Explain female reproductive system first year anatomy
Reading File
Finding Sources
Finding Sources
Searching Images
female reproductive system anatomy diagram
Reading File
Finding Sources
Loading Image
Reading File
Loading Image
Finding Sources
Reading File
Finding Sources
Reading File
Reading File
Reading File
Loading Image
I now have comprehensive material from multiple authoritative textbooks. Let me compile the full answer.
Female Reproductive System — First Year Anatomy
Overview
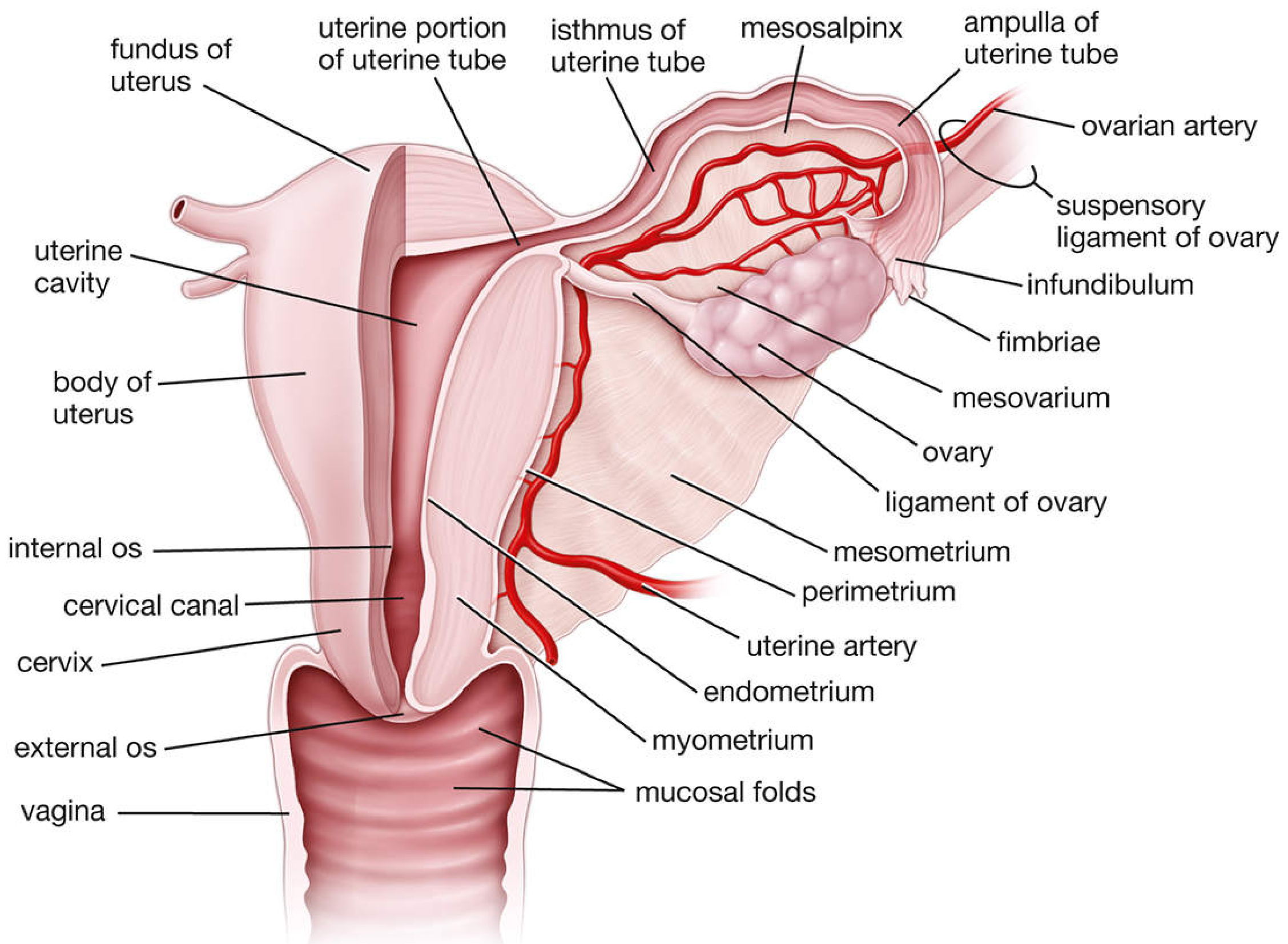
The female reproductive system is divided into internal organs and external genitalia (vulva). The internal organs lie within the pelvis: the ovaries, uterine (fallopian) tubes, uterus, and vagina. They undergo regular cyclical structural and functional changes from puberty (menarche, mean age 12.4 years) to menopause (mean age 51.4 years). — Histology: A Text and Atlas, Gartner
1. Ovaries
Location & Structure
- Paired, almond-shaped organs (~3 × 1.5 × 1 cm) located on the posterior surface of the broad ligament in the lateral pelvic wall
- Attached to the broad ligament by the mesovarium, to the uterus by the ovarian (utero-ovarian) ligament, and to the pelvic sidewall by the suspensory (infundibulopelvic) ligament (which carries the ovarian vessels and lymphatics)
- Covered by germinal epithelium (simple cuboidal) overlying a dense connective tissue capsule: the tunica albuginea
Internal Zones
| Zone | Contents |
|---|---|
| Cortex (outer) | Ovarian follicles at all stages of development embedded in stroma |
| Medulla (inner) | Loose connective tissue, nerves, blood and lymphatic vessels |
Functions
- Gametogenesis (oogenesis) — production of secondary oocytes
- Steroidogenesis — secretion of estrogens (promote maturation of sex organs, secondary sexual characteristics) and progestogens (prepare uterus for pregnancy)
Blood supply: Ovarian arteries (direct branches of the abdominal aorta at L1). Right ovarian vein drains to IVC; left ovarian vein drains to left renal vein.
2. Ovarian Follicles (Key First-Year Concept)
| Stage | Features |
|---|---|
| Primordial follicle | Single primary oocyte arrested in prophase I, surrounded by one layer of squamous follicle cells |
| Primary follicle | Follicle cells become cuboidal; zona pellucida forms (ZP glycoproteins) |
| Secondary (antral) follicle | Multiple layers of granulosa cells; fluid-filled antrum develops; theca interna/externa differentiate |
| Mature (Graafian) follicle | Large antrum; LH surge triggers resumption of meiosis I → secondary oocyte |
At ovulation, the secondary oocyte (arrested at metaphase II) is released. Remaining follicular cells luteinize to form the corpus luteum, which secretes progesterone. If unfertilized, it regresses to the corpus albicans. — Histology: A Text and Atlas, Gartner
3. Uterine (Fallopian) Tubes
Anatomy
- ~10 cm long; extend laterally from the uterine cornua
- Four parts (lateral → medial): Infundibulum → Ampulla → Isthmus → Intramural (uterine) portion
| Part | Feature |
|---|---|
| Infundibulum | Funnel-shaped opening with finger-like fimbriae that sweep the oocyte in at ovulation |
| Ampulla | Widest and longest portion; site of fertilization |
| Isthmus | Narrow, thick-walled segment adjacent to uterus |
| Intramural | Passes through uterine wall |
The tube is supported by the mesosalpinx (part of the broad ligament). Its lining is ciliated columnar epithelium that propels the oocyte/embryo toward the uterus.
4. Uterus
Position & Shape
- Pear-shaped, hollow muscular organ; normally anteverted and anteflexed in the pelvis
- Lies between the bladder (anterior) and rectum (posterior)
Parts
| Region | Description |
|---|---|
| Fundus | Dome-shaped part above the uterine tube openings |
| Body (corpus) | Main portion |
| Isthmus | Junction between body and cervix (becomes the lower uterine segment in pregnancy) |
| Cervix | Lower cylindrical part; ~3 cm long |
Uterine Wall — Three Layers
- Endometrium (inner) — mucosa; cyclically shed during menstruation; has functional and basal layers
- Myometrium (middle, thickest) — smooth muscle arranged in three poorly defined layers; responsible for contractions of labor
- Perimetrium (outer) — peritoneal (serosal) covering
Ligaments Supporting the Uterus
| Ligament | Attachment & Function |
|---|---|
| Broad ligament | Peritoneal fold; contains mesometrium, mesosalpinx, mesovarium |
| Round ligament | Fundus → inguinal canal → labia majora; maintains anteversion |
| Cardinal (transverse cervical) ligament | Cervix → lateral pelvic wall; main support against prolapse |
| Uterosacral ligament | Cervix → sacrum; maintains anteflexion |
Blood supply: Uterine artery (branch of internal iliac artery); anastomoses with ovarian artery at the cornua.
5. Cervix
- Narrow, fibrous distal part of uterus; visualized at the top of the vaginal canal
- Central canal = os (internal os opens into uterine cavity; external os opens into vagina)
- Ectocervix: stratified squamous epithelium
- Endocervix (cervical canal): mucus-secreting columnar epithelium
- Transformation zone: squamocolumnar junction — the clinically important site where cervical intraepithelial neoplasia (CIN) arises — Sabiston Textbook of Surgery
6. Vagina
- Fibromuscular tube extending from cervix to vestibule; lies mostly horizontal in the upright posture
- Wall layers (inside → out): stratified squamous nonkeratinized epithelium → lamina propria (collagen, elastic tissue) → muscular layer → areolar connective tissue
- No glands; lubrication comes from cervical mucus and transudate
- Blood supply: Vaginal artery (branch of internal iliac); multiple anastomoses with uterine, internal pudendal, inferior vesical, and middle rectal arteries
- Nerve supply: Lumbosacral plexus (S2–S4) → pudendal nerve; most sensory innervation is in the distal third — Sabiston Textbook of Surgery
7. External Genitalia (Vulva)
| Structure | Description |
|---|---|
| Mons pubis | Rounded fat pad over pubic symphysis |
| Labia majora | Longitudinal skin folds with adipose tissue, sebaceous and sweat glands |
| Labia minora | Inner folds; connective tissue core; rich sebaceous glands but no fat |
| Clitoris | Erectile organ homologous to penis; composed of glans, body, crura, and vestibular bulbs |
| Vestibule | Space between labia minora; contains vaginal orifice, external urethral orifice, and openings of Bartholin's glands |
| Hymen | Mucosal fold partially covering vaginal orifice |
8. Pelvic Blood Supply Summary
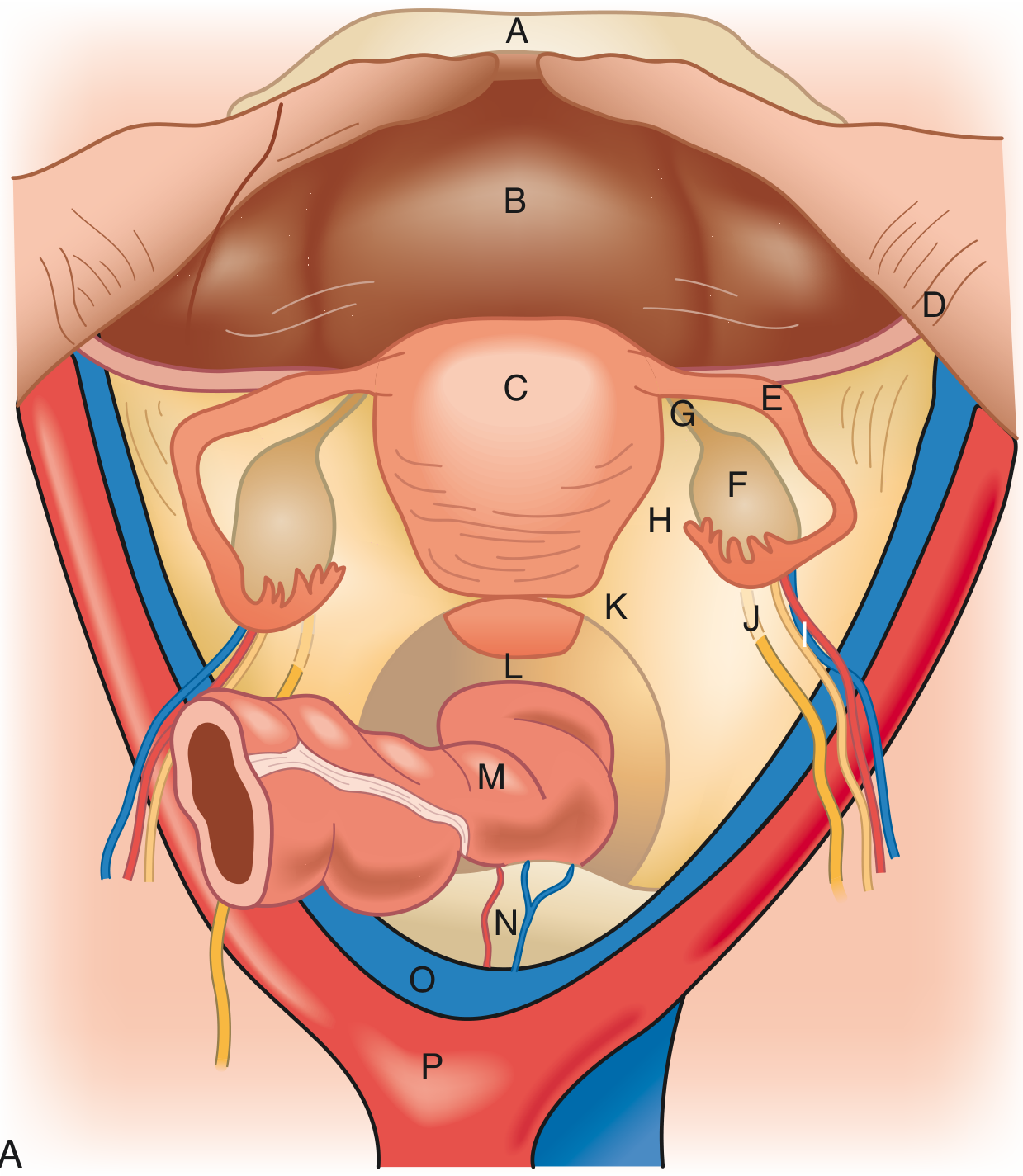
- Common iliac artery → bifurcates at sacral promontory into external and internal iliac arteries
- Internal iliac (hypogastric) artery → anterior division → uterine artery, vaginal artery, superior/inferior vesical arteries, middle rectal artery, obturator artery, pudendal artery
- Ovarian arteries arise directly from the aorta (L1) — Sabiston Textbook of Surgery
9. Innervation
The lumbosacral plexus (T12–S4) provides major nerve supply:
- Obturator nerve (L2–L4): medial thigh
- Femoral nerve (L2–L4): anterior thigh
- Sciatic nerve (L4–S3): posterior thigh and leg
- Pudendal nerve (S2–S4): perineum and external genitalia
- Sympathetic supply regulates uterine and vascular tone; parasympathetic (S2–S4) mediates vasodilation and secretion
Quick Memory Summary
Ovary → Uterine tube (infundibulum–ampulla–isthmus–intramural)
→ Uterus (fundus–body–isthmus–cervix)
→ Vagina → Vestibule (vulva)
Uterine wall: Endometrium / Myometrium / Perimetrium
Ovarian follicle stages: Primordial → Primary → Secondary → Graafian
Fertilization site: Ampulla of uterine tube
Implantation site: Posterior wall of uterine body (endometrium)
Main support ligament: Cardinal ligament (prevents prolapse)
Sources: Histology: A Text and Atlas with Correlated Cell and Molecular Biology (Gartner); Sabiston Textbook of Surgery, 21e
This is a shared conversation. Sign in to Orris to start your own chat.