Plz explain me the concept of purkinje images
Of eyeball at cornea and lens
Reading File
Finding Sources
Searching Images
Purkinje images cornea lens eye reflex
Finding Sources
Finding Sources
Loading Image
Finding Sources
Finding Sources
Finding Sources
Loading Image
Reading File
The Guyton textbook covers general optics of the eye but doesn't specifically mention Purkinje images. I have enough knowledge to give a comprehensive answer on this topic from the library content and well-established optics principles. Let me now compile the full explanation.
Purkinje Images (Purkinje–Sanson Images)
Purkinje images — also called Purkinje–Sanson images or catoptric images — are the reflections of light produced by the four polished surfaces of the optical media of the eye. When a point source of light is held in front of the eye, it produces four distinct reflections, each arising from a different refracting surface. These are purely reflected images (not refracted), formed because every optically smooth curved surface acts as a convex or concave mirror.
The Four Surfaces and Their Images
| Image | Surface | Mirror type | Character |
|---|---|---|---|
| Purkinje I | Anterior surface of cornea | Convex mirror | Erect, virtual, bright, small |
| Purkinje II | Posterior surface of cornea | Convex mirror | Erect, virtual, dimmer (cornea partially absorbs/transmits) |
| Purkinje III | Anterior surface of lens | Convex mirror | Erect, virtual, large, dim |
| Purkinje IV | Posterior surface of lens | Concave mirror | Inverted, real, small, dim |
Memory key: Only Purkinje IV is inverted because the posterior lens surface is concave.
Physical Basis
Each smooth, curved surface of the eye acts as a spherical mirror:
- A convex surface (cornea anterior/posterior, lens anterior) produces an erect, virtual, diminished reflection.
- A concave surface (lens posterior) produces an inverted, real reflection.
The brightness of each image depends on how much light is reflected. The anterior corneal surface (Purkinje I) reflects the most (~4% of incident light) and is thus the brightest and most easily observed. The images from the posterior surfaces are progressively dimmer.
Characteristics at Each Surface
Purkinje Image I — Anterior Cornea
- Brightest of all four
- Erect (upright), virtual image
- Located just behind the corneal surface
- Commonly used clinically in the Hirschberg corneal reflex test (assessing squint/strabismus)
- Used in corneal topography and videokeratoscopy
Purkinje Image II — Posterior Cornea
- Erect, virtual
- Very close to Image I and much dimmer
- Rarely used clinically due to difficulty distinguishing it from Image I
Purkinje Image III — Anterior Lens
- Erect, virtual, largest of the four
- Noticeably large because the anterior lens surface has a large radius of curvature (~10 mm)
- Moves in the same direction as the light source, like Images I and II
Purkinje Image IV — Posterior Lens
- Inverted (the only inverted image)
- Real image
- Smallest and dimmest
- Moves in the opposite direction to Images I–III when a light source is moved
- Its disappearance/change is used in the Purkinje shift test for accommodation studies
Behavior During Accommodation
This is a key clinical use of Purkinje images. When the eye accommodates (focuses on a near object):
| Event | Effect on Image III | Effect on Image IV |
|---|---|---|
| Ciliary muscle contracts | Anterior lens surface steepens (radius ↓) | Posterior lens surface changes slightly |
| Image III | Becomes smaller and moves backward (lens bulges forward) | Becomes larger but remains inverted |
This was used historically by Helmholtz to confirm that accommodation occurs by change in the anterior lens curvature, not by movement of the whole lens.
Clinical Applications
-
Strabismus assessment (Hirschberg test): A penlight is shone at the eyes; the corneal light reflex (Purkinje I) position relative to the pupil center helps estimate the angle of squint.
-
Keratometry and corneal topography: Instruments (Placido disc, keratometers) rely on the size and shape of Purkinje Image I reflections to measure corneal curvature and detect astigmatism.
-
Lens opacity detection (cataract): Distortion or absence of Images III and IV suggests lens opacification.
-
Accommodation studies: Comparison of Image III size before and after accommodation (Scheiner's method, Helmholtz purkinjescope).
-
Intraocular lens (IOL) placement: Scheimpflug cameras use Purkinje reflections to assess anterior segment geometry.
-
Gaze tracking: Many modern eye-tracking devices use the pupil center and Purkinje I reflection to calculate gaze direction.
Diagram — Clinical Photo
Below is an actual clinical photograph showing multiple Purkinje reflections on the corneal surface, used in corneal biometry:
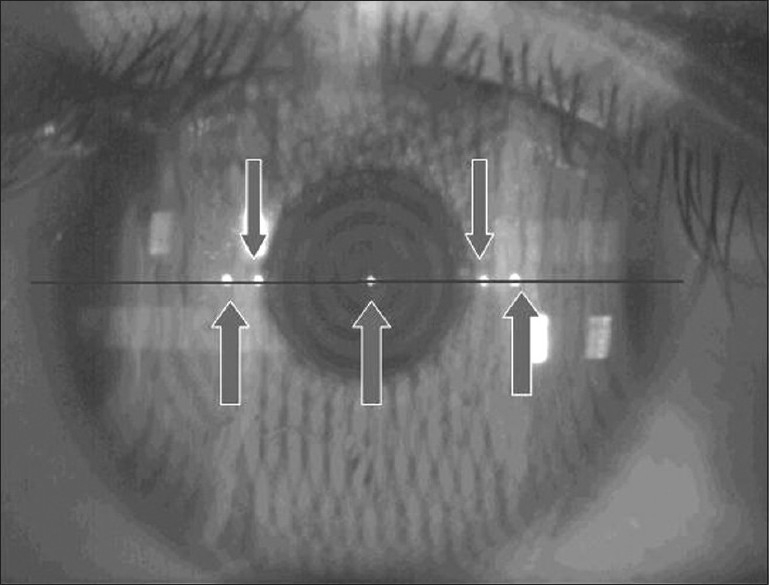
And here is a slit-lamp view showing small Purkinje catoptric reflections visible to the right of the pupillary area:

Summary Table
| Feature | Image I | Image II | Image III | Image IV |
|---|---|---|---|---|
| Surface | Ant. cornea | Post. cornea | Ant. lens | Post. lens |
| Mirror type | Convex | Convex | Convex | Concave |
| Orientation | Erect | Erect | Erect | Inverted |
| Brightness | Brightest | Dim | Dim | Dimmest |
| Size | Small | Smallest | Largest | Small |
| Clinical use | Hirschberg, keratometry | Rarely used | Accommodation studies | Accommodation, gaze tracking |
— Guyton and Hall Textbook of Medical Physiology, Optics of the Eye chapter
Can you explain me this
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
I have all the content needed. Let me now give you a thorough explanation of everything in that image.
Your Notes Explained: Gullstrand's Schematic Eye & Listing's Reduced Eye
1. Gullstrand's Schematic Eye
Allvar Gullstrand (Nobel Prize 1911) created a precise mathematical model of the eye by measuring all 6 optical surfaces and their exact positions, curvatures, and refractive indices. This is called the schematic eye — it's not a simplified model, but a detailed, anatomically accurate one.
The key insight: the eye has 4 refracting surfaces, and each one reflects light → producing the 4 Purkinje images (as you studied).
2. The Purkinje Surfaces Table (from your notes)
| Purkinje Image | Site | Power |
|---|---|---|
| I | Anterior Cornea | +48.8 D (maximum) |
| II | Posterior Cornea | −5.88 D |
| III | Anterior Lens | +19 D |
| IV | Posterior Lens | (not listed — smallest) |
Why these specific values?
Purkinje I — Anterior Cornea → +48.8 D (the biggest contributor)
This is the most powerful refracting surface in the entire eye. The reason:
- Air (refractive index = 1.00) meets cornea (refractive index = 1.376)
- This is the largest difference in refractive indices of any interface in the eye
- A highly curved surface + large RI difference = high refracting power
- This single surface contributes ~⅔ of the eye's total power
Purkinje II — Posterior Cornea → −5.88 D (negative!)
- The posterior cornea is in contact with aqueous humor (RI = 1.336), not air
- The refractive index decreases slightly going from cornea (1.376) to aqueous (1.336)
- This means light diverges slightly → negative power
- It partially cancels the anterior cornea's power
Purkinje III — Anterior Lens → +19 D
- Aqueous humor meets the crystalline lens
- The lens has a higher RI than aqueous, so light converges → positive power
- Lower than the cornea because the RI difference is smaller
- This is also the surface that changes most during accommodation (its curvature increases, power goes up to ~+33 D)
Purkinje IV — Posterior Lens
- Lens meets vitreous humor (RI 1.336, nearly same as aqueous)
- The RI difference is minimal → very small power contribution
- This is why it's the dimmest, least clinically significant Purkinje image
Net total power:
The combined total power of the eye ≈ +58–59 D (at rest, for distance vision)
+48.8 − 5.88 + 19 + small posterior lens contribution ≈ ~59 D ✓
3. Listing's Reduced Eye
Since having 4 surfaces is complex for calculations, Listing simplified the entire eye into a single refracting surface — the Reduced Eye.
Key rules:
- All elements are measured from the anterior corneal surface (the reference point)
- The single refracting surface is placed at the cornea
- Power of reduced eye = 58.6 D (close to 59 D)
Why measure from the anterior corneal surface?
Because it contributes the most power (+48.8 D) and is the first surface light hits — it's the most clinically accessible and measurable surface.
Principal Point (P) and Nodal Point (N):
From the diagram in your notes:
| Point | What it is | Location |
|---|---|---|
| Principal Point (P) | Where the single refracting surface is assumed to lie; the reference for measuring image/object distances | ~1.35 mm behind anterior cornea |
| Nodal Point (N) | A point through which any ray passes without changing direction; used for calculating retinal image size | ~7.08 mm behind anterior cornea (near the posterior lens) |
| Focal Point (F) | Where parallel rays from infinity converge on the retina | ~17 mm behind the principal point (= on the retina in an emmetropic eye) |
The diagram shows:
- F (left) = anterior focal point — where rays going to infinity diverge from
- P, N = principal and nodal points inside the eye (shown as a circle)
- F (right) = posterior focal point — falls on the retina in a normal eye
Factors Determining Power of the Eye:
Your notes list these as the next topic — they include:
- Curvature of cornea (flatter cornea → less power → hyperopia)
- Refractive indices of cornea, aqueous, lens, vitreous
- Axial length of the eye (longer eye → myopia)
- Power of the lens (controlled by accommodation)
Quick Summary
| Concept | Key Point |
|---|---|
| Gullstrand's Schematic Eye | Detailed model with 4 surfaces and real anatomical values |
| Anterior cornea (+48.8 D) | Biggest contributor; air-cornea RI difference is largest |
| Posterior cornea (−5.88 D) | Negative because cornea→aqueous causes slight divergence |
| Anterior lens (+19 D) | Second contributor; changes during accommodation |
| Listing's Reduced Eye | All 4 surfaces simplified into ONE surface at cornea; power = 58.6 D |
| Measured from... | Anterior corneal surface |
| Nodal point | Ray through it doesn't bend; used for retinal image size calculation |
— Guyton and Hall Textbook of Medical Physiology, Optics of the Eye, p. 623
This is a shared conversation. Sign in to Orris to start your own chat.