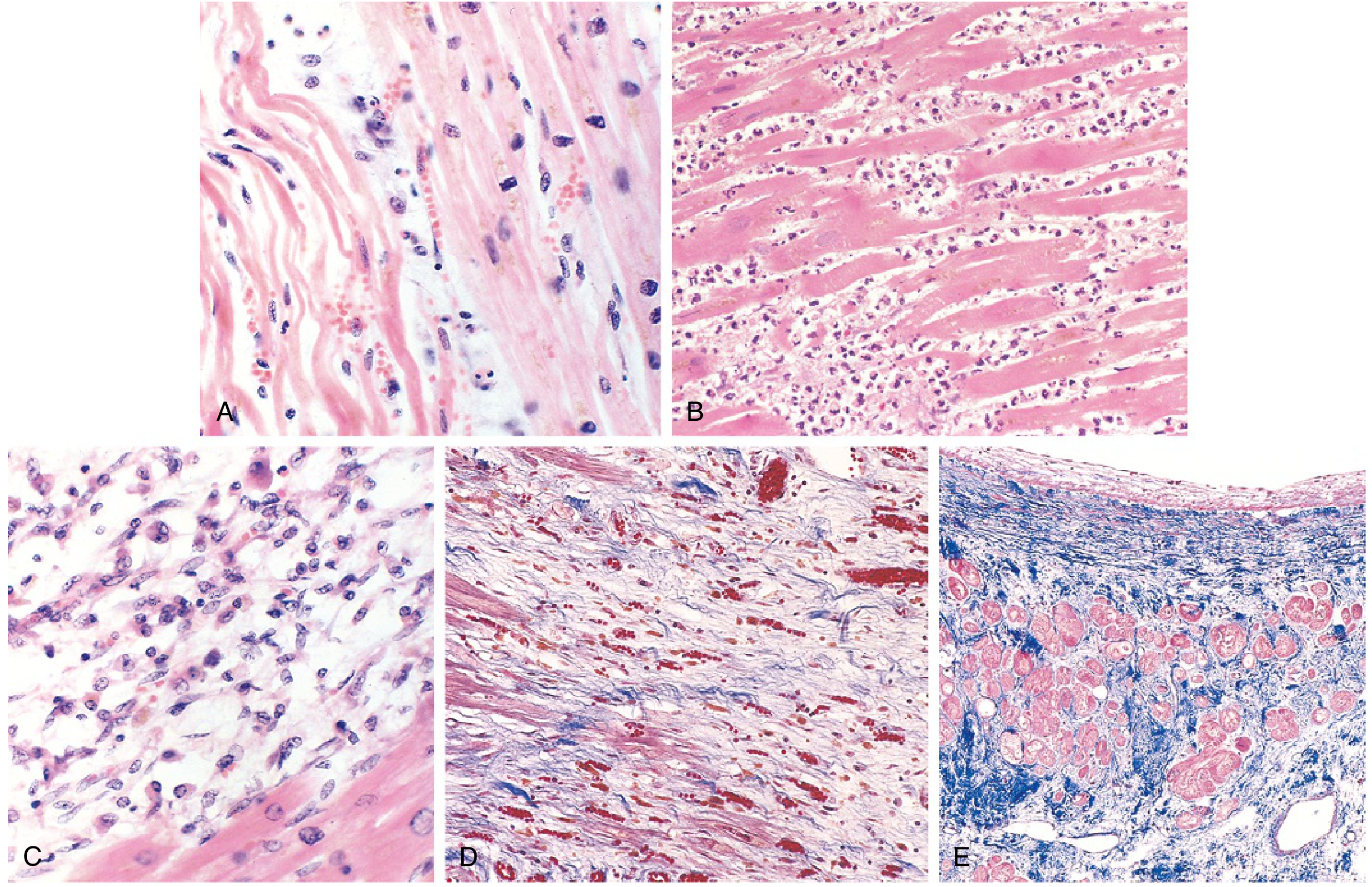
Pathological Changes (Robbins)
| Time | Gross | Microscopy |
|---|---|---|
| 0–30 min | None | None (reversible injury) |
| 30 min–4 hrs | None | None visible |
| 4–12 hrs | Dark mottling (early) | Coagulative necrosis begins, wavy fibres |
| 12–24 hrs | Dark mottling | Coagulative necrosis + oedema |
| 1–3 days | Mottling with yellow-tan centre | Neutrophil infiltration (peak 1–3 days) |
| 3–7 days | Hyperaemic border | Neutrophil degradation; macrophages arrive |
| 7–10 days | Yellow-tan, soft centre | Macrophage phagocytosis of necrotic debris |
| 10–14 days | Red-grey margins | Granulation tissue + new capillaries |
| 2–8 weeks | Grey-white scar forming | Fibrosis progresses |
| >2 months | Dense white scar | Complete fibrous scar |
STEMI vs NSTEMI
| Feature | STEMI | NSTEMI |
|---|---|---|
| Mechanism | Complete occlusion | Partial occlusion or reperfusion |
| ECG | ST elevation + Q waves | ST depression / T-wave changes |
| Troponin | Markedly elevated | Elevated (lower) |
| Infarct type | Transmural | Subendocardial |
| Management | Immediate reperfusion (PCI/thrombolysis) | Medical ± PCI |
Cardiac Biomarkers
| Marker | Rises | Peaks | Returns to normal |
|---|---|---|---|
| Troponin I/T | 3–6 hrs | 24–48 hrs | 7–10 days |
| CK-MB | 3–6 hrs | 24 hrs | 48–72 hrs |
| Myoglobin | 1–3 hrs | 6–9 hrs | 24 hrs |
| LDH | 24–48 hrs | 3–6 days | 8–14 days |
HKMLE key: Troponin = most specific; Myoglobin = earliest to rise; CK-MB = best for re-infarction (returns to normal fastest → rise again indicates new event)
Clinical Features of MI
- Severe, crushing substernal chest pain — lasting hours (not relieved by nitrates or rest)
- Radiation to jaw, neck, left arm, epigastrium
- Diaphoresis, nausea, vomiting (especially posterior wall MI)
- Dyspnoea (LV dysfunction → pulmonary oedema)
- Rapid, weak pulse
- Silent MI in ~25%: especially in diabetics (autonomic neuropathy) and elderly
- With >40% LV loss → cardiogenic shock
6. REPERFUSION INJURY
When blood flow is restored after ischaemia, additional injury occurs:
- Free radical generation (O₂⁻, H₂O₂, •OH, peroxynitrite) within minutes → membrane damage
- Calcium overload → contraction band necrosis (intense eosinophilic bands = hypercontracted sarcomeres; diagnostic of reperfusion)
- Leukocyte aggregation → "no-reflow" phenomenon (microvascular occlusion)
- Platelet + complement activation → endothelial swelling + inflammation
Morphological hallmark of reperfusion injury: Contraction band necrosis (vs. coagulative necrosis in non-reperfused MI)
7. COMPLICATIONS OF MI
| Complication | Timing | Mechanism |
|---|---|---|
| Arrhythmias (VF, VT) | Hours–days | Ischaemia of conduction tissue |
| LV failure / Pulmonary oedema | Hours–days | Loss of contractile mass |
| Cardiogenic shock | Hours–days | >40% LV involvement |
| Pericarditis (Dressler's syndrome) | 1–8 weeks | Autoimmune (anti-myocardial Abs) |
| Papillary muscle rupture | 3–5 days | Necrosis → acute mitral regurgitation |
| Ventricular free wall rupture | 3–7 days | Necrosis → haemopericardium/tamponade |
| IV septal rupture | 3–7 days | Necrosis → VSD + sudden L→R shunt |
| Mural thrombus | Days–weeks | Stasis over infarcted endocardium → embolism |
| LV aneurysm | Weeks–months | Paradoxical bulge, refractory heart failure |
| Sudden cardiac death | Any time | VF |
Papillary muscle most at risk: Posteromedial papillary (single blood supply from RCA/LCx) vs anterolateral (dual supply from LAD + LCx)
8. INVESTIGATIONS
ECG Changes
- Hyperacute T waves → ST elevation → Q waves (transmural necrosis) → T-wave inversion
- LBBB (new onset) = STEMI equivalent
Imaging
- Echo: Wall motion abnormalities, EF, complications (MR, VSD, effusion)
- Stress testing (TMT / stress echo / stress nuclear): For stable angina workup
- Coronary CT Angiography (CCTA): Intermediate pre-test probability, young (<65 yrs)
- Agatston score (calcium scoring) — measures coronary calcification burden
- Invasive coronary angiography (ICA): Gold standard for stenosis; guides revascularisation
- Note: Does NOT image arterial wall → can miss non-stenotic plaques
9. MANAGEMENT SUMMARY
Stable Angina
- Lifestyle: Smoking cessation, weight loss, exercise, diet
- Antiplatelet: Aspirin 75–100 mg OD (or clopidogrel if intolerant)
- Antianginals: Beta-blockers (1st line), nitrates (sublingual for acute; long-acting for prophylaxis), CCBs (especially amlodipine), ivabradine (rate control if BB contraindicated)
- Statins: All patients (plaque stabilisation + lipid lowering)
- ACE inhibitors: If diabetes, LV dysfunction, hypertension
- Revascularisation (PCI/CABG): If refractory to medical therapy or high-risk anatomy
- ISCHEMIA trial: Revascularisation ≠ reduced MI/death vs medical therapy in stable IHD with EF >35%; but better angina relief
ACS / STEMI / NSTEMI
- MONA (mnemonic for acute): Morphine (pain), Oxygen (if SpO₂ <94%), Nitrates, Aspirin
- Dual antiplatelet: Aspirin + P2Y12 inhibitor (ticagrelor preferred > clopidogrel)
- Anticoagulation: LMWH (enoxaparin) or UFH
- STEMI: Primary PCI within 90 min (door-to-balloon) — gold standard; thrombolysis if PCI unavailable within 120 min
- NSTEMI: PCI within 24–72 hrs based on risk score (GRACE, TIMI)
- Beta-blockers: Start within 24 hrs if no cardiogenic shock
- ACE inhibitor/ARB: Start within 24 hrs, especially anterior MI / reduced EF
- Statin: High-intensity (atorvastatin 80 mg or rosuvastatin 40 mg)
10. HKMLE HIGH-YIELD POINTS ⭐
| Topic | Key Fact |
|---|---|
| Most common cause of IHD | Atherosclerosis (>90%) |
| Most common cause of MI | Plaque rupture + acute thrombosis |
| Most common cause of death before hospitalisation | Ventricular fibrillation |
| Most specific marker for MI | Troponin I/T |
| Earliest marker | Myoglobin |
| Best for re-infarction | CK-MB |
| Silent MI most common in | Diabetics (autonomic neuropathy) + elderly |
| Reperfusion injury hallmark | Contraction band necrosis |
| Free wall rupture timing | 3–7 days post-MI (most dangerous week) |
| Dressler's syndrome | Weeks post-MI, autoimmune pericarditis |
| Prinzmetal angina ECG | ST elevation at rest (not depression) |
| Levine's sign | Clenched fist over sternum (typical angina descriptor) |
| CCS Class IV | Angina at rest |
| LAD occlusion | Anterior + septal infarct (V1–V4) |
| RCA occlusion | Inferior infarct + SA/AV node involvement (heart block risk) |
| ISCHEMIA trial finding | PCI ≠ mortality benefit over medical therapy in stable IHD with EF >35% |
| Posteromedial papillary rupture | Single blood supply → more vulnerable to necrosis |
| No-reflow phenomenon | Microvascular occlusion by leukocytes after reperfusion |
| Most common complication in first hour | Arrhythmia (VF/VT) |
| Cardiogenic shock threshold | >40% LV myocardium infarcted |
Sources: Robbins & Kumar Basic Pathology (9e), Harrison's Principles of Internal Medicine (22e, 2025), Braunwald's Heart Disease (11e)
This is a shared conversation. Sign in to Orris to start your own chat.