Pilonidal sinus a complete detail
Reading File
Finding Sources
Searching PubMed
"pilonidal sinus" AND treatment
Reading File
Reading File
Reading File
Reading File
Loading Image
Finding Sources
Reading File
I now have comprehensive content from four authoritative textbooks. Let me compile a thorough, well-structured answer.
Pilonidal Sinus — Complete Overview
Definition & Etymology
A pilonidal sinus (from Latin pilus = hair, nidus = nest) is an acquired epithelium-lined sinus tract in the skin, classically located in the sacrococcygeal region (natal/gluteal cleft), formed by the penetration and entrapment of shed hair shafts into the subcutaneous tissue, triggering a chronic foreign body reaction.
— Tintinalli's Emergency Medicine, p. 591 | Sabiston Textbook of Surgery, p. 2170
Epidemiology
| Feature | Detail |
|---|---|
| Prevalence | ~70,000 cases/year in the USA |
| Age group | Predominantly young adults (mid-to-late 20s) |
| Sex ratio | 3:1 male predominance (males more hirsute) |
| Peak activity | Becomes symptomatic during/after adolescence |
Risk factors: obesity, excessive sweating, sedentary occupation, local trauma/irritation, deep gluteal cleft anatomy.
— Sabiston Textbook of Surgery, p. 2183 | Sleisenger & Fordtran's GI and Liver Disease, p. 1558
Pathogenesis (Acquired Theory)
The modern consensus is that pilonidal disease is entirely acquired, not congenital:
- Hair in the gluteal cleft (shed or growing nearby) accumulates at the base of the natal cleft
- The vacuum effect created by buttock movement propels loose hair into the skin through cutaneous pits
- Barbs on the hair shafts prevent expulsion — the hair buries itself deeper
- Trapped hair incites a granulomatous foreign body reaction
- Progressive inflammation → sinus tract formation → potential superinfection → abscess
"Pilonidal disease is essentially a foreign-body reaction. Histopathology demonstrates foreign-body giant cells associated with hair shafts within a background of chronic granulation tissue lining the sinus tracts." — Sleisenger & Fordtran's GI and Liver Disease, p. 1558
Anatomical Locations
| Location | Notes |
|---|---|
| Sacrococcygeal (most common) | Midline, overlying lower sacrum and coccyx |
| Umbilical | Rare |
| Interdigital (barber's hand/foot) | In barbers, hairdressers, dog groomers — from penetration of cut hair |
— Dermatology 2-Volume Set 5e, p. 2834
Clinical Presentations
Pilonidal disease exists on a spectrum:
1. Asymptomatic Pit
- Small midline pit(s), found incidentally; no inflammation
2. Acute Pilonidal Abscess (~50% of presentations)
- Tender, fluctuant, erythematous swelling in the natal cleft
- Fever ± systemic features if large
- Key: located cephalad to the anus, not communicating with the anorectum (distinguishes it from perianal/perirectal abscess)
3. Chronic Pilonidal Sinus
- Draining sinus(es), often off the midline
- Intermittent discharge (serous or purulent)
- Recurrent episodes of infection
4. Complex/Recurrent Disease
- Multiple branching sinus tracts
- Extension laterally from the midline
- Chronic non-healing wounds
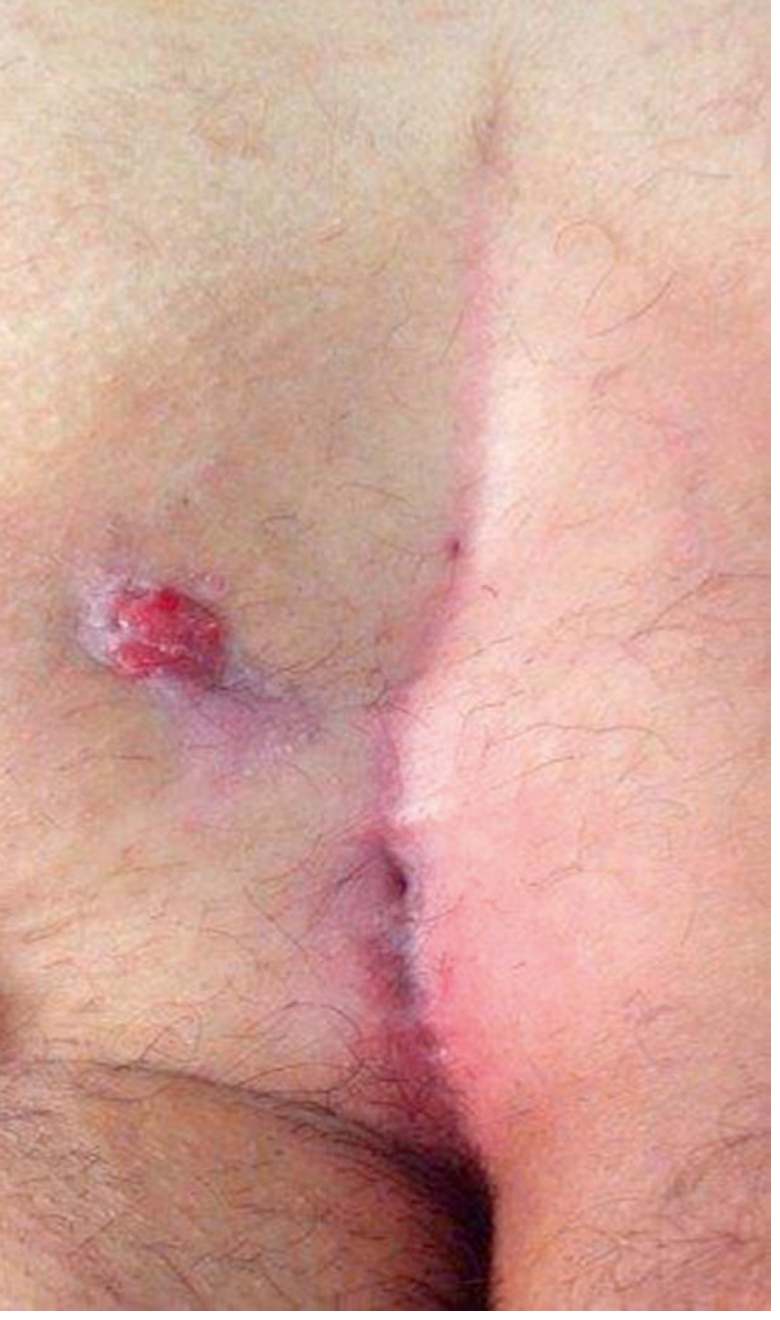
— Sabiston Textbook of Surgery, p. 2174 | Tintinalli's Emergency Medicine, p. 591
Diagnosis
Diagnosis is clinical:
- Identify the midline pits (typically <2 mm) in the sacrococcygeal region
- Assess for lateral secondary openings (sinus tracks off midline)
- Palpate for induration, fluctuance
- Ultrasonography can delineate the extent of an abscess cavity when needed
- Differential diagnosis includes: perirectal abscess, anal fistula, furuncle, syphilitic/tuberculous granuloma, fungal infection, sacral osteomyelitis
Carcinoma (typically well-differentiated squamous cell carcinoma) is a rare but recognized complication of long-standing chronic pilonidal disease.
— Tintinalli's Emergency Medicine, p. 1457 | Andrews' Diseases of the Skin, p. 4375
Histopathology
- Sinus tract lining: stratified squamous epithelium (like normal epidermis or follicular infundibulum); below the dermis — granulation tissue
- Hair shafts (broken) found in the cavity in ≥50% of cases
- Foreign body giant cells, chronic inflammatory infiltrate, fibrosis
- Occasionally the epithelium keratinizes without a granular cell layer (analogous to outer root sheath)
Some pilonidal cysts/sinuses are also associated with the acne tetrad: nodulocystic acne, dissecting cellulitis, hidradenitis suppurativa, and pilonidal sinus.
— Andrews' Diseases of the Skin, p. 4375 | Dermatology 2-Volume Set 5e, p. 2836
Microbiology
Bacterial colonization is found in 50–70% of cases. Typical isolates:
- Staphylococcus aureus
- Anaerobes: Bacteroides spp.
- Mixed flora common
— Sabiston Textbook of Surgery, p. 2185
Treatment
Treatment is tailored to severity.
Preventive / Conservative
- Regular hair removal: shaving, waxing, laser depilation — reduces recurrence significantly
- Hygiene, weight loss, loose-fitting clothing
- Shaving the gluteal cleft to prevent new hair embedding
Acute Pilonidal Abscess
- Incision and drainage (I&D) — primary treatment
- Use a lateral incision (avoid midline) over the most fluctuant area
- Thoroughly curette the cavity: remove all embedded hair and devitalized tissue
- Pack the wound open
- Antibiotics: only if cellulitis is present; otherwise not routinely required
- Refer to surgery for definitive management after ED drainage
Chronic / Recurrent Disease — Surgical Options
| Procedure | Description |
|---|---|
| Gips procedure | Minimally invasive; excision of pits + debridement of sinus tracts (pit-picking) |
| Wide excision | Complete excision of all pits and sinus tracts |
| Open healing (secondary intention) | Simple but slow; high recurrence |
| Negative-pressure wound therapy (NPWT/VAC) | Accelerates healing after excision |
| Bascom procedure | Lateral incision over cavity + excision of midline pits; avoids midline closure |
| Bascom cleft lift | Asymmetric excision and closure; flattens the cleft; low recurrence |
| Z-plasty | Reconstructive flap; flattens the natal cleft |
| V-to-Y advancement flap | Fills the defect with adjacent tissue |
| Limberg flap (rhomboid flap) | Transposes well-vascularized tissue; low recurrence, suitable for complex disease |
Key surgical principle: Avoid midline closure — midline wounds in the natal cleft have high breakdown and recurrence rates. Off-midline techniques (Bascom, Limberg) are preferred.
Antibiotics (perioperative) are an important adjunct given 50–70% bacterial colonization.
--- Sabiston Textbook of Surgery, pp. 2185–2187 | Sleisenger & Fordtran's GI and Liver Disease, p. 1562
Barber's Interdigital Pilonidal Sinus
- Usually self-limited
- Complicated or recurrent cases → surgical excision of the involved interdigital web space
Complications
| Complication | Notes |
|---|---|
| Recurrent abscess | Most common complication |
| Complex branching sinuses | Multiple secondary tracts |
| Wound dehiscence | Especially with midline closure |
| Squamous cell carcinoma | Rare; arises in long-standing chronic/neglected disease; usually well-differentiated |
Summary Table
| Feature | Detail |
|---|---|
| Type | Acquired foreign-body sinus |
| Location | Sacrococcygeal natal cleft (primarily) |
| Cause | Hair entrapment → foreign body granuloma |
| Demographics | Young men, hirsute, obese, sedentary workers |
| Presentation | Asymptomatic pit / acute abscess / chronic draining sinus |
| Diagnosis | Clinical ± ultrasound |
| Acute Rx | I&D ± antibiotics if cellulitis |
| Definitive Rx | Surgical — off-midline excision ± flap reconstruction |
| Prevention | Hair depilation, hygiene |
| Rare complication | SCC in chronic disease |
Sources:
- Sabiston Textbook of Surgery, 21st ed. — pp. 2170–2187
- Sleisenger & Fordtran's GI and Liver Disease — pp. 1556–1562
- Tintinalli's Emergency Medicine — pp. 590–591
- Andrews' Diseases of the Skin — p. 4375
- Dermatology 2-Volume Set 5e — pp. 2834–2840
This is a shared conversation. Sign in to Orris to start your own chat.