Treatment of chalazion
Reading File
Finding Sources
Searching PubMed
chalazion treatment management
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
Here is a comprehensive, textbook-based overview of chalazion treatment:
Treatment of Chalazion
A chalazion is a sterile chronic lipogranuloma of a meibomian (or occasionally Zeis) gland caused by retained sebaceous secretions. It differs from a hordeolum, which is an acute bacterial infection. At least one-third of chalazia resolve spontaneously, so observation is appropriate for early or improving lesions.
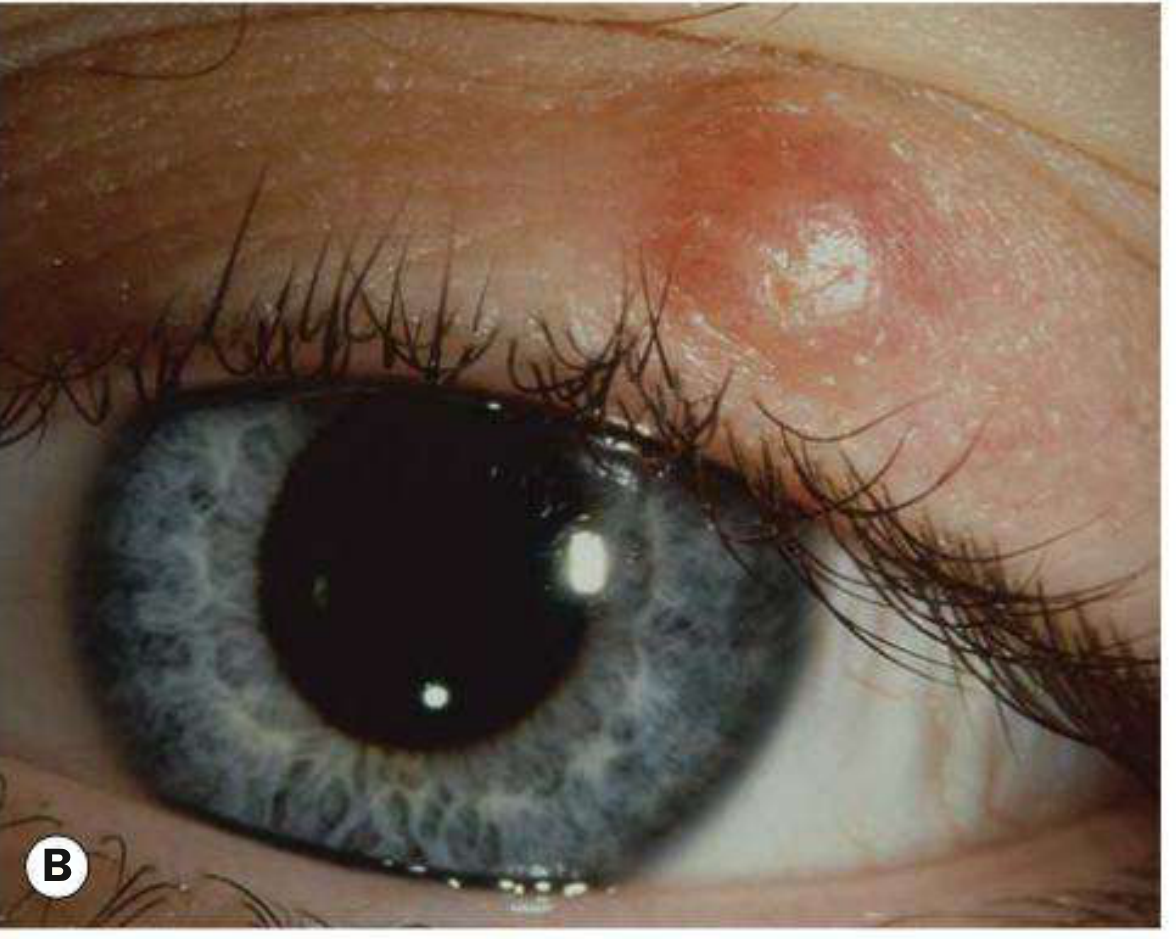
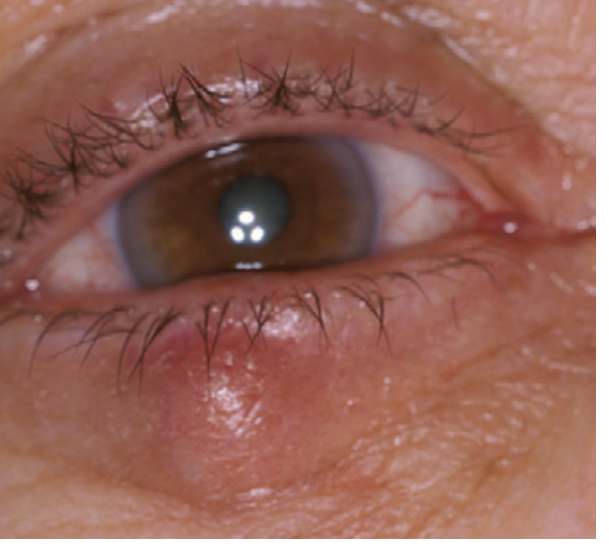
1. Conservative (Medical) Management
| Measure | Details |
|---|---|
| Warm compresses | At least 10 minutes, 4× daily; promotes drainage of inspissated secretions. Most useful in early lesions. |
| Eyelid hygiene/scrubs | Lid margin scrubs at the lash base nightly with diluted baby shampoo or commercial ocular cleansing pads. |
| Expression | Compression between two cotton-tipped applicators can express contents of a fresh, marginal lesion. |
| Topical antibiotics | Erythromycin, bacitracin, or tobramycin ointment b.i.d. for 1–2 weeks (more relevant when secondary infection/hordeolum is also present). |
| Topical antibiotic-steroid | Neomycin/polymyxin B/dexamethasone ointment b.i.d. for up to 1–2 weeks; monitor IOP if using steroid drops. |
| Oral doxycycline | Low-dose 20–50 mg p.o. daily or b.i.d. for its anti-inflammatory and antibacterial properties; especially useful for multiple/recurrent chalazia or associated ocular rosacea. |
Note: Oral antibiotics (e.g., doxycycline) are required only for significant bacterial superinfection, not for the sterile granuloma itself.
2. Intralesional Corticosteroid Injection
Used when conservative treatment fails (typically after 3–4 weeks) or as an alternative to surgery, especially for marginal lesions or those near the lacrimal punctum.
- Agent: Triamcinolone acetonide 40 mg/mL — inject 0.2–1.0 mL (mixed 1:1 with 2% lidocaine with epinephrine) via a 27- or 30-gauge needle through the conjunctival surface
- Alternative formulations: betamethasone sodium phosphate/acetate 6 mg/mL or dexamethasone sodium phosphate 4 mg/mL
- Success rate: ~80% after a single injection; a second injection can be given 1–2 weeks later
- Complications:
- Skin depigmentation and fat atrophy — less likely with the conjunctival approach; caution in dark-skinned individuals
- Rare: retrograde intra-arterial infiltration → central retinal artery occlusion
3. Surgical: Incision and Curettage (I&C)
Indicated when medical therapy fails and the patient desires removal.
Indications for excision:
- Unresponsive to medical management after 3–4 weeks
- Large, palpable lesion
- Cosmetic concern
- Visual disturbance (e.g., astigmatism from eyelid pressure)
Contraindications (relative):
- Chalazion that has recently drained or has very thin overlying skin (risk of full-thickness "buttonhole" defect)
- Markedly inflamed or crusted skin
- Anticoagulated patient
- Chalazion near the lacrimal punctum (refer to ophthalmology)
Technique:
- Local anaesthetic infiltration
- Eyelid everted with a specialized chalazion clamp
- Vertical incision through the tarsal plate on the conjunctival surface
- Contents curetted; solid inflammatory material excised with fine scissors and sent for histopathology
- No suture needed
- Topical antibiotic 3× daily for 5 days post-procedure
4. Recurrent Chalazia — Special Considerations
- Recurrence at the same lid position, particularly in older patients, mandates biopsy to exclude sebaceous carcinoma
- Systemic tetracycline as long-term prophylaxis in patients with recurrent chalazia, especially if associated with acne rosacea
- Blepharitis treatment (daily lid hygiene) is essential to prevent recurrence
- Note: Bortezomib (proteasome inhibitor for multiple myeloma) predisposes to chalazion within 3 months of initiation
Treatment Algorithm
Chalazion diagnosed
↓
Warm compresses + lid hygiene (4–6 weeks)
↓ (if persistent)
Intralesional triamcinolone injection
(preferred for marginal lesions / near punctum)
↓ (if fails after 1–2 injections)
Incision and curettage (I&C) via conjunctival approach
↓
Send specimen for histopathology
(mandatory for recurrent/atypical lesions)
Sources:
- Kanski's Clinical Ophthalmology: A Systematic Approach, 10th ed., pp. 54–55
- The Wills Eye Manual, 8th ed., pp. 381–383
- Pfenninger & Fowler's Procedures for Primary Care, 3rd ed., p. 456
- Rosen's Emergency Medicine, p. 893
Can I use ciplox eye drop
Finding Sources
Searching the Web
ciprofloxacin eye drops chalazion treatment evidence
Ciplox (ciprofloxacin 0.3%) eye drops — the short answer is: not routinely recommended for chalazion, and here's why:
Why Ciplox Is Generally Not Useful for Chalazion
Chalazion is a sterile lipogranuloma — it is not caused by bacterial infection. It results from blockage of a meibomian gland with retained secretions triggering a chronic granulomatous inflammatory reaction. Since there is no active infection, an antibiotic has no direct therapeutic role in the chalazion itself.
Ciprofloxacin eye drops also have poor tissue penetration into the eyelid stroma and tarsal plate — even if infection were present, drops do not reach adequate concentrations there.
When Antibiotics Are Relevant
| Situation | Appropriate antibiotic |
|---|---|
| Secondary bacterial infection / hordeolum | Erythromycin, bacitracin, or tobramycin ointment (not drops) — ointments adhere to the lid margin and penetrate better |
| Associated blepharitis with bacterial overgrowth | Topical ointment ± oral doxycycline |
| Preseptal cellulitis developing from a chalazion | Systemic antibiotics |
Ointment formulations are consistently preferred over drops for eyelid margin infections because drops run off quickly and don't maintain contact with the lid margin.
What Actually Works for Chalazion
Refer to the treatment hierarchy from the previous answer:
- Warm compresses + lid hygiene — first-line
- Topical antibiotic-steroid ointment (e.g., neomycin/polymyxin B/dexamethasone) — if inflammation is prominent
- Intralesional triamcinolone injection — if conservative therapy fails
- Incision and curettage — definitive if all else fails
Bottom line: Ciplox eye drops have no established role in chalazion treatment. If there is associated active infection (hordeolum/blepharitis), use an antibiotic ointment (erythromycin or tobramycin) rather than drops. For the chalazion itself, warm compresses and, if needed, steroid injection or surgery are the appropriate treatments.
What of acute conjuctivitis
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Now, regarding Ciplox (ciprofloxacin 0.3%) for acute conjunctivitis — the answer is yes, it can be used, but the appropriateness depends on the type.
Acute Conjunctivitis — Treatment & Role of Ciplox
Types at a Glance
| Feature | Bacterial | Viral | Allergic |
|---|---|---|---|
| Discharge | Mucopurulent, thick | Watery/serous | Watery |
| Onset | Unilateral → bilateral | Unilateral → bilateral | Bilateral |
| Itch | Mild | Mild–moderate | Prominent |
| Preauricular node | Absent | Present | Absent |
| Lid sticking on waking | Yes | Yes (mild) | No |
| Self-limiting | Yes (~60% in 5 days) | Yes (2–3 weeks) | Yes (if allergen removed) |
1. Bacterial Conjunctivitis
Ciplox (ciprofloxacin 0.3%) — YES, it is appropriate.
Ciprofloxacin is explicitly listed among first-line topical antibiotics for bacterial conjunctivitis alongside chloramphenicol, gentamicin, tobramycin, ofloxacin, moxifloxacin, erythromycin, azithromycin, and fusidic acid.
Standard regimen: 1–2 drops, 4× daily for up to 7 days.
⚠️ Key points:
- ~60% resolve spontaneously within 5 days without treatment; antibiotics mainly speed recovery and reduce transmission
- Ointments provide higher, longer-lasting concentrations than drops but cause blur — best used at night
- No single antibiotic is proven superior to others for routine bacterial conjunctivitis
- Contact lenses must be stopped until 48 hours after full resolution
Gonococcal/meningococcal conjunctivitis (hyperacute purulent discharge): Ciprofloxacin drops 1–2 hourly PLUS urgent systemic therapy (ceftriaxone IM/IV). This is an emergency — refer immediately.
Common causative organisms:
- S. pneumoniae, S. aureus, H. influenzae, Moraxella catarrhalis
- Severe/STI-related: N. gonorrhoeae, N. meningitidis, Chlamydia
2. Viral Conjunctivitis
Ciplox — NOT indicated. This is the most common type (usually adenovirus).
Treatment is supportive:
- Preservative-free artificial tears 4–8× daily for 1–3 weeks
- Cool compresses several times daily
- Antihistamine drops (e.g., epinastine 0.05% b.i.d.) if itching is severe
- Counsel: contagious for 10–12 days; avoid hand shaking, towel sharing, school/work with close contact
- If membrane/pseudomembrane present: gentle peeling + topical steroid (loteprednol 0.5% or prednisolone acetate 1% q.i.d.)
- If subepithelial infiltrates (SEIs) reduce vision: weaker steroid (loteprednol 0.2% b.i.d.) — taper slowly to avoid rebound
Antibiotics including Ciplox add no benefit and should not be routinely used.
3. Allergic Conjunctivitis
Ciplox — NOT indicated.
Treatment:
- Remove inciting allergen; cool compresses
- Mild: Artificial tears 4–8× daily
- Moderate: Dual-action antihistamine/mast-cell stabilizer drops — olopatadine 0.1–0.2%, azelastine 0.05%, bepotastine 1.5%, ketotifen 0.025%
- Severe: Add mild topical steroid (loteprednol 0.2% or fluorometholone 0.1% q.i.d.) for 1–2 weeks
- Oral antihistamine (loratadine 10 mg daily or diphenhydramine 25 mg t.i.d.) for moderate–severe cases
Routine topical antibiotics or steroids are not recommended for uncomplicated allergic conjunctivitis.
Summary: When to Use Ciplox in Conjunctivitis
| Scenario | Ciplox appropriate? |
|---|---|
| Bacterial conjunctivitis (routine) | ✅ Yes — 1–2 drops q.i.d. × 7 days |
| Gonococcal/meningococcal | ✅ Yes — 1–2 hourly + systemic antibiotics (emergency) |
| Viral conjunctivitis | ❌ No |
| Allergic conjunctivitis | ❌ No |
| Chalazion (from previous question) | ❌ No (sterile lesion) |
Sources:
- Kanski's Clinical Ophthalmology, 10th ed., pp. 188–189
- The Wills Eye Manual, 8th ed., pp. 306–313
This is a shared conversation. Sign in to Orris to start your own chat.