Cscr
Checking Date & Time
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
Loading Image
Searching PubMed
"central serous chorioretinopathy" treatment
Central Serous Chorioretinopathy (CSCR)
Overview
Central serous chorioretinopathy (CSCR, also abbreviated CSR) is an idiopathic disorder characterized by a localized serous detachment of the sensory retina at the macula, secondary to leakage from the choriocapillaris through one or more hyperpermeable RPE (retinal pigment epithelium) sites. It is classified within the pachychoroid spectrum of disorders — in eyes with unilateral CSCR, almost two-thirds of fellow eyes show signs of pachychoroid pigment epitheliopathy.
Epidemiology & Risk Factors
| Feature | Detail |
|---|---|
| Typical patient | Young to middle-aged White male |
| Sex ratio | Male:Female = 3:1; women tend to be older at presentation |
| Laterality | Usually unilateral, but can be bilateral |
Risk factors and associations:
- Corticosteroid use (any route — oral, inhaled, nasal spray, topical skin creams, endogenous Cushing syndrome) — strongly linked
- Type A personality / psychological stress
- Systemic hypertension
- Pregnancy (women)
- Lupus (SLE)
- Helicobacter pylori infection
- Renal dialysis
- Sleep apnoea syndrome
- A SNP in the complement factor H gene (chromosome 1) predisposes to the chronic form in White individuals
Presentation
Symptoms:
- Unilateral blurred or dim vision
- Metamorphopsia (distortion) and micropsia (objects appear smaller)
- Central scotoma
- Mild dyschromatopsia (faded colors)
- May be asymptomatic
Signs:
- VA typically 6/9–6/18 (20/30–20/60); improves with a low-strength convex/plus lens (acquired hypermetropia from retinal elevation)
- Round or oval serous detachment of the neurosensory retina at the macula — sloping margins that merge gradually into the attached retina
- Subretinal fluid (clear or turbid); precipitates may be on the posterior retinal surface
- One or more depigmented RPE foci or small PEDs within the detachment
- FAF imaging reveals RPE atrophy/hyperplasia from prior episodes; gravitational tract visible in chronic cases
Fundus Appearance
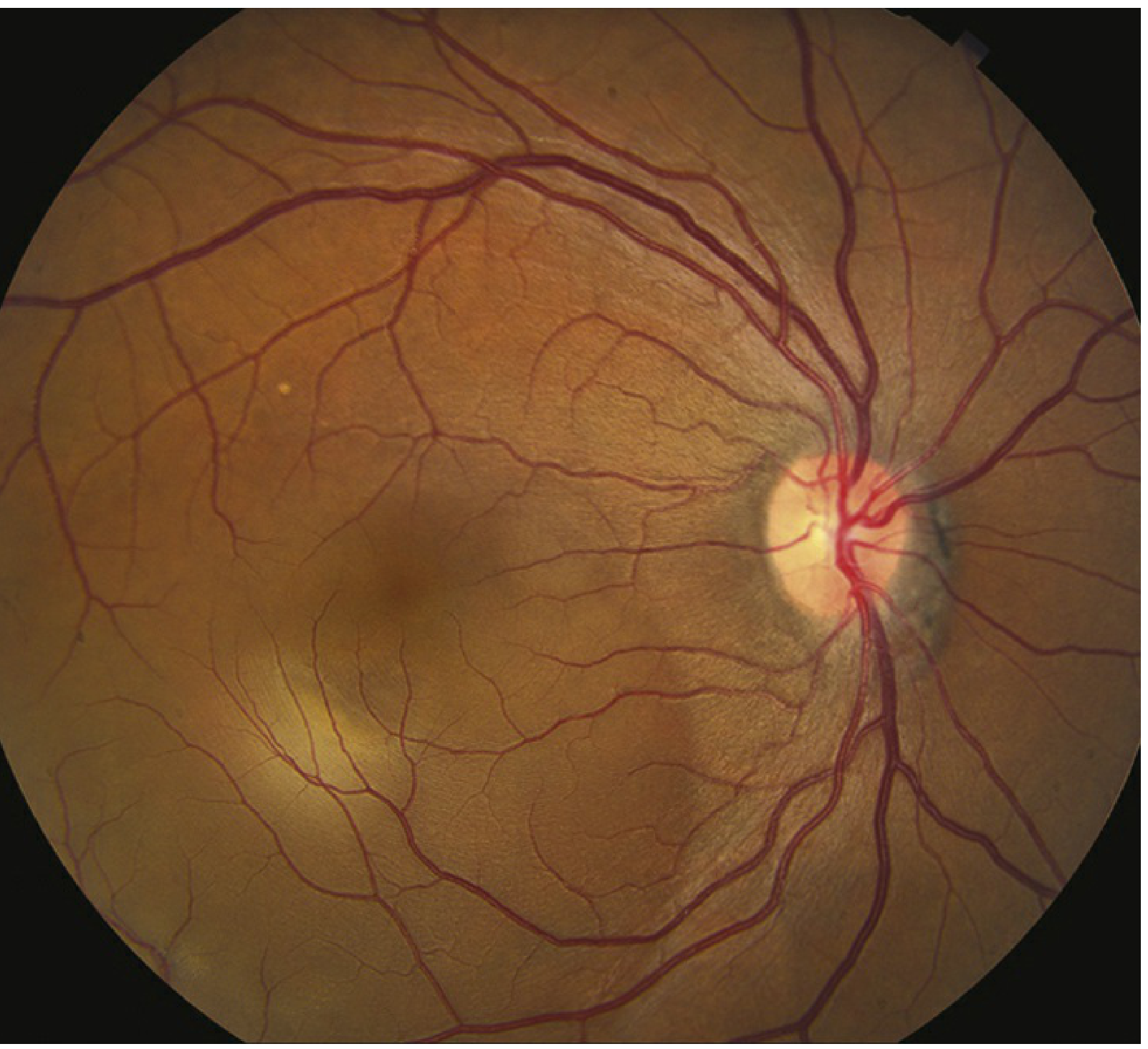
Investigations
- Amsler grid — documents area of field distortion
- Slit-lamp biomicroscopy — rule out concurrent CNV; examine optic disc for pit
- OCT (enhanced-depth imaging) — gold standard for demonstrating subretinal fluid, PEDs, and choroidal thickening (pachychoroid)
- IVFA (fluorescein angiography) — nearly pathognomonic "smoke-stack" pattern of dye leakage in 10–20% of cases; "ink blot" pattern in others
- ICGA (indocyanine green angiography) — choroidal artery/choriocapillaris filling delays; multifocal hyperfluorescent patches in early phase
- For chronic CSCR: systemic workup including cortisol levels and renal function
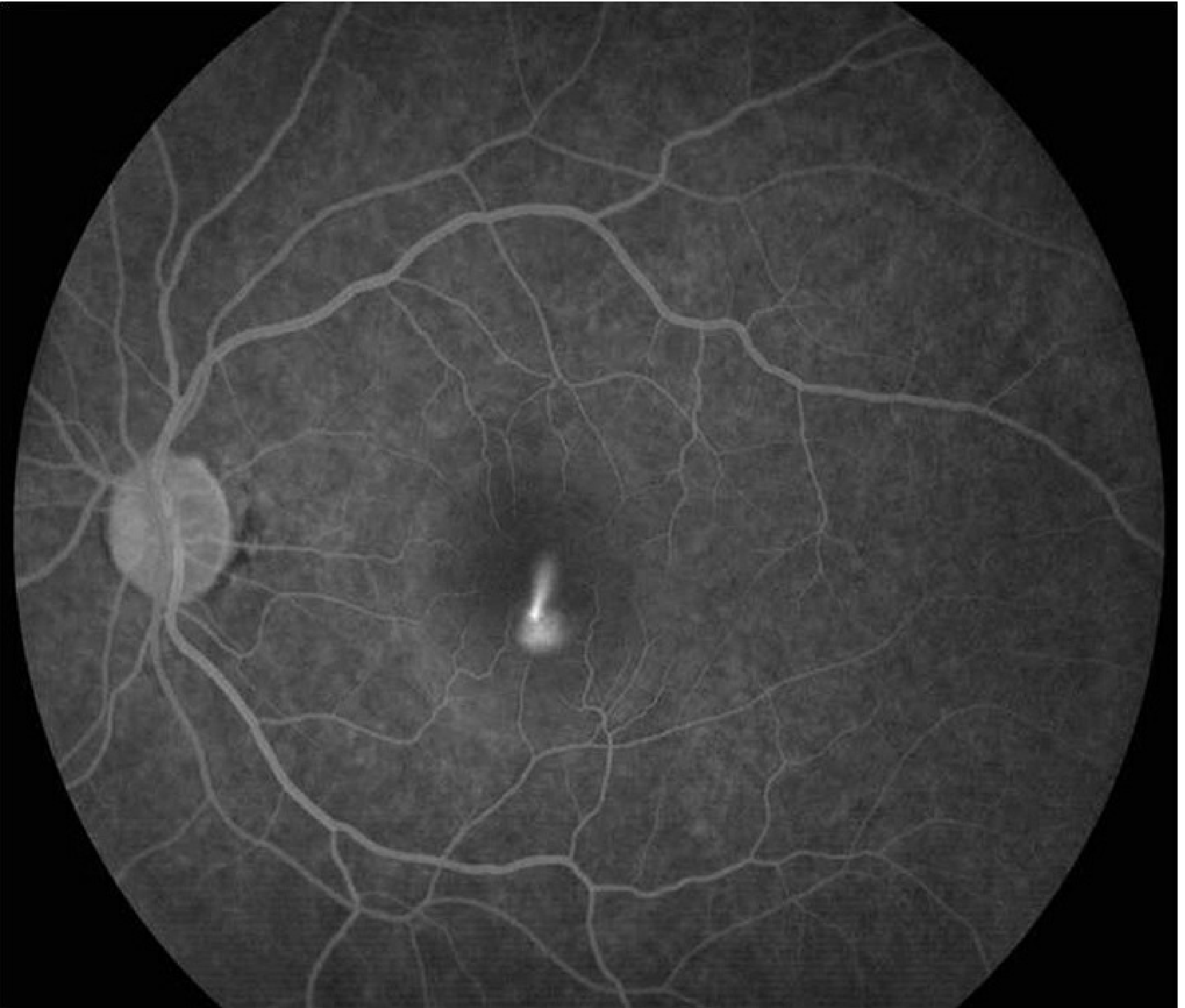
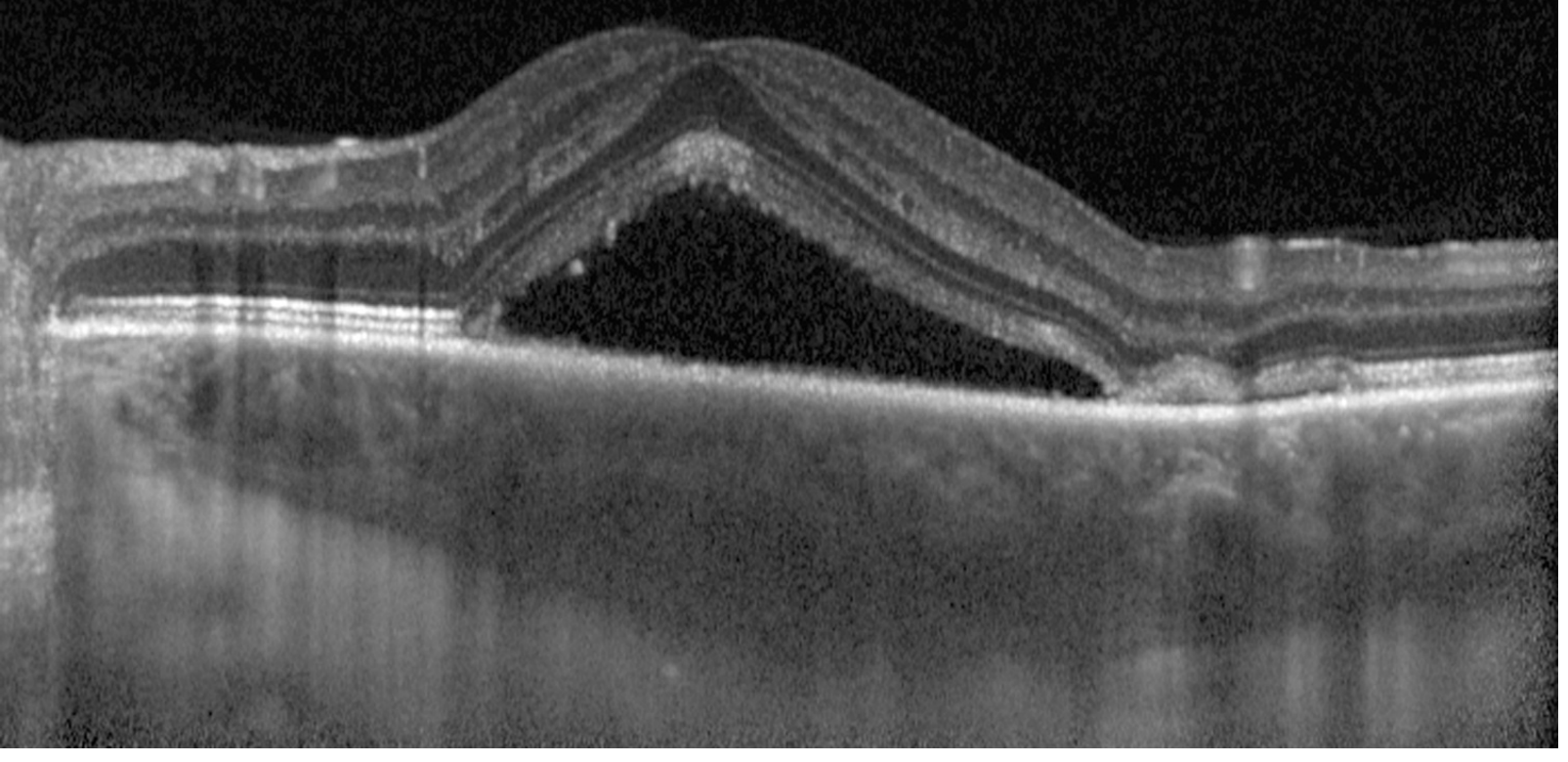
Course & Prognosis
| Form | Description |
|---|---|
| Acute | Self-resolving within 3–6 months; near-normal vision in ~80% |
| Recurrent | Up to 50% recurrence rate |
| Chronic | ~15% follow a course >12 months; associated with photoreceptor and RPE degeneration and permanently reduced vision |
Differential Diagnosis
- AMD — patient usually ≥50 years, drusen, often bilateral, may have CNV
- Optic pit — contiguous serous RD with the optic disc
- Rhegmatogenous retinal detachment / macular hole
- Choroidal tumor (hemangioma, melanoma)
- Hypertensive retinopathy
- PED — more distinct, elevated margins (may accompany CSCR or AMD)
- Uveal effusion syndrome, inflammatory choroidal disorders, chronic renal failure
Management
1. Observation
- First-line for acute CSCR — usually self-limited with good visual prognosis.
2. Stop Corticosteroids
- Discontinue all forms if possible (oral, topical, nasal, inhaled).
Key tip (Kanski): All forms of corticosteroid treatment should be discontinued in patients with chronic or recurrent CSCR.
3. Laser Photocoagulation
- May accelerate visual recovery but long-term benefit is unclear and may increase CNV risk.
- Consider when:
- Detachment persists for several months
- Recurrence with residual visual deficit
- Contralateral eye involvement after a prior episode
- Occupational necessity for prompt visual recovery
4. Photodynamic Therapy (PDT)
- Useful for chronic CSCR.
- Half-dose PDT may be considered for rapid SRF resolution in acute CSCR.
5. Mineralocorticoid Receptor Antagonists
- Eplerenone and spironolactone — associated with improved anatomic and visual outcomes in chronic CSCR.
- A 2025 meta-analysis (PMID: 40513762) specifically evaluated both agents for chronic CSCR.
6. Anti-VEGF Therapy
- If choroidal neovascularization (CNV) develops as a complication.
Sources: Kanski's Clinical Ophthalmology 10th ed., p. 617–618 | Wills Eye Manual, §11.15 | Harrison's Principles of Internal Medicine 22E
This is a shared conversation. Sign in to Orris to start your own chat.