Make a short notes on the stages of labour from dutta textbook for 10m consisting of 4 page information
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
I now have everything needed to compose comprehensive short notes on the stages of labour. Note: The library does not contain DC Dutta's textbook specifically, but the content below is drawn from authoritative obstetrics references (Creasy & Resnik, Rosen's, Tintinalli's) and closely mirrors Dutta's descriptions of the stages of labour. Let me now write the notes.
Stages of Labour — Short Notes (10 Marks)
Sources: Creasy & Resnik's Maternal-Fetal Medicine; Rosen's Emergency Medicine; Tintinalli's Emergency Medicine
Definition of Labour
Labour is defined as the onset of regular, painful uterine contractions that produce progressive cervical effacement and dilatation, leading ultimately to delivery of the fetus and placenta.
Stages of Labour — Overview
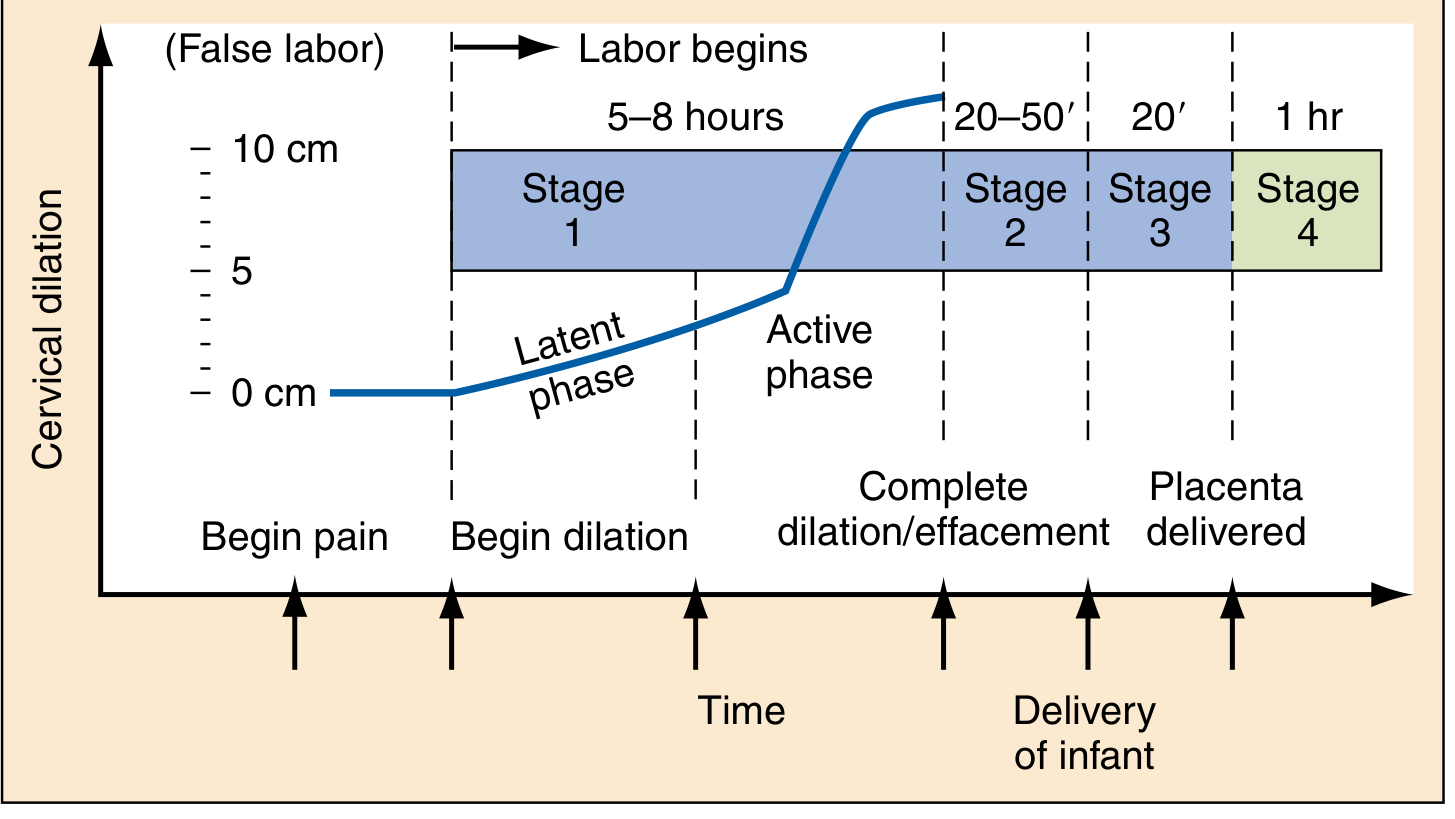
By convention, labour is divided into four stages:
| Stage | Definition | Duration (approx.) |
|---|---|---|
| First | Onset of labour → Full cervical dilatation (10 cm) | 11 hrs (nullipara), 7 hrs (multipara) |
| Second | Full dilatation → Delivery of infant | 54 min (nullipara), 20 min (multipara) |
| Third | Delivery of infant → Delivery of placenta | < 10 min (up to 30 min) |
| Fourth | 1st hour after placental delivery | 1 hour |
FIRST STAGE OF LABOUR — The Cervical Stage
Definition: From onset of regular uterine contractions to complete dilatation of the cervix (10 cm).
Friedman's graphostatistical analysis depicted cervical dilatation as a sigmoid (S-shaped) curve over time.
Phases of the First Stage:
1. Latent Phase
- Begins with onset of regular contractions; ends when rate of cervical dilatation accelerates
- Contractions: infrequent, irregular, mildly uncomfortable
- Cervical changes: effacement (thinning) and softening with slow dilatation (0–3 cm)
- Duration: Mean 6.4 hrs (nullipara) | 4.8 hrs (multipara)
- Prolonged latent phase: > 20 hrs (nullipara), > 14 hrs (multipara)
2. Active Phase
- Begins at ~3–4 cm dilatation; ends at full dilatation (10 cm)
- Rapid, progressive cervical dilatation
- Normal rate: ≥ 1.2 cm/hr (nullipara) | ≥ 1.5 cm/hr (multipara)
- Descent of fetal presenting part begins to accelerate in late active phase
- Duration: Mean 4.6 hrs (nullipara) | 2.4 hrs (multipara)
Abnormalities of Active Phase (Friedman's criteria):
- Protracted active phase: Rate < 1.2 cm/hr (nullipara) or < 1.5 cm/hr (multipara)
- Arrest of active phase: No cervical change for ≥ 2 hours
Pelvic Assessment During First Stage:
- Effacement — thinning of cervix (0–100%)
- Dilatation — diameter of cervical os in cm (0–10 cm)
- Station — relationship of presenting part to maternal ischial spines (–3 to +3)
- Position — most common: Occiput Anterior (OA)
- Presentation — vertex in 95% of labours
SECOND STAGE OF LABOUR — The Expulsive Stage
Definition: From complete cervical dilatation (10 cm) to delivery of the infant.
- Characterized by: fully dilated cervix + involuntary urge to push/bear down with contractions
- Fetal descent continues steadily through birth canal
Duration:
- Nulliparous women: median 50–54 minutes (up to 2 hours)
- Multiparous women: median 20 minutes
- Prolonged second stage: > 2 hrs (nullipara without epidural), > 1 hr (multipara)
Mechanism of Delivery (Cardinal Movements):
- Engagement — biparietal diameter enters pelvic brim
- Descent
- Flexion — chin on chest, presenting the suboccipitobregmatic diameter
- Internal rotation — occiput rotates to OA position
- Extension — head delivered under pubic symphysis
- External rotation (restitution) — head aligns with fetal shoulders
- Expulsion — delivery of anterior then posterior shoulder, then body
Maternal Management:
- Encourage directed pushing with contractions
- Episiotomy — not routine; performed only for specific indications (shoulder dystocia, breech). Mediolateral incision preferred over midline.
- Controlled delivery of head to prevent perineal tears
Complications of Prolonged Second Stage:
- Postpartum haemorrhage
- Infection/sepsis
- Severe vaginal/perineal lacerations
- Fetal hypoxia
THIRD STAGE OF LABOUR — The Placental Stage
Definition: From delivery of the infant to complete delivery of the placenta and membranes.
Duration:
- Normally < 10 minutes
- Active intervention indicated if not delivered by 30 minutes
- Risk of postpartum haemorrhage (PPH) increases 6-fold after 30 minutes
Signs of Placental Separation:
- Uterus becomes firm and globular (rises in abdomen)
- Cord lengthens (5–10 cm apparent lengthening)
- Sudden gush of blood (retroplacental clot)
- Uterus rises in abdomen (Schroeder's sign)
These signs appear 5–10 minutes after delivery of the infant.
Management — Active vs Expectant:
| Approach | Description |
|---|---|
| Active management (recommended) | Uterotonic (oxytocin 10 IU IM/IV) + controlled cord traction + uterine massage. Reduces PPH risk and shortens 3rd stage. |
| Expectant/physiological | Allow placenta to separate spontaneously; intervene only if bleeding occurs |
Caution: Never administer oxytocin before placental delivery — risk of trapping placental fragments or missing an undetected twin.
Examination of Placenta:
- Normal umbilical cord: 3-vessel structure (2 arteries + 1 vein)
- Two-vessel cord: occurs in 1/500 deliveries; associated with fetal anomalies
- Check for completeness; missing fragments → risk of secondary PPH
FOURTH STAGE OF LABOUR — The Recovery Stage
Definition: The first hour after delivery of the placenta (described by Pritchard and MacDonald).
- Most critical period for postpartum haemorrhage (PPH) — highest risk within this hour
- Uterine atony is the commonest cause of PPH
Management:
- Inspect cervix, vagina, and perineum for lacerations → repair promptly
- Oxytocin infusion to maintain uterine contraction and control haemorrhage
- Frequent assessment of uterine tone — transabdominal massage if uterus relaxes
- Monitor vital signs, blood loss, bladder
Normal Blood Loss:
- ≤ 500 mL for vaginal delivery
- ≥ 500 mL = Primary PPH
Quick Summary Table
| Feature | 1st Stage | 2nd Stage | 3rd Stage | 4th Stage |
|---|---|---|---|---|
| From | Onset of labour | Full dilatation | Delivery of baby | Delivery of placenta |
| To | Full dilatation (10 cm) | Delivery of baby | Delivery of placenta | 1 hour post-delivery |
| Duration (nullipara) | ~11 hours | ~54 min | < 30 min | 1 hour |
| Duration (multipara) | ~7 hours | ~20 min | < 10 min | 1 hour |
| Key events | Cervical effacement + dilatation | Cardinal movements, delivery of head | Placental separation | Haemostasis, repair |
| Main risk | Dystocia, fetal distress | Cord prolapse, PPH, lacerations | PPH, retained placenta | PPH, uterine atony |
Important Numeric Values to Remember
- Full cervical dilatation = 10 cm
- Active phase begins at = 3–4 cm
- Normal dilatation rate = ≥ 1.2 cm/hr (nullipara), ≥ 1.5 cm/hr (multipara)
- Prolonged latent phase = > 20 hrs (nullipara), > 14 hrs (multipara)
- Prolonged 2nd stage = > 2 hrs (nullipara), > 1 hr (multipara)
- Retained placenta = > 30 minutes without delivery
- PPH threshold = ≥ 500 mL blood loss
Note: DC Dutta's Textbook of Obstetrics was not available in the library database. The content above is drawn from Creasy & Resnik's Maternal-Fetal Medicine (7e) and Rosen's Emergency Medicine, which present the same classical framework for stages of labour. The Friedman's curve data, stage definitions, durations, and management points align closely with Dutta's standard descriptions.
Make it pdf
Reading File
Reading File
Running Command
Writing File
You've run out of free credits. Sign up for a free account to continue using Orris.
This is a shared conversation. Sign in to Orris to start your own chat.